Whether you’re a seasoned nurse or just starting out in your nursing career, you may encounter patients with amputations. Understanding the essential nursing considerations for these patients is crucial in providing comprehensive care and support. From assessing the patient’s physical and emotional needs to managing their pain and facilitating their rehabilitation, this article will guide you through the important aspects of nursing care for patients with amputation. So, grab a cup of coffee, get comfortable, and let’s dive into this rewarding field of nursing management!
Preoperative considerations

Physical assessment
During the preoperative phase, a comprehensive physical assessment is crucial to evaluate the patient’s overall health and identify any potential risks or complications. This assessment includes vital signs, baseline laboratory tests, and a thorough examination of the amputated limb. Assessing the anatomical condition of the residual limb, including any infections, ulcers, or deformities, helps determine the most appropriate surgical approach. Additionally, assessing the patient’s range of motion, strength, and sensation in the remaining limb aids in planning postoperative rehabilitation.
Psychosocial assessment
Understanding the psychosocial well-being of patients undergoing amputation is essential for their overall care and successful recovery. It involves evaluating their emotional state, coping mechanisms, support systems, and any preexisting psychological conditions. This assessment helps identify potential psychological barriers that may impede the patient’s adaptation to limb loss and guides the development of personalized coping strategies. By acknowledging and addressing the psychosocial impact of amputation, healthcare providers can empower patients to reach their full potential during the rehabilitation process.
Educating the patient and family
Patient education is a vital aspect of preparing individuals and their families for the challenges and changes they will face before and after amputation. It is crucial to explain the surgical procedure, potential complications, and the expected rehabilitation process in a clear and understandable manner. Providing information about pain management, assistive devices, and lifestyle modifications is essential for empowering the patient to actively participate in their recovery. Additionally, involving family members in educational sessions helps create a support network, enabling them to provide emotional support and practical assistance throughout the patient’s journey.
Preparing the patient for surgery
Preparing patients for amputation surgery involves several essential steps. These include obtaining informed consent, ensuring proper documentation, and conducting preoperative assessments and tests. It is crucial to administer medications as ordered, assess the patient’s nutritional status, and provide preoperative skin care to reduce the risk of infection. Preoperative teaching should address postoperative expectations, including wound care, pain management, and rehabilitation options. By adequately preparing patients for surgery, healthcare providers can promote a sense of control and reduce anxiety, ultimately leading to better surgical outcomes and overall patient satisfaction.
Postoperative care
Wound care
After amputation surgery, meticulous wound care is crucial to prevent infections and promote healing. Regular dressing changes, proper wound cleansing, and appropriate use of antimicrobial agents are vital components of wound management. Healthcare providers must closely monitor the wound for signs of infection, such as increased redness, swelling, discharge, or fever, and promptly address any concerns or complications that arise. By providing comprehensive wound care, nurses play a pivotal role in minimizing the risk of complications and supporting the patient’s recovery.
Pain management
Pain management is a vital aspect of postoperative care for individuals with amputations. Nurses play a key role in assessing pain levels, evaluating the effectiveness of pain relief interventions, and advocating for appropriate pain management strategies. This may include administering pain medications as prescribed, implementing non-pharmacological pain relief techniques, and educating the patient and their family about the importance of pain control. By addressing pain effectively, healthcare providers can improve the patient’s comfort, promote better sleep and overall well-being, and facilitate their engagement in rehabilitation activities.
Mobility and ambulation
Assisting patients with amputations in regaining mobility and achieving optimal ambulation is a fundamental aspect of their postoperative care. Nurses collaborate with physical therapists to develop individualized rehabilitation plans that focus on enhancing strength, balance, and coordination. This may involve therapeutic exercises, gait training, and the use of assistive devices such as crutches, canes, or prostheses. Regular monitoring of the patient’s progress and providing ongoing support and encouragement are essential for their successful ambulation and restoration of independence.

Assistive devices
Assistive devices play a significant role in facilitating the functional independence of individuals with amputations. Nurses collaborate with occupational therapists and prosthetists to assess the patient’s needs and provide appropriate assistive devices to enhance their daily living activities. This may include recommending assistive technologies such as grab bars, ramps, and modified utensils to improve self-care and mobility. Furthermore, nurses educate patients on the correct usage and maintenance of assistive devices, ensuring their safety and optimizing their benefits.
