You’re in good hands with this article as it covers the best nursing considerations for ear infections. Whether you’re a nurse or simply interested in learning more about ear infection management, this article has got you covered. From understanding the causes and symptoms to exploring the most effective treatment options, you’ll find everything you need to know to provide optimal care for patients with ear infections. So, sit back, relax, and let’s dive into the world of ear infection nursing considerations.
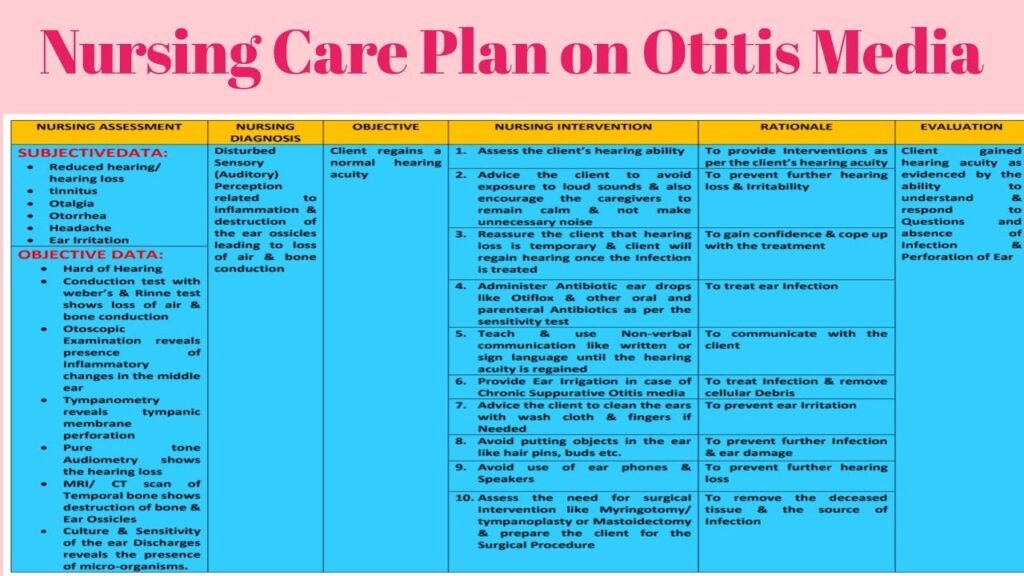
Assessment of the Patient
Collecting patient history
When assessing a patient with an ear infection, collecting a comprehensive patient history is essential. This includes asking the patient about their current symptoms, such as pain, hearing loss, and discharge from the ear. It is important to inquire about any previous ear infections, allergies, or other medical conditions that could impact the management and treatment of the infection. Additionally, gathering information about the patient’s lifestyle and potential exposures to common risk factors for ear infections, such as frequent swimming or exposure to secondhand smoke, can provide insight into the underlying cause.
Performing a physical examination
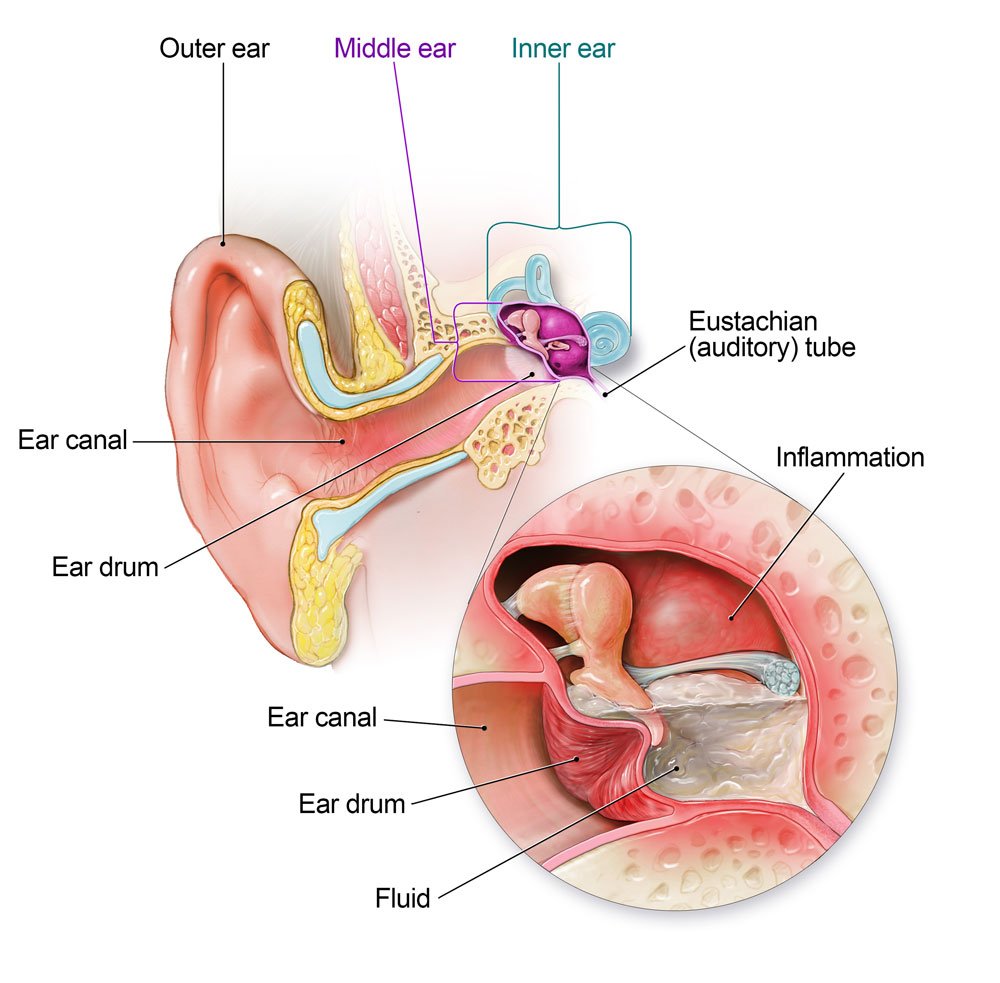
To accurately assess an ear infection, a physical examination of the ear is necessary. This involves visual inspection of the external ear and the ear canal using an otoscope. The nurse should carefully examine the ear for any redness, swelling, or drainage. It is also crucial to observe the eardrum for signs of infection, such as bulging, perforation, or fluid accumulation. Assessing the surrounding lymph nodes for tenderness or swelling can provide further information about the severity and spread of the infection.
Assessing vital signs
As part of the overall assessment, monitoring vital signs is crucial to identify any systemic signs of infection or complications. Assessing the patient’s temperature, heart rate, respiratory rate, and blood pressure can help identify if the infection has spread or if there are any signs of systemic inflammation. Elevated temperatures and increased heart rates may be early indicators of more severe infections or the presence of complications.
Obtaining a sample for laboratory testing
