In this informative article, you’ll explore the essential nursing considerations and management strategies for hypercholesterolemia. We will delve into the vital role that nurses play in the care of patients with this condition, providing you with valuable insights and practical guidance. From understanding the risk factors and diagnostic procedures to implementing effective interventions and patient education, this article will equip you with the necessary knowledge to provide optimal care for individuals with hypercholesterolemia. So let’s dive in and explore the world of nursing considerations for this prevalent cardiovascular disorder.
Assessment
Patient history
When assessing a patient with hypercholesterolemia, it is important to gather a detailed patient history. This includes asking about the patient’s personal and family medical history, as well as any lifestyle factors that may contribute to high cholesterol levels. Additionally, it is important to inquire about any current medications or supplements the patient may be taking, as these can also affect cholesterol levels. By understanding the patient’s history, healthcare providers can better tailor their treatment plan and interventions to address the specific needs of the individual.
Physical assessment
A thorough physical assessment should be performed on patients with hypercholesterolemia to identify any signs or symptoms that may be indicative of underlying complications associated with high cholesterol levels. This includes assessing vital signs such as blood pressure, heart rate, and respiratory rate. Additionally, providers should conduct a cardiovascular examination to assess for the presence of atherosclerosis or other related conditions. A neurological examination should also be performed to evaluate potential signs of cognitive impairment or peripheral neuropathy. By conducting a comprehensive physical assessment, healthcare providers can monitor the progress of the patient’s condition and make necessary adjustments to their treatment plan.
Laboratory tests
Laboratory tests are essential for diagnosing and monitoring hypercholesterolemia. A lipid profile, consisting of measurements of total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides, should be obtained to assess the patient’s cholesterol levels. This provides crucial information for determining the appropriate course of treatment and assessing the patient’s response to interventions. Liver function tests should also be performed regularly to monitor for potential medication-induced liver damage. Additionally, muscle enzyme levels, such as creatine kinase, should be monitored to assess for muscle-related side effects of certain cholesterol-lowering medications. Regular laboratory testing is crucial for guiding treatment decisions and ensuring patient safety.
Education and Counseling
Dietary modifications
One of the key components of managing hypercholesterolemia is making dietary modifications. Patients should be educated about the negative impact of high-fat and high-cholesterol foods on their cholesterol levels. Encourage them to consume a diet that is low in saturated and trans fats and high in fruits, vegetables, whole grains, and lean proteins. They should also be educated about the importance of portion control and reading food labels. By providing patients with the necessary knowledge and support to make dietary changes, healthcare providers can empower them to take control of their cholesterol levels.
Importance of medication compliance
Medication compliance is essential for effectively managing hypercholesterolemia. Patients should be educated about the benefits of taking their prescribed medications as directed and the potential consequences of non-compliance. They should be informed about the specific medications they are prescribed, including their mechanisms of action and potential side effects. Patients should be encouraged to ask questions and voice any concerns they may have. By emphasizing the importance of medication compliance and addressing any barriers patients may face, healthcare providers can help ensure the effectiveness of the treatment plan.
Exercise recommendations
Regular physical activity is an important component of managing hypercholesterolemia. Patients should be educated about the benefits of exercise in improving cholesterol levels and overall cardiovascular health. Encourage them to engage in at least 150 minutes of moderate-intensity aerobic exercise per week, or 75 minutes of vigorous-intensity exercise. Additionally, patients should be educated about incorporating strength training exercises into their routine. It is important to individualize exercise recommendations based on the patient’s abilities and preferences. By providing patients with exercise recommendations and support, healthcare providers can promote their overall well-being.
Stress management techniques
Stress can contribute to elevated cholesterol levels and negatively impact cardiovascular health. Patients with hypercholesterolemia should be educated about stress management techniques to help reduce their overall stress levels. This may include techniques such as deep breathing exercises, mindfulness meditation, physical activity, and engaging in activities they enjoy. Patients should also be encouraged to seek support from friends, family, or professional counselors if needed. By providing patients with stress management techniques, healthcare providers can help them effectively cope with stress and improve their cardiovascular health.
