Bronchiectasis is a condition affecting the airways in children, resulting in symptoms that can significantly impact their daily lives. This article explores the symptoms and treatment options for bronchiectasis, providing valuable insights for parents and caregivers. By understanding the signs to look out for and the available treatments, you can ensure that your child receives the necessary care and support to manage this condition effectively.
Overview of Bronchiectasis
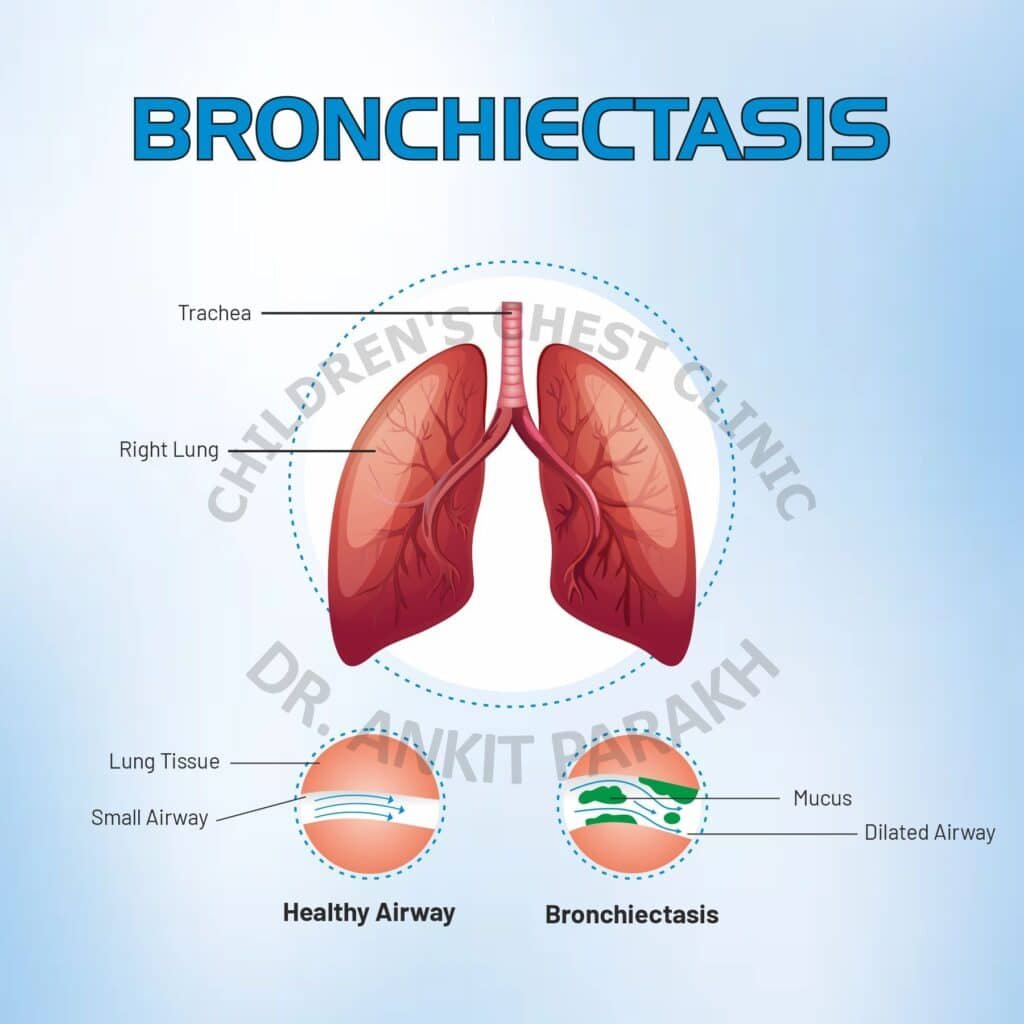
Bronchiectasis is a chronic respiratory condition that affects the bronchi, which are the airways in the lungs. This condition is characterized by the permanent dilation and thickening of the bronchi, leading to the accumulation of mucus and subsequent infections.