In cases where the diagnosis of an ear infection is uncertain, or if the infection is recurrent or severe, obtaining a sample for laboratory testing may be necessary. This usually involves taking a swab of the discharge from the ear and sending it to the laboratory for further analysis. The results can help identify the specific pathogen causing the infection and guide appropriate treatment decisions. Collecting a sample also allows for testing the antibiotic sensitivity of the bacteria, assisting in selecting the most effective medication for treatment. This step is especially important in cases where the infection is not responding to initial treatment or if unusual pathogens are suspected.
Management of Pain
Assessing pain levels
Pain is a common symptom experienced by patients with ear infections, and addressing and managing this pain is crucial for their comfort and well-being. To effectively manage pain, it is essential to assess the patient’s pain levels regularly. The nurse should use appropriate pain assessment tools, such as numerical rating scales or visual analog scales, to determine the intensity of the pain. By regularly assessing pain levels, nurses can tailor pain management interventions to meet the patient’s needs and ensure they are as comfortable as possible.
Administering analgesics
Once pain levels have been assessed, appropriate analgesics can be administered to provide relief. Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used to alleviate pain associated with ear infections due to their anti-inflammatory and analgesic properties. Acetaminophen, if tolerated by the patient, can also be used for pain management. For severe pain, healthcare providers may prescribe opioid analgesics. It is important for nurses to closely monitor the patient’s response to analgesics and adjust the dosage or medication as necessary to ensure adequate pain relief.
Providing comfort measures
In addition to pharmacological pain management, providing comfort measures can enhance the patient’s overall well-being and promote healing. Simple interventions such as applying warm compresses to the affected ear or using a heating pad on a low setting can help alleviate pain and reduce inflammation. Encouraging the patient to rest in a comfortable position and providing a calm and quiet environment can also contribute to their comfort. Lastly, offering distractions such as listening to music or engaging in calming activities can help redirect the patient’s attention away from any discomfort they may be experiencing.
