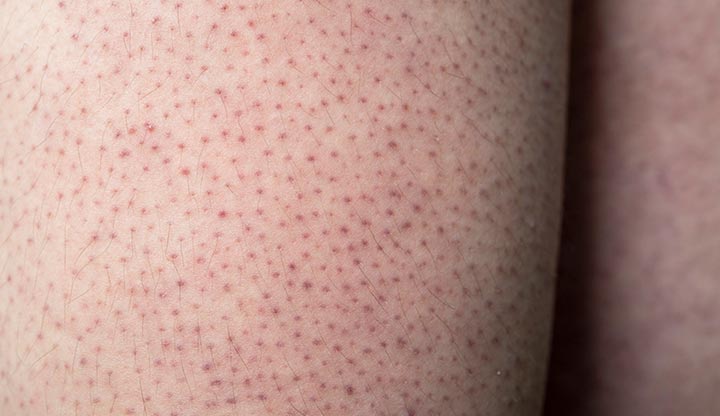
You may have noticed small bumps or rough, dry patches on your skin, particularly on your arms, thighs, or buttocks. Don’t worry, you’re not alone. This common skin condition is called keratosis pilaris, and understanding its causes, symptoms, and treatment options can help you find relief and restore the smoothness to your skin. In this article, we’ll explore what keratosis pilaris is, why it occurs, the signs to look out for, and a range of treatments that can help you manage this condition effectively. So, let’s dive in and discover everything you need to know about keratosis pilaris.
Causes of Keratosis Pilaris
Genetics
Keratosis Pilaris, often referred to as “chicken skin,” is a common skin condition that affects many individuals. One of the primary causes of this condition is genetics. If you have a family history of this condition, there is a higher chance that you may develop it as well. The exact genetic factors that contribute to the development of Keratosis Pilaris are still being studied, but understanding your family history can give you a better idea of your risk.
Dry skin
Dry skin is another leading cause of Keratosis Pilaris. When the skin lacks moisture, it becomes rough and prone to irritation, making it more susceptible to developing small bumps and inflammation associated with Keratosis Pilaris. If you have dry skin, you may be more likely to develop this condition. Keeping your skin well-hydrated is crucial in managing and preventing Keratosis Pilaris.
Keratin buildup
Keratosis Pilaris occurs when there is an overproduction and buildup of keratin in the hair follicles. Keratin is a protein that helps protect the skin, but when there is an excess buildup, it can block the hair follicles, leading to the formation of small bumps and rough, dry skin. Factors such as hormonal changes, certain medications, and other skin conditions can contribute to the excessive buildup of keratin. Understanding the underlying causes of keratin buildup can help you better manage your condition.
