In the world of healthcare, the relationship between diabetes mellitus and aging is a topic of great significance. As you age, it’s crucial to understand how diabetes can impact your overall health and well-being. Diabetes mellitus, a chronic condition characterized by high blood sugar levels, poses unique challenges for older adults. This article aims to shed light on the complexities of diabetes mellitus in relation to the aging population, exploring the implications it can have on various aspects of life such as physical health, mental well-being, and quality of life. By understanding these connections, you’ll be equipped with valuable knowledge to navigate the world of diabetes mellitus as you age.
1. Introduction to Diabetes Mellitus and Aging
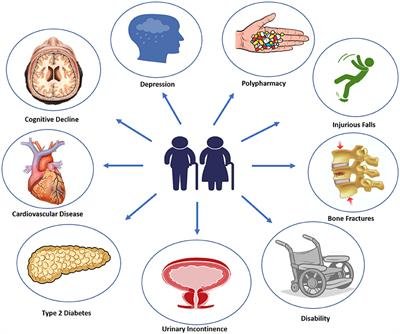
Diabetes Mellitus, commonly known as diabetes, is a chronic metabolic disorder characterized by high blood sugar levels. It occurs when the body either does not produce enough insulin or cannot effectively utilize the insulin it produces. This condition affects people of all ages, but its prevalence increases with age. In this article, we will explore the impact of aging on diabetes and the unique challenges faced by older adults diagnosed with this condition.
1.1 Definition of Diabetes Mellitus
Diabetes Mellitus is a condition in which the body fails to regulate blood sugar levels properly. It can be categorized into three main types: type 1 diabetes, type 2 diabetes, and gestational diabetes. Type 1 diabetes is an autoimmune disorder where the pancreas does not produce insulin. Type 2 diabetes is the most common form, characterized by insulin resistance and insufficient insulin production. Gestational diabetes occurs during pregnancy and usually resolves after childbirth.
1.2 Prevalence of Diabetes Mellitus in Older Adults
The prevalence of diabetes mellitus increases significantly with age. According to the World Health Organization (WHO), around 20% of people aged 65 years and older have diabetes. Older adults are more likely to develop type 2 diabetes due to factors such as physical inactivity, obesity, and age-related changes in metabolism. The high prevalence of diabetes in older adults poses challenges for healthcare systems and emphasizes the importance of addressing this issue effectively.
1.3 Aging Population and Diabetes
The global population is aging rapidly, with a growing number of older adults worldwide. This demographic shift has implications for diabetes management. Aging is associated with changes in insulin production and sensitivity, which can affect blood sugar control. Additionally, older adults often have multiple comorbidities, complicating the management of diabetes. Understanding the effects of aging on diabetes is crucial to tailor effective care for this population.
1.4 Purpose of the Article
The purpose of this article is to provide a comprehensive overview of the relationship between diabetes mellitus and aging. We will explore the effects of aging on diabetes, including changes in insulin production and glucose regulation. Furthermore, we will delve into the impact of diabetes on cognitive function and geriatric syndromes. The article will also discuss specific considerations for managing diabetes in older adults, strategies to improve diabetes management, and the importance of preventive care. Lastly, we will highlight the significance of psychosocial factors and conclude with recommendations for healthcare professionals to promote healthy aging in individuals with diabetes.
2. Effects of Aging on Diabetes Mellitus
Aging can have various effects on diabetes mellitus, ranging from changes in insulin production and sensitivity to an increased risk of comorbidities and complications. Understanding these effects is essential for providing optimal care for aging adults with diabetes.
2.1 Age-related Changes in Insulin Production and Sensitivity
As individuals age, their pancreatic beta cells may exhibit reduced insulin secretion and impaired response to glucose. This decline in insulin production can contribute to higher blood sugar levels in older adults. Additionally, aging is associated with decreased insulin sensitivity, further exacerbating glucose regulation difficulties. These age-related changes highlight the need for individualized treatment plans and monitoring of blood sugar control in older adults with diabetes.
2.2 Impact of Aging on Glucose Regulation
Aging also affects the body’s ability to regulate glucose levels. Older adults may experience delayed and blunted insulin responses following meals, leading to postprandial hyperglycemia. Furthermore, the liver’s capacity to regulate glucose production may be compromised in older individuals, leading to increased fasting blood sugar levels. These age-related changes in glucose regulation necessitate a careful balance of medication, diet, and physical activity to achieve optimal glycemic control.
2.3 Age-related Comorbidities and Diabetes Complications
Older adults with diabetes often have multiple comorbidities, such as cardiovascular disease, hypertension, and kidney disease. These conditions can complicate the management of diabetes and increase the risk of diabetes-related complications. For example, the combination of diabetes and hypertension significantly raises the risk of cardiovascular events. Knowledge of these comorbidities is crucial for healthcare providers to develop comprehensive care plans for aging individuals with diabetes.