Definition of Bronchiectasis
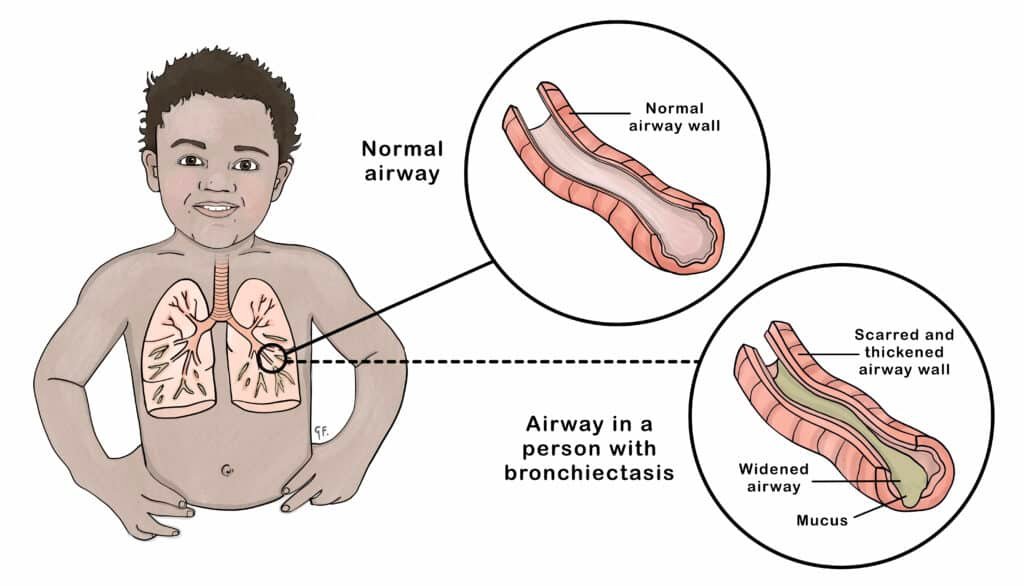
Bronchiectasis is a condition where the bronchi become permanently widened and inflamed. This leads to a build-up of mucus, which can result in recurrent respiratory infections and other symptoms such as coughing, wheezing, and shortness of breath.
Causes of Bronchiectasis
Bronchiectasis can have various causes, including:
- Infections: Repeated respiratory infections, such as pneumonia or whooping cough, can cause damage to the bronchi and lead to bronchiectasis.
- Cystic Fibrosis: This genetic disorder affects the production of mucus in the body, leading to its accumulation in the bronchi.
- Immunodeficiency Disorders: Conditions that weaken the immune system, such as HIV or primary immunodeficiency disorders, can increase the risk of bronchiectasis.
- Abnormalities in the Airways: Structural abnormalities in the airways, such as ciliary dyskinesia or conditions present at birth, can contribute to bronchiectasis.
- Aspiration: Inhalation of foreign objects or stomach acid into the lungs can cause inflammation and damage to the bronchi.
Prevalence of Bronchiectasis in Children
Bronchiectasis is more commonly seen in adults, but it can also occur in children. The prevalence of bronchiectasis in children varies across different populations and countries. In some regions, the prevalence is higher due to factors such as a higher incidence of respiratory infections or a high prevalence of conditions like cystic fibrosis. Early recognition and appropriate management are essential to minimize the impact of bronchiectasis on children’s health and well-being.
Symptoms of Bronchiectasis in Children
Recognizing the symptoms of bronchiectasis in children is crucial for prompt diagnosis and treatment. Common symptoms include:
Persistent cough
Children with bronchiectasis often have a chronic, persistent cough that may be worse in the morning or after physical activity. This cough can produce large amounts of mucus and may be productive.
Excessive mucus production
One noticeable symptom of bronchiectasis is the excessive production of thick, sticky mucus. This mucus can be difficult to clear, leading to further complications and recurrent infections.
Shortness of breath
Children with bronchiectasis may experience shortness of breath, especially during physical exertion or when the airways are narrowed due to mucus blockage.
