Living with Chronic Obstructive Pulmonary Disease (COPD) can be challenging, but with a few simple tips, you can lead a healthy and fulfilling life. COPD is a chronic respiratory condition that affects millions of people worldwide, causing symptoms such as shortness of breath, coughing, and wheezing. In this article, we will explore practical suggestions and lifestyle changes that can help manage COPD symptoms, improve lung function, and enhance overall well-being. With a positive mindset and a few adjustments to your daily routine, you can take control of your health and thrive despite living with COPD.
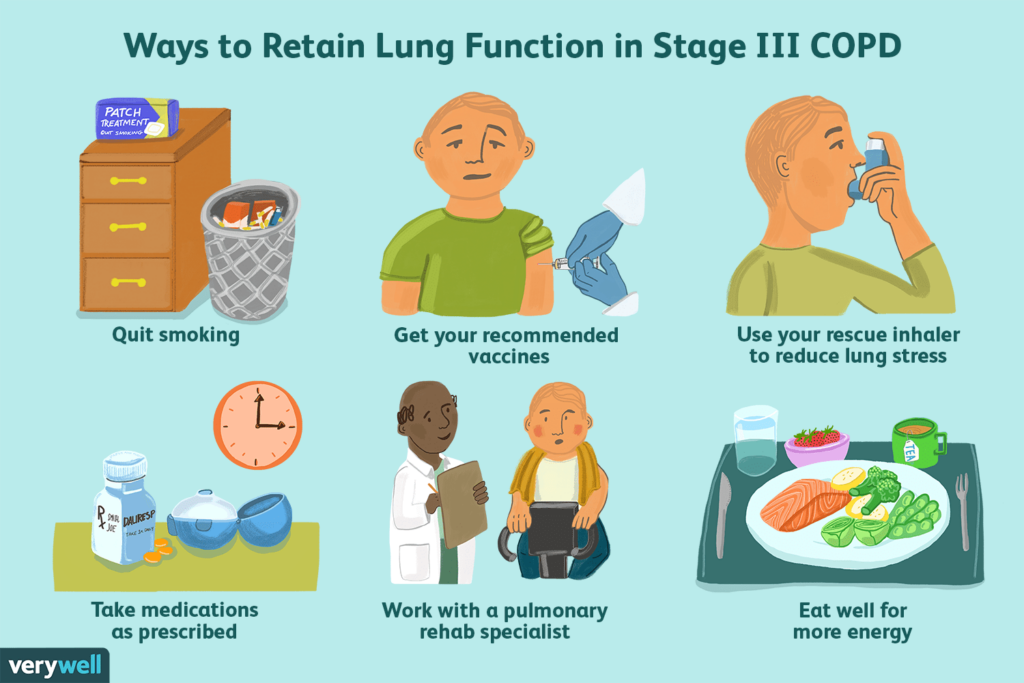
Understanding COPD
Definition of COPD
Chronic Obstructive Pulmonary Disease (COPD) is a chronic lung condition that gradually worsens over time. It is characterized by persistent airflow limitation, making it difficult for you to breathe properly. The two main conditions that fall under COPD are emphysema and chronic bronchitis. Emphysema causes damage to the air sacs in the lungs, while chronic bronchitis involves inflammation of the bronchial tubes. COPD is a progressive disease, meaning it cannot be cured, but with the right management and lifestyle changes, you can improve your quality of life and slow its progression.
Causes and risk factors
The primary cause of COPD is long-term exposure to harmful substances, particularly tobacco smoke, either through smoking or secondhand smoke. Other factors that can contribute to COPD include exposure to certain gases and chemicals in the workplace, air pollution, and a rare genetic condition called alpha-1 antitrypsin deficiency. It is important to note that not everyone who smokes will develop COPD, and some people who have never smoked can still develop the disease. Certain risk factors, such as a family history of COPD and respiratory infections, may increase your chances of developing the condition.
Symptoms of COPD
COPD symptoms may develop slowly and worsen over time. They can vary from person to person but commonly include shortness of breath, a persistent cough with mucus production, frequent chest infections, wheezing, fatigue, and unintended weight loss. You may also experience symptoms that affect your daily activities, such as difficulty climbing stairs, getting dressed, or participating in physical activities. Paying attention to these symptoms and seeking medical help early is crucial for effective management of COPD.
Diagnosing COPD
Medical history and physical examination
When you visit your healthcare provider with respiratory symptoms, they will start by taking a thorough medical history. They will ask you questions about your symptoms, medical conditions, and any risk factors you may have. They will also conduct a physical examination to assess your lung function, listen to your lungs, and check for signs of COPD, such as a prolonged expiratory phase or wheezing.