2.4 Management Challenges in Aging Patients with Diabetes
Managing diabetes in older adults presents unique challenges. Polypharmacy, the use of multiple medications, is common among older individuals with diabetes due to the high prevalence of comorbidities. Balancing different medication schedules, potential drug interactions, and adherence can be complex. Additionally, lifestyle modifications, such as dietary changes and physical activity, may be more challenging to implement in older adults with mobility issues or cognitive impairments. Addressing these management challenges requires a multidisciplinary approach that considers the individual’s overall health and functional status.

3. Diabetes Mellitus and Cognitive Function in Older Adults
The relationship between diabetes mellitus and cognitive function in older adults has garnered significant attention in recent years. Research suggests that diabetes may contribute to an increased risk of cognitive decline, dementia, and Alzheimer’s disease in aging individuals.
3.1 Impact of Diabetes on Cognitive Decline
Studies have shown that older adults with diabetes are at a higher risk of cognitive decline compared to those without diabetes. Diabetes-related factors, such as hyperglycemia, insulin resistance, and chronic inflammation, may contribute to cognitive impairment. The exact mechanisms underlying this relationship are still being explored but are thought to involve vascular damage, oxidative stress, and brain insulin resistance.
3.2 Risk of Dementia and Alzheimer’s Disease
Diabetes has also been linked to an increased risk of dementia and Alzheimer’s disease in older adults. The presence of diabetes appears to accelerate the progression of cognitive decline and increase the likelihood of developing Alzheimer’s disease. Managing diabetes effectively in older adults may have potential benefits in preserving cognitive function and reducing the risk of dementia.
3.3 Mechanisms Underlying the Diabetes-Cognition Relationship
Several mechanisms have been proposed to explain the relationship between diabetes and cognitive function. Chronic hyperglycemia, insulin resistance, and the formation of advanced glycation end products (AGEs) can trigger oxidative stress and inflammation, leading to vascular damage and neural dysfunction. Additionally, the disruption of insulin signaling in the brain may impair synaptic function and contribute to cognitive impairment.
3.4 Implications for Managing Diabetes in Older Adults
Understanding the impact of diabetes on cognitive function highlights the importance of proactive management in older adults with diabetes. Optimal glycemic control, control of vascular risk factors, and lifestyle modifications, such as regular physical activity and a healthy diet, may help mitigate the risk of cognitive decline. Collaborative efforts between healthcare professionals, including endocrinologists, neurologists, and geriatric specialists, are essential in providing comprehensive care and addressing the unique needs of this population.
4. Geriatric Syndromes and Diabetes Mellitus
Older adults with diabetes may experience various geriatric syndromes, which are multifactorial conditions resulting from the interaction of age-related changes and underlying chronic medical conditions. These syndromes are common in aging populations and can complicate the management of diabetes.
4.1 Frailty and Diabetes
Frailty, characterized by decreased strength, endurance, and physiological function, is prevalent in older adults with diabetes. Frail individuals with diabetes have an increased risk of disability, hospitalization, and mortality. The presence of diabetes may contribute to accelerated muscle loss and impaired physical function, further exacerbating frailty. Careful management of diabetes and proactive measures to improve physical function are crucial to prevent or manage frailty in aging adults.
4.2 Polypharmacy and Medication Management Challenges
Older adults with diabetes often have complex medication regimens due to multiple comorbidities. Polypharmacy, the use of multiple medications, can increase the risk of adverse drug reactions, drug interactions, and non-adherence. This can complicate diabetes management and increase the risk of complications. Healthcare providers must regularly assess medication appropriateness, educate patients about their medications, and streamline medication regimens to ensure optimal management of diabetes and minimize medication-related risks.
4.3 Falls and Diabetes-Related Complications
Falls are a significant concern for older adults with diabetes. Peripheral neuropathy, a common complication of diabetes, can impair balance, proprioception, and gait, increasing the risk of falls. Additionally, hypoglycemia, a potential side effect of diabetes medications, can lead to dizziness or loss of consciousness, further increasing fall risk. Addressing falls prevention strategies, such as regular foot examinations, balance exercises, and medication adjustments, is essential in managing the complex care needs of older adults with diabetes.
4.4 Multimorbidity and Complex Care Needs
Older adults with diabetes often have multiple chronic conditions, requiring complex care management. The combination of diabetes with conditions such as hypertension, cardiovascular disease, and kidney disease necessitates a holistic approach to care. Healthcare providers must consider the interactions between these conditions and their respective treatment goals when developing individualized care plans. Collaborative care teams and effective communication among healthcare providers are vital to meet the complex care needs of this population effectively.
