Diabetes Mellitus: The Role Of Medication
Diabetes Mellitus isn’t just a condition; it’s a journey that many individuals navigate, often requiring careful consideration of various factors that impact your health. Understanding the role of medication in diabetes management is crucial, whether you are newly diagnosed or have been living with the condition for years. This article aims to provide you with a comprehensive understanding of how different medications can support your journey with diabetes.
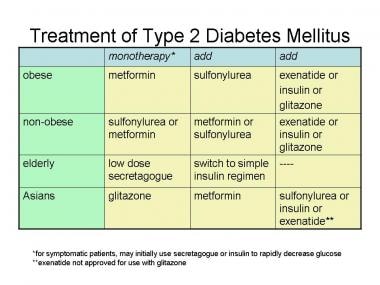
What Is Diabetes Mellitus?
Diabetes Mellitus refers to a group of diseases that affect how your body uses blood sugar (glucose). Glucose is vital for your health as it is a primary fuel source for your cells. When diabetes occurs, the body either doesn’t produce enough insulin, a hormone that helps glucose enter your cells, or can’t effectively use the insulin produced. As a result, glucose remains in your bloodstream, which can lead to serious health complications over time.
Understanding diabetes is the first step to managing it effectively. There are primarily two types of diabetes: Type 1 and Type 2. In Type 1 diabetes, your body fails to produce insulin, meaning you will need to take it externally. Type 2 is more common and often linked to lifestyle factors; in this case, insulin may be produced, but your body cannot use it efficiently. Recognizing which type you have is essential for understanding the appropriate medication approach.
The Importance of Medication in Diabetes Management
Now that you have a basic grasp of what diabetes is, let’s delve into the role medication plays. Even with a healthy lifestyle and diet, medications can be necessary to help you control your blood sugar levels effectively. They work alongside other management strategies, including exercise and dietary changes, to keep your glucose levels stable.
The primary goal of diabetes medication is to maintain your blood sugar levels within a target range. This is vital in reducing the risk of complications, such as neuropathy, retinopathy, and cardiovascular disease, which can arise from prolonged high blood sugar levels. In addition to that, keeping your blood sugar under control helps you maintain a quality of life where you can engage in everyday activities without constant worry.
Types of Medications for Diabetes
When it comes to treating diabetes, different types of medications are available to suit your specific needs. Each class of medication works in a unique way to manage your blood glucose levels.
Insulin
For people with Type 1 diabetes, insulin is not just an option; it’s a necessity. Since your pancreas doesn’t produce this vital hormone, you’ll need to inject insulin or use an insulin pump. Insulin helps your body use glucose for energy, preventing it from accumulating in your bloodstream.
People with Type 2 diabetes may also require insulin, especially if oral medications are insufficient to control blood sugar levels. Insulin comes in various forms that differ in how quickly and for how long they work, allowing for individualized treatment plans. Learning how to take insulin correctly and how to adjust the doses according to your readings can empower you in managing your diabetes effectively.
Sulfonylureas
Sulfonylureas are another class of drugs that stimulate your pancreas to produce more insulin. They might be prescribed if you have Type 2 diabetes and your blood sugar levels aren’t adequately controlled by diet and exercise alone. While they can be effective, it’s important to be aware of potential side effects, such as low blood sugar levels (hypoglycemia) and weight gain. Regular monitoring and communication with your healthcare provider can help mitigate these risks.
Biguanides
One of the most commonly prescribed biguanides is Metformin. This medication works by reducing glucose production in the liver and improving insulin sensitivity, making it easier for your cells to utilize available glucose. Metformin is often the first-line treatment for Type 2 diabetes due to its ability to lower blood sugar levels effectively while also offering benefits such as weight loss and cardiovascular protection.
If you’re starting a regimen that includes Metformin, you might experience some gastrointestinal side effects initially, like nausea or diarrhea. However, many people find that these symptoms subside over time as your body adjusts to the medication.
DPP-4 Inhibitors
DPP-4 inhibitors, like Sitagliptin or Saxagliptin, work by increasing insulin production while lowering glucose production in the liver. They are often preferred for their relatively mild side effect profile compared to some other diabetes medications. They also don’t typically lead to weight gain, which can be a concern for many individuals with Type 2 diabetes. However, it’s crucial to ensure regular monitoring, as DPP-4 inhibitors can still lead to low blood sugar, especially when taken alongside other agents.
