Bronchiectasis is a chronic lung condition that, although not widely known, affects numerous individuals worldwide. This article aims to shed light on the various aspects of bronchiectasis, including its causes, symptoms, and treatment options. By gaining a better understanding of this condition, you can equip yourself with the knowledge needed to identify its signs and seek appropriate medical assistance. So, let’s explore the world of bronchiectasis together, and discover how we can manage this condition effectively for a healthier and happier life.
Understanding Bronchiectasis: Causes, Symptoms, and Treatment
Definition and Overview
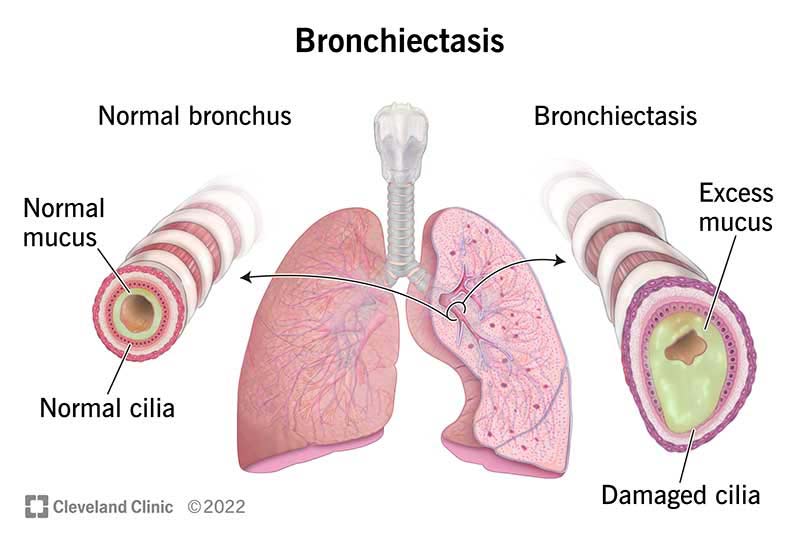
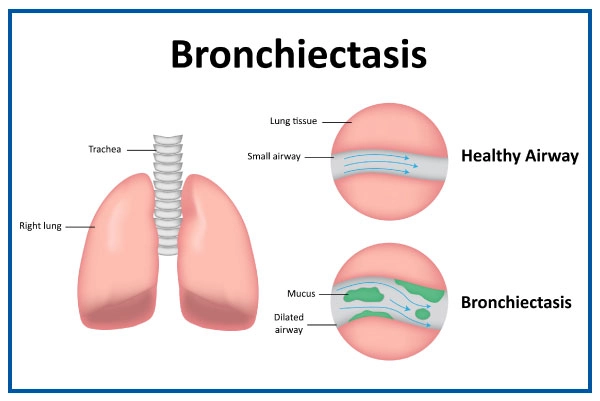
Bronchiectasis is a chronic lung condition characterized by the irreversible dilation and thickening of the bronchial tubes, which carry air to and from the lungs. This abnormal widening of the airways can lead to a buildup of mucus and make it difficult for the lungs to clear out bacteria and other foreign substances. As a result, recurrent respiratory infections and inflammation occur, leading to further damage and deterioration of lung function over time.
Causes of Bronchiectasis
There are several factors that can contribute to the development of bronchiectasis:
1. Genetic Factors
In some cases, bronchiectasis may be caused by genetic factors. Certain inherited conditions, such as cystic fibrosis and primary ciliary dyskinesia, can lead to abnormalities in the structure and function of the airways. This predisposes individuals to develop bronchiectasis at an early age.
2. Respiratory Infections
Recurrent or severe respiratory infections, such as pneumonia or tuberculosis, can cause damage to the bronchial walls, leading to bronchiectasis. Bacterial and fungal infections that are not properly treated or are not responsive to treatment can also contribute to the development of this condition.
3. Chronic Obstructive Pulmonary Disease (COPD)
Long-term exposure to irritants and inhalation of pollutants, such as cigarette smoke or industrial chemicals, can result in the development of COPD. Over time, COPD can lead to the destruction of lung tissue and the development of bronchiectasis.
4. Immune System Disorders
Autoimmune disorders, such as rheumatoid arthritis or lupus, can cause inflammation in the bronchial tubes, leading to their dilation and subsequent bronchiectasis. Conditions that weaken the immune system, such as HIV/AIDS or certain medications, can also make individuals more susceptible to developing bronchiectasis.

5. Other Underlying Conditions
Certain health conditions, such as gastroesophageal reflux disease (GERD), allergic bronchopulmonary aspergillosis (ABPA), or bronchial obstruction, can contribute to the development of bronchiectasis. These conditions create an environment in the airways that is conducive to bacterial growth and can lead to chronic inflammation.
Signs and Symptoms
Bronchiectasis often presents with a range of symptoms that can vary in severity from person to person. Some common signs and symptoms include:
1. Persistent Cough
A persistent cough that produces large amounts of mucus is a hallmark symptom of bronchiectasis. The cough may worsen upon waking up in the morning or when lying down, and may be accompanied by wheezing or a whistling sound during breathing.
2. Recurrent Respiratory Infections
Individuals with bronchiectasis are prone to frequent respiratory infections, such as bronchitis or pneumonia. These infections can be more severe and last longer than in individuals without bronchiectasis.
3. Shortness of Breath
The abnormal dilation of the bronchial tubes can make it difficult for air to flow freely in and out of the lungs, leading to shortness of breath. This symptom may worsen with physical activity or during respiratory infections.
4. Chest Pain
Some individuals with bronchiectasis may experience chest pain or discomfort. This can be due to the strain on the chest muscles during coughing or the inflammation in the airways.
5. Fatigue and Weakness
Bronchiectasis can cause a general feeling of fatigue and weakness. This can be attributed to the body working harder to compensate for the impaired lung function and the chronic inflammation in the airways.
Diagnosis and Medical Evaluation
To diagnose bronchiectasis and determine the underlying cause, several tests and evaluations may be conducted:
1. Medical History and Physical Examination
Your healthcare provider will review your medical history and ask about your symptoms, including any recent infections or exposure to environmental factors. A physical examination, including listening to your lungs and examining your chest, may also be performed to assess any abnormalities.
2. Imaging Tests
Imaging tests, such as chest X-rays or computed tomography (CT) scans, can provide detailed images of the lungs and airways. These tests can help identify any dilation or thickening of the bronchial tubes, as well as evaluate the extent and location of bronchiectasis.
3. Lung Function Tests
Lung function tests, including spirometry and pulmonary function tests, measure how well your lungs are working and help assess the severity of bronchiectasis. These tests measure parameters such as the amount of air you can breathe in and out and how quickly you can exhale.
4. Sputum Culture and Microbiological Analysis
A sample of your sputum may be collected and analyzed to identify any bacteria or fungi that may be causing or contributing to respiratory infections. This can help guide appropriate antibiotic treatment.

