Living with diabetes can have a significant impact on your overall health, including your dental health. Diabetes Mellitus, commonly known as diabetes, is a chronic condition that affects the body’s ability to regulate blood sugar levels. This article explores the connection between diabetes and dental health, highlighting the importance of regular dental care and providing helpful tips for maintaining optimal oral hygiene. Whether you have diabetes or know someone who does, understanding the potential effects on dental health is essential for a happy and healthy smile.
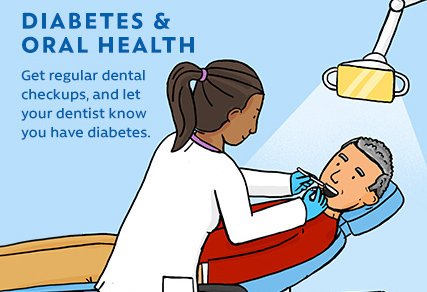
Dental Health Issues Associated with Diabetes Mellitus
Periodontal Disease
One of the most common dental health issues seen in individuals with diabetes mellitus is periodontal disease, also known as gum disease. The high blood sugar levels associated with diabetes can weaken the blood vessels and impair the body’s ability to fight infection, making individuals more susceptible to gum disease. Periodontal disease can cause inflammation, redness, swelling, and bleeding of the gums. If left untreated, it can lead to tooth loss and bone damage.
Dry Mouth
Another dental health issue commonly seen in individuals with diabetes is dry mouth, also known as xerostomia. High blood sugar levels can alter the salivary gland function, leading to decreased saliva production. Saliva plays a crucial role in maintaining oral health as it helps to clean the mouth, neutralize acids, and prevent tooth decay. When there is insufficient saliva, the mouth becomes dry, which can lead to discomfort, difficulty in speaking and swallowing, and an increased risk of developing dental cavities.
Thrush or Oral Candidiasis
Individuals with diabetes are more prone to developing oral thrush, which is an infection caused by the fungus candida. The elevated blood sugar levels provide an ideal environment for the overgrowth of candida in the mouth. Oral thrush can cause creamy white lesions on the tongue, inner cheeks, and roof of the mouth. It can result in discomfort, altered taste perception, and difficulty in swallowing.
Gum Infections
Diabetes can weaken the immune system, making the gums more susceptible to infections. Gum infections can cause pain, swelling, and tenderness in the gum tissue. If left untreated, they can progress to more severe conditions such as abscesses and periodontal disease. Regular dental check-ups are crucial for early detection and treatment of gum infections in individuals with diabetes.
Tooth Decay
High blood sugar levels in individuals with diabetes can increase the risk of tooth decay. The bacteria in the mouth feed on sugars and produce acids that can erode the tooth enamel, leading to cavities. Additionally, dry mouth and reduced saliva production associated with diabetes can further contribute to tooth decay. Maintaining good oral hygiene and controlling blood sugar levels are essential for preventing tooth decay in individuals with diabetes.
Delayed Healing
Diabetes can impair the body’s ability to heal and recover from injuries, including oral wounds. Dental procedures such as tooth extractions, oral surgeries, and implant placements may take a longer time to heal in individuals with diabetes. It is important for dental professionals to closely monitor and manage the healing process to prevent complications and ensure optimal outcomes.
Burning Mouth Syndrome
Burning mouth syndrome is a condition characterized by a burning sensation in the mouth, often accompanied by dry mouth, altered taste, and oral discomfort. While the exact cause of burning mouth syndrome is unknown, it has been observed to occur more frequently in individuals with diabetes. The symptoms can be chronic and significantly impact the quality of life. Close collaboration between dental and medical professionals is necessary for effective management of this condition.
Impact of Diabetes Mellitus on Dental Treatment
Management of Blood Glucose Levels
When providing dental treatment to individuals with diabetes mellitus, one of the key considerations is the management of blood glucose levels. Dental procedures and stress associated with dental visits can potentially affect blood sugar levels. It is important for individuals with diabetes to maintain stable blood sugar levels before, during, and after dental treatment. Dental professionals may need to coordinate with the patient’s medical team to ensure proper management of blood glucose levels during dental procedures.