Phantom limb pain management
Phantom limb pain is a prevalent phenomenon among individuals who have undergone amputations. Nurses play a vital role in assessing and managing this type of pain, which is often described as sensations originating from the amputated limb. By offering psychosocial support, employing techniques such as mirror therapy, and utilizing pharmacological interventions when necessary, nurses contribute to the relief of phantom limb pain. By addressing this distressing symptom, healthcare providers can significantly improve the patient’s overall quality of life and facilitate their adaptation to limb loss.
Psychosocial support
Emotional support
Providing emotional support is crucial for patients with amputations, as they often experience a wide range of emotions throughout the rehabilitation process. Nurses can establish therapeutic relationships, actively listen, and validate the patient’s feelings and concerns. Offering empathetic and compassionate care helps alleviate anxiety, depression, and emotional distress. By fostering a supportive environment, nurses create a safe space where patients can openly discuss their emotions and develop healthy coping strategies.
Coping strategies
Assisting patients in developing effective coping strategies is essential to promote their psychological well-being and enhance their adaptation to limb loss. Nurses can offer guidance and teach coping techniques such as relaxation exercises, breathing techniques, and mindfulness exercises. Encouraging patients to engage in hobbies, participate in support groups, and seek counseling services can also provide valuable outlets for emotional expression. By equipping patients with coping strategies, healthcare providers empower them to navigate the emotional challenges associated with amputation more effectively.
Social engagement
Maintaining social engagement is crucial for individuals with amputations, as it can significantly influence their overall well-being and quality of life. Nurses can encourage patients to participate in social activities, community events, and support groups that cater specifically to individuals with limb loss. Facilitating connections with peers who have experienced similar challenges can foster a sense of belonging, reduce isolation, and promote the sharing of experiences and coping strategies. By promoting social engagement, nurses contribute to the patient’s psychosocial support network and enhance their emotional resilience.
Referral to counseling services
Recognizing the potential need for additional psychological support, nurses should proactively refer patients with amputations to counseling services. These services offer specialized support from mental health professionals who can help individuals navigate the emotional and psychological impact of limb loss. Counseling sessions may address issues such as grief, body image concerns, post-traumatic stress disorder, and adjustment difficulties. By advocating for and facilitating access to counseling services, nurses ensure that patients receive comprehensive care that addresses their unique psychosocial needs.
Promoting independence
Physical therapy
Physical therapy plays a crucial role in promoting independence and optimizing functional outcomes for individuals with amputations. Nurses collaborate with physical therapists to develop individualized rehabilitation plans that focus on restoring strength, flexibility, and balance. Through regular therapeutic exercises, gait training, and mobility assessments, physical therapists help patients regain their physical abilities and build confidence in their movements. Nurses support this process by facilitating access to physical therapy services, monitoring progress, and providing encouragement and reinforcement.

Occupational therapy
Occupational therapy aims to enhance the patient’s ability to engage in meaningful daily activities and regain independence. Nurses collaborate with occupational therapists to assess the patient’s self-care skills, identify areas of difficulty, and develop tailored strategies to improve functionality. Occupational therapists may provide training in activities of daily living, such as dressing, grooming, and cooking, using adaptive techniques and equipment as necessary. Nurses support the patient’s participation in occupational therapy sessions, reinforce the techniques learned, and assist with the procurement of adaptive devices to facilitate independent living.
Assistive technology
The use of assistive technology can greatly enhance the functional independence and quality of life for individuals with amputations. Nurses collaborate with assistive technology specialists to assess the patient’s needs and recommend appropriate devices. This may include prosthetics, wheelchairs, mobility aids, and communication devices. Nurses play a crucial role in educating patients about the capabilities and limitations of assistive technology, ensuring proper usage, and providing ongoing support and guidance. By incorporating assistive technology into the patient’s care plan, healthcare providers empower them to maximize their independence and live fulfilling lives.
Adaptive techniques for activities of daily living
Teaching adaptive techniques for activities of daily living is an essential aspect of promoting independence for patients with amputations. Nurses work closely with occupational therapists to assess the patient’s specific needs and develop customized strategies to overcome challenges in self-care, mobility, and home management tasks. These techniques may involve modifying routines, utilizing devices for one-handed tasks, or adopting alternative methods for completing daily activities. By providing comprehensive training and ongoing support, nurses empower patients to adapt to their new circumstances and regain autonomy in their daily lives.
Preventing complications
Infection prevention
Preventing infections is a top priority in the care of individuals with amputations. Nurses play a crucial role in promoting good hygiene practices, ensuring proper wound care, and monitoring the patient’s overall health status. This includes educating patients about proper hand hygiene, wound cleansing, and avoiding potential sources of infection. Nurses also assess for signs of infection, such as redness, swelling, increased pain, or fever, and promptly report any concerns to the healthcare team. By implementing strict infection prevention protocols, nurses significantly reduce the risk of complications and support optimal healing.