Preventing Complications
Monitoring for signs of complications
Ear infections can sometimes lead to complications, especially if left untreated or unsuccessfully treated. It is crucial for nurses to closely monitor patients for any signs of worsening symptoms or the development of complications. Some common signs to watch for include persistent or severe pain, high fever, worsening hearing loss, dizziness or balance problems, facial weakness, or drainage of pus from the ear. These symptoms may indicate the spread of infection or the involvement of adjacent structures, such as the mastoid bone or inner ear. Recognizing these signs early on allows for prompt intervention and prevention of further complications.
Educating the patient about potential complications
In addition to closely monitoring patients for signs of complications, nurses play a vital role in educating patients about the potential complications of ear infections. This includes explaining how untreated or poorly managed infections can lead to more severe infections, such as mastoiditis or meningitis. Nurses should emphasize the importance of adhering to the prescribed treatment plan and seeking medical attention promptly if symptoms worsen or new symptoms develop. Educating patients about potential complications empowers them to take an active role in their own healthcare and can contribute to better outcomes.
Following the prescribed treatment plan
To prevent complications and promote healing, it is essential for patients to follow the prescribed treatment plan. Nurses play a crucial role in ensuring patients understand the importance of adhering to medication regimens, completing the full course of antibiotics, and attending follow-up appointments. Reinforcing the importance of proper medication administration, including timing and dosage, can help prevent antibiotic resistance and ensure optimal treatment outcomes. Furthermore, providing written instructions and clear explanations can assist patients and their families in accurately following the treatment plan and achieving the best possible outcomes.
Maintaining Ear Hygiene
Teaching proper ear hygiene
To maintain ear health and prevent recurrent infections, teaching patients proper ear hygiene is essential. Nurses should educate patients on the importance of gently cleaning the ears and avoiding excessive or aggressive cleaning, as this can disrupt the natural ear canal environment and increase the risk of infection. Patients should be instructed to use mild soap and warm water to clean the outer portion of their ears, avoiding inserting anything into the ear canal. Stressing the importance of maintaining regular hygiene practices, such as washing hands thoroughly before touching the ears, can also help prevent the introduction of bacteria into the ear.
Instructing on ear care after infection resolution
After an ear infection has resolved, it is important to provide patients with instructions for ongoing ear care. This includes emphasizing the importance of maintaining good ear hygiene, avoiding prolonged exposure to water (such as swimming or bathing), and promptly drying the ears after any exposure to moisture. Patients should also be educated on how to recognize early signs of infection recurrence and when to seek medical attention. By empowering patients with knowledge and instructions for post-infection ear care, nurses can help prevent future infections and promote long-term ear health.
Promoting clean environments
In addition to proper personal ear hygiene, promoting clean environments can contribute to preventing ear infections. Nurses should educate patients and families about the importance of maintaining clean and hygienic living spaces. This includes regularly cleaning and disinfecting surfaces, especially those frequently touched, such as doorknobs, light switches, and electronic devices. Encouraging proper hand hygiene practices, such as regular handwashing or using hand sanitizers, can also help prevent the spread of bacteria and viruses that may contribute to ear infections. By promoting clean environments, nurses can play a crucial role in minimizing the risk of infection and promoting overall well-being.

Administering Medications
Understanding different types of ear infection medications
When it comes to treating ear infections, various types of medications may be prescribed depending on the severity and type of infection. It is essential for nurses to have a comprehensive understanding of these medications to ensure safe and effective administration. The most commonly prescribed medications include antibiotics to target bacterial infections, analgesics for pain relief, and occasionally corticosteroids to reduce inflammation. Nurses should be familiar with different antibiotics commonly used for ear infections, such as amoxicillin, ceftriaxone, or azithromycin. Understanding the mechanism of action, common side effects, and potential drug interactions of these medications is crucial to provide appropriate patient education and monitoring.
Administering antibiotics
Antibiotics are frequently prescribed for bacterial ear infections, and it is important for nurses to understand the proper administration techniques. Oral antibiotics are commonly used for the treatment of ear infections and can be administered with or without food, depending on the specific medication. Nurses should ensure that patients understand the importance of taking the full prescribed course of antibiotics, even if symptoms improve. This helps prevent antibiotic resistance and ensures the complete eradication of the infection. In some cases, healthcare providers may administer intramuscular or intravenous antibiotics for severe or persistent infections. Nurses involved in these routes of administration should adhere to proper aseptic techniques and closely monitor patients for any adverse reactions.
