Living with COPD can be challenging, but with the right strategies in place, you can effectively manage your condition and enjoy a fulfilling life. In this article, you will discover practical tips and techniques that will help you navigate through the complexities of COPD. From lifestyle changes to proper medication administration, you will find invaluable advice that can empower you to take control of your health and enhance your overall well-being. So, let’s explore these tips together and make living with COPD a little bit easier and more manageable.

Understanding COPD
What is COPD?
Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung disease that makes it difficult for you to breathe. It is a long-term condition that worsens over time and affects millions of people worldwide. COPD is primarily characterized by a persistent cough, shortness of breath, wheezing, and chest tightness. It is a condition that requires lifelong management and can have a significant impact on your daily life.
Types of COPD
COPD can be categorized into two main types: chronic bronchitis and emphysema. Chronic bronchitis is characterized by inflammation and irritation of the bronchial tubes, which results in a chronic cough with mucus production. Emphysema, on the other hand, damages the air sacs in the lungs, making it difficult for oxygen to be efficiently absorbed into the bloodstream. Many individuals with COPD have a combination of chronic bronchitis and emphysema.
Causes and risk factors
The primary cause of COPD is long-term exposure to harmful particles or chemicals in the air. Cigarette smoke, both direct smoking and secondhand smoke, is the leading cause of COPD. Other risk factors include exposure to air pollution, dust, chemicals, and genetic factors. It’s important to be aware of these risk factors and take measures to protect yourself from them to reduce the chances of developing or worsening COPD.
Symptoms of COPD
The symptoms of COPD can vary from person to person, but the most common symptoms include a persistent cough, increased production of mucus, shortness of breath (especially during physical activity), wheezing, chest tightness, and frequent respiratory infections. These symptoms can significantly impact your daily life, making it harder to engage in activities and affecting your overall quality of life.
Diagnosis and Treatment
Diagnosing COPD
If you experience symptoms of COPD, it is crucial to seek medical attention for a proper diagnosis. A healthcare professional will evaluate your medical history, perform a physical examination, and conduct pulmonary function tests such as spirometry. Spirometry measures how much air you inhale and exhale, and how quickly you can exhale. This test can help determine the severity and progression of COPD.
Medical tests and evaluations
In addition to spirometry, your healthcare provider may also order other medical tests and evaluations to assess your lung function and overall health. These may include chest X-rays or CT scans, arterial blood gas analysis, exercise tolerance tests, and sputum analysis. These tests provide valuable information to guide your treatment plan and monitor the progression of the disease.
Medications for COPD
There are various medications available to manage COPD symptoms and improve lung function. Bronchodilators are commonly prescribed and work by relaxing the muscles around the airways, allowing them to open up and making it easier to breathe. There are short-acting bronchodilators for quick relief and long-acting bronchodilators for long-term management. Inhaled corticosteroids may also be prescribed to reduce inflammation in the airways. Your healthcare provider will determine the most appropriate medication regimen for you.
Other treatment options
In addition to medication, other treatment options for COPD include oxygen therapy, pulmonary rehabilitation, and lung surgery. Oxygen therapy provides supplemental oxygen to increase the level of oxygen in your blood. Pulmonary rehabilitation programs offer a comprehensive approach to managing COPD through exercise, education, and support. In severe cases, lung surgery may be considered, such as a lung volume reduction surgery or a lung transplant. These treatment options are typically reserved for individuals with advanced stages of COPD.
Importance of regular medical check-ups
Regular medical check-ups are essential for individuals with COPD. These check-ups allow healthcare professionals to monitor your lung function, track the progression of the disease, and make any necessary adjustments to your treatment plan. It is also an opportunity to discuss any new symptoms or concerns you may have and receive guidance on managing your condition effectively.
