Arthritis is a common condition that affects older adults, and it can have a significant impact on their daily lives. In this article, we will explore the age-related factors that contribute to the development of arthritis and discuss effective coping mechanisms that can help individuals manage their symptoms. Whether you are personally dealing with arthritis or looking to support a loved one, this article aims to provide valuable insights and practical advice to enhance your understanding and improve the quality of life for older adults living with arthritis.
Age-Related Factors of Arthritis
Prevalence of arthritis in older adults
Arthritis is a common condition that affects people of all ages, but it is particularly prevalent in older adults. The likelihood of developing arthritis increases with age, with a significant number of seniors being affected. According to the Centers for Disease Control and Prevention (CDC), more than 50% of adults aged 65 years and older have been diagnosed with arthritis. This high prevalence highlights the significance of understanding and managing arthritis in older age.
Types of arthritis commonly found in older adults
There are several types of arthritis that are commonly found in older adults. Osteoarthritis, the most common type, occurs when the protective cartilage on the ends of bones wears down over time. Rheumatoid arthritis, on the other hand, is an autoimmune disease in which the immune system mistakenly attacks the joints. Other types of arthritis that are frequently seen in older adults include gout, psoriatic arthritis, and septic arthritis. Each type of arthritis presents with its unique set of symptoms and requires specific treatment approaches.
Risk factors for developing arthritis in older age
While age is a significant risk factor for developing arthritis, there are other factors that can increase the likelihood of developing the condition in older age. Some common risk factors include a family history of arthritis, previous joint injuries, obesity, and repetitive joint stress due to occupation or leisure activities. Additionally, women tend to have a higher risk of developing arthritis than men. Understanding these risk factors can help individuals take proactive measures to reduce their chances of developing arthritis or manage the condition effectively.
Symptoms and Diagnosis of Arthritis in Older Adults
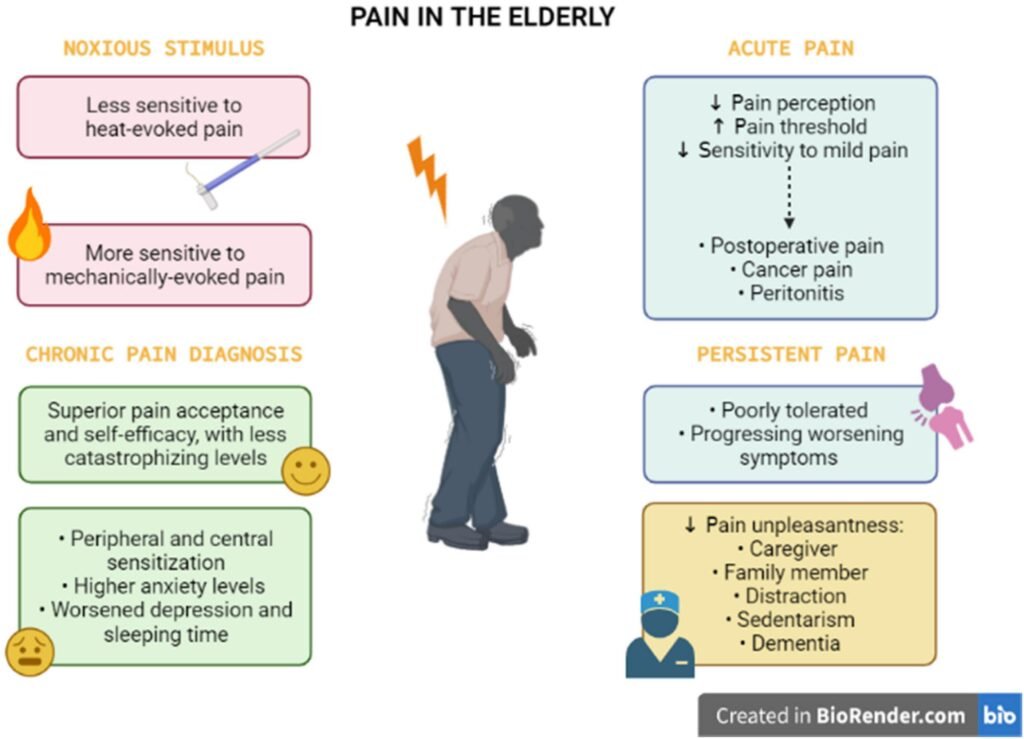
Common symptoms of arthritis in older adults
Arthritis can lead to a variety of symptoms, and older adults may experience these symptoms differently than younger individuals. Common symptoms of arthritis in older adults include joint pain, stiffness, swelling, and difficulty with movement. These symptoms can manifest differently depending on the type of arthritis a person has. For example, those with osteoarthritis may experience joint pain after physical activity or prolonged inactivity, while individuals with rheumatoid arthritis may experience joint swelling and morning stiffness. Recognizing these symptoms is crucial for early intervention and effective management of arthritis.
