Meningococcal Disease is a serious illness caused by a bacteria called Neisseria meningitidis. It can lead to life-threatening complications such as meningitis and blood infections. In order to effectively treat this disease, a comprehensive approach is necessary. This article will explore the various treatment options available for Meningococcal Disease, including antibiotics and supportive care, highlighting the importance of early detection and prompt medical intervention. By understanding the comprehensive approach to treating Meningococcal Disease, you can be better equipped to protect yourself and your loved ones.
Understanding Meningococcal Disease
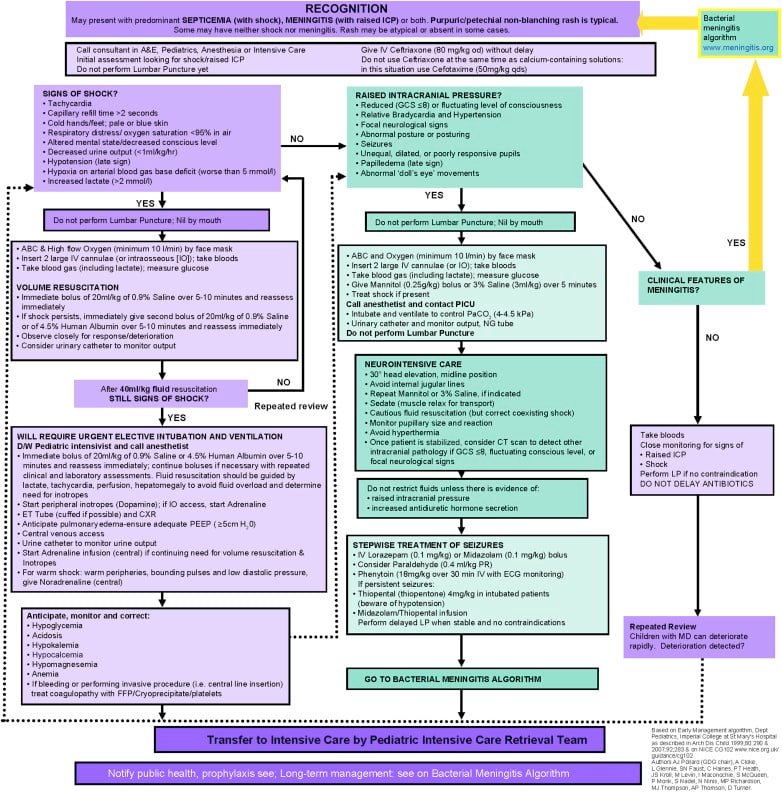
Meningococcal disease is a serious bacterial infection caused by the bacterium Neisseria meningitidis. This infectious disease can lead to severe illness, including meningitis, septicemia (blood infection), and other life-threatening complications. It is important to have a comprehensive understanding of the disease to ensure timely diagnosis and appropriate treatment.
Definition
Meningococcal disease is an acute illness characterized by inflammation of the meninges, the protective membranes that cover the brain and spinal cord. It can present as either meningitis, which affects the meninges, or septicemia, which affects the bloodstream. The disease is caused by Neisseria meningitidis, a bacterium that can be spread through respiratory droplets or direct contact with an infected individual. Meningococcal disease can occur sporadically or in outbreaks, particularly in crowded places such as college campuses or military barracks.
Causes and Transmission
Neisseria meningitidis is typically transmitted from person to person through respiratory droplets. Close contact, such as coughing, sneezing, or kissing, with an infected individual can facilitate the spread of the bacterium. Additionally, sharing contaminated items like utensils or drinking from the same cup can also contribute to transmission. While most individuals who come into contact with the bacterium do not develop the disease, certain factors such as a weakened immune system or genetic predisposition can increase the risk of infection.
Symptoms
The symptoms of meningococcal disease can vary depending on the specific manifestation of the infection. Meningitis typically presents with symptoms such as severe headache, neck stiffness, fever, sensitivity to light, and a rash that does not fade under pressure. On the other hand, septicemia may present with symptoms such as high fever, chills, fatigue, rapid breathing, vomiting, and a petechial or purpuric rash. These symptoms can develop rapidly and progress to life-threatening complications within a few hours, making early recognition and medical intervention essential.