Lifestyle Changes
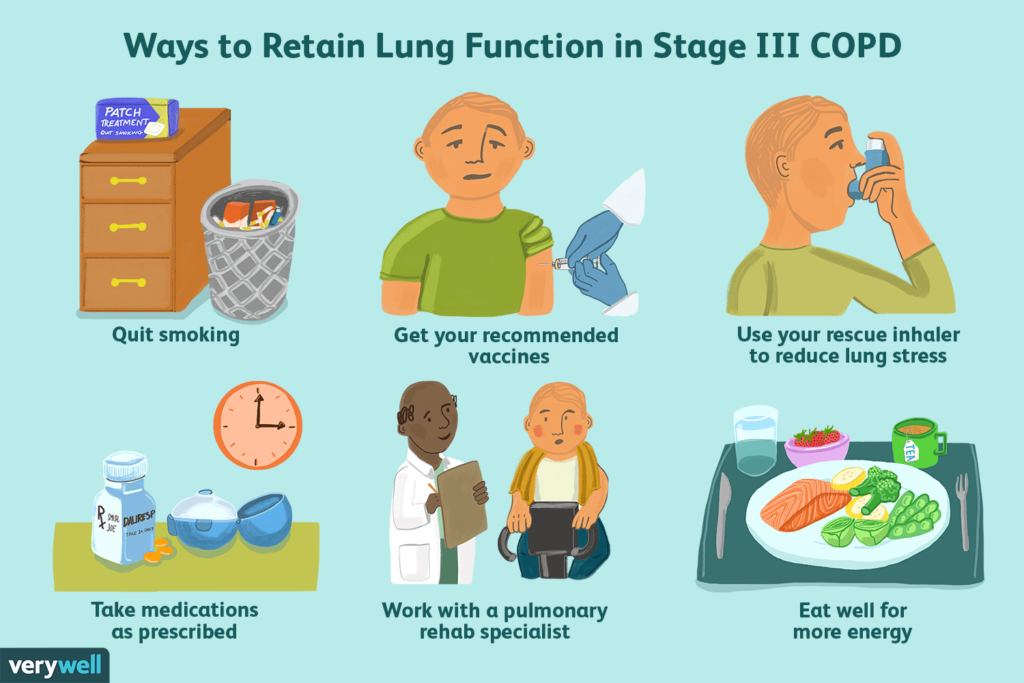
Quitting smoking
If you are a smoker and have been diagnosed with COPD, quitting smoking is the most crucial lifestyle change you can make to improve your lung health. Smoking cessation can slow down the progression of COPD and reduce symptoms. There are numerous resources available to help you quit smoking, including nicotine replacement therapy, counseling, support groups, and medications. Talk to your healthcare provider about the most effective strategies for quitting smoking.
Avoiding environmental triggers
In addition to quitting smoking, it is essential to avoid exposure to environmental triggers that can exacerbate your COPD symptoms. These triggers can include air pollution, allergens, chemicals, and extremes in temperature. Stay updated on air quality index reports and try to plan your outdoor activities when pollution levels are lower. Make sure your home is well-ventilated and free from irritants such as dust, pet dander, and mold.
Healthy eating for COPD
Maintaining a healthy diet can help support your overall health and manage the symptoms of COPD. Aim for a balanced diet that includes a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats. Certain foods, such as those rich in antioxidants and omega-3 fatty acids, may have anti-inflammatory properties and can be beneficial for individuals with COPD. Stay hydrated by drinking an adequate amount of water throughout the day.
Regular exercise and physical activity
Although it may seem counterintuitive, regular exercise and physical activity are essential for individuals with COPD. Engaging in exercise can improve lung function, strengthen the respiratory muscles, and increase overall endurance. Consult with your healthcare provider or a pulmonary rehabilitation specialist to develop an exercise routine that suits your abilities and preferences. Start with low-impact activities such as walking or swimming and gradually increase the intensity and duration as tolerated.
Managing stress and anxiety
Living with a chronic condition like COPD can be stressful, and it is vital to find healthy ways to manage stress and anxiety. Incorporate relaxation techniques such as deep breathing exercises, meditation, or yoga into your daily routine. Engage in activities that bring you joy and help you unwind. Seeking support from a mental health professional or joining a support group can also be beneficial in coping with the emotional challenges that may arise from living with COPD.
Breathing Techniques and Pulmonary Rehabilitation
Breathing exercises for COPD
Breathing exercises can be an effective way to improve lung function and manage COPD symptoms. Deep breathing exercises, pursed-lip breathing, and diaphragmatic breathing are common techniques that can help you breathe more efficiently and decrease shortness of breath. Your healthcare provider or a pulmonary rehabilitation specialist can guide you in performing these exercises properly and incorporate them into your daily routine.
Pulmonary rehabilitation programs
Pulmonary rehabilitation programs are comprehensive programs that focus on improving your overall physical and emotional well-being. These programs usually involve exercise training, education on COPD management, breathing techniques, nutritional counseling, and psychological support. Pulmonary rehabilitation can be done in a hospital setting, outpatient clinic, or even in the comfort of your own home with the guidance of healthcare professionals.
