In this informative article, you will discover valuable insights and practical tips on nursing considerations for individuals dealing with genital warts caused by the Human Papillomavirus (HPV). We will explore the essential elements of nursing management, including prevention strategies, patient education, and effective treatment options. Whether you are a healthcare professional or someone seeking information on how to provide optimum care, this article will equip you with the necessary tools to navigate the complexities of genital warts-HPV, ensuring the best possible outcomes for those under your care.

Assessment
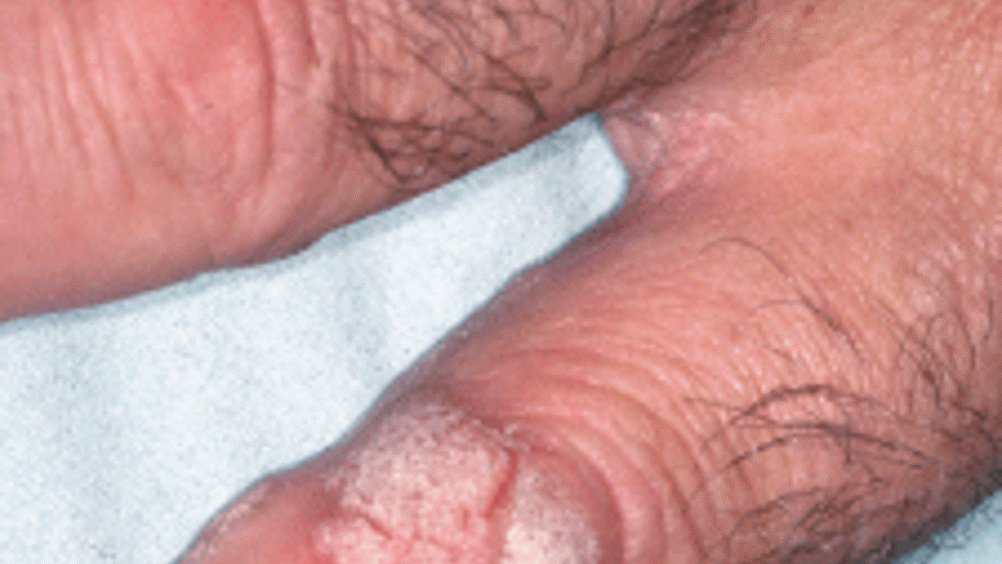
Signs and symptoms
When assessing a patient for genital warts, it is important to look for specific signs and symptoms that are associated with this condition. Genital warts are caused by the Human Papillomavirus (HPV) and can appear as small, flesh-colored bumps or clusters on the genitals or surrounding areas. These warts can vary in size and shape and may resemble cauliflower-like growths. It is also important to note that some individuals may not experience any noticeable signs or symptoms, which is why regular screenings and education are crucial in detecting and managing genital warts.
Physical examination
During a physical examination, the healthcare provider will carefully examine the genital area to identify any visible warts. This examination may include visual inspection and palpation to determine the location, size, and number of warts present. Special attention should be paid to the cervix in female patients, as internal genital warts can also occur. In addition to assessing for physical signs, it is essential to create a safe and comfortable environment for the patient during the examination and maintain their privacy and dignity throughout the process.
Psychosocial assessment
In addition to the physical assessment, it is crucial to conduct a psychosocial assessment when caring for individuals with genital warts. The diagnosis of genital warts can have a significant emotional and psychological impact on patients. They may experience feelings of shame, embarrassment, guilt, or anxiety due to the stigma associated with sexually transmitted infections. It is important for healthcare providers to create a non-judgmental and supportive environment, allowing patients to express their concerns and providing appropriate counseling and resources to address their psychosocial needs.
Diagnosis
Medical history
Obtaining a detailed medical history is an essential part of diagnosing genital warts. The healthcare provider will inquire about the patient’s sexual history, including the number of sexual partners, the presence of other sexually transmitted infections (STIs), and any previous history of genital warts or HPV infection. It is crucial to assess the patient’s understanding of their diagnosis and provide education regarding the virus and its potential complications.
Physical examination
As mentioned earlier, a thorough physical examination is crucial in diagnosing genital warts. Visual inspection and palpation of the genital area can help identify the characteristic appearance of warts. Additionally, the healthcare provider may use a colposcope or magnifying lens to examine the cervix in female patients to detect internal genital warts that may not be visible to the naked eye.
