Nursing considerations for heat rash are crucial to ensure the well-being of patients experiencing this common skin condition. From identifying the symptoms and contributing factors to providing appropriate interventions and patient education, nurses play a vital role in managing and alleviating the discomfort caused by heat rash. This article explores the essential nursing considerations and management strategies for heat rash, equipping nurses with the knowledge and skills needed to provide optimal care and support to patients in need.

Understanding Heat Rash
Heat rash, also known as miliaria, is a common dermatologic condition that occurs as a result of the blockage of sweat ducts. This blockage prevents sweat from evaporating properly, leading to inflammation and the development of a rash. Heat rash can be uncomfortable and itchy, but it is usually not serious and can be managed with the appropriate care.
Definition of Heat Rash
Heat rash is defined as a skin condition characterized by the formation of small, raised bumps on the skin. These bumps may appear red and can be surrounded by a prickly or stinging sensation. Heat rash is most commonly found in areas of the body that are prone to sweating, such as the neck, armpits, groin, and under the breasts. It can affect people of all ages, but it is especially common in infants and young children.
Causes of Heat Rash
Heat rash occurs when sweat ducts become blocked, preventing sweat from reaching the surface of the skin. There are several factors that can contribute to the development of heat rash:
-
Hot and humid weather: Heat rash is most likely to occur in hot and humid climates or during the summer months when sweating is more common.
-
Excessive sweating: Engaging in activities that cause excessive sweating, such as rigorous physical exercise or wearing tight clothing, can increase the risk of developing heat rash.
-
Overheated spaces: Spending time in hot, enclosed spaces where air circulation is limited, such as a sauna or certain types of clothing, can contribute to the development of heat rash.
-
Immature sweat ducts: In infants, the sweat ducts may not be fully developed, making them more prone to blockage and the formation of heat rash.
Types of Heat Rash
Heat rash can present in different forms, depending on the depth of the blockage in the sweat ducts. The three main types of heat rash are:
-
Miliaria crystallina: This is the mildest form of heat rash, characterized by the appearance of clear, fluid-filled blisters on the skin. These blisters often burst and do not leave any lasting marks.
-
Miliaria rubra: Also known as prickly heat, miliaria rubra is the most common form of heat rash. It presents as red bumps surrounded by a prickly or stinging sensation. In some cases, the rash may develop into deeper, inflamed bumps or pustules.
-
Miliaria profunda: This is the least common form of heat rash and occurs when sweat is trapped deep within the skin. Miliaria profunda is characterized by the development of firm, flesh-colored bumps that are not itchy or painful.
Assessment and Diagnosis
To properly assess and diagnose heat rash, healthcare professionals employ various methods to gather information about the patient’s condition. These methods include:
Physical Examination
During a physical examination, healthcare providers examine the affected areas of the patient’s skin to assess the severity of the heat rash. They may look for specific characteristics such as redness, bumps, blisters, or pustules. It is important for the healthcare provider to examine different areas of the body where heat rash commonly occurs.
Medical History
Taking a thorough medical history is crucial in diagnosing heat rash. The healthcare provider will inquire about the patient’s symptoms, their onset, and any potential triggers that may have led to the development of the rash. Additionally, information about the patient’s lifestyle, activities, and environment can help determine the underlying cause of the heat rash.
Differential Diagnosis
Heat rash can sometimes resemble other skin conditions, so a differential diagnosis may be necessary to rule out other potential causes. Conditions such as contact dermatitis, allergic reactions, and certain viral or bacterial infections may have similar symptoms to heat rash. The healthcare provider will consider these possibilities and evaluate the patient’s symptoms and medical history to make an accurate diagnosis.
Laboratory Tests
In most cases, heat rash does not require laboratory tests for diagnosis. However, if the healthcare provider suspects an infection or another underlying condition, they may request additional tests such as swabs or cultures to identify any pathogens. These tests can help guide treatment and ensure appropriate management of the heat rash.
Signs and Symptoms
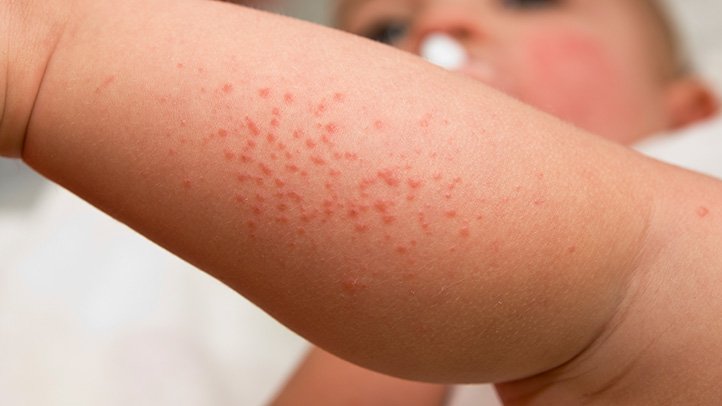
Recognizing the signs and symptoms of heat rash is essential for early identification and effective management. The following are common signs and symptoms associated with heat rash:
Skin Changes
The primary sign of heat rash is the appearance of red bumps, blisters, or pustules on the skin. These may be surrounded by areas of inflammation or redness. The rash is typically located in areas of the body prone to sweating, such as the neck, armpits, groin, and under the breasts.