Using inhalers and other respiratory devices
Inhalers and other respiratory devices play a crucial role in managing COPD symptoms. They deliver medication directly to your lungs, providing quick relief or long-term control of symptoms. There are various types of inhalers available, including metered-dose inhalers, dry powder inhalers, and nebulizers. It is essential to learn how to use these devices correctly to ensure optimal medication delivery. Your healthcare provider or pharmacist can provide instructions and demonstrate the proper technique for using inhalers and other respiratory devices.
Managing Symptoms and Exacerbations
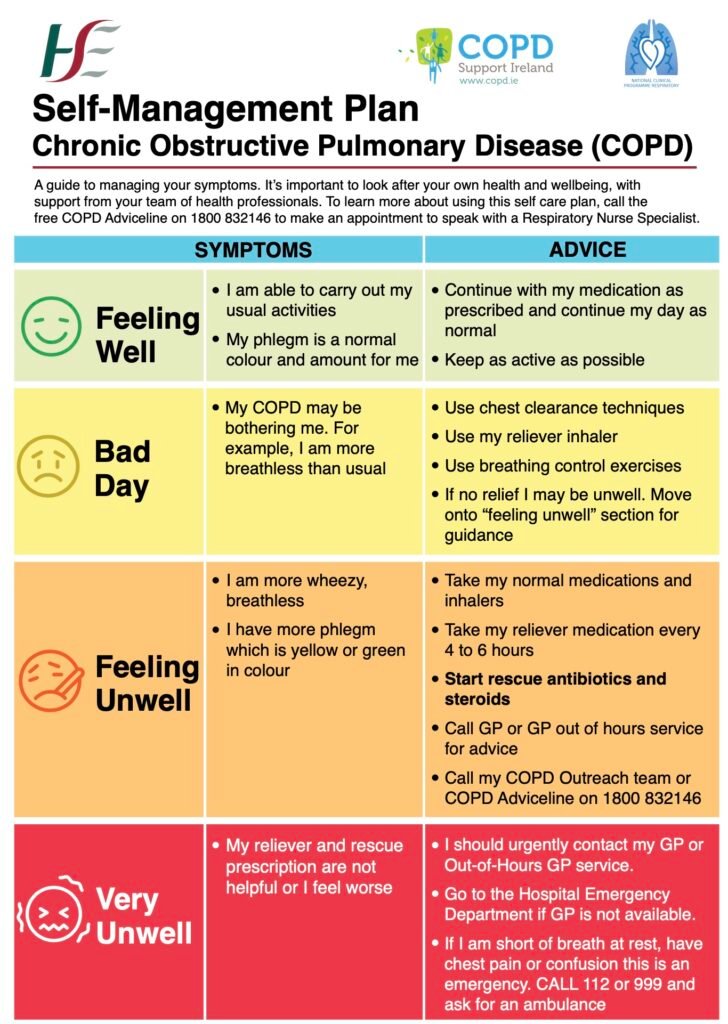
Recognizing and managing COPD symptoms
Understanding and recognizing COPD symptoms is essential for effective management. Pay attention to any changes in your breathing, cough, mucus production, or overall lung function. If you notice a worsening of symptoms, it is crucial to take action and implement your COPD management plan. This may include using rescue medication, practicing breathing exercises, and contacting your healthcare provider for further guidance.
Preventing exacerbations
Exacerbations are episodes of severe worsening of COPD symptoms, often triggered by respiratory infections, exposure to environmental irritants, or failure to adhere to treatment plans. To reduce the risk of exacerbations, practice good hand hygiene, stay up to date with vaccinations (including the flu and pneumonia vaccines), avoid close contact with sick individuals, and follow your treatment plan diligently. It is important to contact your healthcare provider if you experience any signs of an exacerbation, such as increased shortness of breath or change in sputum color.
Emergency action plan
Creating an emergency action plan is crucial for individuals with COPD. This plan should outline the necessary steps to take when experiencing a severe exacerbation or respiratory distress. It should include contact information for emergency services and your healthcare provider, a list of medications and doses, and clear instructions on when to seek medical help. Make sure to share this plan with your family members or close contacts, ensuring they know how to assist you in case of an emergency.
When to seek medical help
It is important to know when to seek medical help for your COPD. If you experience severe shortness of breath, chest pain, bluish discoloration of lips or fingernails, confusion, or difficulty speaking, do not hesitate to call emergency services immediately. Additionally, if your symptoms are worsening despite following your treatment plan, it is important to contact your healthcare provider for further evaluation and adjustment of your medications or treatment regimen.
