Imagine you’re a nurse, caring for patients with bone spurs. You understand the importance of providing comprehensive and thoughtful nursing care to alleviate their discomfort and promote their overall well-being. This article will guide you through the essential nursing considerations and management strategies for bone spurs, enabling you to enhance your patients’ quality of life and ensure their speedy recovery. From assessment and pain management to preventive measures and patient education, you’ll learn valuable insights to optimize your nursing care for individuals dealing with bone spurs. So, let’s dive into the world of nursing approaches specifically tailored for bone spur patients!

Understanding Bone Spurs
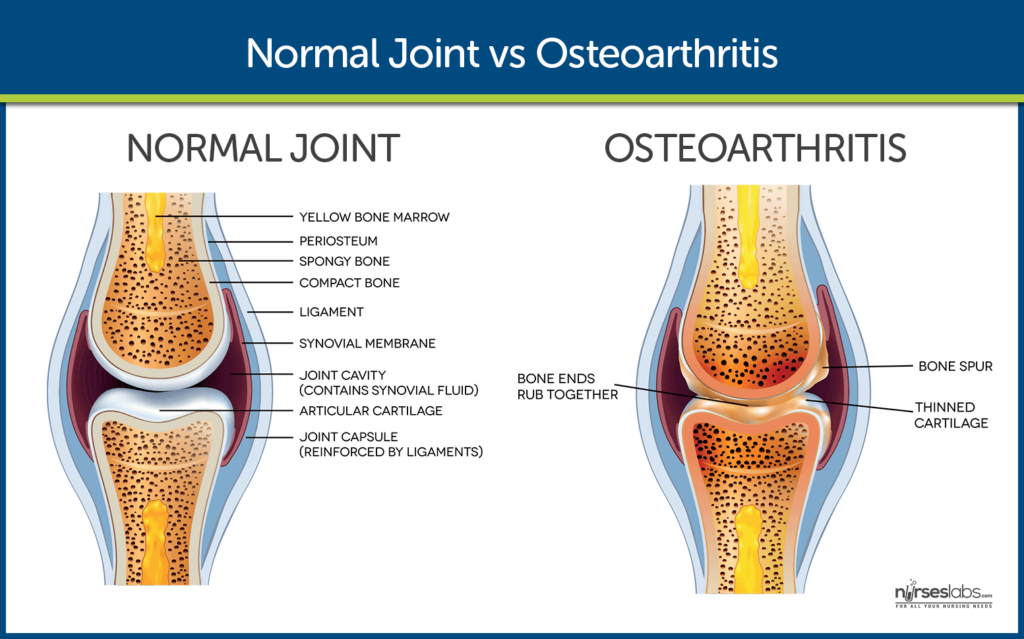
Bone spurs, also known as osteophytes, are bony growths that develop on the edges of existing bones. They often occur in joints where there is excessive friction or pressure, such as the spine, shoulders, knees, and hips. These bone spurs can vary in size and shape, and they typically develop over a long period of time. While some individuals may never experience symptoms from bone spurs, others may experience pain, limited range of motion, and joint stiffness. It is important to understand the causes, risk factors, and common locations of bone spurs in order to provide appropriate care and support to individuals affected by this condition.