Pruritus (Itching)
Heat rash can cause intense itching or a prickling sensation on the affected skin. The itching can vary in severity and may worsen with sweating or heat exposure. Scratching the affected area can further irritate the skin and potentially lead to secondary infections.
Pain or Discomfort
Heat rash may cause mild discomfort or a stinging sensation, especially if the rash becomes inflamed or if it develops into deeper bumps or pustules. However, the pain associated with heat rash is typically minimal and should not cause significant distress.
Excessive Sweating
Heat rash can be accompanied by increased sweating. This excess sweating may contribute to the blockage of sweat ducts and the development of heat rash. It is important to note that excessive sweating is a symptom of heat rash rather than a cause.
Prevention
Preventing heat rash involves taking proactive measures to reduce the likelihood of sweat duct blockages. The following preventive measures can help minimize the risk of developing heat rash:
Avoidance of Triggers
Avoiding triggers that contribute to heat rash is essential. This includes avoiding exposure to hot and humid environments, minimizing physical activities that promote excessive sweating, and wearing loose-fitting clothing that allows for proper air circulation.
Appropriate Clothing and Footwear
Choosing the right clothing and footwear can make a significant difference in preventing heat rash. Opt for lightweight, breathable fabrics that allow sweat to evaporate easily. Avoid tight-fitting clothing and shoes that can trap sweat and heat against the skin.
Regular Hygiene Practices
Practicing regular hygiene can help prevent heat rash. Showering or bathing daily and using mild, non-irritating cleansers can remove excess sweat, dirt, and bacteria from the skin. Be sure to dry the skin thoroughly after bathing to reduce moisture and the risk of sweat duct blockages.
Climate Control Measures
Implementing climate control measures in the living environment can also aid in preventing heat rash. Utilize fans or air conditioning to maintain a comfortable temperature and reduce humidity levels. Avoid spending prolonged periods in hot and cramped spaces, and seek shade or cool areas when outdoors.
Management
Managing heat rash involves a combination of treatment strategies aimed at alleviating symptoms and promoting healing. The management of heat rash may include the following approaches:
Topical Treatments
Applying topical treatments to the affected areas can provide relief from itching and help reduce inflammation. Calamine lotion, hydrocortisone cream, or over-the-counter antihistamine creams can help soothe the skin and alleviate discomfort. It is important to follow the instructions provided with these products and consult a healthcare professional if symptoms persist or worsen.
Cooling Measures
Implementing cooling measures can help relieve the symptoms of heat rash. Applying cool compresses or taking cool showers can alleviate itching, reduce inflammation, and promote healing. Additionally, staying in air-conditioned or well-ventilated spaces can aid in maintaining a cooler body temperature and prevent excessive sweating.
Fluid Intake
It is crucial to maintain adequate hydration when managing heat rash. Drinking plenty of fluids, especially water, can help prevent dehydration and promote sweat production, which can aid in unblocking the sweat ducts. It is important to avoid sugary or caffeinated beverages, as these can contribute to dehydration.
Antihistamines for Pruritus Relief
If itching associated with heat rash becomes severe and interferes with daily activities or sleep, healthcare professionals may recommend oral antihistamines. These medications can help relieve itching and improve overall comfort. However, it is important to consult with a healthcare professional before taking any medications to ensure their safety and effectiveness.
Patient Education
Educating patients about heat rash is essential for understanding the condition, reducing the risk of recurrence, and promoting self-care. The following topics should be addressed during patient education:
Explanation of Heat Rash
Patients should be provided with a clear and concise explanation of what heat rash is, how it occurs, and why it is common during hot and humid weather or excessive sweating. A visual aid, such as diagrams or photographs, can help convey the information effectively.
Preventive Measures
Patients should be educated on preventive measures to reduce the risk of heat rash. This includes avoiding triggers, wearing appropriate clothing, practicing regular hygiene, and implementing climate control measures. Patients should understand the importance of implementing these measures consistently, especially during periods of increased heat and humidity.
Proper Skin Care
Proper skin care can help prevent the development of heat rash and promote healing. Patients should be advised to gently cleanse the affected areas with mild soap and warm water, avoiding excessive scrubbing or use of harsh cleansers. They should also be encouraged to keep the skin dry and moisturized with lightweight, non-comedogenic moisturizers.
Recognition of Worsening Symptoms
Patients should understand the signs and symptoms that may indicate worsening of the heat rash or the development of complications. These may include increased redness, swelling, pus-filled bumps, or the presence of a fever. Patients should be instructed to seek medical attention if these symptoms occur.