Supporting Your Mental and Emotional Health
Coping with the emotional impact of COPD
Living with COPD can be emotionally challenging, as it may affect your ability to perform daily activities and participate in social events. It is normal to experience a range of emotions, including frustration, sadness, anxiety, or even depression. It is crucial to acknowledge these feelings and seek support from loved ones or mental health professionals. Engaging in activities that bring you joy, practicing relaxation techniques, and staying connected with a support network can be helpful in coping with the emotional impact of COPD.
Getting support from family and friends
Having a strong support system is essential when living with a chronic condition like COPD. Reach out to your family and friends for emotional support, understanding, and assistance when needed. Having someone to talk to, share your concerns, or simply spend time with can make a significant difference in your overall well-being. Educate your loved ones about COPD and how it affects your daily life to foster understanding and ensure they are equipped to support you effectively.
Joining COPD support groups
Connecting with others who are going through similar experiences can provide a sense of community, validation, and valuable information. Consider joining COPD support groups, either in-person or online, to connect with individuals who understand the challenges of living with COPD. These support groups can provide a platform to share experiences, exchange coping strategies, and learn from one another. Your healthcare provider or local respiratory health organizations may be able to provide information about support groups in your area.
Mental health resources
It is important to prioritize your mental health when living with COPD. There are numerous mental health resources available that can provide additional support and guidance. Mental health professionals, such as psychologists or counselors, can help you navigate the emotional challenges that may arise from living with a chronic condition. Online resources, educational materials, and reputable websites dedicated to COPD can also provide valuable information, coping strategies, and tips for managing your mental and emotional well-being.

Traveling with COPD
Planning ahead for travel
If you have COPD and plan to travel, it is essential to plan ahead to ensure a smooth and enjoyable trip. Consult with your healthcare provider before traveling to ensure your condition is stable and to receive any necessary vaccinations or medications. Research destinations and accommodations that have good air quality and are easily accessible. Consider travel insurance to ensure financial security in case of unforeseen medical emergencies.
Tips for air travel
Air travel can pose certain challenges for individuals with COPD, but with proper preparation, it can still be manageable. Be sure to inform the airline in advance of any special requirements or assistive devices you may need, such as oxygen or mobility aids. Request an aisle seat for easier access to the restroom and stretch your legs during the flight. Stay hydrated by drinking plenty of fluids and avoid alcohol, as it can contribute to dehydration.
Navigating accommodations
When selecting accommodations, consider factors that will contribute to your comfort and well-being. Look for smoke-free environments, rooms with good ventilation, and easy accessibility. Inquire about any necessary accommodations, such as a ground floor room or a room with grab bars in the bathroom. If you require oxygen therapy, ensure that the accommodations are aware of this and can accommodate your specific needs.
Managing medications while traveling
Ensure that you have an ample supply of medications for the duration of your trip, plus some extra in case of unexpected delays. Keep your medications in your carry-on luggage to ensure easy access during the flight and to prevent loss or damage. If you require oxygen therapy, make arrangements in advance with your oxygen supplier to ensure a portable oxygen concentrator or tanks will be available during your journey. It is also advisable to carry a list of your medications, along with dosage instructions, in case of any medical emergencies.
Home Modifications for Improved Living
Creating a COPD-friendly environment
Making specific modifications to your home can significantly improve your living environment and help manage your COPD symptoms. Ensure good indoor air quality by removing sources of pollution such as cigarette smoke, dust, and chemicals. Use air purifiers or filters to clean the air and consider investing in a dehumidifier if you live in a humid climate. Avoid carpets and opt for easily cleanable flooring, such as hardwood or tile, to minimize dust accumulation.
Improving indoor air quality
Indoor air quality plays a crucial role in managing COPD symptoms. Keep your home well-ventilated by opening windows or using fans to circulate fresh air. Avoid using products with strong odors or irritants, such as certain cleaning agents or air fresheners. Regularly clean and dust your home to minimize the accumulation of dust and allergens. If necessary, wear a mask or ask for assistance when performing activities that may expose you to irritants, such as painting or cleaning.