Lung function tests
To confirm a diagnosis of COPD, your healthcare provider will likely perform lung function tests, such as spirometry. Spirometry measures how much air you can inhale and exhale and how quickly you can exhale. This test helps determine the severity of COPD and assesses the extent of lung damage. Your healthcare provider may also order other lung function tests, such as a lung diffusion capacity test, to evaluate how well oxygen passes from your lungs into your bloodstream.
Chest X-rays and CT scans
In some cases, your healthcare provider may order imaging tests, such as chest X-rays or CT scans, to get a clearer picture of your lungs and rule out other possible conditions. These tests can help detect signs of emphysema, such as lung hyperinflation or bullae (large air-filled spaces), which are common in COPD.

Treatment options for COPD
Medications
Medications are an essential part of managing COPD symptoms and preventing exacerbations. Depending on the severity of your condition, your healthcare provider may prescribe bronchodilators to help relax and open your airways. These medications are usually inhaled through an inhaler or nebulizer. The most commonly prescribed bronchodilators are short-acting or long-acting beta-agonists and anticholinergics. In some cases, your healthcare provider may also recommend corticosteroids to reduce airway inflammation or antibiotics to treat respiratory infections.
Pulmonary rehabilitation
Pulmonary rehabilitation is a comprehensive program designed to improve your physical condition and quality of life if you have COPD. It involves a combination of exercise training, education, and counseling. Pulmonary rehabilitation can help you strengthen your breathing muscles, increase tolerance for exercise, and teach you techniques to manage breathlessness. These programs are typically conducted by a team of healthcare professionals, including respiratory therapists, physiotherapists, and psychologists.
Oxygen therapy
If your blood oxygen levels are low, your healthcare provider may prescribe oxygen therapy. Oxygen therapy involves the use of supplemental oxygen to improve your oxygen levels and relieve breathlessness. Depending on your needs, you might receive oxygen through a nose tube, a mask, or a portable device for activities outside your home. Follow your healthcare provider’s instructions carefully when using oxygen therapy.
Surgery
In severe cases of COPD, surgery may be an option. Surgical procedures such as lung volume reduction surgery or lung transplantation can help improve lung function and quality of life. Lung volume reduction surgery involves removing small wedges of damaged lung tissue to allow healthier lung tissue to expand. Lung transplantation is a complex procedure that involves replacing one or both diseased lungs with healthy lungs from a donor.
Lifestyle changes to manage COPD
Quit smoking
If you smoke, quitting is the most important step you can take to slow the progression of COPD and improve your overall health. Smoking cessation can be challenging, but there are various tools and resources available to support you. Talk to your healthcare provider about smoking cessation strategies, such as nicotine replacement therapy, medications, and counseling. Engage your friends and family for support, and consider joining a cessation program or support group.
Avoid exposure to irritants
Limit your exposure to irritants that can worsen COPD symptoms, such as secondhand smoke, air pollution, dust, chemicals, and fumes. If your workplace exposes you to harmful substances, speak with your employer about ways to reduce your exposure or explore alternative work arrangements. It is also important to be cautious about indoor air pollutants, such as cleaning products, strong odors, and pet dander, which can trigger symptoms. Use ventilation and air purifiers to improve the air quality in your home.
Maintain a healthy weight
Being overweight or underweight can make breathing more difficult and strain your respiratory muscles. Work with your healthcare provider to develop a healthy eating plan that supports your nutritional needs and maintains a healthy weight. A balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can provide the necessary nutrients to keep your body strong and support your lung function.
Adopt a healthy diet
In addition to maintaining a healthy weight, adopting a healthy diet can benefit your overall health and help manage COPD symptoms. Include foods that are rich in antioxidants, such as berries, leafy greens, and nuts, as they can help reduce inflammation in the lungs. Avoid foods that may trigger acid reflux, such as spicy or fatty foods, as acid reflux can worsen COPD symptoms.
Stay physically active
Regular physical activity can improve your breathing and overall fitness, even with COPD. Engage in activities that you enjoy and that are suitable for your condition, such as walking, swimming, or cycling. Start slowly and gradually increase your activity level, aiming for at least 30 minutes of moderate exercise most days of the week. If you experience breathlessness during exercise, use techniques like pursed-lip breathing or diaphragmatic breathing to manage your symptoms.
Manage stress
Living with COPD can be stressful, and stress can worsen your symptoms or trigger exacerbations. Find stress-management techniques that work for you, such as deep breathing exercises, meditation, yoga, or engaging in hobbies and activities that bring you joy. It is also helpful to reach out for emotional support from friends, family, or healthcare professionals who can provide guidance and help you cope with the challenges of living with COPD.