Educating the patient about medication usage
Patient education plays a critical role in the effective management of ear infections. Nurses should provide comprehensive information to patients and their families about the prescribed medications. This includes explaining the purpose of each medication, how to take it correctly, and any potential side effects to watch for. It is essential to emphasize the importance of completing the full course of antibiotics and reporting any concerns or adverse reactions promptly. Clear communication and appropriate education ensure that patients are actively engaged in their treatment and can make informed decisions about their health.
Promoting Effective Communication
Explaining the infection and treatment to the patient
Clear and effective communication is key to promoting patient understanding and compliance with the treatment plan. Nurses should take the time to explain the nature of the infection and the rationale behind the prescribed treatment. Using simple and non-medical language, nurses can help patients understand the cause of their ear infection, how it is being treated, and what they can expect during the healing process. Visual aids such as diagrams or videos can also enhance understanding and ensure that patients feel informed and empowered to participate in their care.
Encouraging questions and addressing concerns
Patients may have questions or concerns about their ear infection and its management. Nurses should encourage patients to actively participate in their healthcare by asking questions and expressing any concerns they may have. By creating a safe and non-judgmental environment, nurses can foster open and honest communication. Addressing patients’ questions and concerns with empathy and respect helps alleviate anxiety and ensures that patients have the knowledge and confidence to manage their condition effectively.
Collaborating with the healthcare team for comprehensive care
As part of a multidisciplinary healthcare team, nurses play a crucial role in collaborating and communicating with other healthcare professionals involved in the care of patients with ear infections. Effective communication ensures seamless and comprehensive care while minimizing the risk of errors or gaps in treatment. Nurses should actively participate in interdisciplinary meetings, sharing important patient information and contributing their expertise. By working collaboratively, the healthcare team can provide holistic care that addresses all aspects of the patient’s health and well-being.

Supporting Patient’s Emotional Well-being
Showing empathy and providing emotional support
Being diagnosed with an ear infection can be distressing for patients, as it can cause pain, discomfort, and disruption to daily life. Nurses should approach patients with empathy and compassion, acknowledging the impact the infection may have on their emotional well-being. By actively listening to patients and displaying genuine care and understanding, nurses can help alleviate anxiety and create a supportive environment. Simple gestures such as holding a patient’s hand, offering a listening ear, or providing emotional reassurance can go a long way in supporting patients’ emotional well-being.
Assessing and addressing anxiety or fear
Anxiety and fear are common emotions experienced by patients with ear infections, especially if they are experiencing severe pain or have a history of recurrent infections. Nurses should assess patients for signs of anxiety or fear and provide appropriate interventions to address these emotions. Techniques such as deep breathing exercises, guided imagery, or distraction techniques can help patients relax and alleviate anxiety. Additionally, providing clear and honest explanations about the infection and the treatment plan can help reduce fear and uncertainty. Referring patients to support groups or counseling services may also be beneficial for those struggling with significant emotional distress.
Helping the patient cope with discomfort
Ear infections can cause significant discomfort, which may impact patients’ overall well-being. Nurses should provide strategies to help patients cope with this discomfort. Applying warm compresses or cold packs, as preferred by the patient, can help relieve pain and reduce inflammation. Teaching relaxation techniques, such as progressive muscle relaxation or meditation, can also provide patients with effective coping mechanisms. It is important for nurses to individualize interventions based on the patient’s preferences and needs, ensuring that they feel supported on their journey towards recovery.
Educating the Patient and Family
Explaining the causes and risk factors of ear infections
Educating patients and their families about the causes and risk factors of ear infections is essential for effective prevention and management. Nurses should provide information on the common causes of ear infections, including bacterial and viral infections, as well as risk factors such as frequent exposure to secondhand smoke, improper ear hygiene, or attendance at daycare. By understanding the underlying causes and risk factors, patients and families can make informed decisions to reduce their susceptibility to ear infections.
Providing information about prevention strategies
Preventing ear infections is an important aspect of overall ear health. Nurses should educate patients and their families about strategies to prevent ear infections. This includes emphasizing the importance of hand hygiene, especially before touching the face or ears, as well as proper ear hygiene practices. Nurses should also educate patients on the benefits of receiving vaccines, such as the pneumococcal vaccine or the influenza vaccine, to reduce the risk of infections that can lead to ear infections. Furthermore, recommending the use of ear protection, such as earplugs or earmuffs, in noisy environments or during swimming can help prevent damage to the ears and reduce the likelihood of infections.