Diagnostic tests for arthritis in older adults
Diagnosing arthritis in older adults can be challenging due to several factors. Healthcare providers use a combination of diagnostic tests to determine the presence and type of arthritis. These tests may include physical examinations, blood tests, imaging studies such as X-rays or MRIs, and joint fluid analysis. It is important to note that the diagnostic process may require multiple visits and tests to ensure an accurate diagnosis. Older adults should communicate their symptoms and medical history effectively to their healthcare providers to facilitate the diagnostic process.
Challenges in diagnosing arthritis in older adults
Diagnosing arthritis in older adults can be complicated by several factors. The presence of other chronic conditions and associated symptoms can sometimes mask or mimic arthritis symptoms, making it difficult to isolate the exact cause. Additionally, the aging process itself can lead to degenerative changes in the joints, which can further complicate the diagnosis. These challenges highlight the need for thorough evaluation and communication between older adults and their healthcare providers to accurately diagnose and manage arthritis.
Effects of Arthritis on Older Adults
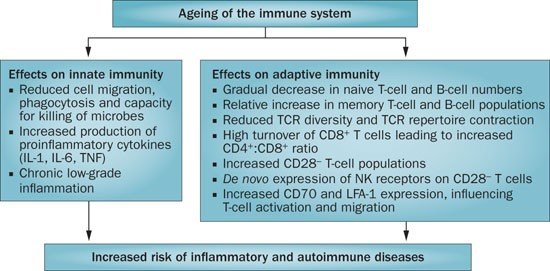
Physical limitations caused by arthritis in older adults
Arthritis can have a significant impact on the physical well-being of older adults. The pain, stiffness, and swelling associated with arthritis can limit mobility and make everyday tasks challenging. For example, simple activities like walking, climbing stairs, or even buttoning a shirt can become difficult or painful. These physical limitations can lead to reduced independence, increased reliance on others, and a loss of overall quality of life. It is crucial for older adults with arthritis to work closely with healthcare professionals to minimize physical limitations and maintain their functional abilities.
Impact of arthritis on mental health in older adults
The effects of arthritis extend beyond physical limitations and can have a profound impact on mental health in older adults. Chronic pain and reduced mobility can lead to feelings of frustration, helplessness, and depression. The loss of independence and the inability to engage in previously enjoyed activities can also contribute to a decline in mental well-being. It is essential for healthcare providers to address both the physical and mental aspects of arthritis in older adults to ensure holistic care and improve overall quality of life.
Quality of life considerations
Arthritis can significantly impact the overall quality of life for older adults. The physical limitations, chronic pain, and psychological distress associated with the condition can lead to reduced social engagement, increased reliance on others for daily activities, and a diminished sense of well-being. However, with the right management strategies, older adults with arthritis can improve their quality of life and maintain independence. It is essential for healthcare providers to assess and address the specific needs and goals of each individual to optimize their overall well-being.
Coping Mechanisms for Arthritis in Older Adults
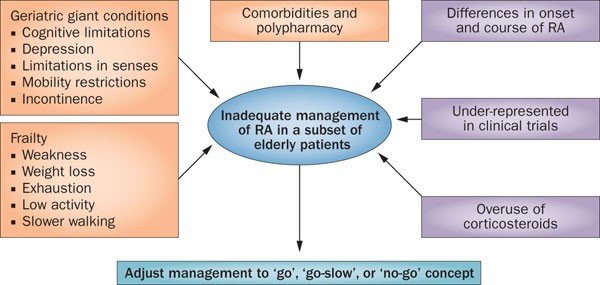
Medical treatment options for arthritis in older adults
Medical treatment options for arthritis in older adults aim to alleviate pain, reduce inflammation, and slow down the progression of the disease. Non-steroidal anti-inflammatory drugs (NSAIDs) are commonly prescribed to manage pain and inflammation. In more severe cases, corticosteroids or disease-modifying antirheumatic drugs (DMARDs) may be recommended. Additionally, therapies such as physical therapy and occupational therapy can help improve mobility and reduce pain. It is important for healthcare providers to tailor treatment plans to the unique needs of older adults to achieve optimal outcomes.