Contracture prevention
Contractures, or the permanent shortening of muscles and tendons, can occur following an amputation if proper precautions are not taken. Nurses collaborate with the interdisciplinary team to develop individualized plans for preventing contractures. This may include regular stretching exercises, positioning techniques, and the use of splints or orthotic devices. Close monitoring of the patient’s joint range of motion, regular skin assessments, and ongoing patient education regarding the importance of maintaining joint mobility are crucial to preventing contractures. By addressing contracture risk proactively, nurses contribute to the patient’s functional recovery and overall well-being.
Skin breakdown prevention
Skin breakdown can occur due to various factors, including prolonged pressure, friction, and moisture, particularly in individuals with amputations. Nurses are responsible for conducting regular skin assessments, particularly in areas prone to pressure ulcers, such as bony prominences. Implementing strategies to prevent skin breakdown, such as positioning, providing pressure-relieving devices, and encouraging regular movement, is essential. Nurses educate patients and caregivers about the importance of proper skin care, including cleansing, moisturizing, and avoiding irritants. By actively addressing the risk of skin breakdown, nurses foster optimal wound healing, reduce discomfort, and enhance the patient’s overall well-being.
Deep vein thrombosis prevention
Individuals with limb amputations may be at an increased risk of developing deep vein thrombosis (DVT). Nurses play a vital role in preventing DVT by implementing preventive measures, including early mobilization, compression stockings, and pharmacological interventions. It is crucial for nurses to educate patients about the signs and symptoms of DVT, such as leg swelling, pain, or redness, and encourage them to report any concerns promptly. Regular assessments to identify risk factors, such as immobility or a history of blood clotting disorders, are essential for implementing appropriate preventive measures. By proactively addressing DVT risk, nurses ensure the patient’s safety and well-being during the recovery period.
Patient education
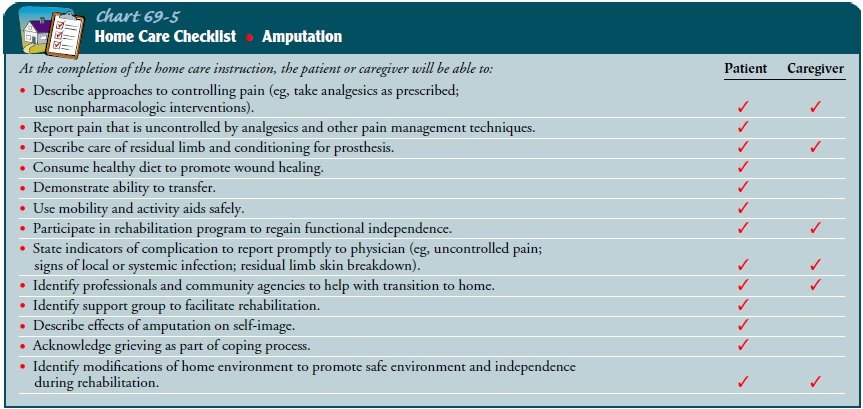
Prosthetic education
Educating patients about prosthetics plays a significant role in their post-amputation care and rehabilitation. Nurses collaborate with prosthetists to provide extensive education on the available options, the fitting process, maintenance requirements, and realistic expectations. By addressing questions and concerns relating to prosthetics, nurses facilitate the patient’s decision-making process and promote their active participation in their care. Additionally, nurses play a crucial role in teaching patients how to wear and use their prosthetic devices effectively, ensuring proper alignment and functional outcomes.
Self-care instructions
Teaching self-care instructions is essential for patients with amputations to promote independence and maintain overall health. Nurses educate patients on proper residual limb care, such as cleaning, drying, and moisturizing, to prevent skin irritation and infection. They also provide guidance on maintaining general hygiene, including bathing, oral care, and grooming. Additionally, nurses educate patients about wound care for any residual limb incisions or skin breakdowns, teaching them proper dressing changes and signs of infection. By equipping patients with self-care knowledge, healthcare providers empower them to actively participate in their own care.
Safety precautions
Ensuring safety is paramount for patients with amputations, particularly during the early stages of recovery. Nurses play a crucial role in educating patients about safety precautions to prevent falls, accidents, and injuries. This may include teaching proper crutch or cane use, recommending modifications to the home environment, and educating patients on strategies to maintain balance and stability. Recognizing potential hazards and addressing them proactively, such as removing tripping hazards or ensuring adequate lighting, helps create a safe living environment for patients. By prioritizing safety, nurses contribute to the patient’s overall well-being and minimize the risk of complications.
