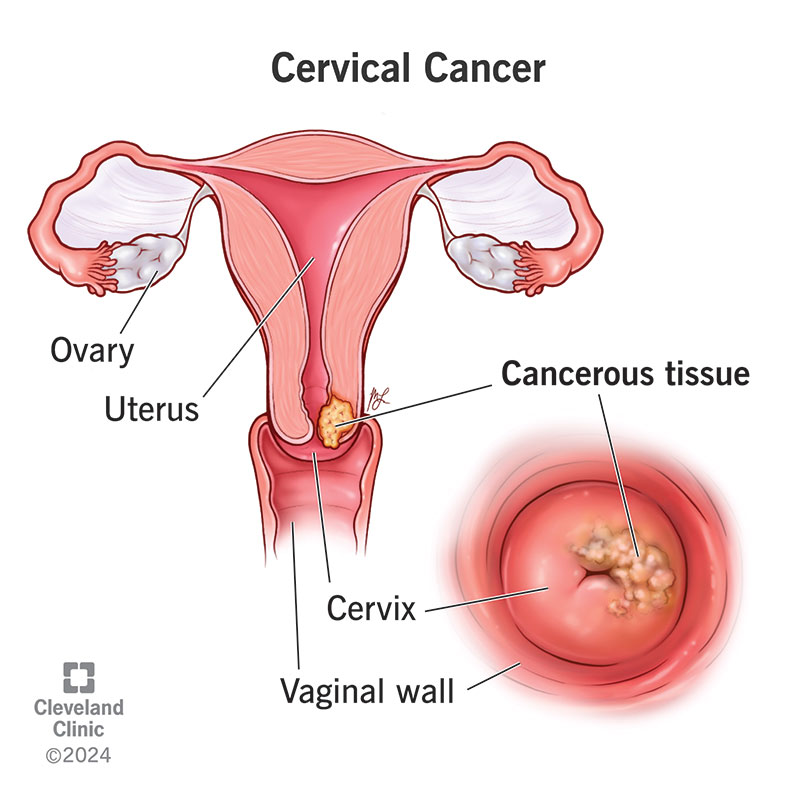
You’re about to embark on a journey to gain a better understanding of cervical dysplasia and its causes and symptoms. This article will shed light on this common medical condition, guiding you through the intricacies of its development and how it can be detected early. So, get ready to arm yourself with knowledge, as we delve into the world of cervical dysplasia together.

Causes of Cervical Dysplasia
Human Papillomavirus (HPV) Infection
One of the main causes of cervical dysplasia is infection with the Human Papillomavirus (HPV). HPV is a sexually transmitted infection that is very common. There are many different strains of HPV, and some of them can lead to the development of cervical dysplasia. When a person is infected with HPV, the virus can cause changes in the cells of the cervix, leading to dysplasia. It is important to note that not all women who have HPV will develop cervical dysplasia, but it is a significant risk factor.
Smoking and Tobacco Use
Smoking and tobacco use have been identified as risk factors for the development of cervical dysplasia. The chemicals in tobacco can affect the cells of the cervix, making them more susceptible to changes that can lead to dysplasia. Studies have shown that smokers are more likely to have persistent HPV infections, which can increase the risk of dysplasia. Quitting smoking can reduce the risk of developing cervical dysplasia and can also improve the chances of successful treatment if dysplasia is already present.
Weakening of the Immune System
A weakened immune system can also contribute to the development of cervical dysplasia. The immune system plays a crucial role in identifying and destroying abnormal cells, including those caused by HPV. If the immune system is not functioning properly, it may not be able to effectively eliminate abnormal cells, allowing them to multiply and progress to dysplasia. Conditions that can weaken the immune system include HIV/AIDS, organ transplantation, and certain medications that suppress immune function.
Sexual History
The number of sexual partners a person has had and the age at which they first became sexually active can also impact the risk of developing cervical dysplasia. Having multiple sexual partners increases the chances of coming into contact with HPV, which can lead to dysplasia. Additionally, starting sexual activity at a young age can also increase the risk, as the cervix may be more susceptible to infection during adolescence.
Unprotected Sex and Multiple Partners
Engaging in unprotected sex and having multiple sexual partners can significantly increase the risk of developing cervical dysplasia. Using barrier methods such as condoms can reduce the risk of contracting HPV and other sexually transmitted infections. It is important to practice safe sex and have open communication with sexual partners about sexual health to minimize the risk of developing cervical dysplasia.
