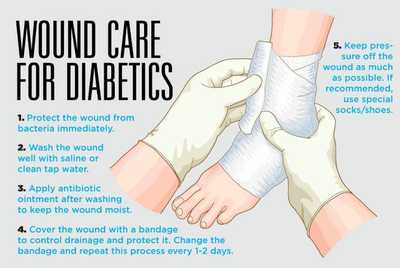
If you or someone you know is living with diabetes, you may be aware of the increased risk of developing wounds that can be difficult to heal. These wounds, known as diabetic ulcers, are a common complication of diabetes and can be a cause for concern. However, there are effective ways to treat and manage diabetes wounds that can help promote healing and prevent further complications. From proper wound care to managing blood sugar levels, this article will explore various strategies that can be implemented to effectively treat diabetes wounds and improve overall health and well-being.
1. Medications and topical treatments
1.1 Insulin therapy
Insulin therapy is a crucial component in the treatment of diabetes wounds. As a person with diabetes, managing your blood sugar levels is vital for wound healing. Insulin helps to regulate your blood sugar levels, which in turn promotes the healing process. By controlling your blood sugar levels, insulin therapy can prevent further complications and support the healing of your wounds.
1.2 Antibiotics
In cases where diabetes wounds become infected, antibiotics are often prescribed. These medications work by eliminating or inhibiting the growth of bacteria in the wound. It is important to take antibiotics as prescribed by your healthcare provider and to complete the full course of treatment. This helps to ensure the infection is fully cleared and prevents the development of antibiotic resistance.
1.3 Antiseptics
Antiseptics are commonly used to clean diabetes wounds and prevent infection. They work by killing or inhibiting the growth of microorganisms on the skin. Antiseptics can be applied topically either as a liquid solution or in the form of ointments or sprays. It is important to follow the instructions provided by your healthcare provider when using antiseptics to ensure proper wound care.
1.4 Growth factors
Growth factors are substances that stimulate the growth and repair of tissues. In diabetes wound care, growth factors can be applied topically or injected into the wound bed. These substances promote the migration of cells to the wound site, enhance tissue regeneration, and accelerate the healing process. Your healthcare provider may recommend the use of growth factors based on the severity and characteristics of your wound.
2. Wound debridement
2.1 Surgical debridement
Surgical debridement is a procedure performed by a healthcare professional to remove dead, damaged, or infected tissue from the wound. This method involves using instruments such as scalpels, scissors, or forceps to carefully remove the non-viable tissue. Surgical debridement facilitates the healing process by promoting the growth of healthy tissue and reducing the risk of infection.
2.2 Mechanical debridement
Mechanical debridement involves the use of physical methods to remove devitalized tissue. This can include methods such as wound irrigation, wet-to-dry dressings, or hydrotherapy. Mechanical debridement helps to remove debris, bacteria, and non-viable tissue from the wound, allowing for better wound healing and reducing the risk of infection.
2.3 Enzymatic debridement
Enzymatic debridement involves applying topical enzymes to the wound to break down and remove necrotic tissue. These enzymes selectively target and break down only the non-living tissue, leaving the healthy tissue intact. Enzymatic debridement can be particularly useful for wounds with large amounts of non-viable tissue or for patients who are not suitable candidates for surgical debridement.

3. Negative pressure wound therapy (NPWT)
3.1 Introduction to NPWT
Negative pressure wound therapy, commonly known as NPWT, is a treatment method that involves the application of negative pressure (suction) to the wound bed. This therapeutic technique promotes wound healing by removing excess fluid, reducing edema, and improving blood flow to the area. NPWT can be applied using specialized dressings and vacuum-assisted devices.
3.2 How NPWT works
NPWT works by creating a controlled environment around the wound. The negative pressure applied to the wound helps to remove excess fluid and reduce swelling, which can aid in the healing process. Additionally, NPWT promotes the formation of granulation tissue and enhances the growth of new blood vessels in the wound bed.
3.3 Benefits of NPWT
NPWT offers several benefits for diabetes wound treatment. It can enhance wound healing by reducing the risk of infection, promoting the formation of healthy tissue, and improving overall wound closure. NPWT can also help manage wound exudate and provide a protective barrier against external contaminants. This therapy has been shown to be effective in various types of wounds, including diabetic foot ulcers.