Dental Complications
Individuals with diabetes mellitus may experience certain complications during dental treatment. This includes delayed wound healing, increased risk of infections, and impaired response to local anesthesia. Dental professionals should carefully evaluate the individual’s medical history, including their diabetes management, to minimize the risk of complications and provide appropriate treatment.
Effects on Anesthesia
Diabetes can affect the body’s response to anesthesia. Individuals with diabetes may require adjustments in the dosage or technique of administering anesthesia to achieve adequate pain control. Close communication between the dental and medical professionals is crucial to ensure the safety and comfort of individuals with diabetes during dental procedures.
Wound Healing Concerns
As mentioned earlier, individuals with diabetes may experience delayed wound healing. This can pose challenges in dental treatment that involves surgical procedures, such as tooth extractions or implant placements. Dental professionals should closely monitor the healing process, provide post-operative care instructions, and recommend appropriate measures to promote optimal wound healing.
Post-treatment Monitoring
After dental treatment, it is important to monitor individuals with diabetes mellitus closely for any signs of infection, delayed healing, or other complications. Dental professionals should educate patients on the signs and symptoms to watch out for and provide guidance on when to seek immediate dental or medical attention. Regular follow-up appointments are crucial to ensure the long-term success of dental treatment in individuals with diabetes.
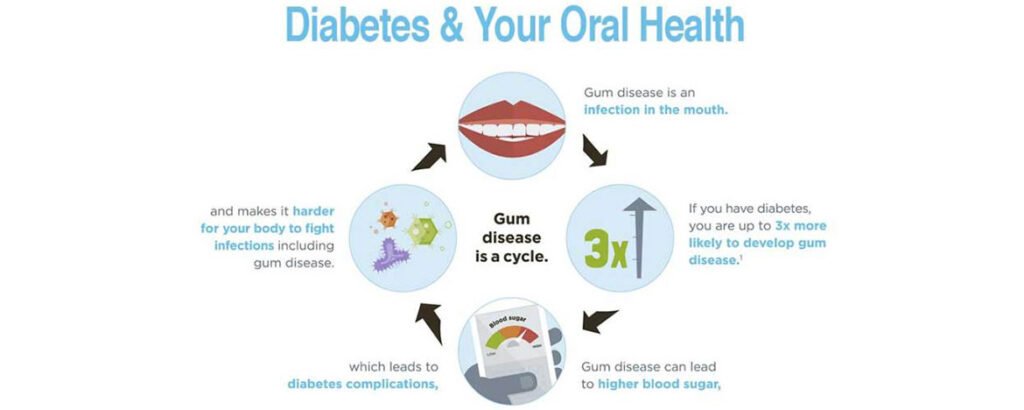
Preventing Dental Complications in Patients with Diabetes Mellitus
Regular Dental Visits
Regular dental visits are essential for preventing dental complications in individuals with diabetes mellitus. Dental professionals can assess the oral health status, detect early signs of dental problems, and provide appropriate interventions. It is generally recommended that individuals with diabetes visit the dentist at least twice a year, or as advised by their dental healthcare provider.
Maintaining Good Oral Hygiene
Maintaining good oral hygiene is crucial for individuals with diabetes to prevent dental complications. This includes brushing twice a day with fluoride toothpaste, flossing daily, and using mouthwash as recommended by the dental professional. Proper oral hygiene practices help to remove plaque, bacteria, and food debris from the mouth, reducing the risk of gum disease, tooth decay, and other oral health problems.
Diabetes-specific Dentistry
Diabetes-specific dentistry focuses on providing specialized oral care for individuals with diabetes mellitus. Dental professionals who are experienced in managing the oral health needs of individuals with diabetes can provide tailored treatment plans and preventive strategies to minimize the risk of dental complications. Seeking dental care from professionals with expertise in diabetes-specific dentistry is highly recommended for individuals with diabetes.