Symptoms of Keratosis Pilaris
Small bumps on the skin
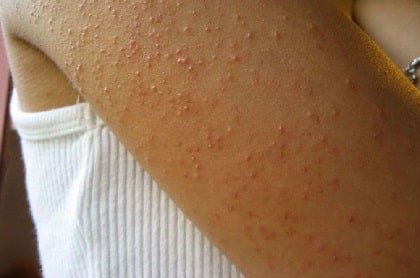
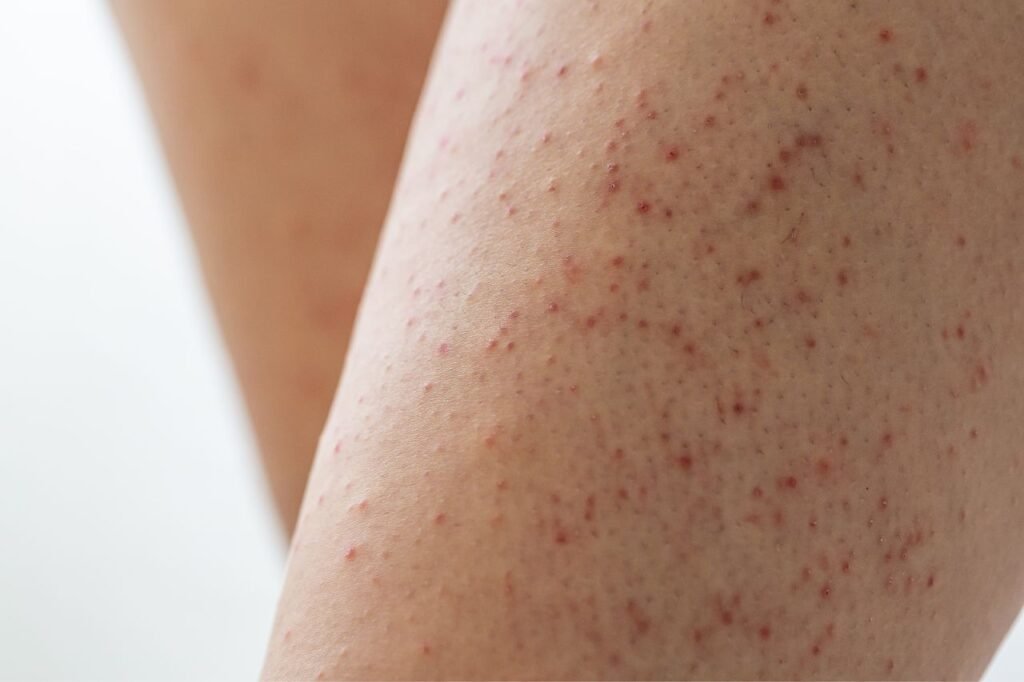
One of the most common symptoms of Keratosis Pilaris is the presence of small, raised bumps on the skin. These bumps are usually flesh-colored or slightly red and can vary in size. They are most commonly found on the upper arms, thighs, buttocks, and sometimes the face. The bumps may be accompanied by a rough texture, making the affected areas feel like sandpaper.
Redness and inflammation
In addition to the small bumps, individuals with Keratosis Pilaris may experience redness and inflammation in the affected areas. This can give the skin a flushed appearance and cause discomfort. The severity of redness and inflammation can vary from person to person, with some individuals experiencing milder symptoms while others may have more pronounced redness and inflammation.
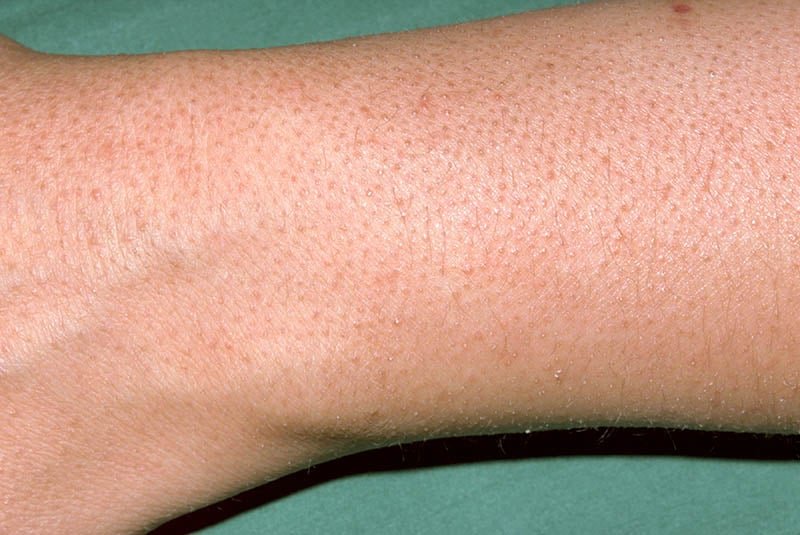
Rough and dry skin
Keratosis Pilaris often results in rough and dry skin in the affected areas. The excessive keratin buildup not only blocks the hair follicles but also disrupts the skin’s natural moisture balance. This can lead to dryness, flakiness, and an overall rough texture of the skin. It is important to note that dry skin can exacerbate the symptoms of Keratosis Pilaris, so proper hydration and moisturization are essential in managing this condition.
Itching and discomfort
Many individuals with Keratosis Pilaris experience itching and discomfort in the affected areas. The constant rubbing or scratching of the itchy skin can further irritate the skin and potentially lead to secondary infections. It is important to resist the urge to scratch the affected areas as much as possible to avoid further complications. Finding relief through proper treatment and skincare can alleviate the itching and discomfort associated with this condition.

