Meningococcal Disease is a serious and potentially life-threatening illness caused by the bacterium Neisseria meningitidis. This article aims to provide you with a better understanding of this disease, its symptoms, risk factors, and available prevention methods. From the importance of early detection to the significance of vaccinations, we will explore everything you need to know about Meningococcal Disease in a friendly and informative manner. So, grab a cup of tea and let’s dive into the world of Meningococcal Disease together.
What is Meningococcal Disease?
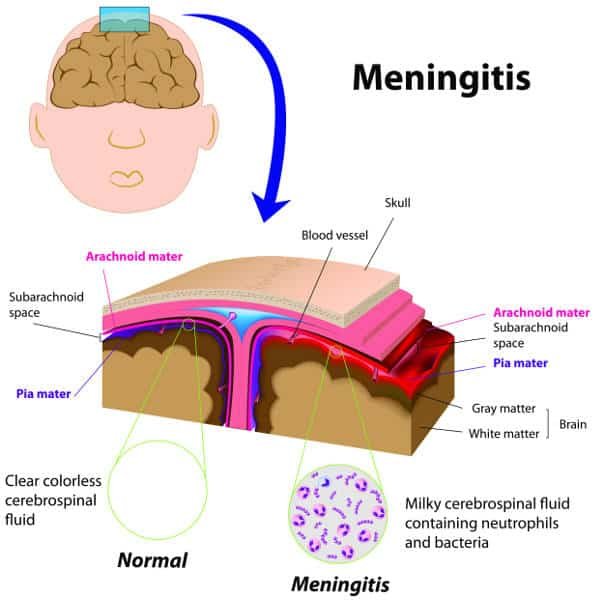
Overview of Meningococcal Disease
Meningococcal disease is a serious bacterial infection caused by the bacterium Neisseria meningitidis. It is a leading cause of meningitis, an inflammation of the protective membranes surrounding the brain and spinal cord. Meningococcal disease can also cause sepsis, a life-threatening blood infection.
Causes of Meningococcal Disease
Meningococcal disease is caused by the bacteria Neisseria meningitidis, which can be found in the nose and throat of individuals. It is transmitted from person to person through respiratory droplets, such as when an infected individual coughs or sneezes. The bacteria can spread easily in crowded places, such as college dormitories, military barracks, or boarding schools.
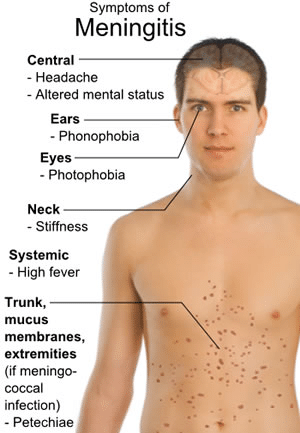
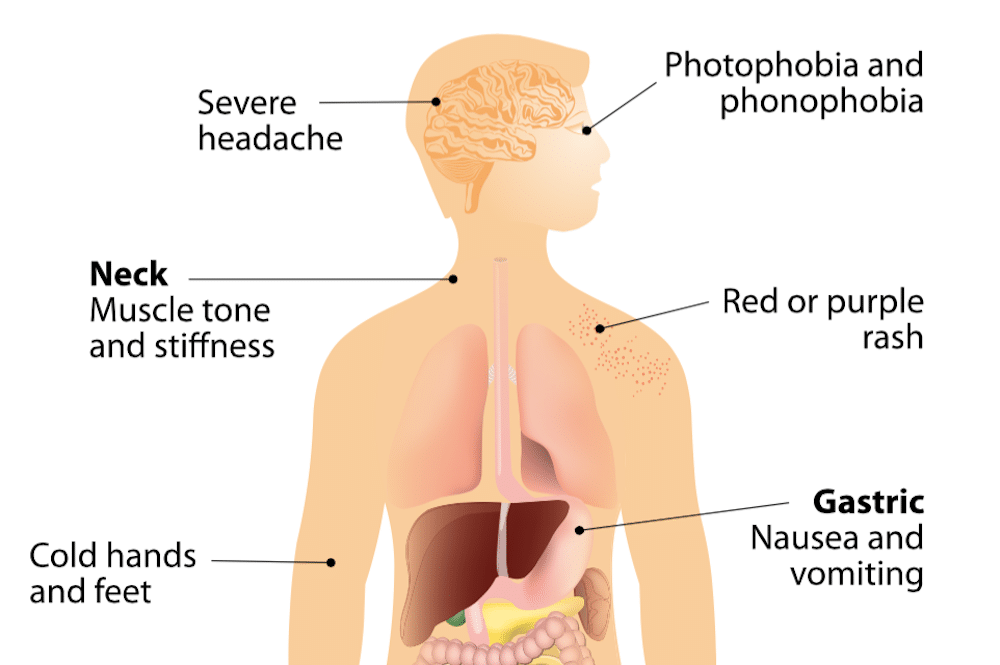
Symptoms of Meningococcal Disease
The symptoms of meningococcal disease can vary, but common signs include high fever, severe headache, stiff neck, nausea, vomiting, sensitivity to light, confusion, and a rash. This rash may start as tiny red or purple spots that quickly develop into larger patches. If you or someone you know is experiencing these symptoms, it is crucial to seek immediate medical attention as early diagnosis and treatment can be life-saving.
Who is at Risk?
Age and susceptibility
Meningococcal disease can affect individuals of all ages, but certain age groups are at a higher risk. Infants, adolescents, and young adults are more susceptible to infection. Additionally, college students living in dormitories, military recruits, and people traveling to countries where meningococcal disease is more common are also at an increased risk.