Recurrent respiratory infections
Frequent respiratory infections, such as pneumonia or bronchitis, are common in children with bronchiectasis. These infections can lead to a worsening of symptoms and may require medical intervention.
Wheezing
Wheezing, a high-pitched whistling sound during breathing, is another common symptom of bronchiectasis. It occurs due to narrowed airways and can be especially noticeable during exhalation.
Fatigue
Children with bronchiectasis may experience fatigue or low energy levels due to the strain on their respiratory system. Fatigue can affect their overall quality of life and daily activities.
Diagnosing Bronchiectasis in Children
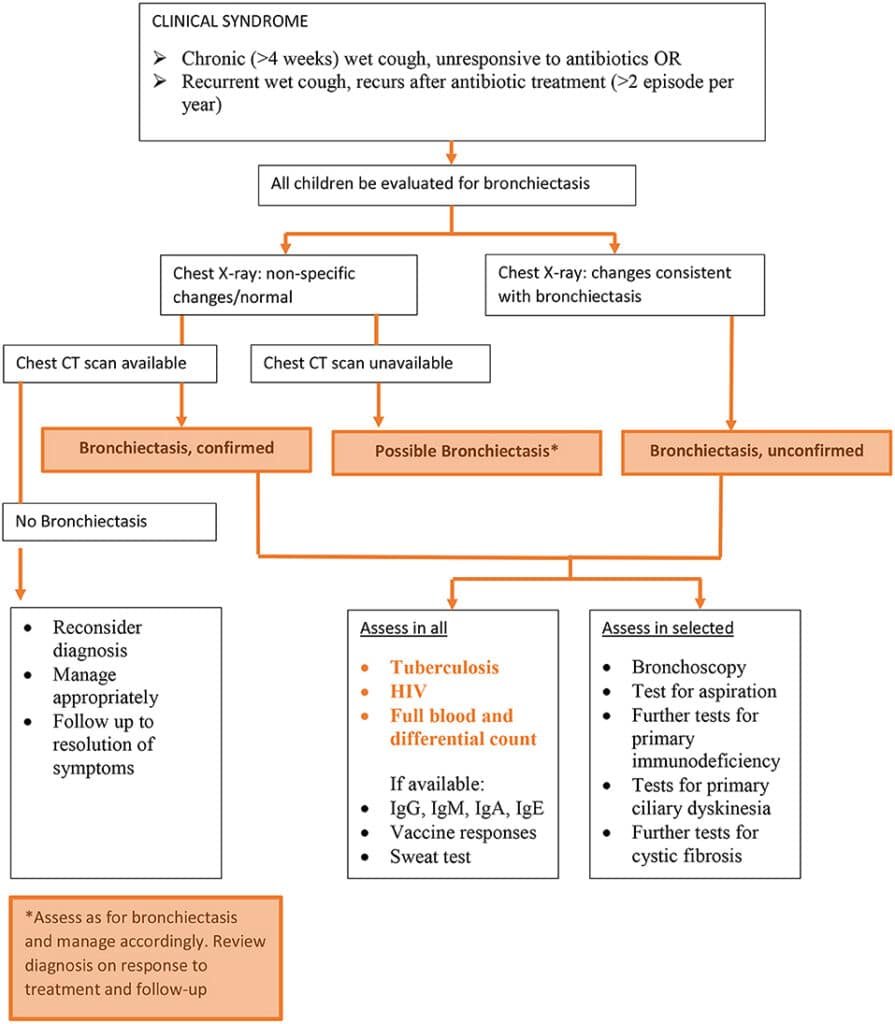
Prompt and accurate diagnosis of bronchiectasis is essential for initiating appropriate treatment and preventing complications. Several diagnostic methods may be used:
Medical history and physical examination
A detailed medical history, including information about respiratory symptoms and previous infections, is important in diagnosing bronchiectasis. A thorough physical examination may reveal abnormal lung sounds or other indicators of the condition.
Chest X-ray
A chest X-ray can provide valuable information about the structure and condition of the lungs. It may show signs of bronchiectasis, such as dilated airways or areas of inflammation.