5. Specific Considerations for Older Adults with Diabetes
Managing diabetes in older adults requires specific considerations tailored to their unique needs and potential limitations. Addressing these considerations is crucial in optimizing their overall health and quality of life.
5.1 Tailoring Treatment Approaches for Aging Patients
When managing diabetes in older adults, healthcare providers should consider factors such as life expectancy, functional status, cognitive abilities, and individual goals of care. Treatment plans should be individualized, taking into account the potential risks and benefits of diabetes medications, as well as the impact of comorbidities on diabetes management.
5.2 Glycemic Control Goals and HbA1c Targets
Setting appropriate glycemic control goals for older adults with diabetes requires balancing the potential benefits of tight glycemic control against the risk of hypoglycemia. The American Diabetes Association (ADA) recommends a more relaxed glycemic control target, considering individual needs and health status. HbA1c targets may vary depending on factors such as life expectancy, comorbidities, and functional status.
5.3 Lifestyle Modifications in Older Adults with Diabetes
Encouraging lifestyle modifications is an essential aspect of diabetes management in older adults. Dietary changes, emphasizing a healthy and balanced diet, can help achieve glycemic control and manage comorbidities. Regular physical activity, tailored to individual capabilities, can improve insulin sensitivity, cardiovascular health, and overall well-being. Healthcare providers should provide education and support to older adults in adopting and maintaining healthy lifestyle habits.
5.4 Screening and Management of Diabetes Complications
Regular screening and management of diabetes complications are essential in older adults to prevent or minimize the impact of complications on their health. Eye examinations for diabetic retinopathy, foot examinations for peripheral neuropathy and ulcers, and screening for kidney disease are crucial components of diabetes care. Early detection and timely intervention can lead to better outcomes and improved quality of life for aging individuals with diabetes.
6. Geriatric Assessment and Diabetes Care
Comprehensive geriatric assessment plays a vital role in providing optimal diabetes care for older adults. It involves evaluating various aspects of an individual’s health and functional status to develop tailored care plans.
6.1 Importance of Comprehensive Geriatric Assessment
A comprehensive geriatric assessment assesses physical, cognitive, emotional, and social aspects of an older adult’s health. It provides a holistic understanding of their overall well-being, identifies potential areas of concern, and guides the development of personalized care plans. In the context of diabetes care, a geriatric assessment can help identify and address specific needs and challenges faced by older adults.
6.2 Functional Assessment and Diabetes Management
Functional assessment is an integral part of geriatric assessment in older adults with diabetes. It evaluates an individual’s ability to perform daily activities, such as self-care, mobility, and instrumental activities of daily living. Assessing functional status helps healthcare providers determine the level of assistance and support required for diabetes management tasks, such as medication administration, glucose monitoring, and meal preparation.
6.3 Nutritional Considerations and Meal Planning
Nutritional considerations are crucial in the management of diabetes in older adults. A comprehensive geriatric assessment can identify specific nutritional needs, dietary restrictions, and challenges faced by aging individuals. Healthcare providers can then develop individualized meal plans that promote glycemic control, address comorbidities, and accommodate unique dietary preferences or restrictions.
6.4 Physical Activity and Exercise Recommendations
Physical activity plays an essential role in maintaining optimal health and managing diabetes in older adults. A geriatric assessment can assess an individual’s physical capabilities, identify any limitations or impairments, and provide recommendations for safe and effective exercise programs. Incorporating physical activity into diabetes management can improve insulin sensitivity, cardiovascular health, and overall well-being in older adults.

7. Strategies to Improve Diabetes Management in Aging Adults
Improving diabetes management in aging adults requires a comprehensive approach that involves patient education, interdisciplinary teamwork, and the integration of technology. The following strategies can help optimize diabetes care in this population.
7.1 Patient Education and Self-Management Support
Patient education is vital in empowering older adults with diabetes to actively participate in their care. Providing clear and concise information about diabetes, its management, lifestyle modifications, and self-care practices is essential. Healthcare providers should also offer ongoing support and resources to enhance self-management skills and encourage adherence to treatment plans.
7.2 Team-Based Care and Interprofessional Collaboration
A team-based approach involving healthcare professionals from various disciplines is crucial in managing diabetes in aging adults effectively. Collaboration between endocrinologists, primary care physicians, nurses, dietitians, pharmacists, and other allied health professionals ensures comprehensive care that addresses various aspects of diabetes management. Interprofessional communication and care coordination are essential in minimizing gaps in care and providing holistic support to older adults with diabetes.
7.3 Integrating Technology in Diabetes Management
Technological advancements offer opportunities to improve diabetes management in aging adults. Continuous glucose monitors, insulin pumps, and mobile applications can assist in glycemic control and simplify self-monitoring tasks. Technology can also facilitate remote patient monitoring, telehealth visits, and real-time data sharing between healthcare providers and patients. Integrating technology into diabetes management can improve accessibility, enhance communication, and empower older adults to take an active role in their care.