Laboratory tests
In some cases, laboratory tests may be recommended to confirm the diagnosis of genital warts. These tests can include a Pap smear or a DNA test to detect the presence of HPV in the cells. It is important to note that a negative test result does not rule out the possibility of HPV infection, as the virus can sometimes be present in low levels and may not be detected by these tests. However, these tests can still provide valuable information and guidance for further management and treatment.
Biopsy
In certain situations where the diagnosis is uncertain or there is a suspicion of other conditions such as malignancy, a biopsy may be performed. During a biopsy, a small sample of tissue is taken from the suspected area and sent for laboratory analysis. This procedure is typically done under local anesthesia and can help confirm the diagnosis and guide appropriate treatment options.

Patient Education
Transmission
Educating patients about the transmission of genital warts is vital in preventing the spread of the infection. Genital warts are primarily transmitted through sexual contact, including vaginal, anal, and oral sex. It is important to emphasize that the virus can be transmitted even when no visible warts are present. The use of barrier methods such as condoms can reduce the risk of transmission but does not eliminate it entirely. Furthermore, pregnant individuals can pass the virus to their infants during childbirth.
Prevention
Preventing the transmission of genital warts involves adopting behavioral and lifestyle changes. Encouraging abstinence or having a mutually monogamous relationship with an uninfected partner can greatly reduce the risk of acquiring or spreading the virus. Safe sexual practices, such as consistent and correct use of condoms, can also help minimize the risk. Additionally, receiving the HPV vaccine, which protects against the most common strains of HPV, can provide further protection.
Treatment options
While there is no cure for the Human Papillomavirus (HPV), treatment options are available to manage the symptoms and reduce the risk of complications. These treatment options may include topical medications, cryotherapy, electrocautery, surgical excision, or immunotherapy. The choice of treatment will depend on factors such as the location, size, and number of warts, as well as the patient’s preferences and overall health. It is essential to discuss the benefits, risks, and potential side effects of each treatment option with the patient before making a decision.
Importance of follow-up
Emphasizing the importance of regular follow-up appointments is crucial in managing genital warts effectively. Follow-up visits allow healthcare providers to monitor the patient’s response to treatment, assess for any potential complications or recurrence, and provide ongoing education and support. It is essential for patients to adhere to the recommended follow-up schedule to ensure optimal treatment outcomes and prevent the progression of the infection or the development of other complications.
Infection Control
Hand hygiene
Proper hand hygiene is a fundamental aspect of infection control when caring for patients with genital warts. Healthcare providers should ensure they wash their hands thoroughly with soap and water or use an alcohol-based hand sanitizer before and after any patient contact. This practice helps prevent the spread of HPV or any other potential infections.
Personal protective equipment
Wearing appropriate personal protective equipment (PPE) is essential when providing care to patients with genital warts. Healthcare providers should don gloves when performing any procedures involving direct contact with the warts or potentially contaminated specimens or objects. It is necessary to dispose of gloves properly and follow institutional guidelines for PPE use and disposal to prevent cross-contamination.
Managing contaminated objects
Proper handling and disposal of contaminated objects are essential in preventing the spread of infection. Contaminated objects, such as biopsy samples or materials used during procedures, should be disposed of according to institutional guidelines and local regulations. Healthcare providers should also consider using single-use equipment when possible to minimize the risk of cross-contamination.
Environmental considerations
Maintaining a clean and hygienic environment is crucial in preventing the transmission of genital warts. Environmental surfaces, such as examination tables, should be cleaned and disinfected regularly using appropriate disinfectants. It is also important to ensure that the environment is well-ventilated to reduce the risk of airborne transmission.
Isolation precautions
In certain situations, isolation precautions may be necessary to prevent the spread of genital warts. Depending on the patient’s condition and institutional guidelines, precautions such as contact isolation or droplet precautions may be implemented. These precautions aim to minimize the risk of transmission to other patients and healthcare providers and should be strictly followed.