Controlling Blood Sugar Levels
Maintaining stable blood sugar levels is crucial for preventing dental complications in individuals with diabetes mellitus. Strict adherence to the prescribed diabetes management plan, including medication, diet, and exercise, can help to control blood sugar levels and reduce the risk of oral health problems. It is important for individuals with diabetes to work closely with their medical and dental healthcare providers to achieve and maintain optimal blood sugar control.
Dietary Considerations
Diet plays a significant role in oral health and diabetes management. Individuals with diabetes should follow a well-balanced diet that includes nutritious foods and limits the intake of sugary snacks and beverages. Dental professionals can provide guidance on diabetes-friendly diets and recommend specific dietary modifications to reduce the risk of dental complications.
Smoking Cessation
Smoking and tobacco use are detrimental to oral health, especially in individuals with diabetes. Smoking increases the risk of gum disease, tooth loss, oral cancer, and other oral health problems. Individuals with diabetes should be encouraged to quit smoking and seek support from healthcare professionals, including dental professionals, for smoking cessation interventions.
Stress Management
Stress can have a negative impact on diabetes management and oral health. High-stress levels can contribute to poor oral hygiene, increased sugar cravings, and difficulty in controlling blood sugar levels. Dental professionals can provide strategies for stress management, such as relaxation techniques and referrals to appropriate resources, to support individuals with diabetes in maintaining good oral health.
Collaboration between Dental and Medical Professionals
Importance of Communication
Effective communication between dental and medical professionals is crucial for providing comprehensive care to individuals with diabetes mellitus. Dental professionals should have open lines of communication with the patient’s medical team to exchange relevant information, discuss treatment plans, and coordinate care. Regular updates and collaboration between healthcare providers ensure that the patient’s overall health and dental needs are addressed effectively.
Risk Assessment and Treatment Planning
Collaboration between dental and medical professionals allows for a comprehensive risk assessment and treatment planning process for individuals with diabetes mellitus. By considering the patient’s medical history, diabetes management, and oral health status, a tailored treatment plan can be developed to minimize the risk of dental complications and ensure optimal outcomes.
Coordinated Care
Coordinated care involves collaborative efforts between dental and medical professionals to provide integrated and seamless care for individuals with diabetes. Dental professionals should be aware of the patient’s diabetes management plan, medications, and any relevant medical conditions to ensure that dental treatments are carried out safely and effectively. Regular communication and shared decision-making are essential components of coordinated care.
Interdisciplinary Approach
An interdisciplinary approach involving dental and medical professionals is beneficial for individuals with diabetes mellitus. This approach recognizes the interconnectedness of oral health and systemic health and aims to provide holistic care. By combining the expertise of multiple healthcare providers, individuals with diabetes can receive comprehensive treatment and support for their overall wellness.
Patient Education and Referrals
Dental professionals play a crucial role in educating individuals with diabetes about the impact of diabetes on oral health and the importance of preventive measures. They can provide guidance on oral hygiene practices, dietary considerations, and self-care strategies specific to individuals with diabetes. In cases where specialized medical care is required, dental professionals can refer individuals to appropriate healthcare providers to address their specific needs.