4. Hyperbaric oxygen therapy (HBOT)
4.1 How HBOT works
Hyperbaric oxygen therapy (HBOT) involves the administration of 100% oxygen at higher than normal atmospheric pressure. This treatment increases the oxygen concentration in the bloodstream, allowing more oxygen to be delivered to the tissues, including the wound site. The increased oxygen supply promotes angiogenesis (formation of new blood vessels), enhances white blood cell function, and stimulates collagen production, all of which are crucial for wound healing.
4.2 Benefits of HBOT
HBOT has shown promising results in the treatment of chronic wounds, including those associated with diabetes. It can help improve oxygenation in poorly perfused areas of the body, promote the growth of new blood vessels, and enhance the body’s natural healing processes. HBOT is particularly beneficial for non-healing wounds that have not responded to other forms of treatment.
4.3 Risks and complications of HBOT
While generally safe, HBOT may have some potential risks and complications. These can include ear barotrauma (pressure-related ear damage), oxygen toxicity, sinus pain or discomfort, and in rare cases, fires in the hyperbaric chamber. It is important to discuss the potential risks and benefits of HBOT with your healthcare provider before undergoing this therapy.

5. Bioengineered skin substitutes
5.1 Types of bioengineered skin substitutes
Bioengineered skin substitutes are artificial materials that are designed to promote wound healing by providing a scaffold for cell growth and tissue regeneration. These substitutes can be classified into two main types: dermal substitutes and epidermal substitutes. Dermal substitutes consist of a biocompatible matrix that mimics the dermal layer of the skin, while epidermal substitutes are designed to mimic the outermost layer of the skin.
5.2 How bioengineered skin substitutes work
Bioengineered skin substitutes work by providing a framework for the growth of new tissue and supporting the healing process. Dermal substitutes help promote the formation of new blood vessels, cellular infiltration, and collagen deposition. Epidermal substitutes provide a barrier against infection and aid in the re-epithelialization of the wound.
5.3 Benefits of using bioengineered skin substitutes
Bioengineered skin substitutes offer several benefits in the treatment of diabetes wounds. They can reduce the risk of infection, provide a protective barrier, and enhance wound closure. Bioengineered skin substitutes can also help manage wound exudate and reduce pain. Additionally, these substitutes can be customized to fit the specific needs of the wound, allowing for optimal healing outcomes.
6. Platelet-rich plasma (PRP) therapy
6.1 Introduction to PRP therapy
Platelet-rich plasma (PRP) therapy is a treatment that involves using the patient’s own blood to promote wound healing. The blood is processed to concentrate the platelets, which contain growth factors and other healing substances. The concentrated platelets are then applied to the wound site to stimulate tissue repair and regeneration.
6.2 How PRP therapy works
PRP therapy works by releasing growth factors and cytokines that promote cell proliferation, angiogenesis, and collagen production. These substances help accelerate the wound healing process and stimulate the formation of healthy tissue. PRP therapy can be particularly beneficial for chronic wounds that have not responded well to other treatments.
6.3 Benefits and limitations of PRP therapy
PRP therapy offers several benefits for diabetes wound treatment. It is a natural and safe treatment option since it utilizes the patient’s own blood. PRP therapy can enhance wound healing, reduce inflammation, and improve tissue regeneration. However, it is important to note that PRP therapy may not be effective for all wounds, and further research is needed to fully understand its limitations and optimal use.

7. Hyperosmolar agents
7.1 Mechanism of action of hyperosmolar agents
Hyperosmolar agents work by creating an osmotic gradient in the wound, helping to draw out excess fluid and reduce edema. These agents have a higher osmolarity compared to the surrounding tissues, which promotes the movement of fluids from the wound bed. This can help improve wound healing by reducing swelling and promoting tissue repair.
7.2 Types of hyperosmolar agents
There are several types of hyperosmolar agents that can be used in wound treatment. Common examples include hypertonic saline solutions and sugar-based solutions. These agents are typically applied topically or used as wound dressings to create the osmotic effect and promote fluid removal from the wound.