Causes of Bone Spurs
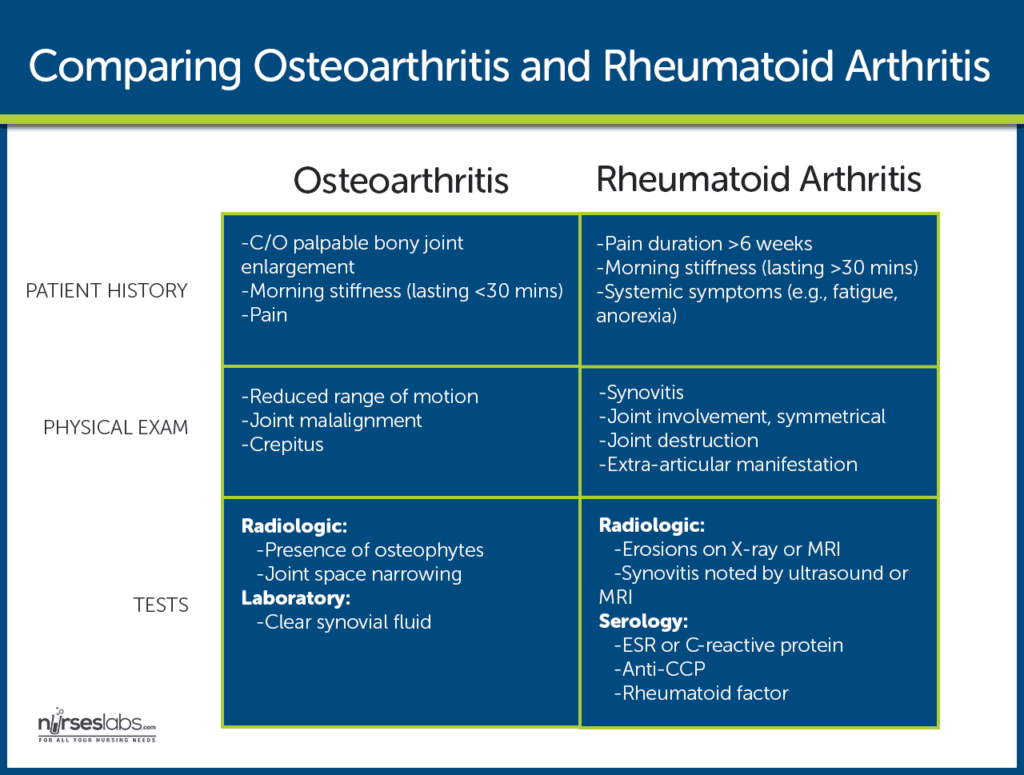
Bone spurs can develop due to a variety of factors. One common cause is the natural aging process. As we age, the cartilage that cushions our joints can break down, leading to bone-on-bone contact. This increased friction can prompt the body to develop bone spurs as a protective mechanism. Additionally, injuries or trauma to the joints can stimulate the growth of bone spurs. This can include repetitive stress injuries, such as those experienced by athletes or individuals with physically demanding occupations. Other contributing factors may include poor posture, obesity, genetic predisposition, and certain medical conditions like osteoarthritis and rheumatoid arthritis.
Risk Factors for Bone Spurs
While bone spurs can affect anyone, certain factors can increase the likelihood of their development. Advanced age is a significant risk factor, as the natural wear and tear on joints over time can contribute to the formation of bone spurs. Additionally, individuals who frequently engage in physical activities that place stress on the joints, such as running or weightlifting, may be at an increased risk. Obesity is another risk factor, as excess weight can place increased pressure on the joints and lead to cartilage deterioration. Those with a family history of bone spurs may also be genetically predisposed to developing them.
Common Locations of Bone Spurs
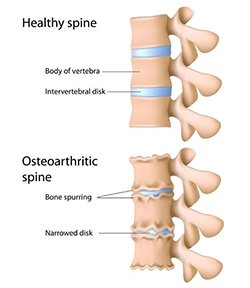
Bone spurs can develop in various locations throughout the body, but there are certain areas that are more commonly affected. In the spine, bone spurs can occur in the neck (cervical spine) or lower back (lumbar spine), potentially leading to spinal stenosis or nerve compression. The shoulders are also a common location for bone spurs, particularly in individuals who frequently perform overhead activities or have experienced shoulder injuries. Other common locations include the hands and fingers, knees, and hips. It is important for healthcare providers to be aware of the typical locations of bone spurs in order to accurately assess and diagnose patients.
Signs and Symptoms
While some individuals with bone spurs may be asymptomatic, others may experience a variety of signs and symptoms. The severity and type of symptoms can vary depending on the location and size of the bone spurs.
Pain and Discomfort
Pain is one of the most common symptoms associated with bone spurs. It can be sharp or dull and may worsen with movement or pressure on the affected area. The pain may also radiate to nearby areas, such as shoulders or hips. Discomfort can vary from mild to severe, and it may impact daily activities and quality of life.
