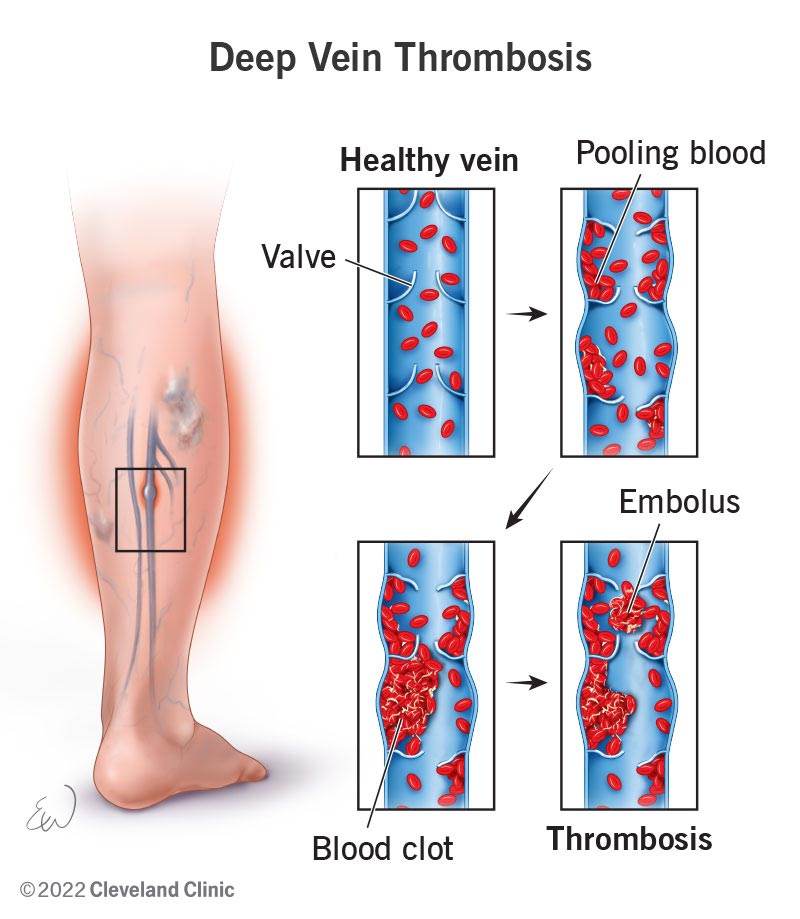
You’ve probably heard the term Deep Vein Thrombosis (DVT) before, but do you really know what it means? DVT is a condition that occurs when a blood clot forms in one of the deep veins in your body, most commonly in your legs. This seemingly harmless clot can lead to some serious complications if left untreated. In this article, we will explore the signs and symptoms of DVT, so you can recognize them and seek medical attention as needed. Whether you’re at risk or just curious about this condition, read on to discover the red flags that could save your life.
Signs and Symptoms of Deep Vein Thrombosis
Overview of Deep Vein Thrombosis
Deep Vein Thrombosis, commonly referred to as DVT, is a medical condition characterized by the formation of blood clots in the deep veins of the body, typically in the legs. This condition can be serious and potentially life-threatening if left untreated, as the blood clots may dislodge and travel to the lungs, causing a blockage known as a pulmonary embolism. Understanding the signs and symptoms of DVT is crucial for early detection and prompt medical intervention.
Risk Factors for Deep Vein Thrombosis
While DVT can occur in anyone, certain factors increase the likelihood of its development. It is essential to be aware of these risk factors to help identify individuals who may be at a higher risk of developing DVT. Inherited risk factors such as genetic disorders and blood clotting disorders may contribute to DVT. Acquired risk factors, including obesity, sedentary lifestyle, smoking, and hormonal changes (such as pregnancy or using birth control pills), also increase the risk. Situational risk factors, such as prolonged immobility during travel or hospitalization, further add to the susceptibility.