Living in close quarters
Living in close quarters, such as college dormitories or military barracks, can increase the risk of meningococcal disease transmission. This is because the bacteria can spread easily in crowded spaces, where respiratory droplets can easily pass between individuals. Close contact, sharing drinks or utensils, and intimate kissing can also facilitate transmission.
Immunocompromised individuals
Individuals with weakened immune systems, such as those with HIV/AIDS, certain cancers, or undergoing immunosuppressive therapy, are more susceptible to meningococcal disease. Their compromised immune response makes it harder for their body to fight off the infection, increasing their risk of severe complications.
Transmission and Prevention
How meningococcal bacteria spreads
Meningococcal bacteria are spread from person to person through respiratory droplets. When an infected individual coughs or sneezes, tiny droplets containing the bacteria can be inhaled by others nearby. Close contact, such as living in close quarters or participating in activities that involve prolonged contact, can increase the risk of transmission. It is important to note that not everyone who carries the bacteria will develop meningococcal disease.
Preventive measures
Preventing the spread of meningococcal disease involves practicing good personal hygiene. This includes covering your mouth and nose when coughing or sneezing, washing your hands frequently with soap and water, and avoiding close contact with people who are sick. Disinfecting commonly touched surfaces, such as doorknobs and countertops, can also help reduce the risk of transmission.
Vaccination
Vaccination is one of the most effective ways to prevent meningococcal disease. There are several types of meningococcal vaccines available, including conjugate vaccines and serogroup B vaccines. Routine vaccination is recommended for infants, adolescents, and young adults. Additionally, certain high-risk groups, such as college students living in dormitories, may need to receive the meningococcal vaccine.