Diagnosing Keratosis Pilaris
Physical examination
Diagnosing Keratosis Pilaris typically involves a physical examination by a dermatologist or healthcare professional. During the examination, the healthcare provider will closely examine the affected areas of your skin, looking for the characteristic small bumps, redness, and dryness associated with Keratosis Pilaris. They may also examine any other areas of concern to rule out similar skin conditions. In some cases, a magnifying device or dermoscope may be used to get a closer look at the affected skin.
Reviewing medical history
In addition to the physical examination, your healthcare provider will likely review your medical history to gain a better understanding of your symptoms and any potential underlying causes. They may ask questions about your family history of skin conditions, any medications you are currently taking, and any other relevant factors that could contribute to the development of Keratosis Pilaris. Providing accurate and detailed information about your medical history can aid in the accurate diagnosis and treatment of this condition.
Treatment Options for Keratosis Pilaris
Moisturizing the skin
Keeping the skin well-moisturized is one of the most important aspects of managing Keratosis Pilaris. Regularly applying a moisturizer or emollient can help hydrate the skin and alleviate dryness, roughness, and itching. Look for moisturizers that are fragrance-free and designed for sensitive skin. Applying moisturizer immediately after a bath or shower can also help lock in moisture and promote smoother skin.
Exfoliating the affected areas
Exfoliating the affected areas can help remove dead skin cells and unclog the hair follicles, reducing the appearance of bumps and roughness. However, it is important to exfoliate gently to avoid irritating the skin further. Use a mild exfoliating scrub or a soft washcloth and gently massage the affected areas in circular motions. Avoid scrubbing too vigorously, as this can cause more harm than good. Exfoliating once or twice a week can help improve the texture of your skin.
Topical creams and lotions
There are a variety of topical creams and lotions available over-the-counter that can help manage the symptoms of Keratosis Pilaris. These products often contain ingredients like alpha hydroxy acids (AHAs) or urea, which can help exfoliate the skin and improve its texture. It is important to follow the instructions on the product packaging and speak with your healthcare provider if you have any concerns or questions.
Prescription medications
In some cases, your healthcare provider may prescribe medications to help manage severe or persistent symptoms of Keratosis Pilaris. These medications may include topical corticosteroids to reduce inflammation, retinoids to promote skin cell turnover, or immunomodulators to reduce immune system responses. It is important to use these medications as directed and follow up with your healthcare provider regularly to monitor their effectiveness and any potential side effects.
Laser therapy
Laser therapy is a treatment option that can help reduce the appearance of Keratosis Pilaris. During this procedure, a laser is used to target the affected areas of the skin, breaking down the excess keratin and promoting healthy skin cell regeneration. Laser therapy can be an effective option for individuals who have not responded well to other treatments or who have severe and persistent symptoms. It is important to consult with a dermatologist to determine if laser therapy is suitable for you.
Light therapy
Light therapy, also known as phototherapy, involves exposing the affected areas of the skin to specific wavelengths of light. This treatment option can help reduce inflammation, promote skin cell turnover, and improve the overall appearance of the skin. Light therapy is often used in combination with other treatment modalities and typically requires multiple sessions for optimal results. Consulting with a dermatologist can help determine if light therapy is a viable option for managing your Keratosis Pilaris.
Natural Remedies for Keratosis Pilaris
Coconut oil
Coconut oil is a popular natural remedy often used to moisturize and hydrate the skin. Its high-fat content helps lock in moisture and soothe dryness. Apply a small amount of coconut oil directly to the affected areas, massaging it gently into the skin. Coconut oil can also be used in combination with other natural remedies or as a carrier oil for essential oils.
Apple cider vinegar
Apple cider vinegar has antiseptic and anti-inflammatory properties that can help reduce redness and inflammation associated with Keratosis Pilaris. Mix equal parts of apple cider vinegar and water and apply the solution to the affected areas using a cotton ball or washcloth. Allow it to sit for a few minutes before rinsing off with lukewarm water.