Signs of complications
Educating patients and their families about the signs of potential complications following amputation surgery is crucial in facilitating early intervention and preventing further harm. Nurses provide comprehensive instruction on recognizing and reporting signs of infection, such as increased pain, redness, swelling, or discharge from the wound. They also educate patients about signs of circulatory problems, skin breakdown, or changes in the residual limb, such as excessive heat or coldness, numbness, or discoloration. By providing clear information on potential complications and encouraging open communication, nurses empower patients to take an active role in their own healthcare.
Nutritional considerations
Balanced diet
Maintaining a balanced and nutritious diet is essential for individuals with amputations to support healing, promote overall health, and prevent complications. Nurses collaborate with dieticians to assess the patient’s nutritional needs and provide education on maintaining a well-rounded diet. Emphasizing the importance of adequate protein intake, as well as consuming a variety of fruits, vegetables, whole grains, and healthy fats, is crucial. Nurses also educate patients about portion control, the importance of hydration, and strategies to manage any dietary restrictions related to existing health conditions. By promoting a balanced diet, nurses support optimal wound healing and enhance the patient’s overall well-being.
Proper hydration
Ensuring proper hydration is vital for patients with amputations, as dehydration can hinder wound healing and affect organ function. Nurses educate patients about the importance of maintaining adequate fluid intake and teach strategies to monitor hydration levels. Encouraging the consumption of water, healthy beverages, and hydrating foods is essential. Nurses also educate patients on the signs and symptoms of dehydration, such as dry mouth, decreased urine output, or dizziness, and emphasize the need to seek prompt medical attention if these occur. By emphasizing proper hydration, nurses support the patient’s overall health and well-being.
Supplements
In some cases, patients with amputations may require nutritional supplementation to meet their specific needs during the recovery process. Nurses collaborate with dieticians and healthcare providers to assess the patient’s nutritional status and determine if any supplements are necessary. This may include protein supplements to support wound healing and muscle recovery or specific micronutrient supplements to address deficiencies. Nurses play a vital role in educating patients on the proper use and potential side effects of supplements, ensuring adherence to the recommended dosage, and monitoring their effectiveness.

Weight management
Maintaining a healthy weight is essential for individuals with amputations to reduce the risk of cardiovascular diseases, diabetes, and other health complications. Nurses collaborate with dieticians to assess the patient’s weight status, develop personalized weight management plans, and provide ongoing support and education. This may involve establishing realistic weight loss or weight maintenance goals, promoting regular physical activity, and encouraging healthy eating habits. Nurses also address any psychological factors that may impact weight management, such as body image concerns or emotional eating. By assisting patients in managing their weight, nurses contribute to their overall health and well-being.
Palliative care
End-of-life discussions
In situations where amputation is part of palliative care, nurses play a vital role in facilitating end-of-life discussions. These conversations address the patient’s goals, preferences, and wishes for their care as their health declines. Nurses provide a supportive and empathetic environment, encouraging open communication and offering emotional support to both the patient and their family. By engaging in end-of-life discussions, nurses ensure that the patient’s wishes are respected and that their care is aligned with their values and beliefs.
Symptom management
Managing symptoms effectively is a crucial aspect of palliative care for patients with amputations. Nurses collaborate with the interdisciplinary team to assess and manage symptoms such as pain, dyspnea, nausea, or anxiety. This may involve the administration of appropriate medications, implementing non-pharmacological interventions, providing emotional support, and facilitating access to any necessary support services. Close monitoring and ongoing assessment of symptoms are essential to ensure that the patient’s comfort is prioritized and that their overall quality of life is optimized.
Comfort measures
Providing comfort measures is a central component of palliative care for individuals with amputations. Nurses focus on alleviating physical discomfort, minimizing pain, and promoting a sense of peace and well-being. This may include positioning techniques, gentle touch, the application of cold or warm compresses, and providing a calm and soothing environment. Nurses also work closely with the patient’s family, ensuring they understand and can actively participate in providing comfort measures. By prioritizing comfort, nurses ensure that patients experience a sense of dignity and respect during this vulnerable stage of their lives.
Psychological support
Psychological support is an integral part of palliative care for patients with amputations and their families. Nurses provide continuous emotional support, actively listening to the patient’s concerns, and offering empathetic presence. Supporting the patient’s psychological well-being may involve encouraging them to express their emotions, referring them to counseling services, facilitating communication with loved ones, and providing education and reassurance. By acknowledging the unique emotional challenges associated with end-of-life care, nurses help patients and their families navigate this difficult journey with compassion and understanding.
