Imagine you’re a dedicated nurse who is always ready to provide the best care for your patients. Today, we will explore the nursing considerations for Graves Disease, a thyroid disorder that can greatly impact a person’s well-being. From understanding the symptoms and complications to managing the treatment plan effectively, this article will equip you with the knowledge and strategies you need to support your patients on their journey towards healing and wellness. So, let’s dive into the world of nursing considerations for Graves Disease and empower ourselves to make a positive difference in the lives of those we care for.
Understanding Graves Disease
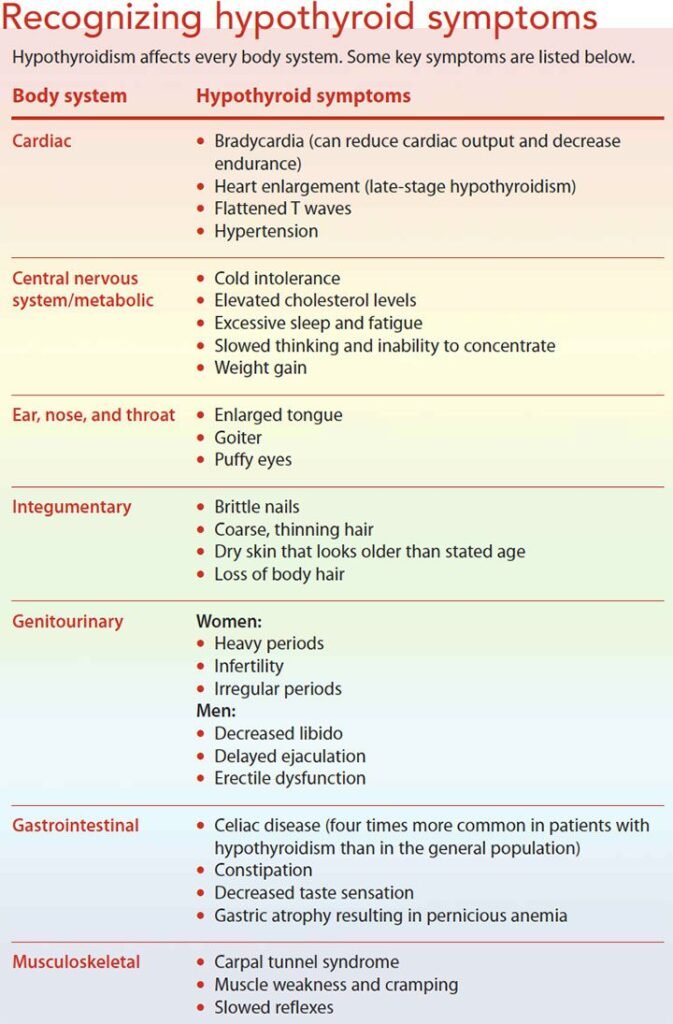
Graves Disease is an autoimmune disorder that affects the thyroid gland, resulting in hyperthyroidism. It is named after the doctor who first described it, Robert J. Graves. This condition is characterized by the overproduction of thyroid hormones T3 and T4, leading to a wide range of symptoms. Some of the common symptoms include weight loss, increased appetite, palpitations, anxiety, tremors, heat intolerance, and goiter. In addition, a distinctive feature of Graves Disease is the development of ophthalmopathy, which causes eye-related symptoms such as bulging eyes, double vision, and dryness.
Etiology and Pathophysiology of Graves Disease
The exact cause of Graves Disease is still unknown, but it is believed to be the result of a combination of genetic and environmental factors. It is thought that certain genetic variations can make individuals susceptible to developing this autoimmune condition. Environmental triggers, such as stress, certain infections, and smoking, may also play a role in triggering the disease in susceptible individuals.
The pathophysiology of Graves Disease involves the production of antibodies called thyroid-stimulating immunoglobulins (TSIs), which bind to the thyroid-stimulating hormone (TSH) receptors on the thyroid gland. This binding stimulates the thyroid gland to produce and release excessive amounts of thyroid hormones. The interactions between the TSIs and TSH receptors also contribute to the development of ophthalmopathy by causing inflammation and tissue remodeling in the orbital tissues.

Diagnosis and Assessment of Graves Disease
Diagnosing Graves Disease involves a comprehensive assessment that includes a thorough history taking, physical examination, and laboratory tests. The patient’s symptoms, such as weight loss, palpitations, and heat intolerance, may provide important clues to the presence of hyperthyroidism. A physical examination may reveal a diffusely enlarged thyroid gland, known as a goiter, and signs of ophthalmopathy.