CT scan
A computed tomography (CT) scan is a more detailed imaging technique that can help confirm the diagnosis of bronchiectasis. It provides clear images of the airways, allowing doctors to assess the extent and severity of the condition.
Sputum culture
A sputum culture involves analyzing a sample of mucus coughed up from the lungs. It helps identify any specific bacteria or fungi causing respiratory infections, guiding the choice of appropriate antibiotics for treatment.
Bronchoscopy
In some cases, a bronchoscopy may be performed to directly visualize the airways using a thin, flexible tube with a camera. This procedure allows the doctor to assess the condition of the bronchi and collect samples for further analysis.
Treating Bronchiectasis in Children
The treatment of bronchiectasis in children focuses on managing symptoms, preventing infections, and improving airway clearance. The following treatment options may be utilized:
Antibiotics
Antibiotics are commonly prescribed to treat respiratory infections associated with bronchiectasis. The choice of antibiotic depends on the specific infection and the results of sputum culture.
Chest physiotherapy
Chest physiotherapy techniques aim to clear mucus from the airways. This can be done through techniques such as postural drainage, percussion, and breathing exercises. Regular chest physiotherapy sessions are often recommended to improve airway clearance.
Bronchodilators
Bronchodilators, such as inhalers or nebulizers, help relax the muscles surrounding the airways, allowing for easier breathing. They may be prescribed to manage symptoms like wheezing or shortness of breath.
Mucus thinning medications
Medications designed to thin and loosen mucus can be beneficial for children with bronchiectasis. These medications make it easier for mucus to be expelled from the airways and reduce the risk of blockages.
Lung transplantation
In severe cases where bronchiectasis leads to significant lung damage, a lung transplantation may be considered. This option is typically reserved for children who do not respond to other treatments and have a decreased quality of life.

Preventing Complications of Bronchiectasis in Children
Preventing complications and reducing the frequency of respiratory infections are important goals in the management of bronchiectasis. The following measures can help minimize the impact of the condition:
Vaccinations
Ensuring that children with bronchiectasis are up to date with their vaccinations, particularly against respiratory infections like influenza and pneumococcal disease, can help prevent severe respiratory infections.
Regular check-ups
Regular check-ups with healthcare professionals are important to monitor the progression of bronchiectasis and identify any potential complications. This allows for prompt intervention and adjustment of treatment plans if necessary.
Maintaining good respiratory hygiene
Practicing good respiratory hygiene, such as covering the mouth and nose when coughing or sneezing, can help prevent the spread of respiratory infections. This is particularly important in settings where children come into close contact with others, such as school or daycare.
Avoiding environmental triggers
Identifying and avoiding environmental triggers that exacerbate respiratory symptoms is crucial. These triggers can include allergens like dust mites or pet dander, smoke, or certain chemicals.
Pulmonary rehabilitation
Pulmonary rehabilitation programs may be beneficial for children with bronchiectasis. These programs can help improve lung function, increase physical activity tolerance, and enhance overall well-being.
Managing Bronchiectasis at Home
Managing bronchiectasis at home is essential for maintaining good health and minimizing symptom flare-ups. The following measures can be taken:
Proper nutrition and hydration
Ensuring that children with bronchiectasis have a well-balanced diet and stay hydrated is important for supporting overall health and immune function. Maintaining a healthy body weight can also help reduce the strain on the respiratory system.
Breathing exercises
Teaching children breathing exercises, such as deep breathing and pursed-lip breathing, can help improve lung function and reduce shortness of breath. These exercises can be incorporated into daily routines or during episodes of respiratory distress.
Airway clearance techniques
Parents and caregivers should be familiar with airway clearance techniques recommended by healthcare professionals. These techniques, such as chest percussion or the use of oscillatory devices, help loosen and clear mucus from the airways.
Medication adherence
Ensuring proper adherence to prescribed medications is crucial for managing bronchiectasis effectively. Parents and caregivers should ensure that medications are taken as directed and maintain a consistent schedule.
Supportive care
Providing emotional support and creating a positive, supportive environment can greatly benefit children with bronchiectasis. It is important to address any concerns or questions they may have and involve them in their own care as they grow older.
