Acute Lymphoblastic Leukemia, often referred to as ALL, is a type of cancer that affects the white blood cells. It is most commonly seen in children but can also occur in adults. In this article, we will explore the current treatments available for ALL, including chemotherapy, targeted therapy, stem cell transplant, and radiation therapy. These treatment options, when combined with supportive care, offer hope for patients diagnosed with ALL, improving their chances of remission and long-term survival. So, let’s delve into the world of ALL treatments and explore the progress being made in fighting this disease.
Chemotherapy
Chemotherapy plays a central role in the treatment of acute lymphoblastic leukemia (ALL). It involves the use of powerful drugs to kill cancer cells and prevent their proliferation. Chemotherapy is typically administered in different stages or phases to maximize its effectiveness and minimize side effects.
Induction therapy
Induction therapy is the initial phase of chemotherapy in ALL treatments. Its goal is to quickly kill as many leukemia cells as possible and achieve remission. This phase usually lasts for several weeks and involves intensive treatment with a combination of chemotherapy drugs. The specific drugs used may vary depending on the patient’s age and overall health, as well as the subtype of ALL.
Consolidation therapy
After achieving remission with induction therapy, consolidation therapy is initiated to eliminate any remaining cancer cells and further reduce the risk of relapse. This phase involves additional cycles of chemotherapy to target residual leukemia cells. Consolidation therapy is also crucial in preparing the body for other treatments, such as stem cell transplantation.
Maintenance therapy
Maintenance therapy is a long-term treatment phase that follows induction and consolidation therapies. Its purpose is to prevent a relapse by keeping any remaining cancer cells in check. Generally, lower doses of chemotherapy drugs are used during this phase, administered over a period of one to two years. The specific drugs and duration of maintenance therapy may vary based on the patient’s individual circumstances.
Central nervous system prophylaxis
ALL has the potential to spread to the central nervous system (CNS), including the brain and spinal cord. To minimize this risk, central nervous system prophylaxis is administered during chemotherapy treatment. This involves the use of chemotherapy drugs that can penetrate the CNS and kill leukemia cells in the brain and spinal fluid. Intrathecal therapy, where medication is directly injected into the cerebrospinal fluid, is often employed for this purpose.
Chemotherapy drugs used
There are several chemotherapy drugs commonly used in the treatment of ALL. Some of the most frequently utilized ones include vincristine, prednisone, doxorubicin, cyclophosphamide, cytarabine, methotrexate, and mercaptopurine. These drugs work in different ways to target and destroy leukemia cells throughout the body. The specific combination of drugs and dosages will depend on factors such as the patient’s age, overall health, and subtype of ALL.
Targeted Therapy
Targeted therapy is a relatively newer approach to treating ALL. It involves the use of drugs that specifically target the abnormalities or genetic mutations present in leukemia cells. This precision targeting enables the medication to selectively attack cancer cells while minimizing harm to healthy cells, thereby reducing side effects.
Tyrosine kinase inhibitors
Tyrosine kinase inhibitors (TKIs) are a type of targeted therapy used in the treatment of specific genetic subtypes of ALL. These drugs work by blocking the activity of enzymes called tyrosine kinases that are involved in the growth and survival of cancer cells. TKIs, such as imatinib, dasatinib, and ponatinib, have shown promising results in patients with Philadelphia chromosome-positive ALL.
Monoclonal antibodies
Monoclonal antibodies are another type of targeted therapy used in the treatment of ALL. These antibodies are designed to recognize and bind to specific proteins found on the surface of leukemia cells. By doing so, they can interfere with the growth and survival of cancer cells, trigger the immune system to attack them or deliver toxic substances directly to the cancer cells. Some examples of monoclonal antibodies used in ALL treatments include rituximab, blinatumomab, and inotuzumab ozogamicin.