Non-pharmacological interventions for managing arthritis symptoms
In addition to medical treatment options, there are several non-pharmacological interventions that can help manage arthritis symptoms in older adults. These may include heat or cold therapy, joint protection techniques, use of assistive devices, and regular physical exercise. Heat therapy, such as warm compresses or hot showers, can help soothe joint pain and stiffness. Cold therapy, in the form of ice packs or cold compresses, can reduce inflammation and swelling. Joint protection techniques involve modifying daily activities to minimize stress on the joints. Assistive devices, such as canes or braces, can provide additional support and improve mobility. Regular exercise, under the guidance of a healthcare professional, can strengthen muscles, improve joint flexibility, and enhance overall well-being.
Assistive devices and aids to improve mobility
Assistive devices and aids can significantly improve mobility and independence for older adults with arthritis. Options may include wheelchairs, walkers, canes, or orthotic devices. These devices provide support, stability, and relieve pressure on the joints, allowing individuals to perform activities with less pain and strain. Healthcare professionals can assess an individual’s specific needs and recommend appropriate assistive devices to aid in mobility and enhance daily functioning.
Lifestyle Modifications to Manage Arthritis
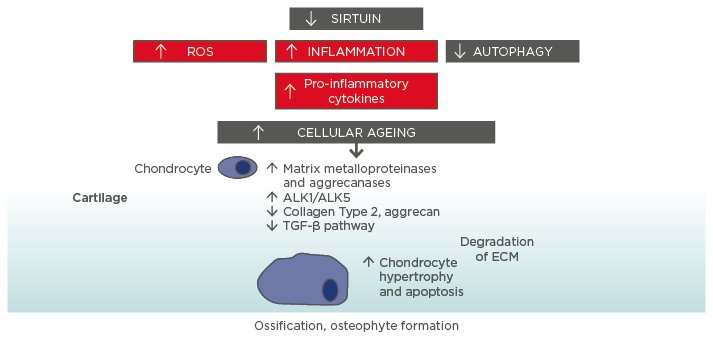
Exercise and physical activity recommendations for older adults with arthritis
Regular exercise and physical activity play a vital role in managing arthritis in older adults. Low-impact exercises, such as swimming, cycling, or walking, can help maintain joint flexibility, strengthen muscles, and improve overall fitness. Healthcare providers may recommend specific exercises tailored to an individual’s condition and capabilities. It is important to start slowly and gradually increase intensity to avoid injury or exacerbation of symptoms. Engaging in regular physical activity can not only alleviate arthritis symptoms but also improve mood, increase energy levels, and enhance overall well-being.
Dietary modifications to reduce arthritis symptoms
While there is no specific diet to cure arthritis, certain dietary modifications can help reduce symptoms and improve overall health in older adults. A well-balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can provide essential nutrients to support joint health and overall well-being. Some individuals may find that certain foods, such as those high in purines (found in red meat and shellfish) or nightshade vegetables (e.g., tomatoes, peppers, and eggplants), worsen their arthritis symptoms. Keeping a food diary and working with a healthcare professional or registered dietitian can help identify any potential trigger foods and create a personalized dietary plan to manage arthritis symptoms effectively.
Weight management strategies for arthritis management
Maintaining a healthy weight is important for managing arthritis in older adults. Excess weight puts additional stress on the joints, exacerbating pain and reducing mobility. Healthcare providers may recommend weight loss strategies through a combination of healthy eating, regular physical activity, and portion control. Achieving and maintaining a healthy weight can not only alleviate arthritis symptoms but also improve overall health and reduce the risk of developing other chronic conditions.
Managing Arthritis Pain in Older Age
Pharmacological pain management options
Pharmacological pain management options are available to help older adults with arthritis cope with pain and improve their quality of life. Commonly used medications include analgesics (pain relievers) such as acetaminophen and opioids, as well as nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen. These medications can help reduce pain and inflammation, but it is important to use them under the guidance of a healthcare professional, considering potential side effects and drug interactions. Regular communication with healthcare providers is essential to ensure the appropriate dosage and duration of medication usage.