Limited Range of Motion
Bone spurs can restrict the movement of affected joints, leading to a limited range of motion. This can make it difficult to perform tasks that require bending, reaching, or lifting. Individuals may notice joint stiffness and find it challenging to fully extend or flex the affected joints.
Joint Stiffness
Stiffness in the joints is a common symptom of bone spurs. This stiffness may be particularly noticeable in the morning or after periods of inactivity. It can make it challenging to initiate movement and may improve with gentle stretching or movement.
Swelling and Inflammation
Inflammation and swelling may occur in the area surrounding the bone spurs. This can cause discomfort and contribute to joint stiffness. The affected area may also feel warm to the touch and appear red or swollen.
Diagnostic Process
Diagnosing bone spurs typically involves a combination of physical examination, imaging studies, and laboratory tests. Healthcare providers will assess the individual’s symptoms, medical history, and conduct a physical examination to determine the most appropriate diagnostic approach.
Physical Examination
During a physical examination, healthcare providers will closely examine the affected joints, looking for signs of swelling, tenderness, or limited range of motion. They may also perform specific maneuvers to assess joint stability and function.
Imaging Studies
Imaging studies, such as X-rays, can help visualize the presence of bone spurs. X-rays can provide detailed images of the bones and joints, revealing any abnormalities or distinctive features associated with bone spurs. In some cases, additional imaging studies, such as magnetic resonance imaging (MRI) or computed tomography (CT) scans, may be ordered to provide a more comprehensive view.
Laboratory Tests
While laboratory tests cannot directly diagnose bone spurs, they can help rule out other potential causes of symptoms. Blood tests may be ordered to assess for signs of inflammation or abnormal levels of certain markers. These tests can help healthcare providers make an accurate diagnosis and develop an appropriate treatment plan.
Nursing Assessment
Nurses play a crucial role in assessing and caring for individuals with bone spurs. A comprehensive nursing assessment involves gathering a detailed history, conducting a pain assessment, performing a physical examination, and assessing functional limitations.
History Taking
Obtaining a thorough history is essential in understanding an individual’s symptoms, potential risk factors, and impact of bone spurs on their daily life. Nurses should inquire about the onset and duration of symptoms, any previous injuries or surgeries, family history of bone spurs, and the individual’s occupation and physical activity level. This information can help guide nursing interventions and provide insight into potential areas of concern.
Pain Assessment
Pain assessment is crucial in understanding the individual’s experience and tailoring appropriate pain management strategies. Nurses should utilize standardized pain scales and ask specific questions to determine the intensity, location, and quality of the pain. They should also assess the individual’s response to previous pain management interventions and any factors that exacerbate or alleviate the pain.
Physical Examination
A physical examination allows nurses to assess the affected joints and surrounding areas, looking for signs of swelling, tenderness, or limitation in range of motion. Palpation can help identify the presence of bone spurs and assess for any complications, such as joint instability or muscle weakness. Nurses should also observe the individual’s gait and overall posture.
Assessing Functional Limitations
Assessing functional limitations ensures that nurses have a comprehensive understanding of the impact of bone spurs on the individual’s daily activities and quality of life. Nurses should inquire about any difficulties in carrying out routine tasks, such as dressing, bathing, or household chores. They should also assess the individual’s ability to perform work-related activities and participate in leisure or recreational activities. This information will guide nursing interventions aimed at maintaining or improving functional independence.
Collaborative Care
Collaborative care involves a multidisciplinary approach to managing bone spurs. Healthcare providers, including nurses, physicians, physical therapists, and orthopedic specialists, work together to develop an individualized treatment plan tailored to the needs of the patient.
Medical Management
Medical management of bone spurs may include various interventions, such as anti-inflammatory medications, corticosteroid injections, and joint mobilization techniques. In some cases, surgical intervention may be necessary to remove the bone spurs or address any associated complications.
Pharmacological Interventions
Pharmacological interventions focus on managing pain and reducing inflammation associated with bone spurs. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, may be prescribed to alleviate pain and discomfort. In more severe cases, stronger pain medications, such as opioids, may be prescribed for short-term pain management.