Laboratory tests are essential for confirming the diagnosis. Blood tests are conducted to measure the levels of thyroid hormones, such as T3 and T4, as well as TSH. In Graves Disease, T3 and T4 levels are elevated, while TSH levels are typically low. The presence of TSIs can also be detected through blood tests, which play a role in confirming the autoimmune nature of the disease.
Medical Treatment for Graves Disease
The treatment for Graves Disease aims to restore normal thyroid function and alleviate the symptoms. Several medical treatment options are available, depending on the severity of the condition and the individual’s preferences.
Antithyroid Medications
Antithyroid medications, such as propylthiouracil (PTU) and methimazole (MMI), are commonly prescribed as the initial treatment for Graves Disease. These medications work by inhibiting the production of thyroid hormones. By doing so, they help to reduce the symptoms of hyperthyroidism and restore the balance of thyroid function.
Radioactive Iodine Therapy
Radioactive iodine therapy involves the administration of a radioactive form of iodine orally. The radioactive iodine is taken up by the thyroid gland, where it destroys the overactive thyroid cells. This treatment option is particularly useful for individuals who have difficulty adhering to antithyroid medications or have a relapse after discontinuing medication. However, it often leads to the development of hypothyroidism, necessitating lifelong thyroid hormone replacement therapy.
Thyroidectomy
Thyroidectomy is the surgical removal of all or part of the thyroid gland. It is typically reserved for individuals who are not suitable candidates for antithyroid medications or radioactive iodine therapy, or for those who have large goiters or severe ophthalmopathy. Thyroidectomy can effectively cure Graves Disease, but it requires the lifelong administration of thyroid hormone replacement therapy.
Psychiatric Medications
Psychiatric medications, such as beta-blockers, may be prescribed to manage some of the symptoms associated with Graves Disease, such as anxiety, tremors, and palpitations. These medications help to alleviate the discomfort caused by excessive thyroid hormones and provide symptomatic relief.

Nursing Assessment
A comprehensive nursing assessment is crucial for identifying the specific needs and potential complications associated with Graves Disease. The assessment should include a detailed history taking and physical examination, as well as specific evaluations.
History and Physical Examination
The nursing assessment should begin with a thorough history taking, including the patient’s medical history, family history, and any previous exposure to risk factors that may contribute to the development of Graves Disease, such as recent stressors or infections. Physical examination should focus on the signs and symptoms of hyperthyroidism, including palpitations, tremors, goiter, and ophthalmic manifestations.
Thyroid Function Tests
The nurse should be knowledgeable about the laboratory tests used to diagnose and monitor Graves Disease. This includes understanding the normal ranges for thyroid hormones, such as T3, T4, and TSH, as well as the significance of TSIs. The nurse should also be prepared to educate the patient about the purpose of these tests and the importance of adhering to the recommended follow-up schedule.
Ophthalmic Evaluation
Due to the high prevalence of ophthalmopathy in Graves Disease, a comprehensive ophthalmic evaluation is an essential component of the nursing assessment. This evaluation may include visual acuity testing, assessment of eye movement and alignment, and evaluation of tear production. The nurse should document any changes in visual acuity, ocular discomfort, or other ophthalmic manifestations, as these may require further intervention.
Nursing Diagnosis
Based on the comprehensive nursing assessment, several nursing diagnoses may be applicable to individuals with Graves Disease. These nursing diagnoses reflect the potential physical and psychosocial issues that can arise from the condition and guide the development of appropriate nursing interventions.
Hyperthyroidism
One of the primary nursing diagnoses for individuals with Graves Disease is hyperthyroidism. This diagnosis reflects the overproduction of thyroid hormones and encompasses symptoms such as increased metabolic rate, weight loss, and cardiac manifestations. Nursing interventions should focus on maintaining fluid and electrolyte balance, alleviating symptoms of hyperthyroidism, and promoting rest and comfort.
Exophthalmos
Exophthalmos, or bulging eyes, is a characteristic feature of Graves Disease. This nursing diagnosis recognizes the potential complications associated with ophthalmopathy, such as impaired vision, eye discomfort, and corneal ulceration. Nursing interventions should aim to protect the patient’s eyes from further damage, maintain eye moisture, and promote regular ophthalmic evaluations.