Physical therapy and rehabilitation for arthritis pain
Physical therapy and rehabilitation are key components in managing arthritis pain in older adults. Physical therapists can design personalized exercise programs targeting specific joints and muscles to improve strength, flexibility, and mobility. These exercises may be performed in a supervised setting or at home, depending on an individual’s needs and abilities. Physical therapy can also include modalities such as heat or cold therapy, electrical stimulation, or manual therapy techniques to further alleviate pain and improve joint function. Rehabilitation programs aim to reduce pain, enhance mobility, and improve overall quality of life for older adults with arthritis.
Alternative therapies and complementary approaches for pain relief
In addition to conventional treatments, some older adults with arthritis may explore alternative therapies and complementary approaches for pain relief. These may include acupuncture, herbal supplements, massage therapy, or mind-body techniques like yoga or mindfulness meditation. While research on the effectiveness of these approaches is limited, some individuals may find them helpful in managing arthritis symptoms. It is essential for older adults to consult with healthcare providers before incorporating any alternative therapies to ensure safety and prevent potential interactions with existing medications or treatments.
Arthritis-Related Fall Prevention
The link between arthritis and falls in older adults
Arthritis can increase the risk of falls in older adults due to joint pain, stiffness, and reduced mobility. The pain and limitations caused by arthritis can disrupt balance, coordination, and gait, making older adults more susceptible to falls. Furthermore, certain medications used to manage arthritis, such as opioids or muscle relaxants, can also contribute to dizziness or drowsiness, further increasing the risk of falls. Recognizing the link between arthritis and falls is crucial for implementing appropriate fall prevention strategies.
Fall prevention strategies for older adults with arthritis
There are several fall prevention strategies that can help older adults with arthritis stay safe and maintain their independence. These strategies may include:
- Removing tripping hazards at home, such as rugs or cluttered pathways.
- Ensuring proper lighting throughout the house, especially in hallways and staircases.
- Installing grab bars and handrails in bathrooms and other areas where support is needed.
- Wearing sturdy, non-slip footwear with proper arch support.
- Using assistive devices, such as canes or walkers, for added stability.
- Engaging in regular exercise and physical activity to improve balance and strength.
- Reviewing medications with healthcare providers to identify potential side effects or interactions that may increase fall risk.
Implementing these strategies can significantly reduce the risk of falls and maintain the safety of older adults with arthritis.
Home modifications for reducing fall risks
Modifying the home environment can effectively reduce fall risks for older adults with arthritis. Simple changes can be made to improve safety and accessibility. Installing grab bars in the bathroom and shower can provide stability when moving around. Removing loose rugs or securing them with non-slip backing can prevent tripping. Ensuring proper lighting throughout the house, especially in hallways and staircases, can improve visibility and reduce the risk of missteps. Making these modifications can create a safer living environment, enhancing the quality of life for older adults with arthritis.
Arthritis and Sleep Issues in Older Adults
How arthritis affects sleep in older adults
Arthritis can significantly impact the sleep patterns and quality of sleep in older adults. The pain, discomfort, and restricted mobility caused by arthritis can make it challenging to find a comfortable sleeping position. Joint stiffness and swelling may be more pronounced in the morning, making it difficult to get out of bed. The lack of a restful sleep can further lead to fatigue, decreased concentration, and worsened pain during the day. Addressing sleep issues is an important aspect of managing arthritis in older adults.
Tips for better sleep with arthritis
There are several tips that can help older adults with arthritis achieve better sleep:
- Establish a consistent sleep routine by going to bed and waking up at the same time each day.
- Create a comfortable sleep environment with a supportive mattress, pillows, and appropriate bedding.
- Practice good sleep hygiene, such as avoiding stimulating activities or electronic devices before bedtime.
- Use relaxation techniques, such as deep breathing exercises or meditation, to promote a sense of calm before sleep.
- Incorporate gentle stretching or relaxation exercises before bed to alleviate pain and stiffness.
- If necessary, use assistive devices such as pillows or mattress toppers to support painful joints during sleep.
- Consult with healthcare providers about potential sleep aids or medications that may facilitate better sleep if other strategies are not effective.
By implementing these tips, older adults with arthritis can improve their sleep quality, leading to enhanced overall well-being.
Sleep aids and accessories for arthritis
Certain sleep aids and accessories can help older adults with arthritis achieve a more comfortable sleep:
- Mattress toppers or overlays designed to provide additional cushioning and support for painful joints.