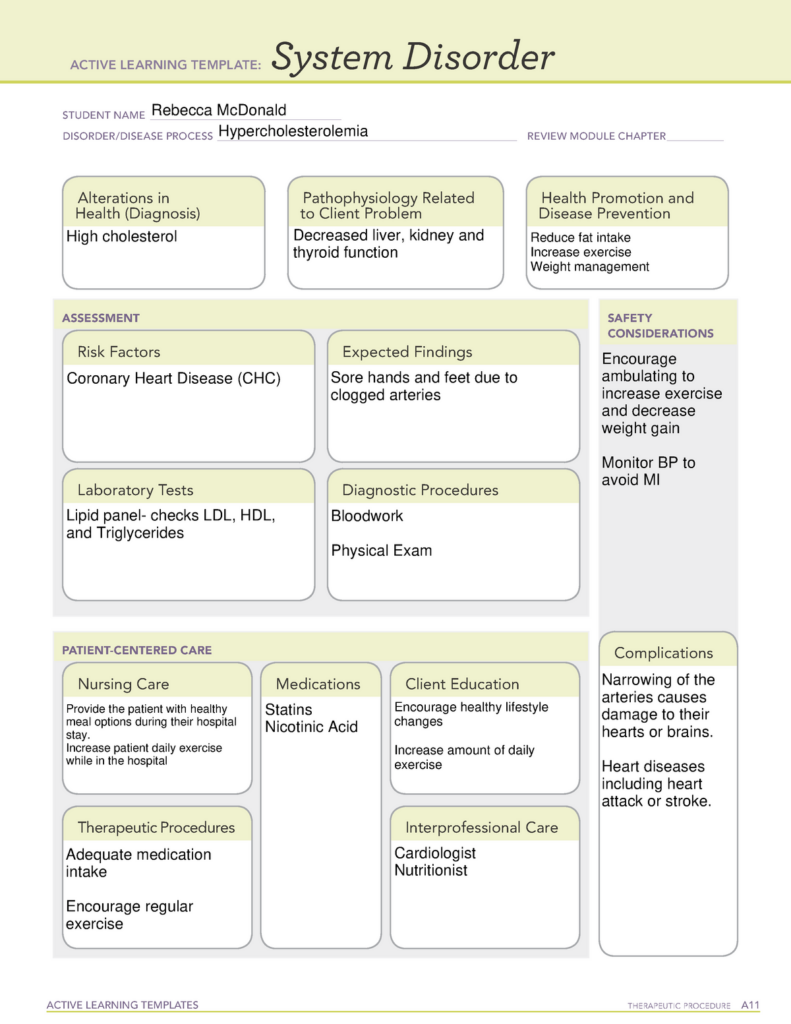

Medication Management
Statins
Statins are commonly prescribed as a first-line pharmacological treatment for hypercholesterolemia. Healthcare providers should educate patients about the benefits of statins in lowering LDL cholesterol and reducing the risk of cardiovascular events. It is important to inform patients about potential side effects, such as muscle pain and liver function abnormalities, and the importance of reporting any symptoms to their healthcare provider. Regular monitoring of lipid levels and liver function is crucial when patients are on statin therapy to ensure the medication’s effectiveness and safety. By educating patients about statins, healthcare providers can ensure optimal medication management.
Other lipid-lowering medications
In some cases, statins alone may not be sufficient to achieve optimal cholesterol levels. Additional lipid-lowering medications, such as bile acid sequestrants, cholesterol absorption inhibitors, and PCSK9 inhibitors, may be prescribed. Healthcare providers should educate patients about these medications, including their mechanisms of action, potential side effects, and monitoring requirements. It is important for patients to understand the importance of medication compliance and reporting any adverse reactions to their healthcare provider. By providing comprehensive education about lipid-lowering medications, healthcare providers can support patients in effectively managing their cholesterol levels.