Diagnosis and Treatment
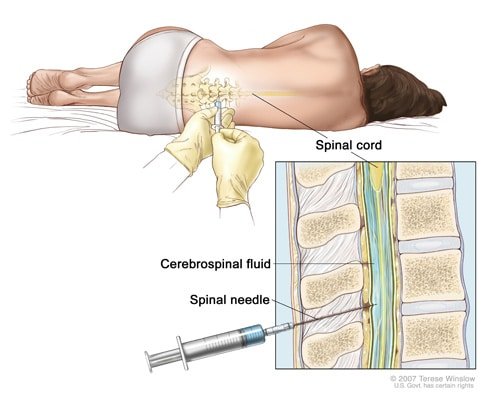
Methods of diagnosis
Diagnosing meningococcal disease involves a combination of clinical evaluations, laboratory tests, and medical history. A healthcare provider may perform a physical examination, checking for signs and symptoms such as neck stiffness, rash, and fever. Samples may be taken from the blood or cerebrospinal fluid to test for the presence of the bacteria. Prompt diagnosis is essential to start treatment as soon as possible.
Treatment options
Meningococcal disease requires immediate medical attention and treatment with antibiotics. This helps eradicate the bacteria from the body and prevent the progression of the infection. In severe cases, hospitalization may be necessary for close monitoring and intravenous administration of antibiotics. Supportive care, including rest, adequate hydration, and pain management, may also be provided to alleviate symptoms.
Antibiotic resistance
In recent years, there has been a growing concern regarding antibiotic resistance in the treatment of meningococcal disease. Some strains of Neisseria meningitidis have developed resistance to commonly used antibiotics. This emphasizes the importance of appropriate antibiotic stewardship and ongoing research to identify and develop new treatment strategies.
Complications of Meningococcal Disease
Potential complications
Meningococcal disease can lead to severe complications, including neurological damage, hearing loss, limb amputation, kidney failure, and even death. The bacteria can cause inflammation in the brain and other organs, resulting in long-term disabilities or permanent damage. Early diagnosis, prompt treatment, and supportive care can help prevent or minimize these complications.
Long-term effects
Survivors of meningococcal disease may experience long-term effects that significantly impact their quality of life. These can include cognitive impairments, hearing loss, mental health issues such as anxiety or depression, and physical disabilities. Rehabilitation and ongoing support may be necessary to help individuals regain function and adjust to these changes.
Mortality rates
While meningococcal disease is relatively rare, it can be life-threatening. According to the World Health Organization, the case-fatality ratio for meningococcal disease can range from 10 to 14 percent. The risk of death is higher in individuals with severe manifestations of the disease, such as sepsis or meningitis. Timely diagnosis, appropriate treatment, and vaccination can play a crucial role in reducing mortality rates.
Meningococcal Disease Outbreaks
Recent outbreaks
Meningococcal disease outbreaks occur sporadically around the world, and their frequency and extent can vary. In recent years, several countries have experienced outbreaks, often affecting specific communities or age groups. These outbreaks highlight the need for ongoing surveillance, rapid response measures, and targeted vaccination campaigns to control the spread of the disease.
Factors contributing to outbreaks
Several factors can contribute to the occurrence of meningococcal disease outbreaks. These include increased contact and close proximity among susceptible individuals, such as in college dormitories or military camps. Factors like decreased vaccine coverage, low immunization rates, and circulation of virulent strains of Neisseria meningitidis can also contribute to outbreaks.
Public health response
When an outbreak of meningococcal disease occurs, public health authorities take immediate action to control the spread of the infection. This can involve measures such as identifying cases, tracing contacts, and providing prophylactic antibiotics to close contacts. Vaccination campaigns may also be conducted to target high-risk groups and prevent further transmission.
Global Impact of Meningococcal Disease
Prevalence worldwide
Meningococcal disease is a global health concern, with varying incidence rates across different regions. Sub-Saharan Africa, commonly referred to as the “meningitis belt,” experiences the highest burden of the disease. However, outbreaks and sporadic cases occur in other parts of the world as well. The exact prevalence of meningococcal disease is difficult to determine due to underreporting and varying surveillance systems.
Economic burden
The economic burden of meningococcal disease extends beyond the cost of medical treatment. Outbreaks can have a significant impact on communities and healthcare systems, resulting in increased hospitalizations, healthcare expenditures, and potential loss of productivity. Investing in prevention strategies, including vaccination programs, can help reduce the economic burden associated with meningococcal disease.