Risk Factors for Developing Cervical Dysplasia
Age
Age is a significant risk factor for developing cervical dysplasia. The likelihood of developing dysplasia increases with age, with the highest incidence seen in women between the ages of 25 and 35. This may be due to the cumulative effects of HPV exposure over time, as well as the natural aging process of cervical cells.
Weakened Immune System
As mentioned earlier, a weakened immune system can increase the risk of developing cervical dysplasia. Conditions such as HIV/AIDS or organ transplantation, as well as certain medications, can weaken the immune system’s ability to detect and eliminate abnormal cells in the cervix.
Sexual History
Engaging in unprotected sex and having multiple sexual partners are risk factors for developing cervical dysplasia. The more sexual partners a person has had, the higher their risk of being exposed to HPV, which can lead to dysplasia. Additionally, starting sexual activity at a young age can also increase the risk.
Smoking and Tobacco Use
Smoking and tobacco use have been identified as risk factors for a variety of health problems, including cervical dysplasia. The chemicals in tobacco can affect the cells of the cervix, making them more susceptible to abnormal changes. Smoking also increases the likelihood of persistent HPV infections, which can lead to dysplasia.
Long-term Use of Oral Contraceptives
Long-term use of oral contraceptives (birth control pills) has been associated with an increased risk of developing cervical dysplasia. It is believed that the hormones in the pills may contribute to the development of abnormal cervical cells. However, the risk is relatively small and should be weighed against the benefits of using oral contraceptives for other reasons.
Symptoms of Cervical Dysplasia
No Symptoms
In many cases, cervical dysplasia does not cause any noticeable symptoms. The condition is often detected during routine Pap smear screenings or colposcopy examinations, which are used to evaluate the health of the cervix. This is why regular screenings are so important, as they can detect dysplasia before it progresses to a more serious condition.
Abnormal Pap Smear
An abnormal Pap smear result is often the first indication of cervical dysplasia. During a Pap smear, cells from the cervix are collected and examined under a microscope for any abnormalities. If the test reveals abnormal cells, further testing may be necessary to determine the extent of the dysplasia and develop an appropriate treatment plan.
Abnormal Bleeding
In some cases, cervical dysplasia can cause abnormal bleeding. This may include bleeding between periods, heavier or longer menstrual periods, or bleeding after sexual intercourse. If you experience any unusual bleeding, it is important to consult with your healthcare provider to determine the cause.
Pelvic Pain
Pelvic pain can be a symptom of more advanced cervical dysplasia. As the abnormal cells multiply and spread, they can cause discomfort or pain in the pelvic region. If you experience persistent pelvic pain, it is important to seek medical attention for further evaluation.
Abnormal Vaginal Discharge
Cervical dysplasia can also lead to changes in vaginal discharge. You may notice increased discharge, changes in color or consistency, or a foul odor. These changes may be caused by the abnormal cervical cells or by an accompanying infection. It is important to consult with your healthcare provider to determine the cause and receive appropriate treatment.
Types of Cervical Dysplasia
Mild Dysplasia (CIN I)
Mild dysplasia, also known as CIN I (cervical intraepithelial neoplasia grade 1), is characterized by the presence of mildly abnormal cells. These cells are considered to be precancerous and have the potential to progress to more severe dysplasia or even cervical cancer if left untreated. Treatment options for mild dysplasia often involve close observation and monitoring, as many cases may resolve on their own without intervention.
Moderate Dysplasia (CIN II)
Moderate dysplasia, also referred to as CIN II, involves the presence of more pronounced abnormal cells. The risk of progression to cervical cancer is higher with moderate dysplasia compared to mild dysplasia. Treatment options for moderate dysplasia may include procedures such as laser therapy, cryotherapy, or cone biopsy to remove the abnormal cells and prevent further progression.
Severe Dysplasia (CIN III)
Severe dysplasia, also known as CIN III, is characterized by the presence of severely abnormal cells that are highly likely to progress to cancer. Prompt and appropriate treatment is necessary to remove the abnormal cells and prevent the development of cervical cancer. Treatment options for severe dysplasia may include treatments like loop electrosurgical excision procedure (LEEP), cone biopsy, or even hysterectomy in more severe cases.
Carcinoma in situ (CIS)
Carcinoma in situ (CIS) refers to the presence of cancerous cells that are confined to the surface layer of the cervix. While CIS is the earliest stage of cervical cancer, it is still considered a form of cervical dysplasia. Treatment typically involves surgical removal of the abnormal cells, and regular follow-up is necessary to monitor for any recurrence or progression.