Side effects and adverse reactions
Patients should be educated about the potential side effects and adverse reactions of cholesterol-lowering medications. This includes common side effects such as gastrointestinal disturbances, muscle pain, and headache, as well as more serious adverse reactions such as liver dysfunction or rhabdomyolysis. Healthcare providers should emphasize the importance of reporting any concerning symptoms to their healthcare provider promptly. By educating patients about potential side effects and adverse reactions, healthcare providers can ensure patient safety and early intervention if needed.
Monitoring medication effectiveness
Regular monitoring of medication effectiveness is essential when managing hypercholesterolemia. This includes performing lipid profile tests to assess the patient’s cholesterol levels and evaluating their response to medication therapy. Liver function tests should also be performed regularly to monitor for any medication-related adverse effects. Additionally, it is important to monitor muscle enzyme levels, such as creatine kinase, to assess for potential muscle-related side effects. By regularly monitoring medication effectiveness, healthcare providers can make appropriate adjustments to the treatment plan and ensure optimal patient outcomes.
Lifestyle Modifications
Dietary changes
In addition to education about dietary modifications, patients should be supported in making sustainable dietary changes. This may include providing resources such as meal plans, recipes, and information about healthier food alternatives. Encourage patients to make gradual changes and set realistic goals to improve long-term adherence. Additionally, ongoing support and follow-up are crucial to address any challenges or barriers patients may face in making dietary changes. By promoting dietary changes and offering ongoing support, healthcare providers can assist patients in adopting a heart-healthy diet.
Weight management
Weight management plays a significant role in managing hypercholesterolemia. Patients should be encouraged to achieve and maintain a healthy weight, as excess body weight contributes to elevated cholesterol levels and cardiovascular risk. Healthcare providers should provide education about the benefits of weight loss and strategies for achieving it, such as portion control, regular physical activity, and behavior modification techniques. Regular monitoring of weight and providing ongoing support are crucial to assist patients in achieving their weight loss goals. By addressing weight management, healthcare providers can significantly improve patient outcomes.
Physical activity
Regular physical activity is an important lifestyle modification for managing hypercholesterolemia. Patients should be encouraged to engage in aerobic exercise, such as walking, swimming, or cycling, for at least 30 minutes a day on most days of the week. Strength training exercises should also be included in their routine to improve overall cardiovascular fitness. It is important to individualize physical activity recommendations based on the patient’s abilities and preferences. Encourage patients to set realistic goals and provide ongoing support to help them maintain an active lifestyle. By promoting physical activity, healthcare providers can enhance patient well-being and cardiovascular health.
Smoking cessation
Smoking is a major risk factor for hypercholesterolemia and cardiovascular disease. Patients should be educated about the detrimental effects of smoking on their cholesterol levels and overall health. Healthcare providers should provide resources and support for smoking cessation, including information about nicotine replacement therapy, counseling services, and support groups. Patients should be reminded of the benefits of quitting smoking and the increased effectiveness of cholesterol-lowering interventions in non-smokers. By advocating for smoking cessation and providing resources, healthcare providers can significantly reduce cardiovascular risk in patients with hypercholesterolemia.