Complications
While heat rash is usually a benign condition, it can lead to potential complications if not properly managed. The following are potential complications associated with heat rash:
Secondary Infections
Scratching the itchy skin or failing to maintain proper hygiene can increase the risk of secondary bacterial or fungal infections. These infections can cause additional inflammation, pain, and discomfort. If a secondary infection is suspected, medical attention should be sought promptly.
Contact Dermatitis
Some individuals may develop an allergic reaction or contact dermatitis in response to topical treatments or substances. This can exacerbate the symptoms and delay the healing process. If any signs of contact dermatitis, such as increased redness, swelling, or a rash, occur, patients should discontinue using the suspected irritant and consult a healthcare professional.
Exacerbation of Underlying Skin Conditions
People with pre-existing skin conditions such as eczema or psoriasis may experience exacerbation of their symptoms when heat rash occurs. The inflamed and sweaty skin can trigger flare-ups of these conditions, necessitating additional management strategies and care coordination with dermatologists or other specialists.
Collaborative Care
Collaborative care is crucial in the management of heat rash, as it involves the expertise and input of multiple healthcare professionals. The following parties play a significant role in the collaborative care of patients with heat rash:
Consultation with Dermatologist
In cases where heat rash is severe, recurrent, or associated with other skin conditions, a dermatologist may be consulted for further evaluation and management. Dermatologists can provide expert advice on treatment options, additional diagnostic tests, and long-term management strategies.
Referral to Allergist
For individuals who develop an allergic reaction or contact dermatitis as a result of heat rash or topical treatments, referral to an allergist may be necessary. Allergists can conduct allergen testing and provide guidance on avoiding triggers and managing allergies or hypersensitivity reactions.
Involvement of Primary Healthcare Provider
Primary healthcare providers, such as general practitioners or family physicians, play a central role in the initial assessment, diagnosis, and management of heat rash. They provide ongoing care, monitor the patient’s progress, and make referrals to specialists if necessary.
Coordination with Other Healthcare Team Members
If a patient with heat rash has underlying medical conditions or requires additional support, coordination with other healthcare team members is essential. This may include collaborating with dietitians, physiotherapists, or social workers to address any related physical or psychosocial needs.

Documentation
Accurate and detailed documentation is critical in the care of patients with heat rash. The following aspects should be documented by healthcare professionals:
Accurate and Detailed Assessment Findings
Precise documentation of the characteristics of the heat rash, such as location, size, color, and presence of any complications or infection, is important. Additionally, noting the severity of symptoms, presence of itching or pain, and any contributing factors will aid in tracking the progress of the condition.
Treatment Interventions
Documentation should include details of the treatments implemented, such as topical creams or oral medications prescribed. It is important to note the frequency, amount, and duration of treatment to monitor the effectiveness and adjust the management plan as necessary.
Patient Response to Interventions
Regular evaluation of the patient’s response to treatments is crucial in determining the effectiveness and adjusting the management plan as needed. Documenting the patient’s subjective improvement, as well as any objective changes observed during physical examinations, will help guide future interventions.
Any Changes in Condition
Any changes in the patient’s condition, such as the worsening of symptoms, the development of complications, or the presence of secondary infections, should be promptly and accurately documented. This information will guide further management decisions and facilitate communication between healthcare professionals involved in the patient’s care.
Follow-up Care
Follow-up care is important in monitoring the progress of the heat rash and ensuring that the patient’s symptoms improve over time. The following aspects should be considered during follow-up care:
Monitoring of Healing Process
Periodic assessments should be conducted to monitor the healing process of the heat rash. This includes evaluating the resolution of the rash, the reduction of inflammation, and the improvement of associated symptoms such as itching or discomfort. Regular follow-up appointments will help track the patient’s progress effectively.
Evaluation of Symptom Improvement
Patient-reported improvement of symptoms should be assessed during follow-up visits. Itching, pain, and other discomforts associated with heat rash should progressively decrease as the condition resolves. Monitoring these symptoms will aid in determining the effectiveness of the management strategies and making necessary adjustments.
Adjustments to Management Strategies
If the heat rash does not improve as expected or if new symptoms develop, adjustments to the management strategies may be required. This can include altering the prescribed treatments, exploring additional diagnostic tests, or making referrals to specialists for further evaluation or input.
Continued Patient Education
Follow-up care provides an opportunity to reinforce patient education and ensure that preventive measures and proper skin care are being implemented consistently. Patient understanding of heat rash, preventive strategies, and recognition of worsening symptoms should be reassessed and reinforced during follow-up appointments.
In conclusion, understanding heat rash is crucial for healthcare professionals to provide comprehensive care and management to patients. By recognizing the causes, signs, and symptoms of heat rash, healthcare providers can offer preventive measures, effective treatments, and ongoing patient education. Collaborative care, accurate documentation, and appropriate follow-up are key components in ensuring the optimal management and recovery of individuals with heat rash.