7.3 How to use hyperosmolar agents for wound treatment
Hyperosmolar agents should be used according to the recommendations of your healthcare provider. They are typically applied directly to the wound or used as a soak. It is important to follow the instructions provided and monitor the wound closely for any signs of adverse reactions or complications.
8. Compression therapy
8.1 Introduction to compression therapy
Compression therapy involves the application of pressure to the affected area to improve blood flow and prevent swelling. In the context of diabetes wound treatment, compression therapy can help manage edema, reduce inflammation, and promote the healing of ulcers and venous stasis wounds.
8.2 Types of compression therapy
There are different types of compression therapy available, including bandages, compression stockings, and intermittent pneumatic compression devices. These methods can be used to apply sustained or intermittent pressure to the affected area, depending on the specific needs of the wound and the patient.
8.3 Benefits and considerations of compression therapy
Compression therapy offers several benefits in the treatment of diabetes wounds. It can help reduce swelling, improve blood circulation, and prevent the recurrence of ulcers. However, it is important to consider individual factors such as the severity of the wound, the presence of arterial disease, and the patient’s overall health status. Compression therapy should be prescribed and monitored by a healthcare professional to ensure optimal results and safety.

9. Offloading and pressure redistribution
9.1 Importance of offloading
Offloading is a critical aspect of wound healing for individuals with diabetes. It involves reducing pressure on the affected area to relieve stress on the wound and promote proper healing. Offloading is particularly important for diabetic foot ulcers, as excessive pressure can impede the healing process and lead to further complications.
9.2 Techniques for offloading
There are various techniques for offloading, including the use of special footwear, orthotic devices, and assistive devices such as crutches or wheelchairs. These methods help to redistribute pressure away from the wound and ensure that it is not subject to excessive stress during the healing process. Your healthcare provider can recommend the most appropriate offloading technique based on your specific needs.
9.3 Devices for pressure redistribution
There are several devices available that can aid in pressure redistribution and offloading. Examples include specialized shoes or boots, foam or gel cushions, and pressure-relieving mattresses. These devices help reduce pressure on the wound and provide support and cushioning to promote healing. It is important to use these devices as instructed and to regularly evaluate their effectiveness in the wound healing process.
10. Nutrition and wound healing
10.1 Role of nutrition in wound healing
Nutrition plays a crucial role in the wound healing process. Proper nutrition provides the body with the necessary nutrients, vitamins, and minerals needed for tissue repair and regeneration. For individuals with diabetes, maintaining a balanced diet is essential for optimal wound healing outcomes.
10.2 Nutritional recommendations for diabetic wound treatment
When it comes to diabetic wound treatment, it is important to focus on a well-balanced diet that includes a variety of nutrients. This should include adequate protein intake to support tissue repair, sufficient vitamins (such as vitamin C and D) for collagen synthesis and bone health, and appropriate hydration to ensure proper blood flow and tissue hydration. It is best to consult with a registered dietitian or healthcare provider to develop a personalized nutrition plan based on your specific needs and health goals.
10.3 Supplements for promoting wound healing
In some cases, supplements may be recommended to support wound healing in individuals with diabetes. These can include omega-3 fatty acids, zinc, vitamin E, and probiotics, among others. However, it is important to consult with your healthcare provider before starting any new supplements, as they can interact with medications or have potential side effects.
In conclusion, effective treatment of diabetes wounds requires a comprehensive approach that incorporates various therapies and interventions. Medications, topical treatments, and debridement methods help manage infections, remove non-viable tissue, and stimulate wound healing. Advanced therapies such as negative pressure wound therapy and hyperbaric oxygen therapy can further enhance the healing process. Additionally, techniques like offloading, compression therapy, and the use of bioengineered skin substitutes offer additional means of promoting wound healing. Lastly, proper nutrition and supplementation play a crucial role in supporting the body’s natural healing processes. By integrating these strategies, you can improve the outcomes of your diabetes wound treatment and facilitate the healing of your wounds. Remember to consult with your healthcare provider for personalized recommendations based on your individual needs and medical history.