Prevention Measures
Preventing meningococcal disease is of utmost importance in reducing its incidence and severity. Several preventive measures can be implemented to minimize the risk of infection and transmission.
Vaccination
Vaccination is a crucial step in preventing meningococcal disease. Vaccines are available that provide protection against several different serogroups of Neisseria meningitidis, including A, B, C, W, and Y. Routine vaccination is recommended for infants and children, with booster doses in adolescence. Additionally, individuals living in close quarters, such as college students residing in dormitories, are advised to receive the meningococcal vaccine. Prompt vaccination in response to an outbreak is also an important preventive strategy.
Prophylactic Antibiotics
Prophylactic antibiotics are sometimes recommended for individuals who have been in close contact with someone diagnosed with meningococcal disease. These antibiotics help prevent the spread of the bacterium to others who may be at increased risk. It is crucial to seek medical advice to determine the necessity and appropriate duration of prophylactic antibiotics, as this may vary depending on the specific circumstances.
Isolation and Quarantine
Isolation and quarantine measures should be implemented to prevent the spread of meningococcal disease within communities or institutions. Infected individuals should be promptly isolated to minimize contact with others and reduce the risk of transmission. Additionally, individuals who have been in close contact with an infected individual may be advised to undergo quarantine to monitor for any signs or symptoms of the disease and prevent further spread.
Diagnosis
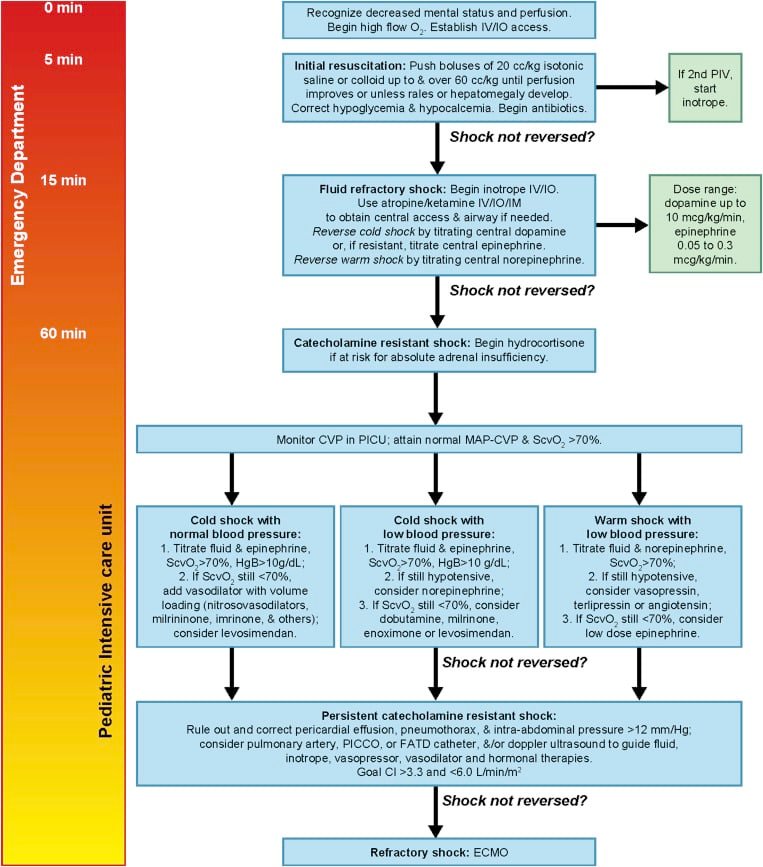
The diagnosis of meningococcal disease requires a comprehensive evaluation, including physical examination and laboratory tests. Prompt and accurate diagnosis is essential in order to initiate timely treatment and prevent complications.