Non-Pharmacological Interventions
Non-pharmacological interventions are an important aspect of bone spur management, as they can help improve function and alleviate symptoms. Physical therapy, including exercises to improve range of motion and strengthen the surrounding muscles, may be recommended. Heat or cold therapy, such as application of ice or heat packs, can also provide temporary relief of symptoms. Assistive devices, such as braces or crutches, may be used to support the affected joints and relieve pressure.
Orthopedic Interventions
Orthopedic interventions, such as arthroscopy or joint replacement surgery, may be considered in severe cases of bone spurs. These surgical procedures aim to remove the bone spurs, repair damaged cartilage, and restore joint function. Orthopedic specialists collaborate with nurses to ensure appropriate preoperative and postoperative care for individuals undergoing these interventions.

Nursing Interventions
Nurses play a vital role in managing the care of individuals with bone spurs. Nursing interventions focus on pain management, assisting with mobility, providing education and psychosocial support, and monitoring for complications.
Pain Management
Effective pain management is crucial in supporting individuals with bone spurs. Nurses should collaborate with healthcare providers to develop a tailored pain management plan that includes pharmacological and non-pharmacological interventions. This may involve administering prescribed medications, implementing heat or cold therapy, teaching relaxation techniques, and facilitating physical therapy sessions.
Assisting with Mobility
Bone spurs can significantly impact an individual’s mobility and independence. Nurses should assist individuals in maintaining optimal mobility by promoting safe movement techniques and providing assistance when needed. This may include teaching proper body mechanics, helping with transfers and ambulation, and recommending the use of assistive devices, such as canes or walkers.
Providing Education and Psychosocial Support
Educating individuals about their condition and providing psychosocial support can help alleviate anxiety and promote self-management. Nurses should explain the nature of bone spurs, discuss treatment options, and provide information on self-care strategies. They should also address any emotional or psychosocial concerns, encouraging open communication and connecting individuals to support resources if needed.
Monitoring Complications
While complications from bone spurs are rare, nurses should remain vigilant in monitoring for any signs of infection, nerve compression, or other complications. Regular assessments of the affected joints, vital signs, and laboratory values can help detect any changes or abnormalities. Nurses should also educate individuals on potential warning signs to look out for and when to seek immediate medical attention.
Patient Education
Patient education plays a crucial role in promoting self-management and empowering individuals with bone spurs to actively participate in their care. Nurses should provide comprehensive education on various aspects of bone spurs, including understanding the condition, self-management strategies, home care instructions, and when to seek medical help.
Understanding Bone Spurs
Nurses should explain the anatomy of bone spurs, their causes, and the potential impact on joint function. They should provide information on the signs and symptoms of bone spurs, emphasizing the individual’s unique experiences and risks.
Self-Management Strategies
Educating individuals about self-management strategies can help them better cope with the challenges of living with bone spurs. Nurses should provide information on lifestyle modifications, such as maintaining a healthy weight, engaging in regular physical activity, and practicing proper body mechanics to minimize stress on the affected joints.
Home Care Instructions
Nurses should provide clear and concise home care instructions to individuals with bone spurs. This may include recommendations for pain management techniques, guidelines for using assistive devices, and instructions for applying heat or cold therapy. Nurses should ensure that individuals understand the importance of following their prescribed medications and attending follow-up appointments.
When to Seek Medical Help
Nurses should educate individuals on the potential complications associated with bone spurs and provide clear guidelines on when to seek immediate medical help. This may include signs of infection (such as fever or increased redness and swelling), severe pain or limitation in range of motion, or any new or worsening symptoms.
Prevention Strategies
While it may not be possible to prevent the development of bone spurs entirely, certain strategies can help reduce the risk and minimize the impact of the condition. Nurses should educate individuals on various preventive measures and encourage the adoption of healthy lifestyle choices.
Healthy Lifestyle Choices
Maintaining a healthy lifestyle can contribute to overall joint health and reduce the risk of developing bone spurs. Nurses should emphasize the importance of a balanced diet, rich in nutrients that support bone health, such as calcium and vitamin D. Smoking cessation and limiting alcohol consumption are also essential for maintaining optimal joint function.