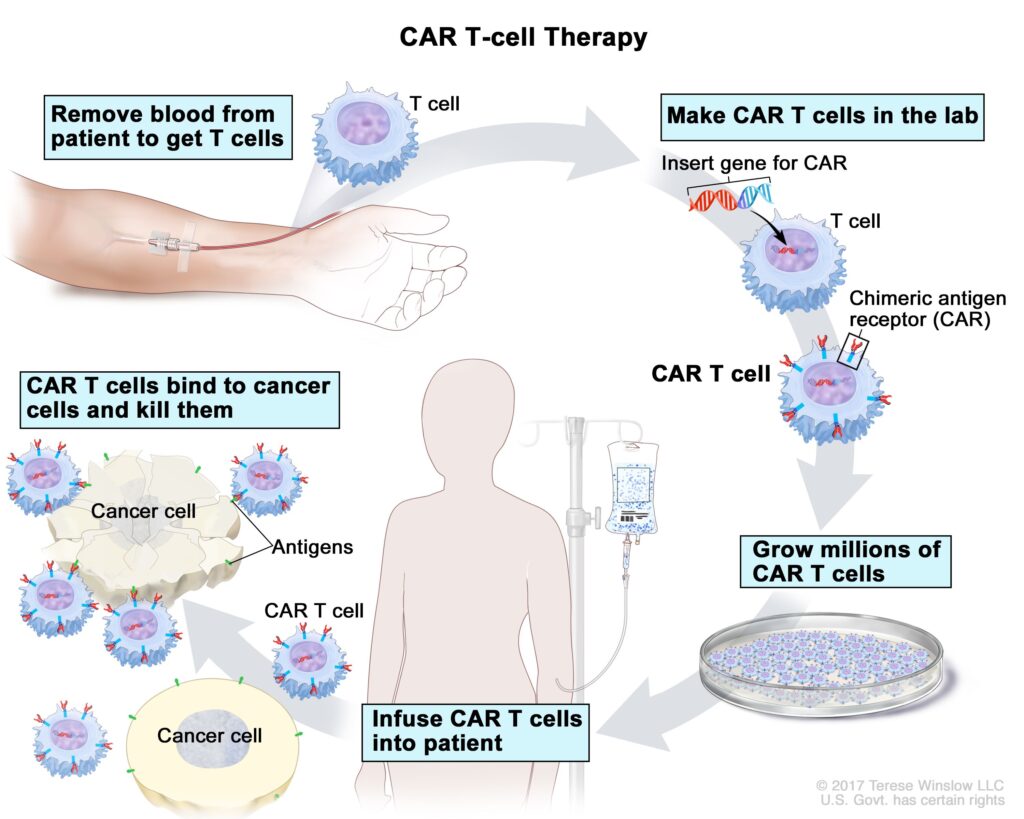
Chimeric antigen receptor (CAR) T-cell therapy
CAR T-cell therapy is an innovative immunotherapy approach that has shown remarkable success in treating relapsed or refractory ALL. It involves modifying a patient’s own T cells to express a chimeric antigen receptor, which enables them to recognize and kill cancer cells. These modified CAR T cells are then infused back into the patient’s bloodstream. CAR T-cell therapies such as tisagenlecleucel and axicabtagene ciloleucel have demonstrated high response rates and durable remissions in some patients with ALL.
Bispecific antibodies
Bispecific antibodies are a type of targeted therapy that can simultaneously bind to both cancer cells and immune cells. By bringing them into close proximity, they enhance the immune system’s ability to recognize and eliminate cancer cells. Blinatumomab is a notable example of a bispecific antibody used in the treatment of ALL. It connects T cells with leukemia cells bearing specific markers, resulting in the destruction of the cancer cells.

Stem Cell Transplantation
Stem cell transplantation is a treatment option for some patients with ALL, particularly those at high risk of relapse or who have relapsed after initial treatment. It involves replacing the patient’s diseased bone marrow with healthy stem cells from a donor (allogeneic stem cell transplantation) or the patient’s own stem cells (autologous stem cell transplantation).
Allogeneic stem cell transplantation
Allogeneic stem cell transplantation, also known as allograft, uses stem cells from a genetically matched donor, usually a sibling or an unrelated donor. The healthy stem cells are collected from the donor and infused into the patient’s bloodstream, where they migrate to the bone marrow and begin producing new, healthy blood cells. This procedure allows for a complete replacement of the patient’s immune system and has the potential for a curative effect in ALL.
Autologous stem cell transplantation
Autologous stem cell transplantation, also known as autograft, utilizes the patient’s own stem cells, which are collected prior to high-dose chemotherapy treatment. These stem cells are stored and then reinfused into the patient after the intensive chemotherapy has been completed. Autologous stem cell transplantation aims to restore the patient’s blood cell production and shorten the recovery time following high-dose chemotherapy.
Radiation Therapy
Radiation therapy utilizes high-energy beams to target and kill cancer cells. It is often used in combination with other treatments in ALL, such as chemotherapy or stem cell transplantation. Radiation therapy is typically given locally to specific areas of the body that are affected by leukemia, such as the brain or lymph nodes. There are different types of radiation therapy used in ALL treatments, depending on the specific need.