Influence on public health policies
The impact of meningococcal disease on public health policies cannot be underestimated. The occurrence of outbreaks and the potential for severe complications has prompted policymakers to prioritize prevention and control strategies. National immunization programs have been implemented in many countries, ensuring routine vaccination for eligible populations and targeted vaccination during outbreaks.
Emerging Research and Innovations
Advancements in meningococcal vaccines
Continued research and development have led to advancements in meningococcal vaccines. This includes the introduction of conjugate vaccines that provide protection against multiple serogroups of Neisseria meningitidis. Serogroup B vaccines, which were previously unavailable, have also been developed to address the challenge posed by this particular serogroup.
New treatment strategies
In addition to vaccination, the development of new treatment strategies is crucial in combating meningococcal disease. Researchers are exploring alternative antibiotics and combinations of antibiotics to combat antibiotic-resistant strains. Other treatment modalities, such as immunotherapies and anti-inflammatory drugs, are also being investigated to prevent severe complications and improve outcomes.
Genomic surveillance
Genomic surveillance plays a pivotal role in understanding the epidemiology and evolution of meningococcal disease. By analyzing the genetic makeup of Neisseria meningitidis strains, scientists can identify specific clones responsible for outbreaks and track the spread of virulent strains. This information helps inform public health responses and guide vaccine development efforts.
Meningococcal Disease Awareness and Education
Promoting awareness
Raising awareness about meningococcal disease is crucial in preventing its spread and minimizing its impact. Public health campaigns, educational materials, and targeted messaging can help increase knowledge about the disease, its symptoms, transmission, and prevention measures. Collaboration between public health organizations, healthcare providers, and community leaders is essential in effectively disseminating awareness messages.
Informing the public
Efforts should be made to inform the public about the importance of vaccination to protect against meningococcal disease. Providing accurate and reliable information about the safety and efficacy of vaccines can dispel misconceptions and address vaccine hesitancy. Transparent communication channels, such as websites, helplines, and social media platforms, can be utilized to ensure widespread dissemination of information.
Resources and campaigns
Several resources and campaigns are available to support meningococcal disease awareness and education. National health agencies, international organizations, and advocacy groups offer informational materials, online resources, and tools for healthcare providers. Public health campaigns, both local and global, aim to reach specific populations and raise awareness about the disease and its prevention.
The Future of Meningococcal Disease Control
Challenges and opportunities
The control of meningococcal disease continues to face challenges and opportunities. Global disparities in vaccination coverage, surveillance systems, and healthcare resources pose obstacles to effective control strategies. However, advancements in vaccine development, technological innovations, and international collaborations provide opportunities for improved prevention and control of the disease.
Global eradication efforts
Achieving global eradication of meningococcal disease is a long-term goal, but it remains a considerable challenge due to the complexity of the disease and its transmission. It requires sustained efforts in areas such as vaccine coverage, surveillance, and outbreak response. International collaborations and sharing of best practices are crucial for coordinating these eradication efforts.
Improved prevention strategies
Future prevention strategies for meningococcal disease will focus on improving vaccine coverage, particularly in high-risk populations. Ongoing research will help identify new serogroups and strains, allowing for the development of effective vaccines. Additionally, public health campaigns and educational initiatives will continue to play a vital role in promoting prevention measures, such as good personal hygiene and timely vaccination.
In conclusion, meningococcal disease is a serious bacterial infection that can cause meningitis and sepsis. It can be transmitted through respiratory droplets and affects individuals of all ages, with certain groups at higher risk. Prevention and control efforts, including vaccination, public health responses to outbreaks, and public education, are essential in reducing the burden of the disease. Ongoing research and innovations provide hope for improved prevention strategies and future eradication efforts. By working together, we can continue to raise awareness, prevent transmission, and protect individuals from the potentially devastating effects of meningococcal disease.