Body Image Disturbance
Body image disturbance is a common psychosocial concern for individuals with Graves Disease, especially those with visible physical manifestations such as goiter or ophthalmopathy. This nursing diagnosis acknowledges the potential impact of these physical changes on the individual’s self-esteem and body image. Nursing interventions should include providing emotional support, encouraging open communication, and facilitating access to counseling services if needed.
Risk for Infection
Individuals with Graves Disease may be at an increased risk of infection due to the immunosuppressive effects of hyperthyroidism, as well as the potential complications associated with ophthalmopathy. This nursing diagnosis highlights the importance of identifying and addressing factors that may increase the risk of infection, such as poor wound healing or ocular surface damage. Nursing interventions should focus on promoting infection prevention measures and providing education on proper wound care and eye hygiene.
Nursing Interventions
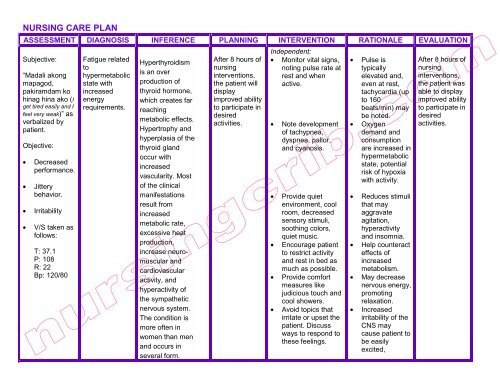
To provide optimal care for individuals with Graves Disease, nursing interventions should be tailored to address the specific nursing diagnoses identified during the nursing assessment. These interventions aim to promote thyroid function balance, manage ophthalmopathy, address emotional and psychological needs, and prevent complications.
Promoting Thyroid Function Balance
Nursing interventions to promote thyroid function balance include promoting a quiet and restful environment, providing comfort measures, and assisting with the administration of antithyroid medications as prescribed. Nurses should also monitor the patient’s vital signs, assess for signs of worsening hyperthyroidism, and educate the patient about the importance of medication compliance.
Managing Exophthalmos
Managing exophthalmos involves protecting the patient’s eyes from injury, promoting eye comfort, and facilitating ophthalmic evaluations. Nurses can provide education on proper eye care, such as using lubricating eye drops or ointments, avoiding eye strain, and wearing eye protection when necessary. Additionally, nurses should monitor the patient’s visual acuity and report any changes to the healthcare team promptly.
Addressing Emotional and Psychological Needs
Addressing the emotional and psychological needs of individuals with Graves Disease is an essential aspect of nursing care. Nurses should provide emotional support, engage in active listening, and encourage the patient to express their concerns and fears. Referrals to mental health professionals, such as counselors or support groups, may be beneficial for individuals struggling with body image disturbance or coping with the diagnosis.
Preventing Complications
Preventing complications involves a proactive approach to patient care. Nurses should educate the patient about potential complications, such as thyroid storm or infections, and provide guidance on recognizing and reporting symptoms. Additionally, nurses should monitor for signs of infection, assess wound healing if a thyroidectomy was performed, and collaborate with the healthcare team to ensure appropriate follow-up care.
Patient Education
Patient education is an essential component of nursing care for individuals with Graves Disease. By providing education, nurses empower patients to actively participate in their own care and make informed decisions about their health. The following topics should be addressed during patient education:
Understanding Graves Disease
Patients should be educated about the nature of Graves Disease, including its causes, symptoms, and potential complications. Understanding the underlying mechanisms of the disease can help patients cope with their condition and adhere to treatment plans.
Medication Management
Patients taking antithyroid medications should receive thorough education on the proper administration technique, dosage schedule, and potential side effects. They should also understand the importance of medication compliance and regular follow-up appointments.
Signs and Symptoms of Thyroid Storm
Thyroid storm is a severe complication of Graves Disease characterized by an exacerbation of hyperthyroid symptoms. Patients should be educated about the signs and symptoms of thyroid storm, such as high fever, severe agitation, and altered mental status. They should understand the importance of seeking immediate medical attention if these symptoms occur.
Lifestyle Modifications
Patients should be encouraged to adopt lifestyle modifications to support their overall health and manage the symptoms of Graves Disease. This may include maintaining a well-balanced diet, engaging in regular exercise, managing stress, and avoiding known triggers, such as smoking or excessive caffeine intake.