Diagnosing Cervical Dysplasia
Pap Smear
The Pap smear is a commonly used screening test for cervical dysplasia. During this test, cells are collected from the cervix and examined under a microscope for any abnormal changes. If abnormal cells are detected, further testing may be needed to determine the severity and extent of the dysplasia.
Colposcopy
Colposcopy is a procedure that allows for a closer examination of the cervix. A special instrument called a colposcope is used to magnify the cervix and visualize any abnormal areas. If suspicious areas are identified, a biopsy may be performed to collect a small sample of tissue for further evaluation.
Biopsy
A biopsy involves the removal of a small sample of cells or tissue for examination under a microscope. It is often performed during a colposcopy if abnormal areas are detected. The biopsy can provide more information about the stage and severity of the dysplasia, helping to guide treatment decisions.
HPV DNA Test
The HPV DNA test is used to detect high-risk types of HPV that are associated with the development of cervical dysplasia and cervical cancer. This test is often performed in conjunction with a Pap smear, especially in women over 30 years of age, to provide a more comprehensive assessment of the risk of dysplasia.
Endocervical Curettage
Endocervical curettage (ECC) is a procedure that involves scraping the inside of the cervix to collect cells from the endocervical canal. This can help to identify any abnormal changes in the deeper layers of the cervix that may not be visible during a colposcopy. ECC is usually performed if there are concerns about the extent of the dysplasia or if a biopsy is inconclusive.
Treatment Options for Cervical Dysplasia
Observation
In some cases, mild dysplasia may resolve on its own without any specific treatment. This often involves close monitoring of the condition through regular follow-up appointments and Pap smears. If the dysplasia does not progress or improves over time, no further intervention may be needed. However, regular screening is essential to ensure prompt detection of any changes.
Laser Therapy
Laser therapy is a treatment option for cervical dysplasia that uses a laser beam to destroy abnormal cells on the cervix. The laser precisely targets the abnormal tissue while minimizing damage to healthy tissue. Laser therapy is often used for mild to moderate dysplasia and can be performed on an outpatient basis.
Cryotherapy
Cryotherapy involves using freezing temperatures to destroy abnormal cells on the cervix. A probe is used to apply extreme cold to the cervix, killing the abnormal cells. Cryotherapy is a commonly used treatment option for mild dysplasia but may also be used for more severe cases.
Loop Electrosurgical Excision Procedure (LEEP)
LEEP is a procedure that uses a thin wire loop heated by an electrical current to remove abnormal cells from the cervix. It is often used for moderate to severe dysplasia or when more extensive removal of abnormal tissue is necessary. LEEP is usually performed under local anesthesia and can be done on an outpatient basis.
Cone Biopsy
A cone biopsy involves the removal of a cone-shaped piece of tissue from the cervix. This procedure is typically performed for cases of severe dysplasia or when the dysplasia extends into the deeper layers of the cervix. Cone biopsy may be performed under local or general anesthesia and may require hospitalization.
Hysterectomy
In very severe cases of cervical dysplasia or when other treatment options have failed, a hysterectomy may be recommended. A hysterectomy involves the surgical removal of the uterus, cervix, and sometimes the surrounding tissues. This procedure is considered a last resort and is typically reserved for cases in which the dysplasia has progressed to cervical cancer or when fertility is no longer a concern.

Preventing Cervical Dysplasia
HPV Vaccination
Vaccination against HPV is an effective method of preventing cervical dysplasia. The HPV vaccine protects against the most common high-risk strains of the virus that are associated with dysplasia and cervical cancer. It is recommended for both males and females, ideally before the onset of sexual activity.
Safe Sex Practices
Engaging in safe sex practices can help reduce the risk of HPV infection and subsequent development of cervical dysplasia. Using barrier methods, such as condoms, can provide a certain level of protection against HPV transmission. It is important to practice safe sex with all sexual partners and to have open discussions about sexual health.
Smoking Cessation
Quitting smoking is not only beneficial for overall health but can also reduce the risk of cervical dysplasia. The chemicals in tobacco can weaken the immune system and make cervical cells more susceptible to abnormal changes. By quitting smoking, you can decrease the likelihood of developing dysplasia and improve the chances of successful treatment if dysplasia is already present.