Treatment
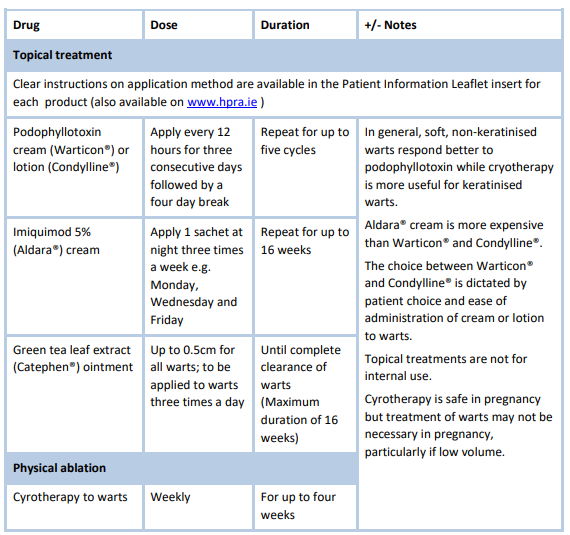
Topical medications
Topical medications are often used as a first-line treatment for genital warts. These medications contain ingredients such as podophyllotoxin or imiquimod that work by destroying the wart tissue or stimulating the immune system to fight the virus. It is important for patients to follow the prescribed instructions and apply the medication only to the affected areas, avoiding healthy skin. It is also essential to educate patients about potential side effects such as local irritation or redness and when to seek medical advice.
Cryotherapy
Cryotherapy involves the use of freezing temperatures to destroy the wart tissue. Liquid nitrogen is applied directly to the warts, causing them to freeze and subsequently fall off. This treatment may require multiple sessions and can cause discomfort or mild pain. Patients should be informed about the potential side effects, such as blistering or temporary skin discoloration, and the importance of proper wound care during the healing process.
Electrocautery
Electrocautery is a procedure that uses an electric current to heat a small loop or needle, which is then used to burn or cut off the wart tissue. This procedure is typically performed under local anesthesia and may leave a small wound that requires care and monitoring. Patients should be provided with post-procedure instructions and educated on signs of infection or complications.
Surgical excision
In cases where the warts are large, extensive, or resistant to other treatments, surgical excision may be necessary. During this procedure, the warts are surgically removed using a scalpel or other surgical instruments. It is important to consider the potential risks, such as scarring or bleeding, and discuss them with the patient before proceeding with surgical excision.
Immunotherapy
Immunotherapy involves the use of medications or substances that stimulate the body’s immune system to attack and eliminate the wart tissue. These treatments, such as interferon injections or immune response modifiers, can be administered directly into the warts or applied topically. However, it is important to note that immunotherapy is not always effective and may be associated with potential side effects or adverse reactions. Patients should be thoroughly informed about the benefits and risks of this treatment option.
Complications
Recurrence
One of the potential complications of genital warts is recurrence. Even with successful treatment and resolution of visible warts, the virus may remain in the body and can lead to the reemergence of warts in the future. It is important for patients to understand that recurrence is possible and that regular follow-up visits are necessary to monitor for any new lesions and provide appropriate management.
Spread of infection
Genital warts are highly contagious and can be easily transmitted through sexual contact. It is vital for patients to be aware of the potential risk of spreading the infection to their sexual partners. Educating patients on safe sexual practices, such as consistent and correct condom use, can help reduce the risk of transmission. Additionally, providing information on the importance of regular screening and testing for other sexually transmitted infections can help identify and prevent the spread of infection.
Malignancy risk
Certain strains of HPV, especially those associated with genital warts, have been linked to an increased risk of developing certain types of cancer, including cervical, penile, and anal cancer. It is crucial to educate patients about this potential risk and the importance of regular screenings, such as Pap smears or anal cytology, as appropriate, to detect any precancerous or cancerous changes early on. Encouraging vaccination against HPV can also help reduce the risk of developing these malignancies.
Ethical Considerations
Confidentiality
Protecting patient confidentiality is of utmost importance when caring for individuals with genital warts. Healthcare providers must ensure that patient information is kept strictly confidential and is accessible only to those involved in the patient’s care. Following institutional guidelines and regulations regarding privacy and confidentiality is crucial to maintain trust and ensure patient autonomy.
Informed consent
Obtaining informed consent from patients is an ethical obligation and a legal requirement. It is essential to explain the diagnosis, treatment options, potential risks, benefits, and alternatives to the patient in a clear and understandable manner. Patients should have the opportunity to ask questions, seek clarification, and make informed decisions regarding their care. Documenting the informed consent process is important to prevent any misunderstandings and protect both the patient and the healthcare provider.