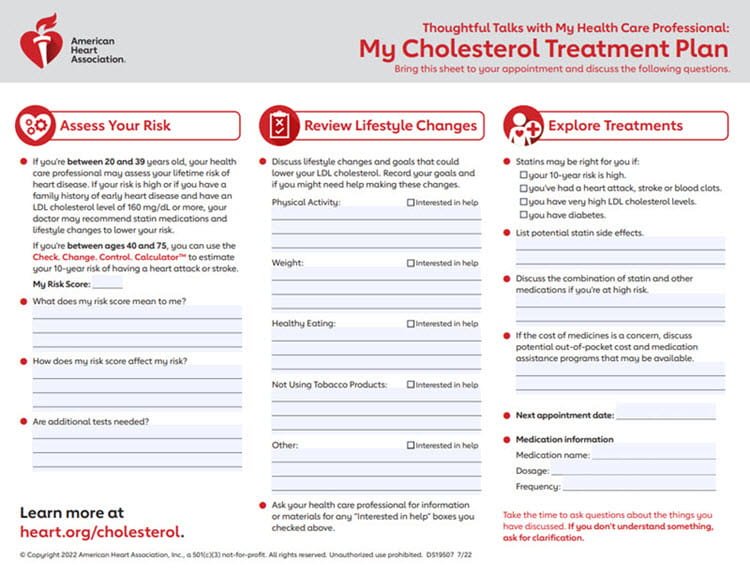

Patient Monitoring
Vital signs
Regular monitoring of vital signs is essential to assess the overall well-being and cardiovascular health of patients with hypercholesterolemia. This includes measuring blood pressure, heart rate, respiratory rate, and temperature. Monitoring vital signs provides valuable information about the patient’s response to treatment and can help identify any potential complications or adverse reactions. By regularly monitoring vital signs, healthcare providers can ensure early detection and prompt intervention if needed.
Lipid profile
Regular lipid profile testing is crucial for monitoring and managing hypercholesterolemia. This includes measuring total cholesterol, LDL cholesterol, HDL cholesterol, and triglyceride levels. Monitoring lipid levels allows healthcare providers to assess the effectiveness of interventions and make necessary adjustments to the treatment plan. Regular lipid profile testing also helps identify any underlying lipid abnormalities, such as familial hypercholesterolemia. By regularly monitoring lipid levels, healthcare providers can optimize patient management and reduce cardiovascular risk.
Liver function tests
Certain cholesterol-lowering medications can affect liver function, and regular monitoring of liver enzymes is important to ensure patient safety. Liver function tests, including serum transaminases and bilirubin levels, should be performed regularly. Monitoring liver function can help detect medication-induced liver damage and guide appropriate management decisions. By regularly monitoring liver function tests, healthcare providers can minimize the risk of medication-related adverse effects.
Muscle enzyme levels
Some cholesterol-lowering medications, such as statins, can cause muscle-related side effects. Monitoring muscle enzyme levels, specifically creatine kinase (CK), can help detect muscle damage or rhabdomyolysis. Patients should be educated about the signs and symptoms of muscle-related adverse effects, such as unexplained muscle pain, weakness, or dark urine, and the importance of reporting them promptly. By regularly monitoring muscle enzyme levels, healthcare providers can ensure patient safety and intervene early if necessary.
Collaborative Care
Consultation with healthcare team
Hypercholesterolemia management often involves a multidisciplinary approach, and collaboration with the healthcare team is vital. Healthcare providers should consult with other specialists, such as cardiologists and endocrinologists, to ensure comprehensive and coordinated care. Regular communication and sharing of patient information can help optimize treatment decisions and interventions. By collaborating with the healthcare team, providers can ensure that patients with hypercholesterolemia receive the best possible care.
Referral to dietitian or nutritionist
Patients with hypercholesterolemia can benefit from the expertise of a dietitian or nutritionist. Referring patients to these professionals can provide specialized dietary guidance and support to meet their individual needs. Dietitians or nutritionists can assist patients in developing personalized meal plans, providing education about food choices, and addressing any challenges or questions patients may have. By referring patients to dietitians or nutritionists, healthcare providers can enhance the efficacy of dietary interventions.
Coordinating with pharmacist
Pharmacists play an important role in medication management for patients with hypercholesterolemia. Healthcare providers should coordinate with pharmacists to ensure appropriate prescribing, monitoring, and patient education. Pharmacists can provide valuable information about medication interactions, side effects, and monitor for potential drug-drug interactions. By coordinating care with pharmacists, providers can optimize medication management and enhance patient safety.
Referral to support groups or counseling services
Living with hypercholesterolemia can be challenging, and patients may benefit from the support of others going through similar experiences. Referring patients to support groups or counseling services can provide emotional support and practical guidance. Support groups allow patients to share their experiences, exchange information, and learn coping strategies. Counseling services can provide additional support for managing stress, anxiety, or depression related to the diagnosis and management of hypercholesterolemia. By referring patients to support groups or counseling services, healthcare providers can address the unique psychosocial needs of patients with hypercholesterolemia.