Physical Examination
During a physical examination, healthcare providers will assess for common signs and symptoms of meningococcal disease. This may include evaluating for neck stiffness, examining the skin for any rash, assessing vital signs, and evaluating neurological status. The presence of these clinical findings, along with a thorough medical history, can help guide further diagnostic investigations.
Laboratory Tests
Laboratory tests are essential for confirming the diagnosis of meningococcal disease. These tests may include blood cultures, cerebrospinal fluid analysis, and polymerase chain reaction (PCR) testing. Blood cultures help identify the presence of Neisseria meningitidis in the bloodstream, while cerebrospinal fluid analysis can provide valuable information about the inflammatory response within the central nervous system. PCR testing is a highly sensitive technique that can detect the genetic material of the bacterium, further aiding in the diagnosis of meningococcal disease.
Treatment Options
Treating meningococcal disease requires a comprehensive approach that includes the use of antibiotics and supportive care. Timely initiation of treatment is crucial to improve outcomes and reduce the risk of complications.
Antibiotics
Antibiotics are the cornerstone of treatment for meningococcal disease. Empirical antibiotic therapy is typically initiated as soon as the diagnosis is suspected, even before confirmation through laboratory tests. Intravenous antibiotics, such as ceftriaxone or cefotaxime, are commonly used to target the Neisseria meningitidis bacterium. The choice of specific antibiotics may depend on factors such as local resistance patterns and the age of the individual affected.
Supportive Care
Supportive care is an essential component of treatment for meningococcal disease. This may include measures to manage symptoms of meningitis, such as pain relief and fever reduction. Adequate hydration and fluid replacement are important to maintain cardiovascular stability and prevent d- dehydration. In severe cases, intensive care management may be necessary, including respiratory support, circulatory support, and close monitoring of organ function.
Hospitalization
Hospitalization is typically required for individuals diagnosed with meningococcal disease. This allows for close monitoring of clinical progress, administration of intravenous antibiotics, and provision of necessary supportive care. In the hospital setting, healthcare providers can promptly identify and manage potential complications, ensuring the best possible outcome for the individual affected.
Antibiotics for Meningococcal Disease
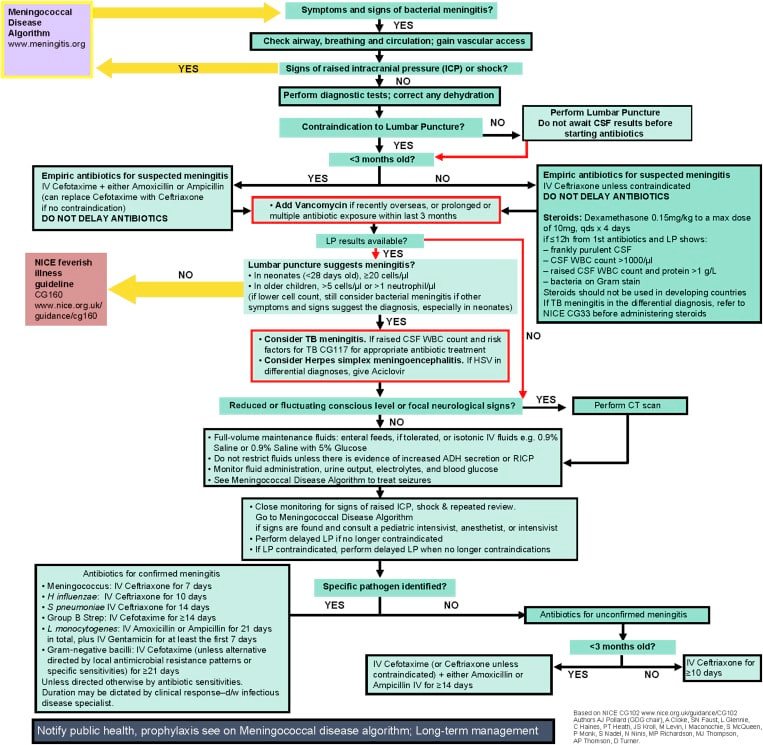
The choice and duration of antibiotic treatment for meningococcal disease are key factors in achieving successful outcomes and preventing complications.