- Pillows specifically designed to support the neck, back, or knees, depending on the individual’s needs.
- Electric blankets or heating pads to apply gentle warmth to sore joints before sleep.
- Adjustable beds that allow for customization of sleeping positions based on comfort needs.
- Orthopedic sleepwear, such as gloves or socks with built-in joint supports, that can provide compression and alleviate pain.
It is important to consider individual preferences and consult with healthcare providers or sleep specialists to identify the most suitable sleep aids and accessories for addressing arthritis-related sleep issues.
Psychological Support for Arthritis in Older Adults
The importance of mental health support for older adults with arthritis
Arthritis can have a significant impact on the mental well-being of older adults. The chronic pain, physical limitations, and changes in lifestyle associated with arthritis can lead to increased stress, anxiety, and depression. It is important to recognize the emotional challenges faced by older adults with arthritis and provide appropriate mental health support. Addressing the psychological aspects can enhance overall well-being and improve the management of arthritis.
Counseling and therapy options for arthritis-related emotional challenges
Counseling and therapy can provide valuable support for older adults with arthritis who are struggling with emotional challenges. Cognitive-behavioral therapy (CBT) can help individuals develop coping strategies, manage pain perception, and improve overall mental well-being. Supportive counseling or talk therapy can provide a safe space for individuals to express their feelings, concerns, and frustrations related to arthritis. These therapeutic approaches can empower older adults to develop resilience, enhance self-management skills, and improve their overall quality of life.
Support groups and community resources
Support groups and community resources can offer invaluable support and connection for older adults with arthritis. Joining a support group allows individuals to share experiences, gain insights, and receive emotional support from others who are going through similar challenges. Support groups can be in-person or online, providing a range of options depending on an individual’s comfort and accessibility. Additionally, community resources such as senior centers or nonprofit organizations may offer educational programs, workshops, or recreational activities specifically tailored for older adults with arthritis. These resources can not only provide information but also foster a sense of community and belonging.
Planning for Arthritis Management in Older Age
Developing an arthritis management plan in coordination with healthcare providers
Developing an arthritis management plan is essential for older adults to effectively manage the condition and optimize their overall well-being. A comprehensive plan should involve coordination and collaboration with healthcare providers, including doctors, physical therapists, occupational therapists, and mental health professionals. The plan should outline specific goals, treatment options, exercise recommendations, and lifestyle modifications tailored to an individual’s needs and preferences. Regular communication, follow-up appointments, and adjustments to the plan as needed are crucial for achieving desired outcomes.
Financial considerations for arthritis treatment and management
Managing arthritis in older age may come with financial considerations. Healthcare costs can vary depending on the type and severity of arthritis, as well as the specific treatments involved. It is important for older adults to understand their insurance coverage, Medicare benefits, and any potential out-of-pocket expenses. Exploring financial assistance programs, discounts on medications, or community resources can help alleviate any financial burden associated with arthritis treatment and management. Open communication with healthcare providers about financial concerns can further facilitate access to appropriate resources and support.
Long-term care options for older adults with arthritis
In some cases, older adults with arthritis may require long-term care options to ensure a safe and supportive environment. Assisted living facilities, nursing homes, or residential care communities can provide comprehensive care and assistance with daily activities for individuals with arthritis. These options can offer 24/7 support, medication management, physical therapy services, and social engagement opportunities. It is important for older adults and their families to explore and discuss long-term care options with healthcare providers and consider their specific needs, preferences, and financial situations.
In conclusion, understanding the age-related factors of arthritis is crucial for effectively managing the condition in older adults. Recognizing the prevalence, types, and risk factors associated with arthritis can guide healthcare providers and individuals in implementing appropriate strategies. Addressing the symptoms and achieving an accurate diagnosis are essential for early intervention and improved outcomes. The physical and mental impact of arthritis can be significant, emphasizing the importance of holistic care and support. Coping mechanisms, lifestyle modifications, and fall prevention strategies can enhance overall well-being and independence for older adults with arthritis. Additionally, managing arthritis-related pain, sleep issues, and psychological challenges can significantly improve the quality of life in older age. By planning for arthritis management in coordination with healthcare providers, considering financial considerations, and exploring long-term care options if necessary, older adults can navigate arthritis and maintain their well-being in older age.