Total body irradiation
Total body irradiation (TBI) involves the delivery of radiation to the entire body, including the bone marrow. It is commonly used as part of the conditioning regimen prior to allogeneic stem cell transplantation. TBI helps eliminate any remaining leukemia cells and suppresses the recipient’s immune system, allowing for successful engraftment of the donor stem cells.
Cranial irradiation
Cranial irradiation is a targeted radiation therapy where the beams are focused on the brain and spinal cord. It is primarily used to prevent or treat leukemia cells that have spread to the central nervous system. Cranial irradiation is often administered as prophylaxis in high-risk ALL patients to reduce the risk of CNS relapse.
Intrathecal radiation
Intrathecal radiation involves the administration of a radioactive substance directly into the cerebrospinal fluid through a lumbar puncture. This localized radiation therapy targets any leukemia cells present in the CNS and spinal fluid. Intrathecal radiation is typically given as part of CNS prophylaxis in combination with systemic chemotherapy.

Supportive Care
During the treatment of ALL, supportive care measures are essential to manage side effects, maintain overall well-being, and prevent complications. Supportive care interventions aim to alleviate symptoms, improve quality of life, and maximize the effectiveness of the primary treatments.
Blood transfusions
In the course of ALL treatment, patients may experience low levels of red blood cells (anemia) or platelets (thrombocytopenia). Transfusions of packed red blood cells or platelets can help restore adequate blood counts, reduce fatigue, and prevent bleeding-related complications.
Platelet transfusions
Low platelet counts can increase the risk of bleeding in patients with ALL. Platelet transfusions provide additional platelets to maintain a safe level and minimize bleeding complications.
Antibiotics
Infections pose a significant risk to ALL patients, particularly during intensive chemotherapy treatment. Antibiotics may be prescribed to prevent or treat bacterial infections, ensuring the patient’s immune system can recover and continue combating the leukemia cells effectively.
Antifungal medications
ALL treatment can weaken the immune system, making patients more susceptible to fungal infections. Antifungal medications, such as fluconazole or voriconazole, are often administered prophylactically or therapeutically to prevent or treat fungal infections.
Antiviral medications
To protect against viral infections, which can be particularly dangerous in individuals with weakened immune systems, antiviral medications may be used. These medications may be prescribed prophylactically or to treat active viral infections.
Management of side effects
Chemotherapy and radiation therapy can cause a range of side effects, including nausea, vomiting, hair loss, fatigue, and mucositis. Supportive care measures, such as anti-nausea medications, pain management strategies, and nutritional support, are employed to minimize these side effects and help patients tolerate and complete their treatment effectively.
Immunotherapy
Immunotherapy is a rapidly advancing field of cancer treatment that aims to enhance the body’s immune system to recognize and destroy cancer cells more effectively.
Blinatumomab
Blinatumomab is an immunotherapy medication approved for the treatment of relapsed or refractory ALL that expresses a specific protein called CD19. It works by connecting T cells to CD19-positive leukemia cells, stimulating the immune system to attack and eliminate the cancer cells.
Inotuzumab ozogamicin
Inotuzumab ozogamicin is an immunotherapeutic antibody-drug conjugate used in the treatment of relapsed or refractory ALL. It combines an antibody that targets CD22, a protein found in leukemia cells, with a cytotoxic agent that kills the cancer cells.
CAR T-cell therapy
As mentioned earlier, CAR T-cell therapy is a revolutionary form of immunotherapy. It involves modifying a patient’s own T cells to express a chimeric antigen receptor that can recognize and destroy cancer cells. CAR T-cell therapy has shown exceptional results in some patients with relapsed or refractory ALL.
Bispecific T-cell engager (BiTE) antibodies
BiTE antibodies are a type of immunotherapy that works by connecting T cells to cancer cells, enabling the T cells to recognize and eliminate the cancer cells. Blinatumomab mentioned earlier, is an example of a BiTE antibody used in the treatment of ALL.
Checkpoint inhibitors
Checkpoint inhibitors are a type of immunotherapy that blocks certain proteins in immune cells, allowing the immune system to better recognize and attack cancer cells. While they have shown promising results in other types of cancer, their use in ALL is currently being investigated in clinical trials.

Clinical Trials
Clinical trials are essential for advancing knowledge and developing new treatments for ALL. They allow researchers to evaluate the safety and effectiveness of innovative therapeutic approaches before they can be widely adopted as standard treatments.
