Hey there! If you’ve ever wondered about those pesky little companions called hemorrhoids, then this article is just for you! In this comprehensive guide, we will take a closer look at what causes hemorrhoids, the common symptoms to look out for, and some effective treatments to provide relief. So, grab a cup of tea, sit back, and let’s dive into the world of hemorrhoids together! Whether you’re experiencing discomfort or just genuinely curious, understanding these pesky piles will surely be beneficial.

Causes of Hemorrhoids
Hemorrhoids, also known as piles, can be caused by a variety of factors. Understanding these causes can help you prevent or manage this common condition.
Prolonged sitting or standing
One major culprit behind hemorrhoids is prolonged sitting or standing. When you spend long hours in a seated or standing position, the blood flow to the rectal area can be restricted. This can lead to the formation of hemorrhoids over time. To prevent this, it’s important to take regular breaks and move around to improve circulation.
Chronic constipation or diarrhea
Another common cause of hemorrhoids is chronic constipation or diarrhea. When you strain during bowel movements due to constipation, the pressure on the veins in your rectal area can increase. Similarly, frequent episodes of diarrhea can irritate the rectal area and lead to hemorrhoids. Maintaining a healthy diet, staying hydrated, and addressing any underlying digestive issues can help prevent hemorrhoids caused by constipation or diarrhea.
Obesity and lack of physical activity
Obesity and lack of physical activity can contribute to the development of hemorrhoids. Being overweight puts extra pressure on the veins in your rectal area, making them more susceptible to developing hemorrhoids. Regular exercise not only helps manage your weight but also improves blood circulation, reducing the risk of hemorrhoids.
Pregnancy and childbirth
Pregnancy and childbirth are common causes of hemorrhoids in women. The increased pressure on the rectal area during pregnancy, along with hormonal changes, can lead to the development of hemorrhoids. Additionally, the act of pushing during childbirth can further aggravate existing hemorrhoids or cause new ones to form. Taking measures to manage constipation during pregnancy, such as eating a high-fiber diet and staying hydrated, can help prevent hemorrhoids.
Straining during bowel movements
One of the most common causes of hemorrhoids is straining during bowel movements. Straining puts excessive pressure on the veins in the rectal area, leading to the formation of hemorrhoids. It’s important to have regular bowel movements and avoid straining. Eating a diet high in fiber, staying hydrated, and practicing good bathroom habits can help prevent straining and reduce the risk of hemorrhoids.
Types of Hemorrhoids
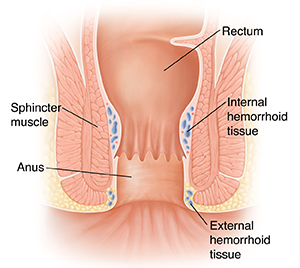
Hemorrhoids can be classified into three main types: internal, external, and prolapsed hemorrhoids.
Internal hemorrhoids
Internal hemorrhoids are located inside the rectum and are not visible to the naked eye. They usually don’t cause pain but may result in bleeding during bowel movements. If they become enlarged or prolapse, they can cause discomfort and may need medical intervention.
External hemorrhoids
External hemorrhoids develop outside the anus and can be seen or felt. They can cause itching, pain, and irritation. External hemorrhoids may become swollen or thrombosed, which means a blood clot has formed inside. This can cause intense pain and may require medical attention.
Prolapsed hemorrhoids
Prolapsed hemorrhoids occur when internal hemorrhoids protrude outside the rectum. They can be felt as moist lumps, and they may cause discomfort or pain. Prolapsed hemorrhoids may need to be treated if they don’t retract on their own.
Symptoms of Hemorrhoids
Recognizing the symptoms of hemorrhoids is crucial for early detection and management. Here are some common symptoms to be aware of:
Bleeding during bowel movements
One of the most noticeable symptoms of hemorrhoids is bleeding during bowel movements. You may notice bright red blood on the toilet paper or in the toilet bowl. It’s important not to ignore this symptom, as it can be a sign of both internal and external hemorrhoids.
Itching and irritation
Hemorrhoids can cause itching and irritation in the anal area. This can be quite uncomfortable and may lead to scratching, which can further worsen the condition. Keeping the area clean and using soothing creams or ointments can help alleviate these symptoms.
Pain and discomfort
Hemorrhoids can be painful, especially if they become swollen or thrombosed. The pain may range from mild to severe, and it can make sitting, standing, or bowel movements uncomfortable. Over-the-counter pain relievers and warm baths can help manage the pain.