Gentle exfoliation with oatmeal
Oatmeal is a gentle exfoliant that can help remove dead skin cells and soothe irritated skin. Grind rolled oats into a fine powder and mix it with water to create a paste. Apply the paste to the affected areas and gently massage in circular motions. Rinse off with warm water and pat the skin dry.
Omega-3 fatty acids
Omega-3 fatty acids, found in foods such as fish, flaxseeds, and walnuts, have anti-inflammatory properties and can help improve the overall health of the skin. Incorporating these foods into your diet or taking omega-3 fatty acid supplements may help reduce inflammation and promote healthier skin.
Aloe vera
Aloe vera gel has soothing and hydrating properties that can alleviate dryness and irritation associated with Keratosis Pilaris. Apply pure aloe vera gel directly to the affected areas and massage it into the skin until fully absorbed. Repeat this process regularly to keep the skin moisturized and calm.
Preventing Keratosis Pilaris
Keep the skin moisturized
One of the key preventive measures for Keratosis Pilaris is maintaining adequate skin hydration. Using a moisturizer regularly can help prevent dryness and itching. Look for moisturizers that are fragrance-free and designed for sensitive skin. Applying moisturizer immediately after bathing or showering can help lock in moisture and promote healthier skin.
Avoid excessive hot water and harsh soaps
Hot water and harsh soaps can strip away the skin’s natural oils, leading to dryness and irritation. It is important to avoid using excessively hot water for bathing and to opt for lukewarm water instead. Similarly, choose gentle, fragrance-free soaps or cleansers that are specifically formulated for sensitive skin. Avoid scrubbing the affected areas too harshly, as this can worsen the condition.
Use gentle exfoliation techniques
Exfoliating the skin can help prevent the buildup of dead skin cells and keratin. However, it is important to exfoliate gently and avoid scrubbing too vigorously, as this can irritate the skin and potentially worsen the condition. Use a mild exfoliating scrub or a soft washcloth and gently massage the affected areas in circular motions. Exfoliating once or twice a week is generally sufficient to promote healthier skin.
Wear loose cotton clothing
Tight-fitting clothing can rub against the skin and potentially irritate the hair follicles, leading to increased symptoms of Keratosis Pilaris. Choosing loose, breathable clothing made from natural fibers like cotton can reduce friction and allow the skin to breathe. Avoid wearing rough or synthetic fabrics that may further irritate the skin.
Managing Keratosis Pilaris in Children
Gentle skincare routine
When managing Keratosis Pilaris in children, it is essential to establish a gentle skincare routine. Use mild cleansers and avoid scrubbing the affected areas too vigorously. Pat the skin dry instead of rubbing and apply a gentle moisturizer immediately after bathing. Regular skincare practices can help keep the skin moisturized and prevent further irritation.
Avoiding irritants
To prevent worsening of symptoms, it is important to identify and avoid potential irritants. This may include harsh soaps, fragranced skincare products, and rough fabrics. Opt for hypoallergenic, fragrance-free products specifically formulated for children’s sensitive skin. Choosing soft, cotton clothing can also minimize friction and reduce irritation.
Monitoring symptoms
Regularly monitoring and tracking your child’s symptoms can help you identify triggers and patterns that may exacerbate Keratosis Pilaris. Keep note of any changes in the appearance or severity of the bumps, redness, or itching. This information can be valuable when discussing treatment options with a healthcare provider.
Seeking medical advice
If your child’s symptoms persist or worsen despite at-home remedies and care, it is advisable to seek medical advice from a dermatologist. They can evaluate the severity of your child’s condition and recommend appropriate treatment options. It is essential not to self-diagnose or attempt aggressive treatments without professional guidance, especially when managing Keratosis Pilaris in children.
Keratosis Pilaris and Other Skin Conditions
Eczema
Keratosis Pilaris and eczema are two separate skin conditions, but they can occur concurrently or appear similar in some cases. Eczema, also known as atopic dermatitis, is a chronic inflammatory skin condition characterized by red, itchy, and often dry skin patches. While both conditions can result in redness and inflammation, distinguishing between them is important, as the treatment approaches may vary. Consulting with a dermatologist can help differentiate between Keratosis Pilaris and eczema and ensure proper management.