Tips for Parents and Caregivers
Parents and caregivers play a vital role in caring for children with bronchiectasis. The following tips can help them navigate the challenges of managing this condition:
Educating themselves about bronchiectasis
By learning about bronchiectasis, its symptoms, treatment options, and potential complications, parents and caregivers can better advocate for their child’s health needs and communicate effectively with healthcare professionals.
Creating a safe and clean environment
Ensuring that the child’s living environment is clean and free from potential respiratory irritants, such as smoke or strong chemicals, can help reduce the risk of exacerbations. Regular cleaning and proper ventilation are important.
Developing a routine for treatments and medications
Establishing a consistent routine for treatments and medication administration can help ensure that they are not missed or overlooked. This routine should be age-appropriate and adaptable as the child grows older.
Being vigilant for signs of complications
Parents and caregivers should be aware of any changes in their child’s symptoms or overall health. If there are signs of worsening bronchiectasis or complications, timely medical intervention should be sought.
Seeking support from healthcare professionals and support groups
Seeking guidance and support from healthcare professionals and connecting with support groups or organizations dedicated to bronchiectasis can be invaluable. These resources can provide information, emotional support, and a sense of community for parents and caregivers.
Long-Term Outlook for Children with Bronchiectasis
The long-term outlook for children with bronchiectasis varies depending on the underlying cause of the condition, the severity of symptoms, and the effectiveness of treatment. With appropriate management and adherence to treatment plans, many children with bronchiectasis can lead fulfilling and healthy lives.
Prognosis and life expectancy
Prognosis and life expectancy in children with bronchiectasis can be influenced by several factors. Early diagnosis, appropriate treatment, and diligent management of symptoms can improve long-term outcomes and reduce the risk of complications.
Monitoring and managing disease progression
Regular monitoring of lung function and overall health is important in managing bronchiectasis. This may involve periodic lung function tests, imaging studies, and regular check-ups with healthcare professionals to assess any changes in symptoms or disease progression.
Transitioning to adult care
As children with bronchiectasis grow older, they will need to transition from pediatric care to adult care. This transition may involve finding appropriate healthcare providers who specialize in adult bronchiectasis management and ensuring a smooth transfer of medical records and treatment plans.
Supporting overall well-being
Supporting overall well-being involves addressing not only the physical aspects of bronchiectasis but also the emotional and social aspects. Encouraging a positive mindset, providing opportunities for social interaction, and supporting the child’s interests and goals can contribute to their overall well-being and quality of life.
Research and Advances in Bronchiectasis Treatment
Ongoing research and advancements in the field of bronchiectasis treatment offer hope for improved outcomes and new treatment options. Some areas of focus include:
Emerging therapies
Researchers are exploring new therapies, including novel antibiotics, anti-inflammatory medications, and immune-modulating agents, to better manage bronchiectasis and its associated complications.
Clinical trials
Clinical trials provide opportunities for children with bronchiectasis to access new treatment options and contribute to medical advancements. These trials help evaluate the safety and effectiveness of new therapies and may offer promising options for future management.
Advances in imaging techniques
Advancements in imaging techniques, such as high-resolution CT scans and functional pulmonary imaging, allow for more accurate assessment of bronchiectasis and the underlying lung function. This can aid in diagnosis, treatment planning, and monitoring disease progression.
Improved understanding of underlying mechanisms
Researchers are continually striving to better understand the underlying mechanisms of bronchiectasis. This knowledge can help identify new therapeutic targets and develop personalized treatment approaches for children with bronchiectasis.
Conclusion
Bronchiectasis is a chronic respiratory condition that can significantly impact the health and well-being of children. Prompt recognition of symptoms, accurate diagnosis, and appropriate management are essential for minimizing the impact of bronchiectasis, preventing complications, and improving the quality of life for affected children. With advances in treatment options and ongoing research, there is hope for continued improvement in the management of bronchiectasis in children. By working together with healthcare professionals, parents, and caregivers can provide the necessary support and care to help children thrive despite the challenges posed by this condition.