Collaboration with interdisciplinary team
Surgeons
Collaborating with surgeons is essential in providing comprehensive care for patients with amputations. Nurses work closely with surgeons to ensure effective communication, accurate documentation, and collaboration throughout the preoperative and postoperative phases. This collaboration includes sharing vital patient information, participating in interdisciplinary rounds, and addressing any concerns or complications that arise. By facilitating effective teamwork, nurses contribute to the patient’s seamless care and optimal surgical outcomes.
Physical therapists
Collaboration with physical therapists is vital in promoting the functional recovery and mobility of individuals with amputations. Nurses collaborate with physical therapists to develop individualized rehabilitation plans, set achievable goals, and monitor the patient’s progress. Clear and open communication between the nursing and physical therapy teams allows for a holistic approach to be taken towards the patient’s care. By working together, nurses and physical therapists optimize the patient’s rehabilitation journey and support their independence.
Occupational therapists
Collaboration with occupational therapists is crucial in enabling patients with amputations to regain independence in their activities of daily living. Nurses work closely with occupational therapists to assess the patient’s needs, develop personalized care plans, and provide ongoing support and education. Collaboration also involves monitoring the patient’s progress, addressing any challenges or barriers, and ensuring continuity of care. By working as a team, nurses and occupational therapists empower patients to overcome functional limitations and enhance their quality of life.
Prosthetists
Collaboration with prosthetists is essential in providing individuals with amputations with the appropriate prosthetic devices and assistive technologies. Nurses collaborate with prosthetists to assess the patient’s needs, educate them about prosthetic options, and facilitate the fitting process. This collaboration ensures that the patient receives a prosthetic device that is tailored to their specific requirements and goals. Nurses also play a crucial role in educating patients on the proper use and maintenance of prosthetics, addressing any concerns or difficulties that may arise. By partnering with prosthetists, nurses contribute to the patient’s successful prosthetic rehabilitation and overall well-being.
Advocacy and ethical considerations
Patient rights
Advocating for and upholding patient rights is a fundamental responsibility of healthcare providers caring for individuals with amputations. Nurses ensure that patients are treated with dignity, respect, and autonomy throughout their healthcare journey. This includes respecting their right to informed consent, privacy, confidentiality, and participation in decision-making. Nurses also advocate for patients’ access to appropriate care, support services, and resources. By advocating for patient rights, nurses foster a patient-centered approach to care and uphold the principles of ethical practice.
Dignity and respect
Treating patients with dignity and respect is an essential aspect of nursing care for individuals with amputations. Nurses strive to create a supportive environment that recognizes and values the uniqueness of each patient. This involves using appropriate language and terminology, preserving privacy and confidentiality, and actively listening to the patient’s concerns and preferences. Nurses create a culture of respect by involving the patient in their plan of care, seeking their input, and acknowledging their expertise in their own lives. By promoting dignity and respect, nurses enhance the patient’s overall experience and contribute to their emotional well-being.
Ethical decision-making
Ethical decision-making plays a crucial role in the care of patients with amputations. Nurses encounter ethical dilemmas that require careful consideration and adherence to ethical principles. This may include decisions regarding pain management, end-of-life care, consent, or resource allocation. Nurses collaborate with the interdisciplinary team, engage in reflective discussions, and consult ethical frameworks or policies to guide their decision-making process. By approaching ethical dilemmas with integrity and critical thinking, nurses ensure that the patient’s best interests and ethical principles are upheld.
Advance directives
Advance directives are legally binding documents that outline an individual’s healthcare preferences in the event that they are unable to communicate or make decisions for themselves. Nurses play a vital role in promoting advance care planning for patients with amputations, ensuring that their wishes are respected and followed. Educating patients and their families about the importance of advance directives, assisting with the completion of documents, and ensuring their accurate documentation in the patient’s medical record are essential nursing responsibilities. By facilitating advance care planning, nurses support patient autonomy and promote a patient-centered approach to care.
In conclusion, providing comprehensive care for patients with amputations encompasses various considerations across the preoperative and postoperative phases. From assessing physical and psychosocial needs to implementing preventive measures and promoting independence, nurses play a crucial role in each aspect of care. By collaborating with the interdisciplinary team, advocating for patient rights, and addressing ethical considerations, nurses ensure that individuals with amputations receive holistic and compassionate care throughout their healthcare journey.