Regular Pap Smears
Regular Pap smears are crucial for early detection and prevention of cervical dysplasia. Pap smears can detect abnormal changes in the cells of the cervix before they progress to dysplasia or cancer. It is important to follow the recommended screening guidelines and discuss with your healthcare provider how often you should have a Pap smear.
Early Detection and Treatment of Dysplasia
Early detection and prompt treatment of cervical dysplasia are essential for preventing the progression to cervical cancer. Regular screenings can help identify dysplasia at an early stage when it is more easily treatable. If dysplasia is detected, it is important to follow the recommended treatment plan and attend all follow-up appointments.
Complications Associated with Cervical Dysplasia
Progression to Cervical Cancer
If left untreated, cervical dysplasia can progress to cervical cancer. The risk of progression is higher with more severe forms of dysplasia, such as severe dysplasia or carcinoma in situ. Regular screenings and prompt treatment are essential to prevent the development of cervical cancer.
Emotional Distress
A diagnosis of cervical dysplasia can be emotionally distressing. It may cause anxiety, fear, or worry about the future and the potential for developing cervical cancer. It is important to seek emotional support, whether from friends, family, or a healthcare provider, to help cope with these feelings.
Fertility Issues
In some cases, more extensive treatments for cervical dysplasia, such as cone biopsy or hysterectomy, may impact fertility. These procedures can remove or affect the reproductive organs, making it more difficult to conceive or carry a pregnancy. If fertility preservation is a concern, it is important to discuss this with your healthcare provider before undergoing any treatment.
Pregnancy Complications
Cervical dysplasia, especially in its more advanced stages, can increase the risk of pregnancy complications. These complications may include premature birth, low birth weight, or the need for cesarean delivery. Regular prenatal care and close monitoring can help reduce the risk of complications and ensure a healthy pregnancy.

Living with Cervical Dysplasia
Supportive Care
Living with cervical dysplasia may require ongoing supportive care. This may involve regular follow-up appointments with your healthcare provider to monitor the condition and ensure early detection of any changes. Your provider can also provide guidance on lifestyle modifications, such as quitting smoking or practicing safe sex, to reduce the risk of dysplasia progression.
Emotional Support
Dealing with a diagnosis of cervical dysplasia can be emotionally challenging. It is important to seek emotional support from loved ones, support groups, or mental health professionals if needed. They can provide guidance, reassurance, and coping strategies to navigate through the emotional aspects of living with dysplasia.
Follow-up and Monitoring
Regular follow-up appointments and monitoring are essential for individuals living with cervical dysplasia. These appointments may involve Pap smears, colposcopies, or other tests to assess the progression or regression of the dysplasia. Compliance with recommended follow-up schedules is crucial to ensure early detection and timely intervention if necessary.
Coping Strategies
Living with cervical dysplasia may require adopting coping strategies to manage the challenges associated with the condition. These strategies may include stress management techniques, engaging in regular physical activity, seeking support from friends and family, and staying informed about the latest research and treatment options. Each person’s coping strategies may be unique, and it is important to find what works best for you.
FAQs about Cervical Dysplasia
What is the main cause of cervical dysplasia?
The main cause of cervical dysplasia is infection with the Human Papillomavirus (HPV). HPV is a sexually transmitted infection that can lead to changes in the cells of the cervix, increasing the risk of dysplasia.
Can cervical dysplasia be cured?
Yes, cervical dysplasia can be cured, especially when detected early. Treatment options such as laser therapy, cryotherapy, cone biopsy, or loop electrosurgical excision (LEEP) can remove or destroy the abnormal cells and prevent further progression.
What are the treatment options for cervical dysplasia?
Treatment options for cervical dysplasia depend on the severity of the dysplasia. Mild cases may require no specific treatment and are often monitored closely. Moderate to severe dysplasia may be treated with procedures such as laser therapy, cryotherapy, LEEP, cone biopsy, or even hysterectomy in more severe cases.
Can cervical dysplasia lead to cancer?
Yes, if left untreated, cervical dysplasia can progress to cervical cancer. Regular screenings and prompt treatment are essential for preventing the development of cervical cancer.
How often should Pap smears be done?
The frequency of Pap smears may vary depending on factors such as age, sexual history, and previous Pap smear results. As a general guideline, it is recommended to start Pap smears at age 21 and have them done every three years until age 29. After age 30, Pap smears can be done every three to five years in conjunction with an HPV DNA test. It is important to discuss the recommended screening frequency with your healthcare provider based on your individual circumstances.