Creating a healthy home environment
Improving indoor air quality
Improving indoor air quality is crucial for individuals with COPD, as irritants and pollutants can trigger symptoms and exacerbate the condition. Keep your home well-ventilated by opening windows when weather permits. Use exhaust fans in the kitchen and bathroom to remove cooking fumes and moisture. Consider installing carbon monoxide detectors and fire alarms to ensure your safety.
Reducing allergens and pollutants
Take steps to reduce allergens and pollutants that can worsen COPD symptoms. Regularly clean your home to remove dust, pet dander, and other allergens. Use allergen-proof covers on your mattresses and pillows, and wash bedding regularly in hot water. Avoid using strong cleaning products and opt for natural or fragrance-free alternatives whenever possible.
Keeping a clean and dust-free home
Maintaining a clean and dust-free home can help minimize your exposure to irritants and pollutants. Vacuum frequently using a vacuum cleaner with a HEPA filter to trap dust and allergens. Dust surfaces with a damp cloth instead of dry dusting, as dry dusting can stir up particles into the air. Keep your pets well-groomed and minimize their access to areas where you spend most of your time.
Using air purifiers and humidifiers
Consider using air purifiers with HEPA filters to remove airborne particles and improve indoor air quality. Place air purifiers in commonly used rooms or areas where you spend a significant amount of time. Humidifiers can also be beneficial, especially in dry environments, as they add moisture to the air and help alleviate symptoms of dryness and irritation in the respiratory tract. Clean and maintain both air purifiers and humidifiers according to the manufacturer’s instructions to ensure their effectiveness.
Tips for managing breathlessness
Pursed-lip breathing technique
Pursed-lip breathing is a simple technique that can help you breathe more efficiently and reduce breathlessness during activities. To practice pursed-lip breathing, inhale slowly through your nose for a count of two, then purse your lips (as if you are blowing out a candle) and exhale slowly for a count of four. This technique helps to keep your airways open longer, preventing them from collapsing and allowing for more complete exhaling.
Practicing diaphragmatic breathing
Diaphragmatic breathing, also known as belly or abdominal breathing, helps you use your diaphragm and abdominal muscles to breathe more effectively. To practice diaphragmatic breathing, place one hand on your abdomen and the other on your chest. Breathe in slowly through your nose, allowing your abdomen to rise as you fill your lungs with air. Exhale slowly through pursed lips, and feel your abdomen fall as you release the air. Diaphragmatic breathing helps improve oxygen exchange, relaxes your breathing muscles, and reduces the effort of breathing.
Using breathing exercises
In addition to pursed-lip breathing and diaphragmatic breathing, there are various breathing exercises that can help manage breathlessness and improve your lung function. Your healthcare provider or pulmonary rehabilitation program can guide you in specific breathing exercises tailored to your condition. Some examples of breathing exercises include deep breathing, huff coughing, and inspiratory muscle training.
Using relaxation techniques
Relaxation techniques, such as meditation, guided imagery, and progressive muscle relaxation, can help alleviate anxiety and reduce breathlessness. These techniques promote a sense of calm and relaxation, making it easier to manage breathlessness during daily activities. Practice relaxation techniques regularly and find what works best for you to incorporate them into your COPD management routine.

Maintaining a regular exercise routine
Types of exercises suitable for COPD patients
Regular exercise is beneficial for individuals with COPD, as it helps improve lung function, increases stamina, and enhances overall well-being. Choose exercises that suit your physical abilities and preferences. Low-impact activities like walking, swimming, cycling, and tai chi can be particularly helpful for individuals with COPD. Consider activities that involve both aerobic exercise, which improves cardiovascular fitness, and strength training, which strengthens your muscles.
Importance of warm-up and cool-down exercises
Before starting any exercise, it is important to warm up your muscles and prepare your body for physical activity. Warm-up exercises, such as gentle stretching and light cardio, help increase blood flow to your muscles, loosen your joints, and raise your body temperature. A warm-up session should last approximately 5-10 minutes. Similarly, cooling down after exercise is crucial as it helps your body return to a resting state gradually. Cool-down exercises should involve gentle stretching and gradually decreasing the intensity of the exercise.
Guidelines for exercising with COPD
When exercising with COPD, it is important to follow some guidelines to ensure safety and maximize the benefits. Start with shorter exercise sessions and gradually increase the duration and intensity as you build up your fitness level. Pace yourself and listen to your body’s signals. If you experience shortness of breath or fatigue, take breaks and modify the activity as needed. It is important to stay hydrated during exercise and consume enough fluids. Consult with your healthcare provider or a pulmonary rehabilitation specialist before starting an exercise program to determine the most suitable exercises for your condition and receive proper guidance.