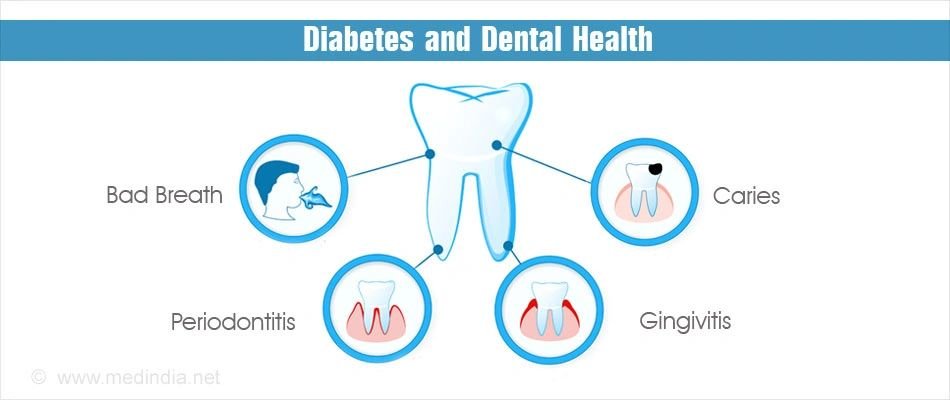
Key Considerations for Dental Professionals
Recognizing Signs of Diabetes
Dental professionals should be vigilant in recognizing the signs and symptoms of diabetes mellitus. Common oral signs of diabetes include dry mouth, frequent gum infections, and delayed wound healing. By being aware of these signs, dental professionals can initiate necessary conversations about diabetes with their patients and facilitate timely referrals for medical evaluation and treatment.
Communication with Patients
Open and effective communication with patients is crucial for dental professionals when providing care to individuals with diabetes. They should provide a safe and non-judgmental environment where patients feel comfortable discussing their diabetes management, oral health concerns, and any other related issues. Dental professionals should actively listen to their patients, address their questions and concerns, and provide appropriate guidance and support.
Risk Assessment and Medical History
Conducting a thorough risk assessment and evaluating the patient’s medical history is essential for dental professionals when treating individuals with diabetes mellitus. This includes understanding the patient’s diabetes management plan, medications, blood glucose control, and any medical conditions that may impact dental treatment. By considering these factors, dental professionals can develop individualized treatment plans and minimize the risk of complications.
Oral Manifestations
Understanding the oral manifestations associated with diabetes mellitus is important for dental professionals to provide appropriate care. They should be familiar with the signs and symptoms of gum disease, dry mouth, oral thrush, and other oral health conditions commonly seen in individuals with diabetes. Early detection and timely intervention can help prevent the progression of these conditions and maintain optimal oral health.
Assessment of Blood Glucose Control
Dental professionals should assess the patient’s blood glucose control before initiating dental treatment in individuals with diabetes. Uncontrolled blood sugar levels can increase the risk of complications during and after dental procedures. Dental professionals should collaborate with the patient’s medical team to ensure that blood glucose levels are well-managed before proceeding with dental treatment.
Collaborating with Medical Team
Collaboration with the patient’s medical team is essential for dental professionals when treating individuals with diabetes mellitus. They should maintain open lines of communication with the patient’s primary care physician, endocrinologist, or other healthcare providers involved in the management of diabetes. This collaboration allows for the exchange of important information, coordination of care, and shared decision-making to ensure comprehensive treatment for the patient.
Role of Dental Professionals in Diabetes Management
Screening for Diabetes
Dental professionals can play a vital role in screening for diabetes mellitus, especially in individuals who may be undiagnosed or at risk. By recognizing the signs and symptoms of diabetes, such as frequent gum infections, dry mouth, and delayed wound healing, dental professionals can initiate conversations about diabetes with their patients and recommend appropriate medical evaluation and follow-up.
Early Detection and Referrals
Early detection of diabetes in the dental setting can lead to timely interventions and improved health outcomes. Dental professionals should be vigilant in identifying individuals who may be at risk for diabetes based on their oral health status, medical history, and lifestyle factors. In such cases, dental professionals can refer patients to appropriate healthcare providers for further evaluation, diagnosis, and management of diabetes.
Educating Patients on Oral Health and Diabetes
Dental professionals have a crucial role in educating individuals with diabetes about the bidirectional relationship between oral health and diabetes. They can provide information on how diabetes can impact oral health and vice versa. Dental professionals can also educate patients on the importance of maintaining good oral hygiene, controlling blood sugar levels, and seeking regular dental and medical care to prevent dental complications and improve overall health.
