In the rapidly evolving landscape of medical advancements, the diagnosis and treatment of acute pancreatitis have seen remarkable progress in recent years. This article explores the modern era’s exciting developments in diagnosing and treating acute pancreatitis. From innovative diagnostic techniques to novel treatment options, the medical community has made significant strides in improving outcomes for individuals suffering from this condition. Join us as we delve into the fascinating world of acute pancreatitis and uncover the groundbreaking advancements that are shaping its diagnosis and treatment.
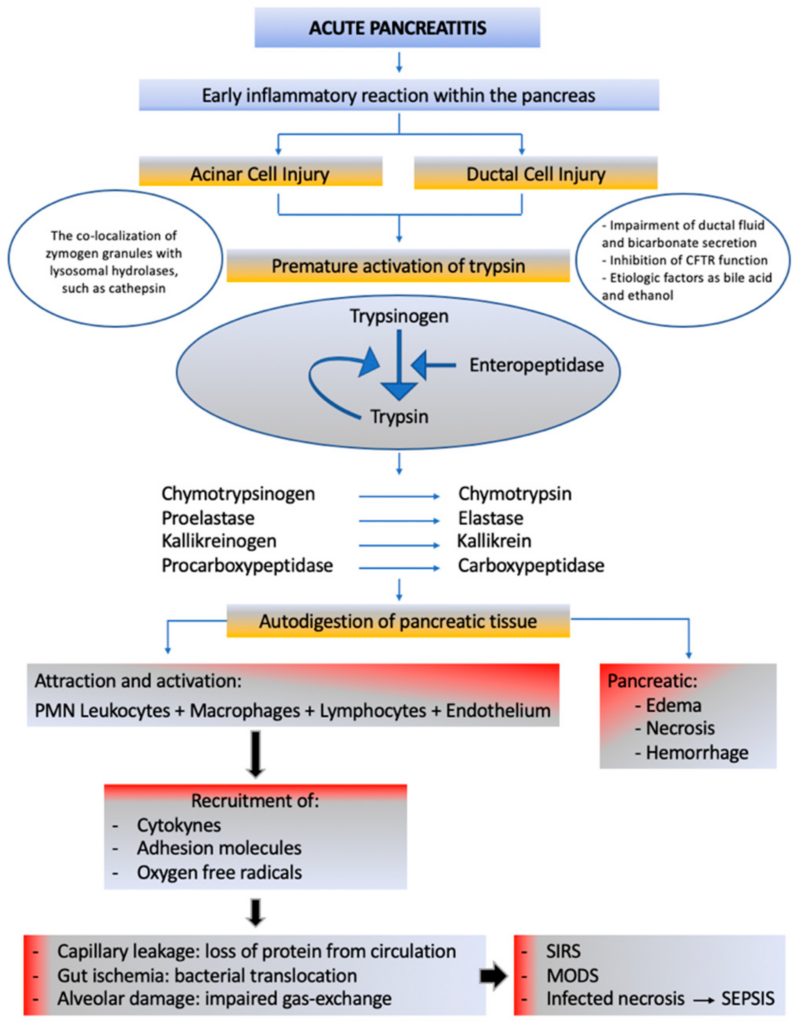
Pathophysiology of Acute Pancreatitis
Inflammatory pathway
Acute pancreatitis is characterized by inflammation of the pancreas, which can be caused by various factors such as gallstones, alcohol abuse, or certain medications. The inflammatory pathway begins with an initial insult to the pancreas, triggering the activation of inflammatory cells and the release of pro-inflammatory mediators. This inflammatory response leads to tissue damage and the subsequent release of pancreatic enzymes.
Role of pancreatic enzymes
Pancreatic enzymes play a crucial role in the development and progression of acute pancreatitis. Normally, these enzymes are produced by the pancreas and are released into the small intestine to aid in digestion. However, in cases of acute pancreatitis, these enzymes become activated within the pancreas itself, leading to autodigestion of the pancreatic tissue. This autodigestion further perpetuates the inflammatory response, causing more tissue damage and exacerbating the disease.
Activation of immune response
The activation of the immune response is an integral part of the pathophysiology of acute pancreatitis. As pancreatic enzymes leak into the surrounding tissues, they trigger an immune response, attracting immune cells to the site of inflammation. The immune cells, such as neutrophils and macrophages, release additional pro-inflammatory mediators, amplifying the inflammatory cascade. This immune response not only contributes to tissue damage but also plays a role in the systemic manifestations of acute pancreatitis.