Managing exacerbations and flare-ups
Recognizing early signs of exacerbations
Exacerbations, or flare-ups, are periods when COPD symptoms worsen suddenly. It is important to recognize the early signs of exacerbations to prevent them from worsening and to seek prompt medical attention. Early signs may include increased breathlessness, increased coughing, change in the color or amount of mucus, fever, chest tightness, fatigue, and decreased exercise tolerance. Pay attention to these signs and symptoms and keep a record of them to share with your healthcare provider.
Having an action plan
Developing an action plan with your healthcare provider can help you manage exacerbations effectively. An action plan outlines what steps you should take in case of a flare-up, including when to increase or change medications, when to seek medical help, and what emergency contact numbers to have on hand. Follow your action plan closely and communicate any changes or concerns with your healthcare provider to ensure your COPD is well-managed.
Knowing when to seek medical help
If your symptoms worsen significantly or if you experience a sudden change in your condition, it is important to seek medical help immediately. Contact your healthcare provider or go to the nearest emergency department if you have severe shortness of breath, a rapid heart rate, confusion, bluish lips or fingernails, or if you are having trouble speaking in full sentences. These symptoms may indicate a severe exacerbation that requires immediate medical attention.

Coping with anxiety and depression
Understanding the emotional impact of COPD
Living with COPD can have a significant emotional impact on individuals, leading to feelings of anxiety, depression, frustration, and isolation. COPD symptoms can affect your ability to engage in activities you once enjoyed, cause breathlessness and fatigue, and disrupt your daily routine. Understanding and acknowledging the emotional impact of COPD is an important step towards finding ways to cope and improve your emotional well-being.
Seeking support from healthcare professionals
If you are experiencing anxiety or depression related to your COPD, it is beneficial to seek support from healthcare professionals, such as therapists or counselors. These professionals can provide you with tools and coping strategies to manage your emotions and adjust to the challenges of living with COPD. They can also help you develop strategies to improve your overall well-being and address any concerns or fears you may have.
Joining support groups
Joining support groups or participating in COPD-related communities can provide valuable emotional support. Connecting with others who have similar experiences and challenges can help you feel understood and less isolated. Support groups can offer a safe space to share your thoughts and feelings, learn from others, and gain valuable insights and coping strategies. Consider reaching out to local hospitals, community centers, or online resources to find support groups tailored for COPD patients in your area.
Seeking help and support
Working closely with healthcare providers
Managing COPD requires a collaborative effort between individuals and their healthcare providers. Regular follow-ups with your healthcare provider are crucial to monitor and adjust your treatment plan as needed. Be proactive in expressing any concerns or questions you may have during these visits. Be prepared to provide updates on your symptoms, any changes or exacerbations you have experienced, and any challenges you are facing in managing your condition. This collaborative approach ensures that your healthcare provider has a comprehensive understanding of your condition and can provide you with personalized care.
Involving family and friends in COPD management
Involving your family and friends in your COPD management can provide invaluable support and assistance. Share information about your condition with your loved ones so they can better understand the challenges you are facing. Educate them about COPD, its symptoms, and treatment options. Encourage open communication and ask for their help when needed, whether it’s with household chores, transportation, or emotional support. Together, you can create a strong support network that eases the burden of managing COPD.
Utilizing community resources
Communities often offer resources and services that can assist individuals with COPD. Contact local healthcare organizations, community centers, or support groups to inquire about available resources. These resources may include educational programs, exercise classes tailored for individuals with COPD, financial assistance programs, and additional support services. Utilizing community resources can provide you with valuable tools, information, and connections to others who understand and can support you in managing your condition.
Considering therapy and counseling
Therapy and counseling can be beneficial for individuals with COPD who are experiencing emotional distress or struggling to cope with the challenges of living with a chronic condition. Mental health professionals can provide you with a safe space to discuss your feelings, fears, and concerns, and help you develop coping strategies specific to your needs. Therapy and counseling can empower you to maintain a positive outlook, reduce stress and anxiety, and improve your overall well-being.
Living with COPD requires a comprehensive approach that combines medical treatment, lifestyle changes, and emotional support. With the right strategies and support in place, you can effectively manage COPD symptoms, slow its progression, and enjoy a fulfilling life. By understanding COPD, recognizing its symptoms, and implementing the recommended strategies, you are taking an important step towards a healthier life with COPD. Remember, you are not alone in this journey, and there are healthcare professionals, support groups, and resources available to help you every step of the way.