Monitoring Oral Complications
Regular dental check-ups allow for the monitoring of oral complications in individuals with diabetes mellitus. Dental professionals can assess the oral health status, detect early signs of gum disease, tooth decay, oral infections, and other complications, and provide appropriate interventions. By closely monitoring oral health, dental professionals can prevent the progression of dental problems and ensure timely treatment.
Routine Dental Treatments
Dental professionals are responsible for providing routine dental treatments to individuals with diabetes mellitus. This includes professional cleanings, examinations, and preventive interventions such as fluoride treatments and dental sealants. Routine dental treatments help to maintain good oral health, prevent dental complications, and contribute to the overall well-being of individuals with diabetes.
Collaboration with Diabetes Specialists
Collaboration between dental professionals and diabetes specialists is beneficial for individuals with diabetes mellitus. Dental professionals can work closely with endocrinologists, diabetes educators, and other healthcare providers to develop comprehensive care plans that address both the oral health and systemic health needs of the patient. This collaborative approach ensures that individuals with diabetes receive the best possible care and support.

Dental Treatments for Patients with Diabetes Mellitus
Routine Cleanings and Examinations
Routine cleanings and examinations are essential for individuals with diabetes mellitus to maintain good oral health. Dental professionals can thoroughly clean the teeth, remove plaque, and assess the oral health status. Regular check-ups allow for early detection of dental problems, such as gum disease or tooth decay, and prompt intervention.
Scaling and Root Planing
Scaling and root planing, also known as deep cleaning, may be necessary for individuals with diabetes who have periodontal disease. This non-surgical procedure involves removing plaque and tartar from below the gumline and smoothing the tooth roots to promote gum tissue reattachment. Scaling and root planing can help control gum disease and prevent further damage to the gums and supporting structures.
Antibiotics and Antifungal Medications
In cases where individuals with diabetes develop oral infections such as gum abscesses or oral thrush, dental professionals may prescribe antibiotics or antifungal medications. These medications help to eliminate the bacteria or fungi causing the infection and promote healing. It is important for individuals with diabetes to adhere to the prescribed medication regimen and complete the full course of treatment.
Prescribing Pain Medications
Individuals with diabetes may require pain medications after dental procedures, such as tooth extractions or oral surgeries. Dental professionals can prescribe appropriate pain medications to manage post-operative pain and ensure the patient’s comfort. However, it is important to consider the individual’s medical history, allergies, and potential drug interactions when prescribing pain medications.
Tooth Extraction and Dental Surgery
Tooth extraction and dental surgery may be necessary for individuals with diabetes mellitus who have severely damaged or infected teeth. Dental professionals should carefully evaluate the patient’s overall health, blood glucose control, and risk of complications before proceeding with tooth extraction or dental surgery. Close monitoring and follow-up care are essential to ensure proper healing and prevent complications.
Dental Implants and Prosthetics
Individuals with diabetes mellitus who have missing teeth may benefit from dental implants or other prosthetic solutions. Dental professionals should assess the patient’s overall health, blood sugar control, and bone density before recommending dental implants. Collaboration between dental and medical professionals is crucial to ensure that the patient is a suitable candidate for implants and to coordinate care throughout the treatment process.
Special Considerations for Children and Adolescents with Diabetes
Preventive Care
Preventive care plays a vital role in maintaining the oral health of children and adolescents with diabetes. Dental professionals should work closely with parents and caregivers to establish good oral hygiene habits, including regular brushing, flossing, and the use of fluoride products. Early intervention and preventive measures, such as dental sealants and fluoride treatments, can help to prevent dental complications in this vulnerable population.
Early Intervention and Monitoring
Dental professionals should prioritize early intervention and close monitoring of oral health in children and adolescents with diabetes. Regular dental check-ups allow for the detection of dental problems at an early stage, enabling timely intervention and appropriate treatment. Dental professionals can provide education and support to empower young patients with diabetes to take charge of their oral health.