New treatment approaches
Clinical trials often focus on novel treatment approaches, such as combining different chemotherapy drugs, targeted therapies, or immunotherapies. These trials aim to optimize treatment outcomes and identify more effective and less toxic therapies for patients with ALL.
Combination therapies
Combination therapies refer to the use of multiple drugs or treatment modalities together to achieve better treatment outcomes. Clinical trials often explore different combinations of chemotherapy, targeted agents, radiation therapy, or immunotherapies to determine their synergistic effects and potential for improved patient outcomes.
Transplant-Related Therapies
Transplant-related therapies are specific treatment approaches associated with stem cell transplantation in the context of ALL treatment.
Donor lymphocyte infusion
Donor lymphocyte infusion (DLI) involves infusing additional lymphocytes from the original donor into the patient after allogeneic stem cell transplantation. DLI is primarily used to treat or prevent a relapse of leukemia by boosting the graft-versus-leukemia (GVL) effect. The GVL effect occurs when the donor’s immune cells recognize and attack the leukemia cells in the recipient’s body.
Reduced-intensity conditioning (RIC) regimens
Reduced-intensity conditioning regimens are used in the context of allogeneic stem cell transplantation in patients who are older or may not tolerate intensive chemotherapy. These regimens involve lower doses of chemotherapy and sometimes radiation therapy to prepare the patient’s body for the stem cell transplant.
Post-transplant maintenance therapy
Following a stem cell transplant, post-transplant maintenance therapy may be administered to prevent relapse and promote long-term remission. This may involve the continuation of certain chemotherapy drugs or targeted therapies for a defined period to consolidate the treatment benefits of the transplant.

Prognosis and Risk Stratification
Prognosis and risk stratification help physicians estimate the likely course of the disease and tailor treatment decisions accordingly.
Risk factors
Numerous risk factors are considered in predicting the prognosis of ALL. These factors include age, white blood cell count at diagnosis, specific genetic abnormalities in leukemia cells, response to initial treatment, and the presence of minimal residual disease (MRD).
Minimal residual disease monitoring
Minimal residual disease refers to the small number of leukemia cells that may remain in the body after initial treatment. Monitoring MRD allows doctors to assess the effectiveness of treatment and predict the risk of relapse. Techniques such as flow cytometry, polymerase chain reaction (PCR), or next-generation sequencing are used to detect and quantify MRD.
Genetic testing
Genetic testing plays a vital role in risk stratification and treatment decision-making for ALL. It helps identify specific genetic abnormalities or mutations present in leukemia cells, which can guide treatment choices. Genetic testing is now routinely performed in clinical practice to identify high-risk subtypes of ALL and provide targeted therapies accordingly.
Emerging Therapies
The field of ALL research is continuously evolving, and scientists are exploring various emerging therapies to improve treatment outcomes.
Novel targeted agents
Researchers are actively investigating new targeted agents that can selectively attack leukemia cells while sparing normal cells. These agents could potentially improve response rates and reduce side effects compared to standard chemotherapy.
Immunotherapies
Immunotherapies, such as checkpoint inhibitors or novel CAR T-cell therapies, continue to be researched and refined for ALL treatments. These approaches exploit the power of the immune system to recognize and eliminate cancer cells more effectively.
Gene therapy
Gene therapy aims to modify a patient’s own cells to correct genetic abnormalities or enhance their anti-leukemia properties. This cutting-edge approach holds significant promise for ALL treatments and is being explored in clinical trials.
Epigenetic therapies
Epigenetic therapies focus on modifying the chemical modifications of DNA or proteins to regulate gene expression and control cancer cell growth. These therapies offer the potential for targeted and precise intervention against leukemia cells.
As research advances and new discoveries are made, the landscape of ALL treatments continues to evolve. Multimodal approaches and personalized treatment plans are becoming increasingly common, allowing for tailored therapies based on individual factors and risk stratification. Through ongoing research, innovation, and clinical trials, the prognosis for patients with ALL continues to improve, providing hope for better outcomes and ultimately a cure.
Watch This Video Below
Related Terms About Current Treatments for Acute Lymphoblastic Leukemia
Acute Lymphoblastic Leukemia Cure Rate, Acute Lymphoblastic Leukemia Treatment Guidelines, Acute Lymphoblastic Leukemia Treatment In India, Common Treatment Of Acute Lymphoblastic Leukemia, How Long Is Treatment For Acute Lymphoblastic Leukemia, New Treatments For Acute Lymphoblastic Leukemia