Complications and Risk Factors
Atherosclerosis
Hypercholesterolemia is a major risk factor for the development of atherosclerosis, a condition characterized by the buildup of plaque in the arteries. Healthcare providers should educate patients about the link between high cholesterol levels and atherosclerosis, as well as the potential complications, such as heart attacks and strokes. Emphasize the importance of cholesterol control in reducing the risk of atherosclerosis and its associated complications. Regular monitoring and appropriate interventions are crucial to manage this risk factor effectively.
Cardiovascular disease
Hypercholesterolemia is strongly associated with the development of cardiovascular disease, including coronary artery disease, peripheral artery disease, and stroke. Patients should be educated about the increased risk of cardiovascular events and the importance of cholesterol control in reducing this risk. Healthcare providers should closely monitor patients with hypercholesterolemia for signs and symptoms of cardiovascular disease and intervene promptly. By addressing this risk factor and optimizing cholesterol management, healthcare providers can significantly reduce the incidence and progression of cardiovascular disease.
Diabetes
Hypercholesterolemia is frequently seen in individuals with diabetes, and the presence of both conditions significantly increases the risk of cardiovascular events. Patients with hypercholesterolemia and diabetes should receive comprehensive education and management for both conditions. Healthcare providers should emphasize the importance of tight glycemic control and cholesterol management in reducing the risk of cardiovascular complications. Regular monitoring of both cholesterol and blood glucose levels is necessary to optimize treatment outcomes and prevent complications.
Hypertension
Hypertension frequently coexists with hypercholesterolemia and significantly contributes to the risk of cardiovascular disease. Healthcare providers should assess and manage blood pressure levels in patients with hypercholesterolemia and provide education about the importance of blood pressure control. Lifestyle modifications, including dietary changes, regular exercise, and stress management, play a crucial role in managing both hypercholesterolemia and hypertension. Medication management should be individualized to address both conditions effectively.
Patient Safety
Preventing falls
Hypercholesterolemia management often involves medication therapy, and certain cholesterol-lowering medications can increase the risk of falls, especially in the elderly. Healthcare providers should assess patients’ fall risk and implement strategies to prevent falls, such as counseling patients about potential side effects and providing recommendations for modifications to the home environment. By prioritizing fall prevention and patient safety, healthcare providers can reduce the risk of injury and promote optimal patient outcomes.
Monitoring for medication interactions
Patients with hypercholesterolemia may have other comorbidities, requiring multiple medications. Healthcare providers should be vigilant in assessing medication interactions and potential adverse effects. Regular medication reviews can help identify possible interactions and ensure the safe and effective use of medications. Patients should be educated about the importance of informing their healthcare provider about all prescribed and over-the-counter medications they are taking. By monitoring for medication interactions, healthcare providers can reduce the risk of adverse effects and optimize treatment outcomes.
Educating patients on potential risks
Patients with hypercholesterolemia should be educated about potential risks associated with their condition and treatment. This includes educating them about the risk of cardiovascular events, potential side effects of medication, and the importance of early intervention for any concerning symptoms. Patients should be encouraged to seek medical attention promptly if they experience chest pain, shortness of breath, or any other symptoms of cardiovascular disease. By providing comprehensive education on potential risks, healthcare providers can empower patients to take an active role in their health and seek appropriate care when needed.
Promoting adherence to treatment plan
Adherence to the treatment plan is crucial for effectively managing hypercholesterolemia. Healthcare providers should provide education and support to help patients understand the importance of following their prescribed treatment regimen, including taking medications as directed, making dietary changes, engaging in regular physical activity, and attending follow-up appointments. Regularly assessing and addressing any barriers to adherence can help improve patient outcomes. By promoting adherence to the treatment plan, healthcare providers can optimize cholesterol management and reduce the risk of complications.