Assistive devices for daily activities
Assistive devices can make daily activities easier and less physically demanding for individuals with COPD. Consider using mobility aids such as walkers or canes to conserve energy and reduce stress on your lungs. Portable oxygen concentrators can provide oxygen therapy while allowing for greater mobility and independence. Devices such as reachers or long-handled tools can help with tasks that require bending or reaching, reducing strain on your respiratory system.
Home oxygen therapy
For individuals with severe COPD, oxygen therapy may be necessary to improve oxygen levels in the blood and alleviate symptoms. Home oxygen therapy involves the use of oxygen concentrators or oxygen tanks to provide supplemental oxygen. Your healthcare provider will determine the appropriate oxygen flow rate and duration based on your specific needs. It is essential to follow your oxygen therapy plan as prescribed and maintain regular communication with your healthcare provider regarding your oxygen needs.

The Role of Exercise
Benefits of exercise for COPD
Exercise plays a crucial role in managing COPD and improving overall health. Regular exercise can help improve lung function, strengthen respiratory muscles, and increase endurance. Physical activity also promotes cardiovascular health, reduces the risk of other chronic conditions, and enhances overall well-being. Engaging in exercise can also have positive effects on your mental and emotional health, reducing symptoms of anxiety and depression commonly associated with COPD.
Choosing appropriate exercises
When choosing exercises, it is important to consider your lung function, physical abilities, and any limitations you may have. Low-impact exercises such as walking, swimming, cycling, or using an elliptical machine are generally well-tolerated for individuals with COPD. Breathing and relaxation exercises, such as yoga or tai chi, can also help improve lung capacity and reduce dyspnea. Consult with your healthcare provider or a pulmonary rehabilitation specialist to determine the most appropriate exercises for you.
Creating an exercise routine
It is beneficial to establish a regular exercise routine and make it a part of your daily or weekly schedule. Start with shorter durations and lower intensity exercises, gradually increasing the duration and intensity as tolerated. Aim for at least 30 minutes of moderate-intensity exercise most days of the week. If you experience any worsening of symptoms during exercise, such as increased shortness of breath or chest pain, stop and seek medical advice.
Safety tips for exercising with COPD
When exercising with COPD, it is important to prioritize safety and make adjustments as needed. Warm up before exercise and cool down afterward to prevent strain on your muscles and reduce the risk of injury. Stay hydrated by drinking water before, during, and after exercise. Pace yourself and listen to your body – take breaks when needed and adjust the intensity as necessary. If you experience any chest pain or severe shortness of breath during exercise, stop and seek medical attention.
Caring for Yourself and Preventing Complications
Self-care practices for COPD
Self-care is crucial when living with COPD to maintain optimal health and prevent complications. Follow your prescribed treatment plan, take medications as directed, and attend regular medical check-ups. Practice good hand hygiene to reduce the risk of respiratory infections, such as the flu or common cold. Avoid exposure to individuals who are sick, and consider wearing a mask in crowded or high-risk situations. Prioritize your physical and mental well-being by engaging in activities that promote relaxation and enjoyment.
Preventing complications
COPD can increase the risk of certain complications, such as respiratory infections, lung cancer, and cardiovascular diseases. To prevent these complications, it is important to take steps to manage your COPD effectively. Quit smoking if you are a smoker, avoid exposure to environmental irritants, and follow your treatment plan diligently. Practice good hygiene, stay up to date with vaccinations, and maintain a healthy lifestyle that includes regular exercise, a nutritious diet, and stress management techniques.
Early detection of complications
Regular medical check-ups are essential for the early detection and management of any potential complications associated with COPD. Your healthcare provider will closely monitor your lung function and overall health, ensuring the timely identification of any changes or signs of complications. It is important to report any new or worsening symptoms to your healthcare provider promptly, as early intervention can make a significant difference in the outcome and management of potential complications.
Importance of vaccination
Vaccinations are a crucial component of preventive care for individuals with COPD. Getting vaccinated against influenza (flu) is highly recommended, as respiratory infections can exacerbate COPD symptoms and lead to complications. Additionally, getting vaccinated against pneumonia can reduce the risk of developing pneumonia, a common infection that can be severe for individuals with COPD. Talk to your healthcare provider about the appropriate vaccinations for you and the recommended schedule for administration.
Living with COPD can be challenging, but with proper management, lifestyle modifications, and support, you can improve your quality of life and effectively manage your condition. Remember to prioritize self-care, follow your treatment plan, and stay connected with your healthcare provider for regular check-ups and guidance. With the right tools and support, you can lead a fulfilling and active life despite COPD.