Folliculitis
Folliculitis is a skin condition characterized by the inflammation of hair follicles, often caused by bacteria, fungi, or other factors. Although it can sometimes resemble Keratosis Pilaris, folliculitis usually presents with red bumps that contain pus and can be accompanied by pain or tenderness. Diagnosis by a healthcare professional is crucial to differentiate between the two conditions and determine the appropriate treatment.
Psoriasis
Psoriasis is a chronic autoimmune skin condition characterized by the rapid buildup of skin cells, leading to the formation of red, scaly patches. While Keratosis Pilaris primarily affects the hair follicles, psoriasis can affect larger areas of the body. The appearance of psoriasis lesions may differ significantly from the small bumps associated with Keratosis Pilaris. Consultation with a dermatologist is essential for an accurate diagnosis and appropriate management.
Ichthyosis
Ichthyosis is a group of genetic skin disorders that primarily affect the skin’s outer layer, resulting in dry, scaly, and sometimes thickened skin. It can resemble certain aspects of Keratosis Pilaris, especially the rough and dry skin. However, the severity and extent of the symptoms can differ significantly between the two conditions. A dermatologist can perform a thorough evaluation to differentiate between Keratosis Pilaris and ichthyosis and recommend suitable treatment options.
Coping with the Emotional Impact of Keratosis Pilaris
Self-confidence and self-esteem
Living with Keratosis Pilaris can sometimes have a significant emotional impact on individuals. The visible bumps and redness can lead to feelings of self-consciousness and impact self-confidence and self-esteem. It is important to remember that Keratosis Pilaris is a common skin condition that affects many people and does not pose any serious health risks. Building self-confidence and focusing on one’s positive attributes can help manage the emotional impact of this condition.
Support systems
Seeking support from friends, family, or support groups can be incredibly beneficial for individuals with Keratosis Pilaris. Sharing experiences and finding solace in others who understand the challenges can provide a sense of belonging and alleviate feelings of isolation. Surrounding yourself with a supportive network can help boost self-esteem and provide encouragement during the journey of managing Keratosis Pilaris.
Educating others
Educating others about Keratosis Pilaris can help raise awareness and foster understanding. Many people are unaware of this condition and may misinterpret or judge individuals with visible symptoms. By educating friends, family, and the general public, you can promote empathy, dispel misconceptions, and contribute to a more inclusive and compassionate society.
When to See a Doctor
Persistent or worsening symptoms
If you have been managing Keratosis Pilaris with at-home remedies and lifestyle changes but notice persistent or worsening symptoms, it is advisable to consult with a healthcare professional. They can assess your condition, provide further guidance, and recommend additional treatment options if necessary. Remember, seeking medical advice is essential to ensure an accurate diagnosis and appropriate management.
Complications
Although Keratosis Pilaris is generally a harmless condition, complications can occur in rare cases. If you develop signs of infection, such as increased redness, warmth, pain, or discharge, it is crucial to seek medical attention promptly. Additionally, if you notice any severe discomfort, persistent itching, or other unusual symptoms, consulting with a healthcare professional is recommended to rule out potential complications and address your concerns.
Concerns about self-image
If you are experiencing significant emotional distress due to the impact of Keratosis Pilaris on your self-image and mental well-being, it is important to seek support. A dermatologist or mental health professional can provide guidance and resources to help you navigate the emotional challenges. They can offer coping strategies, therapy, or other interventions to improve your overall well-being and self-esteem. Remember, you do not have to face these challenges alone, and seeking help is a sign of strength.
In conclusion, understanding the causes, symptoms, and treatment options for Keratosis Pilaris can empower individuals to effectively manage their condition. While it may not be possible to completely cure Keratosis Pilaris, implementing a consistent skincare routine, utilizing various treatment options, and seeking medical advice as needed can significantly improve the appearance and alleviate associated symptoms. Remember, you are not alone in your journey, and with the right knowledge and support, you can navigate this common skin condition with confidence and grace.