Autonomy
Respecting patient autonomy is a fundamental ethical principle in healthcare. Patients have the right to make decisions about their own bodies and health, including their chosen treatment options. Healthcare providers should empower patients by providing them with accurate information, discussing available options, and supporting their choices. It is essential for healthcare providers to understand and respect their patients’ cultural, religious, and personal beliefs when providing care.
Non-judgmental attitude
A non-judgmental attitude is crucial when providing care for individuals with genital warts. Stigma and misconceptions surrounding sexually transmitted infections can often lead to feelings of shame, guilt, or embarrassment in patients. Healthcare providers should create a safe and supportive environment where patients can openly discuss their concerns and ask questions without fear of judgment. Providing empathetic and compassionate care can help alleviate patient distress and contribute to a positive therapeutic relationship.
Psychosocial Support
Counseling
Counseling plays a crucial role in providing psychosocial support for individuals with genital warts. Patients may experience a range of emotions, including anxiety, guilt, or feelings of isolation. Counseling sessions can provide a safe space where patients can express their concerns and receive guidance on managing their emotions, relationships, and sexual health. Counselors can also address any misconceptions or myths surrounding genital warts and provide education to foster a better understanding of the condition.
Emotional support
Providing emotional support is essential for patients coping with the diagnosis of genital warts. Healthcare providers should be available to listen and validate the patient’s feelings and emotions. Offering empathy, reassurance, and encouragement can help patients feel supported and lessen their psychological burden. Additionally, connecting patients with support groups or online communities specifically dedicated to individuals with genital warts can provide them with a sense of belonging and an opportunity to share experiences and resources.
Addressing stigma
Genital warts are often associated with stigma and can significantly impact an individual’s self-esteem and social well-being. Healthcare providers should actively challenge and address the stigma surrounding genital warts and promote public understanding and acceptance. By providing education and dispelling myths, healthcare providers can help reduce the negative impact of stigma on patients’ lives and encourage an open dialogue about sexually transmitted infections.
Follow-up Care
Monitoring
Regular monitoring is essential to ensure the ongoing management and treatment of genital warts. Follow-up appointments allow healthcare providers to assess the patient’s response to treatment, monitor for recurrence or complications, and provide necessary education and support. These appointments should be scheduled based on individual patient needs and treatment plans, and healthcare providers should document the patient’s progress and any changes observed during each visit.
Reevaluation
Periodic reevaluation of the patient’s condition is crucial in determining the effectiveness of the chosen treatment and making any necessary adjustments. Healthcare providers should assess whether the treatment is achieving the desired outcomes and whether any modifications are required. Reevaluation may involve physical examinations, laboratory tests, or imaging studies, depending on the patient’s individual circumstances.
Screening for other STIs
Genital warts often coexist with other sexually transmitted infections (STIs). Regular screening for other STIs, such as syphilis, gonorrhea, chlamydia, or HIV, is important to identify and treat any additional infections that may be present. The presence of one STI increases the risk of acquiring or transmitting others, highlighting the importance of comprehensive screening and appropriate treatment for all sexually active individuals.
Collaborative Care
Multidisciplinary approach
Caring for patients with genital warts often requires a multidisciplinary approach. Healthcare providers from various specialties, including dermatology, gynecology, urology, and infectious diseases, may be involved in the patient’s care. Collaboration and communication among healthcare professionals help ensure comprehensive and holistic care for the patient. This includes exchanging information, discussing treatment options, and coordinating follow-up care.
Referrals
In some cases, referrals to specialists may be necessary to further evaluate or manage specific aspects of genital warts. For example, referrals to a dermatologist may be appropriate for complex or extensive cases, while referrals to a gynecologist or urologist may be needed to address specific concerns related to sexual health and fertility. Collaboration with specialists allows for specialized care and expertise, enhancing the overall quality of patient care.
Consultations
Consultations with other healthcare professionals can provide valuable insights and support in managing genital warts. Healthcare providers may seek consultations with infectious disease specialists, psychologists, or counselors to address specific concerns or obtain expert advice. These consultations help ensure that the patient receives the most current and appropriate care and benefit from the collective knowledge and experience of the healthcare team.