Swelling and inflammation
Hemorrhoids can cause swelling and inflammation around the anus. This can make the area feel tender and cause discomfort. Applying cold compresses or using over-the-counter anti-inflammatory creams can help reduce the swelling and inflammation.
Sensitive lumps around the anus
You may feel small, sensitive lumps around the anus when you have hemorrhoids. These lumps can be both internal and external hemorrhoids. If you notice any unusual lumps, it’s important to have them examined by a healthcare professional to determine the appropriate treatment.
Diagnosis of Hemorrhoids
If you suspect you have hemorrhoids, it’s important to seek a proper medical diagnosis. Here are the common methods used to diagnose hemorrhoids:
Physical examination
A healthcare provider will perform a physical examination of the anal area to look for any visible signs of hemorrhoids. They may use gloves and lubrication to examine the rectal area for any lumps or abnormalities.
Medical history and symptoms
Your healthcare provider will ask about your medical history and inquire about your symptoms. They may ask questions about your bowel habits, diet, lifestyle, and any previous occurrences of hemorrhoids.
Visual inspection with an anoscope or sigmoidoscope
In some cases, a healthcare provider may use a specialized instrument called an anoscope or sigmoidoscope to get a closer look at the rectal area. These instruments allow them to visualize the internal hemorrhoids and determine the appropriate course of treatment.

Treatments for Hemorrhoids
There are various treatment options available for hemorrhoids, ranging from conservative measures to more invasive procedures. The choice of treatment depends on the severity of the hemorrhoids and the individual’s preferences. Here are some common treatment options:
Home remedies and lifestyle changes
Mild cases of hemorrhoids can often be managed with home remedies and lifestyle changes. These may include increasing fiber intake, drinking plenty of water, taking over-the-counter pain relievers or anti-inflammatory creams, and practicing good hygiene. Avoiding excessive straining during bowel movements and maintaining regular bowel habits can also help prevent hemorrhoids from worsening.
Over-the-counter creams and ointments
Over-the-counter creams and ointments, such as hydrocortisone or witch hazel, can help alleviate itching, pain, and inflammation associated with hemorrhoids. These topical treatments are readily available and can provide temporary relief.
Sitz baths and cold compresses
Taking sitz baths, where you sit in warm water for 10-15 minutes, can help soothe the discomfort and reduce swelling. Applying cold compresses or ice packs to the affected area can also provide relief from pain and inflammation.
Prescription medications
In some cases, prescription medications may be recommended to manage hemorrhoids. These may include topical creams containing stronger steroids or medications to alleviate pain or itching. Your healthcare provider will determine the most appropriate medication based on your symptoms and medical history.
Rubber band ligation
Rubber band ligation is a common procedure used to treat internal hemorrhoids. It involves placing a small rubber band around the base of the hemorrhoid, cutting off its blood supply. Over time, the hemorrhoid shrinks and falls off. This procedure is typically performed in a healthcare provider’s office and may cause some discomfort during recovery.
Sclerotherapy
Sclerotherapy is another treatment option for internal hemorrhoids. It involves injecting a chemical solution into the hemorrhoid, causing it to shrink and eventually disappear. Sclerotherapy is usually done as an outpatient procedure and may require multiple sessions for optimal results.
Infrared coagulation
Infrared coagulation is a non-surgical procedure that uses heat to shrink the hemorrhoid. A healthcare provider will use a device that emits infrared light to create scar tissue, which helps to reduce the blood flow to the hemorrhoid. This causes it to shrink over time.
Hemorrhoidectomy
In severe cases of hemorrhoids, a surgical procedure called hemorrhoidectomy may be necessary. This involves the complete removal of the hemorrhoid tissue. Hemorrhoidectomy is typically reserved for large or recurrent hemorrhoids and is performed under anesthesia in a hospital setting. Recovery can be uncomfortable, and it may take a few weeks for complete healing.
Hemorrhoid stapling
Hemorrhoid stapling, or stapled hemorrhoidopexy, is a surgical procedure that aims to reposition the hemorrhoid tissue back into its normal position. Staples are used to block blood flow to the hemorrhoid, reducing its size and symptoms. This procedure is less painful than a hemorrhoidectomy and generally has a faster recovery time.
Prevention of Hemorrhoids
Preventing hemorrhoids is possible by adopting certain lifestyle habits and making changes to your daily routine. Here are some preventive measures you can take:
Maintain regular bowel habits
Establishing regular bowel habits can help prevent constipation and reduce the risk of straining during bowel movements. Aim to have a bowel movement at the same time each day and avoid holding in stools when you feel the urge to go.