5. Bronchoscopy
In some cases, a bronchoscopy may be performed to directly visualize the airways using a flexible tube with a camera. This procedure allows your doctor to examine the bronchial tubes for any abnormalities, take biopsies if required, and collect samples for further analysis.
Treatment Options
The treatment of bronchiectasis aims to manage symptoms, prevent complications, and improve overall lung function. Treatment options may include:
1. Medications
Bronchodilators, which help relax the muscles around the airways, and inhaled corticosteroids, which decrease inflammation in the airways, may be prescribed to improve airflow and alleviate symptoms. In certain cases, medications to thin mucus and facilitate its clearance may also be prescribed.
2. Chest Physiotherapy
Chest physiotherapy techniques, such as postural drainage, percussion, and breathing exercises, can help mobilize mucus in the lungs and improve its clearance. These techniques are typically taught by respiratory therapists and can be performed at home or in clinical settings.
3. Antibiotics
Antibiotics may be prescribed to treat bacterial infections associated with bronchiectasis. The choice of antibiotics is based on the results of sputum culture and microbiological analysis. Long-term antibiotic therapy may be necessary in some cases to prevent recurrent infections.
4. Vaccinations
Vaccinations, such as the influenza vaccine and the pneumococcal vaccine, can help prevent respiratory infections and their complications. It is important for individuals with bronchiectasis to stay up to date with all recommended vaccinations.

5. Surgical Interventions
In severe cases of bronchiectasis that do not respond to conservative treatment, surgical interventions may be considered. Surgical options include the removal of diseased lung segments or lobes (lobectomy), or lung transplantation in extreme cases.
Preventive Measures
Taking certain precautions can help minimize the risk of developing bronchiectasis or prevent its progression:
1. Avoidance of Respiratory Infections
Practicing good hand hygiene, avoiding close contact with sick individuals, and maintaining a clean environment can help reduce the risk of respiratory infections. It is also important to seek appropriate medical treatment for any respiratory infections to prevent them from becoming chronic.
2. Regular Exercise and Healthy Lifestyle
Engaging in regular physical activity and maintaining a healthy lifestyle can help strengthen the immune system and improve overall lung function. Regular exercise can also support the clearance of mucus from the airways.
3. Vaccinations and Immunizations
Keeping up to date with vaccinations, as recommended by healthcare professionals, can provide protection against respiratory infections and their complications. It is essential for individuals with bronchiectasis to receive the influenza vaccine annually and the pneumococcal vaccine as recommended.
4. Self-Care and Monitoring
Learning to manage symptoms and taking appropriate self-care measures, such as staying well-hydrated and avoiding environmental irritants, can help individuals with bronchiectasis maintain better control over their condition. Regular monitoring of symptoms and seeking medical advice when needed is also crucial for early intervention.
5. Support and Education for Patients and Caregivers
Support groups and educational resources can provide valuable information and emotional support for individuals living with bronchiectasis and their caregivers. Learning about the condition, its management, and available resources can empower patients and improve their quality of life.
Prognosis and Outlook
The prognosis of bronchiectasis can vary depending on the underlying cause, the severity of the condition, and the individual’s overall health. Early diagnosis and appropriate treatment can help slow down the progression of bronchiectasis, manage symptoms, and improve quality of life.
1. Disease Progression and Prognostic Factors
If left untreated or poorly managed, bronchiectasis can progress and lead to further lung damage and decreased lung function. Factors such as the underlying cause, the presence of other health conditions, and adherence to treatment can influence the prognosis of bronchiectasis.
2. Quality of Life and Psychosocial Impact
Bronchiectasis can have a significant impact on a person’s quality of life. The chronic cough, recurrent infections, and shortness of breath can limit physical activities, disrupt sleep, and cause emotional distress. Managing symptoms, seeking support, and maintaining a positive mindset can help improve the overall well-being and mental health of individuals with bronchiectasis.
3. Management and Long-Term Outlook
With proper management, individuals with bronchiectasis can experience improved lung function and a better quality of life. Adhering to treatment plans, staying informed about the condition, and maintaining regular follow-ups with healthcare providers can help ensure long-term control and optimal outcomes.
Conclusion
Bronchiectasis is a chronic lung condition that requires comprehensive understanding and targeted treatment. By identifying the underlying causes, recognizing the symptoms, and implementing appropriate management strategies, individuals with bronchiectasis can enhance their overall well-being and maintain a fulfilling life. Stay informed, seek support, and work closely with your healthcare team to effectively manage bronchiectasis and enjoy a healthier future.