7.4 Addressing Health Disparities in Older Adults
Health disparities can affect diabetes management outcomes in older adults, particularly among marginalized populations. Access to healthcare services, socioeconomic factors, cultural beliefs, and health literacy can all contribute to these disparities. Healthcare professionals must be aware of these factors and strive to provide equitable care by addressing barriers, tailoring interventions, and promoting health education initiatives that are accessible and culturally sensitive.
8. Preventive Care and Early Detection in Aging Diabetes Patients
Preventive care and early detection play crucial roles in managing diabetes in aging adults. Regular health screenings, immunizations, and targeted preventive strategies can help prevent complications and improve overall health outcomes.
8.1 Routine Health Screenings and Immunizations
Regular health screenings are essential in detecting potential complications and comorbidities in older adults with diabetes. Monitoring blood pressure, lipid levels, kidney function, and eye health can help identify early signs of complications and guide appropriate interventions. Additionally, staying up to date with immunizations, such as influenza and pneumonia vaccines, is crucial in preventing infectious diseases.
8.2 Age-Appropriate Diabetes Prevention Strategies
Preventing type 2 diabetes in aging adults involves adopting age-appropriate strategies that target modifiable risk factors. Encouraging regular physical activity, promoting healthy eating habits, and addressing obesity are key components of diabetes prevention. Lifestyle interventions that emphasize sustainable and realistic changes can significantly reduce the risk of developing diabetes in aging adults.
8.3 Managing Diabetes Complications in Older Adults
Early detection and management of diabetes-related complications are essential in preserving the health and well-being of aging adults. Regular screening for complications such as diabetic retinopathy, peripheral neuropathy, nephropathy, and cardiovascular disease can facilitate timely interventions and prevent further deterioration. Collaborative care teams and specialty referrals may be necessary to address specific complications effectively.
8.4 Importance of Regular Follow-up and Monitoring
Regular follow-up visits and ongoing monitoring of diabetes management are critical in aging adults. Regular blood glucose monitoring, HbA1c testing, and medication reviews are essential to assess the effectiveness of treatment plans and make necessary adjustments. Ongoing support, education, and reassessment of goals and preferences are key components of long-term diabetes care for older adults.

9. Psychosocial Factors and Diabetes in Older Adults
Psychosocial factors, including mental health, social support, and emotional well-being, play a significant role in diabetes management for aging adults. Addressing these factors is essential to promote optimal health outcomes and overall well-being.
9.1 Impact of Aging on Mental Health and Diabetes
Aging adults with diabetes are vulnerable to mental health challenges, including anxiety and depression. The chronic nature of diabetes, its associated complications, and the demands of self-management can contribute to psychological distress. Recognizing and addressing mental health concerns is crucial in providing comprehensive care and improving diabetes management outcomes.
9.2 Social Support and Diabetes Self-Care
Social support is vital for aging adults with diabetes to enhance their self-care practices and overall well-being. Family members, friends, and peers can provide emotional support, assist with medication management, encourage healthy lifestyle habits, and help navigate the healthcare system. Healthcare providers should assess an individual’s social support system and, if needed, connect them with community resources or support groups.
9.3 Addressing Anxiety and Depression in Older Adults
Anxiety and depression are common among older adults with diabetes and can negatively impact self-care behaviors and health outcomes. Healthcare providers should screen for anxiety and depression regularly and provide appropriate interventions, such as counseling, cognitive-behavioral therapy, or medication. Collaborative care involving mental health professionals can ensure a holistic approach to managing both diabetes and psychological well-being.
9.4 Strategies for Emotional Health and Well-being
Promoting emotional health and well-being is vital for aging adults with diabetes. Cultivating coping strategies, stress management techniques, and healthy lifestyle habits can positively impact overall mental and emotional well-being. Encouraging participation in support groups, engaging in meaningful activities, and fostering a sense of purpose and belonging are important strategies to enhance emotional health in older adults with diabetes.
10. Conclusion
Diabetes mellitus in aging adults presents unique challenges that necessitate a comprehensive and individualized approach to care. Understanding the effects of aging on diabetes and its impact on various aspects of health and well-being is crucial for healthcare professionals. By tailoring treatment approaches, addressing geriatric syndromes, incorporating a geriatric assessment, and promoting preventive care, healthcare professionals can optimize diabetes management and enhance the overall health and quality of life of aging adults with diabetes. The integration of technology, attention to psychosocial factors, and efforts to address health disparities are essential in providing equitable and comprehensive care to this population. By promoting healthy aging and providing effective diabetes management, healthcare professionals can make a significant impact on the lives of aging adults with diabetes.