Eat a high-fiber diet
Consuming a diet rich in fiber can help maintain regular bowel movements and prevent constipation. Include plenty of fruits, vegetables, whole grains, and legumes in your diet. Fiber softens the stool, making it easier to pass.
Stay hydrated
Drinking an adequate amount of water throughout the day is essential for maintaining healthy bowel movements. Staying hydrated helps soften the stool and prevents constipation.
Avoid prolonged sitting or standing
Prolonged sitting or standing can increase the pressure on the veins in the rectal area, leading to the development of hemorrhoids. Take regular breaks and try to incorporate movement into your daily routine.
Exercise regularly
Regular exercise promotes healthy digestion, improves blood circulation, and helps maintain a healthy weight. Aim for at least 30 minutes of moderate-intensity exercise most days of the week.
Manage weight
Maintaining a healthy weight reduces the strain on the veins in the rectal area. Incorporate a balanced diet and regular physical exercise to manage your weight effectively.
Avoid straining during bowel movements
Avoid straining or holding your breath while having a bowel movement, as this can increase pressure in the rectal area. If you’re having difficulty passing stool, try using a footstool to elevate your feet, which can help align your body for easier elimination.
Take breaks during prolonged sitting or standing
If your job or lifestyle involves prolonged sitting or standing, make sure to take regular breaks to move around and improve blood circulation. Sitting or standing for long periods can contribute to the development of hemorrhoids.
Complications of Hemorrhoids
While hemorrhoids are generally not serious, they can sometimes lead to complications. Here are some potential complications of hemorrhoids:
Thrombosed hemorrhoids
A thrombosed hemorrhoid occurs when a blood clot forms inside an external hemorrhoid. This can cause severe pain and swelling. Thrombosed hemorrhoids often require medical intervention to alleviate symptoms and promote healing.
Anemia
Chronic bleeding from hemorrhoids can lead to anemia, a condition characterized by a deficiency of red blood cells or hemoglobin in the blood. Anemia can cause fatigue, weakness, and other symptoms. If you experience persistent bleeding, it’s important to seek medical advice to determine the cause and appropriate treatment.
Fecal incontinence
In rare cases, large prolapsed hemorrhoids can lead to fecal incontinence, which is the inability to control bowel movements. This can occur if the hemorrhoids obstruct the anal canal or weaken the anal sphincter muscles. If you experience persistent loss of bowel control, consult a healthcare professional for an evaluation.
Infection or abscess
Hemorrhoids that become infected or develop an abscess can cause severe pain, swelling, and discomfort. In some cases, an abscess may need to be drained surgically. If you notice signs of infection, such as increased pain, fever, or discharge, seek medical attention.
Strangulated hemorrhoids
In rare cases, internal hemorrhoids can become strangulated, meaning the blood supply to the hemorrhoid is cut off. Strangulated hemorrhoids can cause severe pain and can lead to tissue death. Immediate medical attention is necessary to prevent further complications.
When to See a Doctor
While many cases of hemorrhoids can be managed at home with self-care measures, there are certain circumstances where you should seek medical attention. Here are some situations when it’s important to consult a healthcare professional:
Presence of severe bleeding
If you experience excessive or persistent bleeding from hemorrhoids, it’s important to see a doctor. Severe bleeding may indicate a more serious underlying condition that requires medical intervention.
Excessive pain and discomfort
Intense or prolonged pain, especially in combination with other symptoms, should prompt a visit to a healthcare provider. They can assess your condition and suggest appropriate pain management strategies or treatment options.
Persistent symptoms despite self-care
If your symptoms don’t improve or worsen despite self-care measures, it’s advisable to seek medical advice. Persistent symptoms may indicate an underlying issue that requires professional attention.
Changes in bowel habits
Significant changes in bowel habits, such as sudden and persistent diarrhea or constipation, should be evaluated by a healthcare provider. These changes may be a sign of an underlying condition that needs to be addressed.
Recurrent hemorrhoids
If you have frequent episodes of hemorrhoids or develop new ones regularly, it’s important to consult a healthcare professional. They can help identify any underlying factors contributing to the recurrence and discuss appropriate treatment options.

Conclusion
Hemorrhoids are a common condition that can cause discomfort, pain, and inconvenience. Understanding the causes, symptoms, and treatment options can empower you to prevent or manage hemorrhoids effectively. By implementing lifestyle changes, home remedies, and seeking medical advice when necessary, you can alleviate symptoms and improve your overall well-being. Remember, it’s always important to consult a healthcare professional for a proper diagnosis and guidance tailored to your specific situation.