SGLT2 Inhibitors
SGLT2 inhibitors, such as Canagliflozin or Dapagliflozin, are newer oral diabetes medications that help lower blood sugar by causing the kidneys to remove glucose from the bloodstream through urine. This class of medication has gained popularity not only for its blood sugar-lowering effects but also for aiding in weight loss and providing protective benefits for heart health. However, dehydration or urinary tract infections can be potential side effects to watch out for, so staying informed and connected with your healthcare provider is essential.
Personalized Treatment Plans
One size does not fit all when it comes to diabetes treatment. Factors such as your age, lifestyle, existing health conditions, and personal health goals all contribute to developing a personalized diabetes management plan. Your healthcare provider will work with you to understand your unique circumstances and determine the most appropriate medications and dosages.
When discussing your treatment plan, it’s beneficial to come prepared with questions and concerns. Understanding how each medication works, what side effects to watch for, and how they interact with your daily life will help set you up for success. The more engaged you are in your care, the more empowered you will feel in the management of your condition.
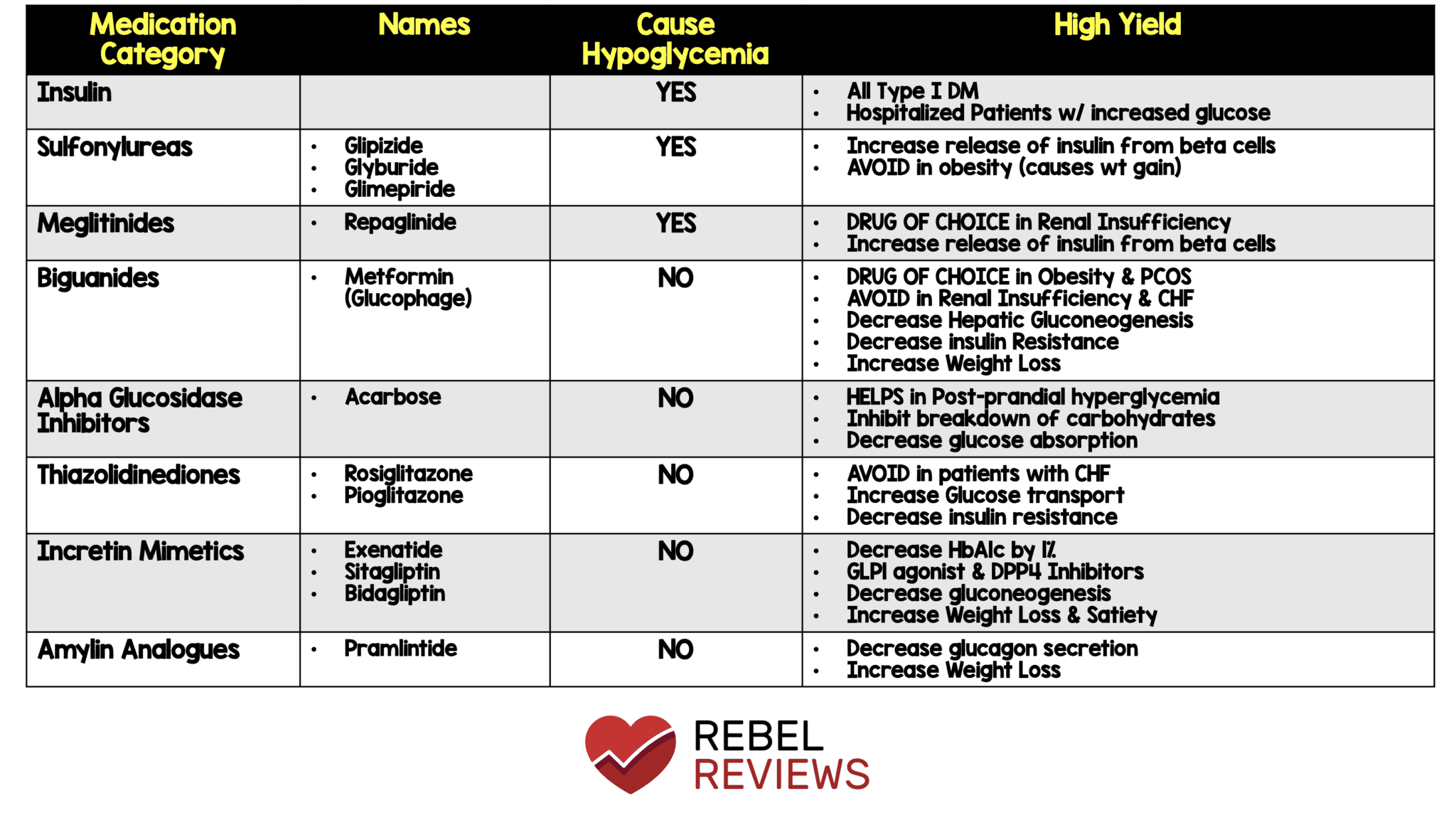
The Role of Lifestyle Changes
Medication is undoubtedly crucial in your journey with diabetes, but it should not be viewed as a standalone solution. Incorporating lifestyle changes is equally vital in managing your blood sugar levels effectively. Dietary modifications, regular exercise, and stress management can have a profound impact on your overall well-being.