Collaborative Care
Collaboration with the healthcare team is crucial in the management of Graves Disease. The nurse plays a vital role in communicating relevant information and coordinating care with various healthcare professionals involved in the patient’s treatment. The following collaborative care strategies should be implemented:
Working with Endocrinologist
Endocrinologists are physicians specializing in the diagnosis and treatment of endocrine disorders, including Graves Disease. Nurses should collaborate closely with endocrinologists in monitoring the patient’s response to treatment, assessing thyroid hormone levels, and adjusting medication dosages as needed.
Consulting with Ophthalmologist
Ophthalmologists specialize in eye care and are particularly important in managing the ophthalmic manifestations associated with Graves Disease. Nurses should consult with ophthalmologists to ensure regular ophthalmic evaluations, monitor for changes in visual acuity or eye discomfort, and provide appropriate interventions to manage symptoms.
Involving Mental Health Professionals
Mental health professionals, such as counselors or psychologists, can play a crucial role in supporting individuals with Graves Disease who experience emotional distress or body image disturbance. Nurses should involve these professionals as needed, either through referrals or by facilitating access to support groups or counseling services.
Coordinating with Surgeons
For individuals who require thyroidectomy as part of their treatment plan, coordination with surgeons is essential. Nurses should advocate for timely and appropriate preoperative and postoperative care, including wound assessment, pain management, and education about post-thyroidectomy care and potential complications.
Nursing Considerations during Medical Procedures
Nurses have a significant role in assisting with and monitoring patients undergoing medical procedures related to Graves Disease. The following nursing considerations should be taken into account:
Antithyroid Medication Administration
Nurses should be knowledgeable about the specific antithyroid medications prescribed to the patient and follow the appropriate administration protocols. This includes verifying the correct dosage, timing, and potential side effects, as well as educating the patient on self-administration if applicable.
Radioactive Iodine Therapy Monitoring
During radioactive iodine therapy, nurses should closely monitor the patient for potential side effects, such as nausea, thyroid pain, or radiation-related complications. They should also educate the patient about necessary precautions, such as avoiding close contact with pregnant individuals or infants.
Preoperative and Postoperative Care for Thyroidectomy
Nurses should collaborate with the surgical team to ensure comprehensive preoperative and postoperative care for patients undergoing thyroidectomy. This includes conducting preoperative assessments, educating the patient about the procedure and potential complications, and providing appropriate wound care and pain management during the postoperative period.
Psychiatric Medication Administration
When psychiatric medications are part of the treatment plan for Graves Disease, nurses should follow the appropriate protocols for medication administration. This includes assessing the patient for potential contraindications or side effects, educating the patient about the purpose and expected outcomes of the medication, and monitoring the patient’s response to treatment.
Monitoring and Evaluation
Monitoring the patient’s progress and evaluating the effectiveness of the nursing interventions are essential aspects of nursing care for individuals with Graves Disease. The following areas should be assessed and evaluated:
Assessing Thyroid Hormone Levels
Regular monitoring of thyroid hormone levels, including T3, T4, and TSH, is crucial to evaluate the patient’s response to treatment and adjust medication dosages as needed. Nurses should be knowledgeable about the recommended frequency of these tests and the interpretation of the results.
Evaluating Ophthalmic Manifestations
The nurse should assess the patient’s ophthalmic manifestations, such as visual acuity, eye discomfort, or the presence of exophthalmos, at regular intervals. Any changes should be documented and reported to the healthcare team promptly to ensure comprehensive evaluation and intervention.
Patient’s Response to Treatment
Continuous evaluation of the patient’s response to treatment, including symptomatic relief and thyroid hormone level stabilization, is essential. Nurses should assess for improvements in hyperthyroidism symptoms, such as weight stabilization or reduction in palpitations, and communicate these findings to the healthcare team.
Identifying Complications and Adverse Reactions
Prompt identification and management of complications or adverse reactions is crucial in the care of individuals with Graves Disease. Nurses should remain vigilant for potential complications, such as thyroid storm, infectious processes, or worsening ophthalmic manifestations, and communicate any concerning findings to the healthcare team.
Conclusion
In conclusion, the nursing considerations for Graves Disease encompass a wide range of aspects, including comprehensive assessments, the development and implementation of appropriate nursing interventions, patient education, and collaboration with the healthcare team. By understanding the specific needs of individuals with Graves Disease and providing holistic care, nurses can play a crucial role in promoting optimal health outcomes and improving the quality of life for those affected by this autoimmune disorder.