Clinical Presentation
Abdominal pain
Abdominal pain is the hallmark symptom of acute pancreatitis. The pain is usually severe, constant, and located in the upper abdomen, often radiating to the back. The pain may be aggravated by eating or lying flat and can last for several days. It is important to note that not all abdominal pain is due to acute pancreatitis, and other conditions should be considered in the differential diagnosis.
Nausea and vomiting
Nausea and vomiting are common symptoms seen in patients with acute pancreatitis. These symptoms may be a result of the inflammatory response affecting the normal functioning of the gastrointestinal tract. Additionally, the release of pancreatic enzymes into the bloodstream can cause irritation to the stomach, leading to nausea and vomiting.
Fever and chills
Fever and chills may accompany acute pancreatitis, particularly if there is an associated infection or systemic inflammatory response. The fever is often low-grade, but it can persist if there are complications such as pancreatic abscess or infected necrotic tissue. Chills are usually experienced along with the fever and are a result of the body’s response to the infection or inflammation.

Diagnostic Modalities
Imaging studies
Imaging studies play a crucial role in the diagnosis and evaluation of acute pancreatitis. Computed tomography (CT) scan is the most commonly used imaging modality, as it can provide detailed information about the extent of pancreatic inflammation, the presence of complications such as necrosis or pseudocysts, and any structural abnormalities. Magnetic resonance imaging (MRI) and endoscopic ultrasound (EUS) are also valuable imaging techniques that may be used in specific cases.
Laboratory tests
Laboratory tests help in the diagnosis and assessment of acute pancreatitis. Blood tests, such as amylase and lipase levels, are commonly measured as they are often elevated in cases of acute pancreatitis. However, it is important to note that these tests are not specific to pancreatitis and can be influenced by other factors. Other laboratory tests, such as liver function tests and complete blood count, may also be performed to assess the severity of the disease and screen for any associated complications.
Endoscopic retrograde cholangiopancreatography (ERCP)
Endoscopic retrograde cholangiopancreatography (ERCP) is both a diagnostic and therapeutic procedure that may be performed in selected cases of acute pancreatitis. It involves the insertion of a flexible endoscope into the duodenum to visualize the pancreatic and bile ducts. ERCP can be used to identify the cause of acute pancreatitis, such as gallstones or strictures, and to perform interventions such as stone removal or stent placement.
Scoring Systems for Severity Assessment
Ranson’s criteria
Ranson’s criteria are a set of clinical and laboratory parameters used to assess the severity of acute pancreatitis and predict patient outcomes. These criteria include various factors such as age, white blood cell count, blood glucose level, and serum lactate dehydrogenase. The presence of multiple criteria indicates a higher risk of complications and a worse prognosis.
Balthazar scoring system
The Balthazar scoring system is a radiological scoring system that evaluates the severity of acute pancreatitis based on findings from a CT scan. It takes into account factors such as the extent of pancreatic necrosis, peripancreatic fluid collections, and the presence of complications. The higher the Balthazar score, the more severe the pancreatitis and the greater the risk of adverse outcomes.
Acute Physiology and Chronic Health Evaluation (APACHE) II score
The APACHE II score is a widely used scoring system to assess the severity of various critical illnesses, including acute pancreatitis. It takes into account various physiological parameters such as vital signs, laboratory values, and the presence of organ dysfunction. A higher APACHE II score indicates a greater severity of disease and a higher risk of mortality.
Early Management of Acute Pancreatitis
Fluid resuscitation
Fluid resuscitation is a cornerstone of the early management of acute pancreatitis. Patients with acute pancreatitis often experience intravascular fluid depletion due to the third spacing of fluids and ongoing inflammation. Intravenous fluids, such as crystalloids, are administered to restore and maintain adequate circulating blood volume. The goal is to prevent hypovolemia, maintain organ perfusion, and support overall patient stability.
Pain management
The management of pain in acute pancreatitis is essential to provide comfort and aid in patient recovery. Pain medications such as opioids may be used to control severe pain. Nonsteroidal anti-inflammatory drugs (NSAIDs) may also be used, although caution should be exercised in patients with renal impairment or bleeding tendencies. Pain management may involve a multimodal approach, combining pharmacological interventions with non-pharmacological techniques such as relaxation and positioning.
Nutritional support
In the early stages of acute pancreatitis, patients are often kept nil per os (NPO) to reduce pancreatic stimulation and allow the pancreas to rest. However, as the condition improves, enteral nutrition is gradually introduced to meet the patient’s nutritional needs. Enteral nutrition, delivered via nasogastric or nasojejunal tubes, is preferred over parenteral nutrition as it helps maintain gut integrity, reduces the risk of infections, and improves patient outcomes.