Nutrition
Adopting a balanced diet specifically tailored for diabetes can make a significant difference in your blood sugar control. Focusing on whole foods, such as vegetables, lean proteins, healthy fats, and whole grains, will provide your body with the nutrients it needs without spiking your glucose levels. You may want to consider working with a registered dietitian who specializes in diabetes to develop a personalized meal plan.
Exercise
Regular physical activity can enhance your body’s sensitivity to insulin and help regulate blood sugar levels. Aim for at least 150 minutes of moderate aerobic activity each week, combined with strength training exercises. Not only does exercise play a role in diabetes management, but it also contributes to improved mood, better sleep, and increased energy levels. Finding activities you enjoy—whether it’s walking, swimming, or dancing—will make it easier to maintain a consistent routine.
Stress Management
Managing stress is another critical factor in your diabetes journey. Chronic stress can lead to hormonal fluctuations that negatively affect your blood sugar levels. Finding effective techniques for stress relief, such as mindfulness, yoga, deep breathing exercises, or even engaging in hobbies, can significantly impact your ability to manage your condition.
The Psychological Aspect of Diabetes
Living with diabetes can take a toll on your mental health. Many individuals experience feelings of anxiety or depression related to managing the condition. The burden of daily glucose monitoring, diet restrictions, and medication management can feel overwhelming, but you are not alone.
Recognizing the emotional weight that comes with diabetes is the first step toward addressing it. Seeking support—whether through a therapist, support groups, or friends and family—can offer you a safe space to share your feelings and experiences. Opening up about your struggles can lead to a greater understanding of your condition, making it easier to cope.

Regular Monitoring and Follow-up
To ensure your diabetes treatment plan is effective, regular monitoring and check-ups with your healthcare provider are essential. Tracking your blood sugar levels—be it at home or during your medical appointments—will help you understand how well your medications and lifestyle choices are working. Keeping an eye on other relevant health markers, like HbA1c levels, will paint a fuller picture of your overall diabetes management.
Your healthcare provider will also evaluate how well your medications are working, making adjustments as necessary. Stay proactive about your health by communicating any concerns or changes you notice, whether they relate to your blood sugar control, side effects, or any new symptoms that arise.
The Importance of Education
Education is a powerful tool in diabetes management. The more knowledgeable you are about your condition, the better equipped you’ll be to take charge of your health. Many organizations and resources provide valuable information on diabetes, its medications, and how to live well with the condition.
Consider seeking out diabetes education classes or workshops in your area. These programs often cover essential topics like nutrition, physical activity, medication management, and coping strategies. Learning alongside others who share similar experiences can foster a sense of community and support, making your journey with diabetes feel less isolating.

Staying Informed on New Developments
The field of diabetes management continues to evolve, with new medications and technological advancements emerging regularly. Staying informed about these developments can help you work more collaboratively with your healthcare team to explore the best options for your treatment plan. Whether it’s new insights on insulin delivery systems, studies highlighting the effectiveness of certain medications, or other innovations, being an informed patient is crucial.
Engaging with reputable resources—journals, newsletters, or educational platforms—will help you remain up-to-date. Consider subscribing to diabetes-related publications or following organizations dedicated to improving the lives of individuals with diabetes. Knowledge is power, and staying informed will empower you to make the best choices for your health.
Conclusion: Empowering Yourself in Your Diabetes Journey
Living with Diabetes Mellitus is undoubtedly challenging, but it’s essential to remember that you are not alone. Medication plays a pivotal role in managing your blood sugar levels and reducing the risk of complications. Alongside medications, lifestyle modifications, ongoing education, and support systems can empower you to navigate this journey with confidence.
Embracing this holistic approach to diabetes management can lead you to a healthier and more fulfilling life. So, take charge of your health, engage with your healthcare team, and utilize all the tools available to you.
If you found this article helpful, consider giving it a clap, leaving a comment, and subscribing to my Medium newsletter for more updates. Your voice and engagement matter, and together we can navigate the path of diabetes management more effectively.