Cultural Considerations
Understanding cultural beliefs and practices
Healthcare providers should be culturally sensitive and respectful of the diverse beliefs and practices of their patients with hypercholesterolemia. Recognize that cultural factors may influence dietary preferences, lifestyle choices, and healthcare decisions. Take the time to understand and address any cultural beliefs that may impact the patient’s willingness or ability to make necessary lifestyle modifications or adhere to treatment recommendations. By embracing cultural diversity and tailoring care accordingly, healthcare providers can build trust and promote patient-centered care.
Respecting dietary preferences and restrictions
Dietary preferences and restrictions are deeply rooted in cultural and religious practices. Healthcare providers should respect and accommodate their patients’ dietary preferences and restrictions as much as possible when providing dietary recommendations for managing hypercholesterolemia. It is important to provide culturally appropriate alternatives and suggestions that align with the patient’s beliefs. This approach fosters patient autonomy and increases the likelihood of long-term adherence to dietary changes.
Language barriers and communication assistance
Language barriers can impede effective communication between healthcare providers and patients with hypercholesterolemia. Healthcare providers should identify any language barriers and provide appropriate communication assistance, such as interpreter services or multilingual educational materials. Clear communication is essential to ensure that patients understand their condition, treatment plan, and potential risks. By addressing language barriers, healthcare providers can facilitate effective communication and promote patient engagement and understanding.
Health literacy and education level
Health literacy levels and education levels can significantly impact a patient’s understanding and ability to manage hypercholesterolemia. Healthcare providers should assess the patient’s health literacy and education levels and provide information in a clear and concise manner using plain language. Visual aids, written materials, and teach-back techniques can enhance patient comprehension. By tailoring education to the patient’s health literacy and education level, healthcare providers can empower patients to actively participate in their care and make informed decisions.
Patient Advocacy
Ensuring patient rights and autonomy
Patient advocacy is a fundamental role of healthcare providers when caring for patients with hypercholesterolemia. This includes respecting and protecting the patient’s rights and autonomy. Healthcare providers should ensure that patients are fully informed about their condition, treatment options, and potential risks. Patients should be actively involved in the decision-making process and have the opportunity to ask questions and voice their concerns. By advocating for patient rights and autonomy, healthcare providers can build trust, promote patient-centered care, and enhance treatment outcomes.
Assisting in accessing healthcare resources
Navigating the healthcare system can be challenging for patients with hypercholesterolemia. Healthcare providers should assist patients in accessing appropriate healthcare resources, including specialist consultations, diagnostic tests, and support services. This requires providing guidance and support to help patients understand the healthcare system, access necessary services, and overcome any barriers they may face. By assisting patients in accessing healthcare resources, healthcare providers can ensure continuity of care and optimize patient outcomes.
Advocating for patient needs and concerns
Healthcare providers should actively advocate for their patients with hypercholesterolemia, ensuring that their needs and concerns are addressed. This includes advocating for adequate access to healthcare services, medications, and support resources. Healthcare providers can act as a voice for their patients, advocating for the necessary interventions and support to manage their condition effectively. By advocating for patient needs and concerns, healthcare providers can help patients navigate the complexities of hypercholesterolemia management and achieve optimal health outcomes.
Supporting patient in decision-making process
Shared decision-making is crucial when managing hypercholesterolemia. Healthcare providers should support patients in the decision-making process, providing them with information about treatment options, potential risks, and benefits. Patients should be encouraged to actively participate in their care, ask questions, and express their preferences and concerns. By supporting patients in the decision-making process, healthcare providers can foster a therapeutic partnership, improve patient satisfaction, and promote patient-centered care.
In conclusion, the nursing considerations for hypercholesterolemia encompass a comprehensive approach to patient management, including assessment, education and counseling, medication management, lifestyle modifications, patient monitoring, collaborative care, complications and risk factors, patient safety, cultural considerations, and patient advocacy. By addressing each of these areas, healthcare providers can optimize patient outcomes, reduce cardiovascular risk, and provide patient-centered care for individuals with hypercholesterolemia.