Complications of Acute Pancreatitis
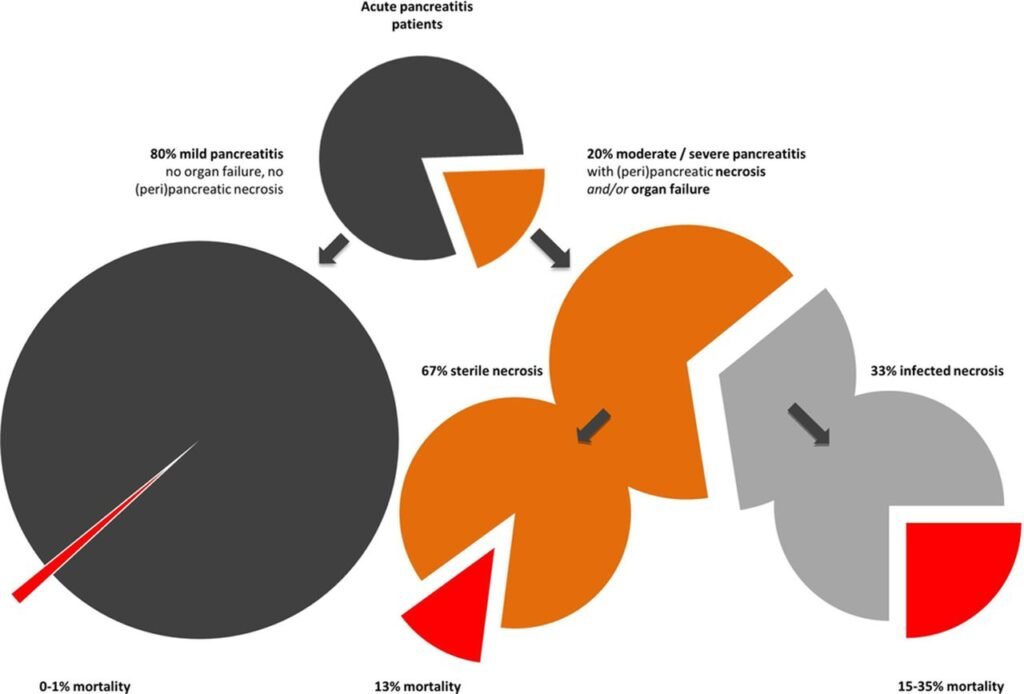
Pancreatic necrosis
Pancreatic necrosis refers to the death of pancreatic tissue, which can occur as a complication of severe acute pancreatitis. It is associated with a high risk of infection and is a major determinant of patient outcomes. Pancreatic necrosis often requires intervention, such as debridement and drainage, to remove the necrotic tissue and prevent complications such as abscess formation.
Pseudocyst formation
Pseudocysts are fluid-filled sacs that develop as a result of inflammation and tissue damage in acute pancreatitis. They usually occur within 4-6 weeks after the onset of pancreatitis and can be detected by imaging studies. While some pseudocysts resolve spontaneously, others may persist and require drainage or surgical intervention if they cause symptoms, become infected, or lead to complications such as rupture or fistula formation.
Pancreatic abscess
A pancreatic abscess is a serious complication that can arise from infected pancreatic necrosis or pseudocysts. It is characterized by the formation of a localized collection of pus within or near the pancreas. Pancreatic abscesses are associated with a high mortality rate and often require surgical intervention, such as drainage and debridement, in addition to antibiotic therapy.

Advanced Imaging Techniques
Magnetic resonance imaging (MRI)
Magnetic resonance imaging (MRI) is a valuable tool in the evaluation of acute pancreatitis. It provides detailed images of the pancreas and surrounding structures, allowing for the detection and characterization of complications such as necrosis, pseudocysts, or abscesses. MRI can also be used to monitor the response to treatment and guide further management decisions.
Endoscopic ultrasound (EUS)
Endoscopic ultrasound (EUS) combines endoscopy and ultrasound to provide highly detailed images of the pancreas and adjacent structures. EUS is particularly useful in detecting small pseudocysts or early necrosis that may not be visible on other imaging modalities. It can also be used to guide interventions such as fine-needle aspiration or cystic fluid drainage.
Computed tomography (CT) angiography
CT angiography is a specialized form of CT scan that focuses on the visualization of blood vessels within the pancreas and surrounding areas. It can provide valuable information about vascular complications of acute pancreatitis, such as pseudoaneurysm formation or thrombosis. CT angiography helps guide further management decisions and may be useful in planning surgical interventions or endovascular procedures.