Choice of Antibiotics
The choice of antibiotics for treating meningococcal disease is guided by factors such as the likely causative serogroup, local resistance patterns, and individual patient characteristics. Third-generation cephalosporins, such as ceftriaxone or cefotaxime, are commonly used as they have shown efficacy against the Neisseria meningitidis bacterium. These antibiotics have excellent tissue penetration, making them effective against both meningitis and septicemia.
Duration of Treatment
The duration of antibiotic treatment for meningococcal disease depends on several factors, including the severity of the infection, the individual’s response to treatment, and the presence of complications. Typically, antibiotic therapy is administered for a minimum of 5 to 7 days, but the duration may be extended if required. Close monitoring of clinical progress, along with regular reassessment, is crucial in determining the appropriate duration of antibiotic treatment.
Supportive Care
In addition to antibiotic therapy, supportive care plays a vital role in managing meningococcal disease and its associated symptoms.
Fluid Replacement
Ensuring adequate fluid intake and hydration is crucial in managing meningococcal disease. Intravenous fluid replacement may be required in severe cases to maintain adequate blood volume, prevent dehydration, and support cardiovascular stability. Close monitoring of fluid balance is important to prevent complications such as electrolyte imbalances and organ dysfunction.
Pain Management
Meningococcal disease can cause significant pain, particularly with meningitis. Medications for pain relief, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids, may be prescribed to alleviate discomfort. Pain management strategies should be tailored to the individual’s needs and closely monitored for effectiveness and potential side effects.
Fever Reduction
High fever is a common symptom of meningococcal disease and can worsen general discomfort. Fever-reducing medications, such as acetaminophen or ibuprofen, may be recommended to help control temperature and improve the individual’s overall well-being. Regular monitoring of body temperature and appropriate medication administration can aid in fever reduction and provide relief.

Complications and Management
Meningococcal disease can lead to severe complications that require prompt management to prevent long-term consequences.
Septic Shock
One of the most life-threatening complications of meningococcal disease is septic shock. This occurs when the bacterium enters the bloodstream and triggers a systemic inflammatory response, leading to organ dysfunction and poor circulation. Management of septic shock involves aggressive fluid resuscitation, the administration of vasopressor medications to support blood pressure, and measures to restore tissue perfusion and oxygenation.
Meningitis
Meningitis is a significant complication of meningococcal disease and can lead to long-term neurological damage if not promptly treated. Close monitoring of neurological status is important, along with the administration of appropriate antibiotic therapy and supportive care. In severe cases, additional interventions such as dexamethasone may be considered to reduce inflammation and protect the central nervous system.
Long-term Effects
While most individuals recover fully from meningococcal disease with appropriate treatment, some may experience long-term effects. These can include hearing loss, neurologic deficits, cognitive impairments, and psychological sequelae such as anxiety or depression. Individuals who have experienced meningococcal disease should receive appropriate follow-up care and support to address any potential long-term effects and promote overall well-being.
Follow-up Care
Follow-up care is essential in monitoring the progress of individuals who have been affected by meningococcal disease and ensuring their continued health and well-being.
Monitoring Progress
Regular medical follow-up is important to monitor the individual’s progress and assess for any signs of relapse or complications. Healthcare providers will evaluate the results of laboratory tests, assess clinical improvement, and determine the need for additional interventions. Early detection and intervention can help prevent the recurrence of symptoms or the development of long-term complications.
Vaccination Updates
As part of follow-up care, it is important to ensure that individuals receive any necessary vaccinations or booster doses. Vaccination updates, particularly for meningococcal disease, can help maintain long-term protection against future infections. Healthcare providers will provide guidance on the appropriate timing and type of vaccines needed based on the individual’s age, vaccination history, and risk factors.
Psychological Support
Meningococcal disease can have a significant psychological impact on individuals and their families. It is important to provide appropriate psychological support and counseling to address any emotional or mental health concerns that may arise. This may include support groups, individual counseling, or referrals to specialized mental health professionals. Addressing the psychological well-being of those affected by meningococcal disease is crucial in promoting overall recovery and quality of life.