Teaching warning signs to watch for
Recognizing the warning signs of ear infections is crucial for early intervention and prevention of complications. Nurses should educate patients and families about the common symptoms of ear infections, such as ear pain, pressure, hearing loss, fever, or drainage from the ear. Informing them about when to seek medical attention, such as when symptoms persist or worsen, can prevent delays in treatment and potential complications. By teaching patients and families to be vigilant for warning signs, nurses empower them to take proactive steps in their healthcare and ensure timely intervention.

Collaborating with the Multidisciplinary Team
Communicating with physicians for appropriate interventions
Collaboration with physicians is paramount to ensure appropriate interventions and holistic care for patients with ear infections. Nurses should effectively communicate important patient information, such as the current symptoms, treatment responses, and any concerns or complications, to the physician. This enables the physician to make informed decisions regarding necessary medical interventions, such as adjusting the treatment plan or prescribing additional tests. By maintaining open lines of communication, nurses and physicians can coordinate care effectively and provide the best possible outcomes for patients.
Consulting with audiologists for hearing evaluations
Hearing loss is a potential complication of ear infections, and consulting with audiologists can help assess and manage this aspect of the patient’s care. Nurses should collaborate with audiologists to ensure timely hearing evaluations for patients with suspected hearing concerns. Audiologists can perform comprehensive hearing tests to assess any hearing loss and provide appropriate recommendations, such as hearing aids or auditory rehabilitation. By involving audiologists in the care of patients with ear infections, nurses contribute to providing comprehensive care that addresses all aspects of the patient’s well-being.
Coordinating care with pharmacists for medication management
Pharmacists play a vital role in medication management and safety. Nurses should collaborate with pharmacists to ensure appropriate medication selection, dosing, and administration for patients with ear infections. Pharmacists can provide valuable input regarding potential drug interactions, allergies, or contraindications. Additionally, pharmacists can assist nurses in educating patients and their families about medication usage, potential side effects, and proper storage and disposal of medications. By involving pharmacists in the care of patients with ear infections, nurses contribute to safe and effective medication management, promoting optimal treatment outcomes.
Ensuring Follow-up Care
Scheduling follow-up appointments
Follow-up appointments are essential to monitor the patient’s progress and ensure that treatment is effective. Nurses should assist in scheduling follow-up appointments for patients with ear infections. The timing of these appointments may vary depending on the severity of the infection and the response to treatment. Ensuring that patients understand the importance of attending these appointments and providing them with clear instructions on the date, time, and location of the follow-up visit helps prevent missed appointments and ensures continuity of care.
Monitoring the patient’s progress
Regular monitoring of the patient’s progress is crucial to evaluate the effectiveness of the treatment plan and identify any signs of complications. Nurses should closely monitor the patient’s symptoms, such as pain levels, fever, and drainage from the ear, to assess whether the infection is resolving appropriately. In cases where additional interventions or adjustments to the treatment plan are necessary, nurses should promptly communicate this information to the healthcare team. By closely monitoring the patient’s progress, nurses can ensure timely interventions and optimize the overall outcome of the treatment.
Addressing any ongoing concerns
Throughout the course of treatment, patients may have ongoing concerns or questions. Nurses should be attentive to these concerns and provide appropriate support and guidance. Addressing concerns promptly and effectively helps alleviate anxiety and ensures that patients feel heard and supported. Nurses should be open to discussing any ongoing issues with the patient and their family, seeking solutions to address their concerns and enhance overall satisfaction with their healthcare experience.
In summary, nursing considerations for ear infections encompass a comprehensive assessment of the patient, effective pain management strategies, prevention of complications, maintenance of ear hygiene, administration of medications, promotion of effective communication, support for the patient’s emotional well-being, education of the patient and their family, collaboration with the multidisciplinary team, and ensuring appropriate follow-up care. By conducting a thorough assessment, managing pain effectively, preventing complications, promoting ear hygiene, providing the necessary medications, fostering effective communication, supporting the patient’s emotional well-being, educating the patient and their family, collaborating with the multidisciplinary team, and ensuring follow-up care, nurses play a vital role in the holistic and optimal care of patients with ear infections.