Endoscopic Intervention
Endoscopic retrograde cholangiopancreatography (ERCP)
Endoscopic retrograde cholangiopancreatography (ERCP) is not only a diagnostic tool but also a therapeutic intervention in acute pancreatitis. It allows for direct visualization of the pancreatic duct and the bile ducts, facilitating the identification and treatment of the underlying cause of acute pancreatitis, such as gallstones or strictures. ERCP also enables interventions such as stone removal, stent placement, or sphincterotomy.
Endoscopic necrosectomy
Endoscopic necrosectomy is a minimally invasive procedure used to remove necrotic tissue from the pancreas. It involves the insertion of an endoscope into the pancreatic cavity, followed by the use of specialized instruments to break up and remove the necrotic material. Endoscopic necrosectomy can be an effective alternative to surgical intervention in selected cases, reducing the morbidity and mortality associated with open surgery.
Stent placement
Stent placement is a therapeutic intervention used in acute pancreatitis to relieve obstruction of the pancreatic or bile ducts. In cases of acute pancreatitis caused by gallstones or strictures, stents may be placed during ERCP procedures to restore normal bile and pancreatic flow. Stents can help alleviate symptoms, prevent complications, and promote healing of the pancreatic tissue.

Surgical Management of Acute Pancreatitis
Debridement and drainage of pancreatic necrosis
Surgical debridement and drainage of pancreatic necrosis may be necessary in cases of severe acute pancreatitis with extensive necrosis or infected necrotic tissue. This procedure involves the removal of necrotic material from the pancreas and the creation of drainage channels to help evacuate debris and infected fluid. Surgical debridement and drainage should be performed by experienced surgeons in specialized centers to minimize complications and optimize patient outcomes.
Pancreatic resection
Pancreatic resection is a surgical procedure that involves the removal of a portion of the entire pancreas. It may be considered in cases of severe acute pancreatitis with extensive necrosis, complications such as abscesses or hemorrhage, or in the presence of underlying pancreatic malignancy. Pancreatic resection is a complex procedure that requires careful patient selection and should be performed by experienced surgeons in specialized centers.
Laparoscopic approaches
Laparoscopic approaches to the management of acute pancreatitis, such as laparoscopic debridement or drainage, have gained popularity in recent years. These minimally invasive procedures offer the advantages of smaller incisions, reduced postoperative pain, shorter hospital stays, and faster recovery compared to traditional open surgery. However, laparoscopic approaches require expertise and careful patient selection, as they may not be suitable for all cases of acute pancreatitis.
Novel Therapeutic Approaches
Enzyme replacement therapy
Enzyme replacement therapy involves the administration of exogenous pancreatic enzymes to supplement the deficiency caused by acute pancreatitis. This therapy helps improve digestion and nutrient absorption, particularly in patients with pancreatic insufficiency. Enzyme replacement therapy can help alleviate symptoms such as abdominal pain, steatorrhea (fatty stools), and malnutrition.
Anti-inflammatory agents
Anti-inflammatory agents, such as corticosteroids or specific cytokine inhibitors, have been investigated as potential therapeutic options in acute pancreatitis. These agents aim to modulate the inflammatory response and reduce the severity of tissue damage. However, the use of anti-inflammatory agents in acute pancreatitis remains controversial, and their efficacy and safety need to be further evaluated through well-designed clinical trials.
Stem cell therapy
Stem cell therapy holds promise as a novel approach in the treatment of acute pancreatitis. Mesenchymal stem cells, derived from various sources such as bone marrow or adipose tissue, have shown potential in modulating the inflammatory response, promoting tissue repair, and improving pancreatic function. However, further research is needed to determine the optimal source of stem cells, the mode of administration, and their long-term effects in the management of acute pancreatitis.
Acute pancreatitis is a complex condition with a multifactorial pathophysiology and a wide range of clinical presentations. Early diagnosis and appropriate management are crucial to prevent complications and improve patient outcomes. Advances in diagnostic modalities, scoring systems, imaging techniques, endoscopic interventions, surgical approaches, and novel therapeutic options have significantly contributed to the modern era of acute pancreatitis management. With ongoing research and advancements in the field, the hope is to further refine and personalize the management of this challenging disease.
Watch This Video Below
Related Terms About Acute Pancreatitis in the Modern Era Advancements in Diagnosis and Treatment
Acute Pancreatitis Diagnosis And Treatment, Acute Pancreatitis Symptoms Diagnosis And Management, Acute Pancreatitis Treatment Algorithm, Acute Pancreatitis Treatment Guidelines, Chronic Acute Pancreatitis Diagnosis, Diagnosis And Treatment Of Acute Pancreatitis, How To Diagnose Acute Pancreatitis, Most Specific Diagnostic Test For Acute Pancreatitis