Public Health Measures
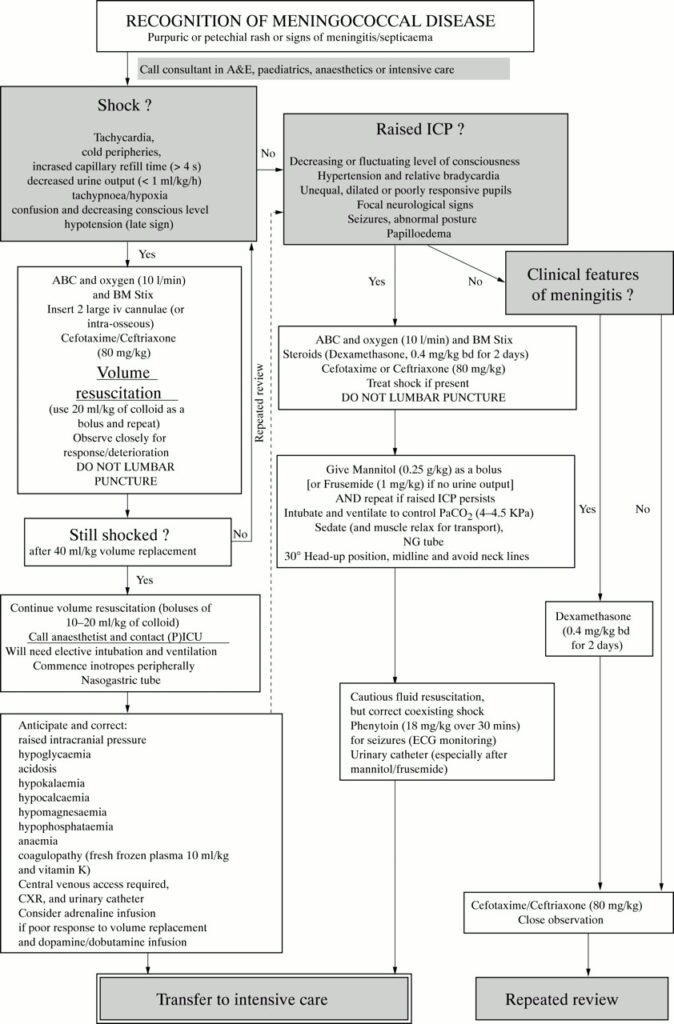
In addition to individual care, public health measures play a crucial role in preventing the spread of meningococcal disease and managing outbreaks.
Contact Tracing
Contact tracing is an important public health measure to identify individuals who may have been exposed to the bacterium. By identifying and notifying close contacts, public health officials can provide necessary guidance, such as vaccination or prophylactic antibiotic administration, to reduce the risk of further transmission. Contact tracing helps contain the spread of the disease within communities and limit its impact.
Education and Awareness
Public education and awareness campaigns are vital in preventing meningococcal disease. These campaigns aim to inform the public about the signs and symptoms of the disease, the importance of vaccination, and the need for prompt medical attention. By raising awareness, individuals can become proactive in seeking appropriate care and taking preventive measures, ultimately reducing the burden of the disease.
Outbreak Management
In the event of an outbreak of meningococcal disease, prompt and coordinated outbreak management is critical. Public health officials work closely with healthcare providers, community organizations, and other stakeholders to implement effective control measures, including vaccination campaigns, contact tracing, and public awareness initiatives. By responding quickly and efficiently to outbreaks, the impact of the disease can be minimized, and further spread can be contained.
Conclusion
Understanding meningococcal disease is crucial in preventing its spread, ensuring timely diagnosis, and implementing appropriate management strategies. By following preventive measures such as vaccination, practicing good hygiene, and seeking prompt medical attention, the burden of meningococcal disease can be significantly reduced. Public health measures, including contact tracing and education, play a vital role in containing the disease and preventing outbreaks. With a comprehensive approach encompassing diagnosis, treatment, supportive care, and follow-up, we can effectively manage meningococcal disease, promoting the health and well-being of individuals and communities.