Common Signs and Symptoms of Deep Vein Thrombosis
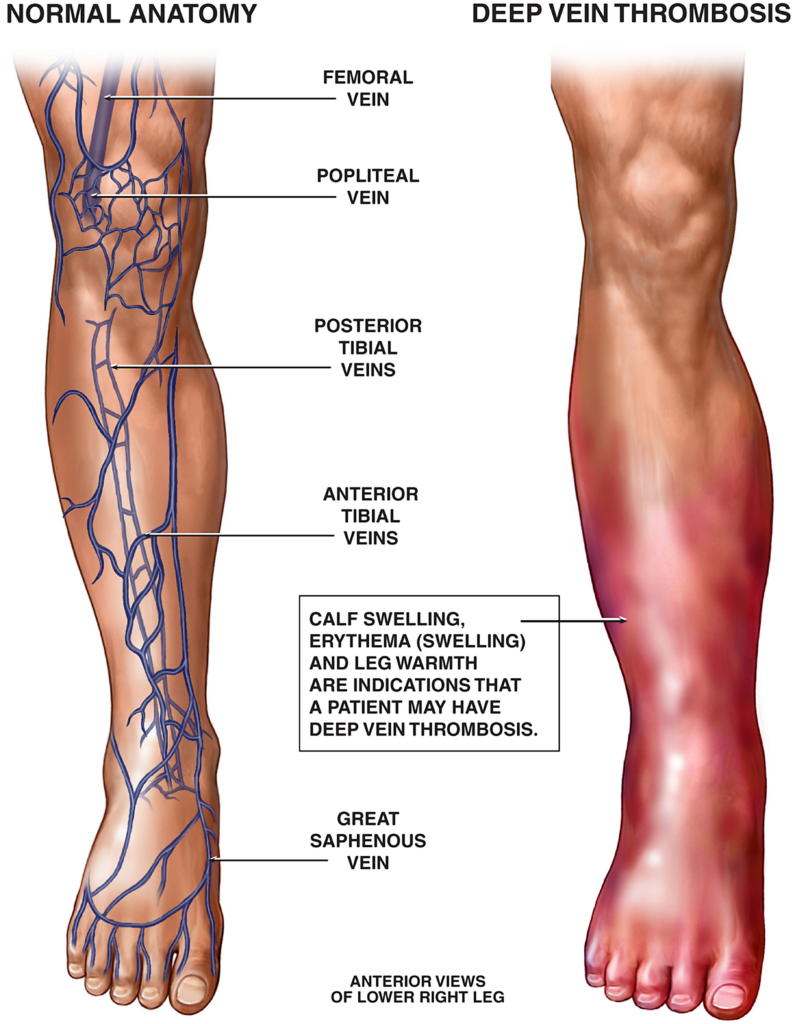
Recognizing the signs and symptoms of DVT is crucial for early diagnosis and timely medical intervention. While some individuals may not experience any symptoms, common signs of DVT include swelling and pain in the affected limb. The affected area may also feel warm to the touch and appear reddish in color. Another noticeable sign is the visibility of surface veins, which may appear enlarged or prominent. Additionally, individuals with DVT may experience leg fatigue or heaviness, skin discoloration, calf tenderness, and even a low-grade fever.
Recognizing Deep Vein Thrombosis
Differentiating DVT from other conditions is essential to avoid misdiagnosis and provide appropriate medical care. If you experience persistent pain or swelling in one leg without an obvious cause, it is crucial to suspect DVT and seek further medical evaluation. It is important to remember that the signs and symptoms of DVT may vary from person to person, and some individuals may not experience any noticeable symptoms. Therefore, it is crucial to be vigilant and listen to your body, especially if you have any underlying risk factors for DVT.
Understanding the Complications of Deep Vein Thrombosis
Deep Vein Thrombosis can lead to severe complications if not managed promptly. One such complication is a pulmonary embolism, which occurs when a blood clot dislodges from the deep vein and travels to the lungs. This condition can be life-threatening and requires immediate medical attention. Another complication is Post-Thrombotic Syndrome, which can cause chronic pain, swelling, and skin ulcers in the affected limb. Chronic Venous Insufficiency, characterized by long-term damage to the veins, is also a potential complication of DVT. Recognizing these complications underscores the importance of early detection and treatment.
When to Seek Medical Attention
Certain signs and symptoms of DVT require immediate medical attention. If you experience sudden shortness of breath, chest pain, rapid heart rate, or coughing up blood, these may be indications of a pulmonary embolism. In such cases, it is crucial to seek emergency medical care without delay. For less severe symptoms such as swelling, pain, or warmth in one leg, it is advisable to consult a healthcare professional as soon as possible to determine the cause and appropriate course of action.

Diagnosing Deep Vein Thrombosis
To diagnose DVT, healthcare professionals employ various methods to assess the condition accurately. Clinical evaluation involves reviewing the individual’s medical history and risk factors, as well as conducting a physical examination. During the examination, the healthcare provider may inspect the affected limb for visible signs of DVT and assess the area for warmth, tenderness, and swelling. Imaging tests such as ultrasound, venography, and MRI scans are commonly used to detect blood clots and evaluate their severity and location.