Regular Physical Activity
Regular physical activity, including both weight-bearing and non-weight-bearing exercises, can help strengthen the muscles surrounding the joints and improve overall joint stability. Nurses should work with individuals to develop individualized exercise plans suited to their abilities and preferences.
Proper Body Mechanics
Practicing proper body mechanics is essential in preventing excessive strain on the joints and reducing the risk of developing bone spurs. Nurses should educate individuals on proper posture, lifting techniques, and ergonomics, particularly for individuals with physically demanding occupations or those who frequently engage in repetitive activities.
Maintaining Optimal Weight
Maintaining a healthy weight is crucial in minimizing joint stress and reducing the risk of developing bone spurs. Nurses should provide information on healthy eating habits, portion control, and the benefits of regular physical activity in weight management.
Patient Safety
Ensuring patient safety is of utmost importance, particularly for individuals with bone spurs who may experience limitations in mobility and increased risk of falls or other accidents. Nurses should assess the individual’s home environment and provide recommendations for promoting safety and preventing injuries.
Fall Prevention
Falls can significantly impact individuals with bone spurs and may lead to further injury or complications. Nurses should conduct a thorough fall risk assessment and implement interventions aimed at preventing falls. This may include removing tripping hazards, improving lighting, and educating individuals on safe movement techniques and the appropriate use of assistive devices.
Assistive Devices
Assistive devices, such as canes, walkers, or braces, can provide support and stability for individuals with bone spurs. Nurses should assess the individual’s needs and ensure proper fitting and education on how to use these devices safely and effectively.
Environmental Modifications
Modifying the home environment can help minimize fall risks and promote overall safety. Nurses should assess the individual’s living space and make recommendations for modifications, such as adding grab bars in the bathroom, installing handrails on stairs, or removing loose rugs.
Home Safety Assessment
A comprehensive home safety assessment can help identify potential hazards and promote a safe living environment. Nurses should evaluate factors such as lighting, flooring, accessibility of commonly used items, and the presence of assistive devices. This assessment can guide interventions aimed at optimizing patient safety.
Promoting Long-Term Outcomes
Promoting long-term outcomes involves ongoing assessment, monitoring, and collaboration among healthcare providers. Nurses play a crucial role in supporting individuals with bone spurs and ensuring continuity of care throughout their treatment journey.
Encouraging Adherence to Treatment Plan
Nurses should educate individuals on the importance of adhering to their treatment plan, including prescribed medications, recommended exercises, and follow-up appointments. By explaining the rationale behind each aspect of the plan, nurses can motivate individuals to actively participate in their care and maintain consistency in their self-management strategies.
Monitoring Progress and Adjusting Care
Regular monitoring of an individual’s progress is vital in determining the effectiveness of interventions and adjusting care as needed. Nurses should assess pain levels, range of motion, functional limitations, and overall well-being during follow-up visits. This information can be used to guide modifications to the treatment plan and ensure the individual’s ongoing needs are met.
Multidisciplinary Collaboration
Bone spurs often require a collaborative approach involving various healthcare providers. Nurses should facilitate effective communication and collaboration among team members, ensuring that everyone involved is aware of the individual’s goals, progress, and potential challenges. This multidisciplinary approach can optimize care and improve outcomes for individuals with bone spurs.
Supporting Self-Efficacy
Promoting self-efficacy is essential in empowering individuals with bone spurs to actively engage in their care and make informed decisions. Nurses should provide ongoing education, emotional support, and resources to help individuals navigate the challenges associated with living with bone spurs. By fostering self-efficacy, nurses can encourage individuals to take an active role in managing their condition and strive for the best possible outcomes.
In conclusion, bone spurs can significantly impact an individual’s quality of life and mobility. Nurses play a crucial role in providing comprehensive care, from assessing and managing symptoms to educating individuals on self-management strategies and promoting long-term outcomes. By understanding the causes, risk factors, and common locations of bone spurs, healthcare providers can provide high-quality care and support to individuals affected by this condition. Through collaborative care, nursing interventions, patient education, and preventive measures, individuals with bone spurs can be empowered to effectively manage their condition and improve their overall well-being.