Orthodontic Treatment
Orthodontic treatment may be necessary for children and adolescents with diabetes who require correction of misaligned teeth or bite issues. Dental professionals should carefully evaluate the patient’s overall health, blood sugar control, and dental condition before recommending orthodontic treatment. Close collaboration between the orthodontist and the patient’s diabetes healthcare team is essential to ensure safe and effective treatment.
Dietary Recommendations
Diet plays a crucial role in diabetes management and oral health. Dental professionals should provide specific dietary recommendations for children and adolescents with diabetes, taking into consideration their nutritional needs and their oral health. Encouraging a well-balanced diet, limiting sugary snacks and beverages, and promoting regular meal patterns can help to maintain stable blood sugar levels and minimize the risk of dental complications.
Patient and Parent Education
Patient and parent education is key in supporting the oral health of children and adolescents with diabetes. Dental professionals should provide age-appropriate education and guidance on maintaining good oral hygiene, controlling blood sugar levels, and seeking regular dental check-ups. They should also address any concerns or questions raised by parents or young patients and provide resources for additional support.

Supporting Oral Health in Older Adults with Diabetes
Oral Hygiene and Denture Care
Maintaining good oral hygiene and proper denture care is crucial for older adults with diabetes mellitus. Dental professionals should provide guidance on effective oral hygiene practices, including brushing, flossing, and cleaning dentures. Regular dental check-ups allow for the assessment of oral health status, early detection of dental problems, and appropriate interventions to maintain oral health in older adults with diabetes.
Dry Mouth Management
Dry mouth is a common concern among older adults with diabetes. Dental professionals should provide guidance on managing dry mouth, such as drinking plenty of water, using saliva substitutes, and avoiding alcohol-based mouthwashes. They can also recommend sugar-free chewing gum or lozenges to stimulate saliva production. Close monitoring of oral health and regular dental visits are important for individuals with dry mouth to prevent dental complications.
Root Caries Prevention
Older adults with diabetes mellitus may be at a higher risk of root caries, which are cavities that develop on the tooth roots. Dental professionals should emphasize the importance of maintaining good oral hygiene, limiting sugary snacks and beverages, and using fluoride products to prevent root caries. Regular dental check-ups allow for the early detection and treatment of root caries, ensuring optimal oral health in older adults with diabetes.
Regular Oral Cancer Screenings
Older adults with diabetes should undergo regular oral cancer screenings as part of their dental check-ups. Dental professionals can perform a thorough examination of the oral tissues, including the lips, tongue, cheeks, and throat, to detect any abnormalities or signs of oral cancer. Early detection of oral cancer can lead to timely interventions and improve the chances of successful treatment.
Research and Advances in Diabetes Mellitus and Dental Health
Oral Health Biomarkers
Research is being conducted to identify oral health biomarkers that may help in the early detection and monitoring of diabetes mellitus. These biomarkers may include specific proteins or genetic markers that can be detected in saliva, dental plaque, or other oral fluids. The development of reliable oral health biomarkers has the potential to revolutionize diabetes management and improve oral health outcomes.
Impact of Dental Infections on Diabetes Control
Researchers are exploring the bidirectional relationship between dental infections and diabetes control. Studies have suggested that severe gum disease can negatively impact blood sugar control in individuals with diabetes, potentially leading to complications. Understanding the impact of dental infections on diabetes management can help dental and medical professionals develop more effective preventive strategies and treatment approaches.
Novel Dental Treatment Approaches
Advances in dental research and technology have resulted in the development of novel treatment approaches for individuals with diabetes mellitus. This includes the use of laser therapy for periodontal treatment, innovative restorative materials, and minimally invasive procedures. These advancements aim to improve treatment outcomes, minimize discomfort, and reduce the risk of complications in individuals with diabetes.
Diabetes-specific Oral Care Products
Companies are developing oral care products specifically designed for individuals with diabetes mellitus. These products may include toothpaste, mouthwash, and dental floss that are tailored to the unique oral health needs of individuals with diabetes. Diabetes-specific oral care products aim to provide additional benefits, such as enhanced gum health and improved blood sugar control, to support overall oral health in individuals with diabetes.