Preventing Deep Vein Thrombosis
Preventing DVT is crucial, particularly for individuals who are susceptible due to their risk factors. Lifestyle modifications play a significant role in reducing the risk of DVT. Maintaining an active lifestyle, regular exercise, and avoiding prolonged periods of immobility can help reduce the risk. Wearing compression stockings, especially during long-haul flights or extended bed rest, can improve blood flow and minimize the chance of clot formation. Additionally, individuals with high-risk factors may benefit from preventive medications or interventions, which should be discussed with a healthcare professional.
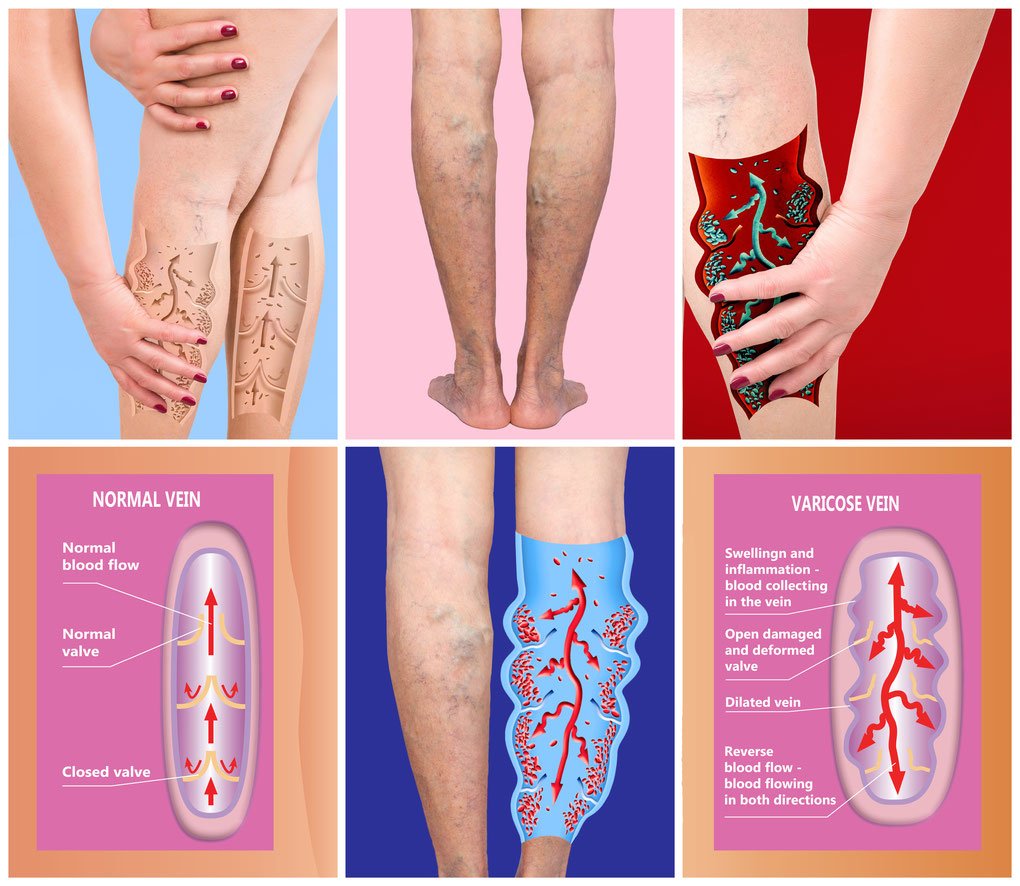
Treatment Options for Deep Vein Thrombosis
If diagnosed with DVT, several treatment options are available depending on the individual’s condition and the severity of the blood clot. Anticoagulant medications are commonly prescribed to prevent the clot from growing larger and to reduce the risk of additional blood clots. In some cases, thrombolytic therapy may be used to dissolve the clot. For more severe cases, surgery or catheter-based procedures can be utilized to remove or break up the clot. Treatment plans are tailored to each individual, and it is crucial to follow the healthcare provider’s recommendations for the most effective outcome.
Recovery and Long-Term Management
Recovery from DVT involves diligent management and ongoing monitoring to prevent future complications. Regular follow-up appointments with healthcare professionals are essential to assess the progress and monitor for any signs of recurrence or related issues. Managing symptoms and complications, such as Post-Thrombotic Syndrome or Chronic Venous Insufficiency, may require medication, lifestyle modifications, compression therapy, or other interventions. It is important to communicate any concerns or changes in symptoms to the healthcare team to ensure appropriate long-term management for optimal health and well-being.