If you’ve been experiencing persistent digestive issues and are seeking answers, this article is for you. “Diagnosing Celiac Disease” explores the key aspects of identifying this common autoimmune disorder, focusing on the importance of an accurate diagnosis. From explaining the symptoms to shedding light on the diagnostic process, this comprehensive article will give you an insight into Celiac Disease, helping you on your journey towards improved health and well-being. So, if you’re ready to better understand the intricacies of this condition and how it can be diagnosed, let’s begin!

Symptoms and Signs of Celiac Disease
Common Symptoms of Celiac Disease
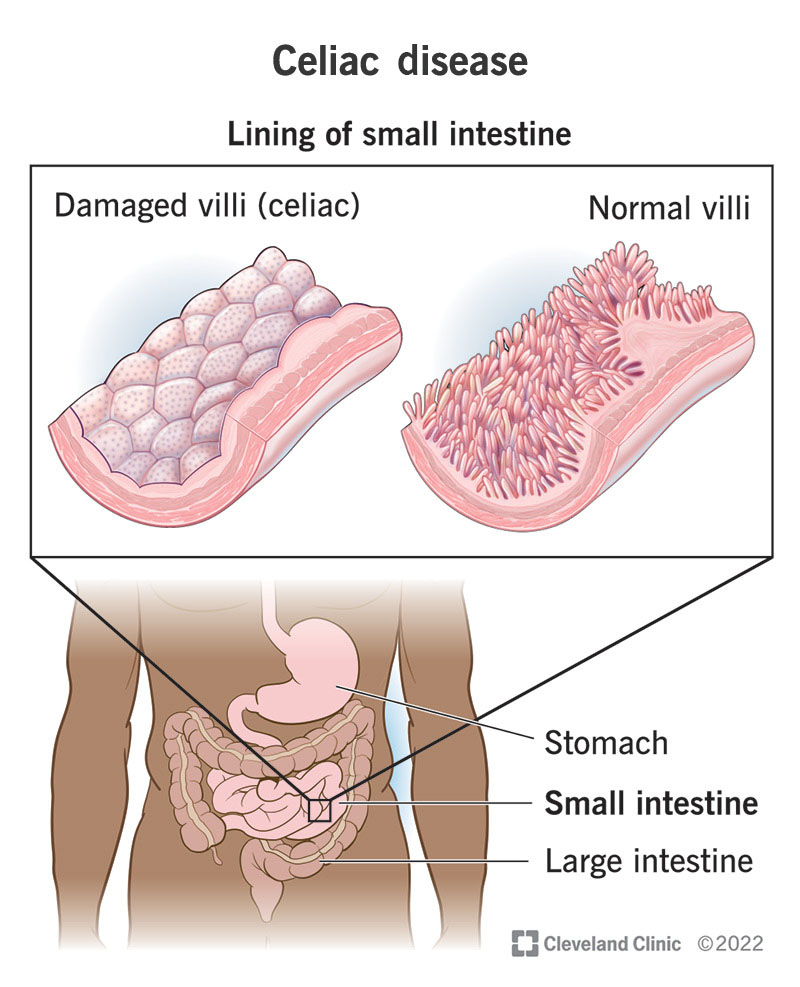
Celiac disease is a condition that affects the small intestine and is triggered by the consumption of gluten, a protein found in wheat, barley, and rye. The most common symptoms of celiac disease include:
-
Digestive Issues: Abdominal pain, bloating, diarrhea, constipation, and vomiting are frequently experienced by individuals with celiac disease. These symptoms are a result of the body’s inability to properly absorb nutrients.
-
Weight Loss: Unintentional weight loss is often seen in individuals with undiagnosed celiac disease. This occurs because the body is unable to absorb essential nutrients from food.
-
Fatigue: Chronic fatigue and a lack of energy are common symptoms of celiac disease. The body’s inability to properly absorb nutrients can lead to a deficiency in iron and other essential vitamins and minerals, causing fatigue.
-
Skin Rash: Some individuals with celiac disease may develop a skin rash called dermatitis herpetiformis. This rash is characterized by itchy, blistering, and burning skin lesions.
Less Common Symptoms of Celiac Disease
While the symptoms mentioned above are more commonly associated with celiac disease, there are also several less common symptoms that individuals may experience, including:
-
Joint Pain: Some individuals with celiac disease may experience joint pain and swelling, similar to symptoms of rheumatoid arthritis.
-
Anemia: Celiac disease can lead to anemia, which occurs when the body lacks enough healthy red blood cells to carry an adequate oxygen supply to tissues. This can result in fatigue, weakness, and shortness of breath.
-
Headaches: Recurrent headaches and migraines can be a symptom of celiac disease.
-
Behavioral Changes: Irritability, depression, anxiety, and ADHD-like symptoms have been reported in some individuals with undiagnosed celiac disease.
Atypical Symptoms of Celiac Disease
Celiac disease can present itself in various ways, and some individuals may experience atypical symptoms that are not commonly associated with the condition. These atypical symptoms may include:
-
Dental Issues: Celiac disease can lead to enamel defects and tooth discoloration, as well as an increased risk of cavities.
-
Delayed Puberty: In some cases, undiagnosed celiac disease can delay the onset of puberty in adolescents.
-
Short Stature: Children with celiac disease may have difficulty reaching their expected height due to nutrient malabsorption.
Signs of Celiac Disease
While symptoms can vary from person to person, there are certain signs that healthcare professionals look for when suspecting celiac disease:
-
Villous Atrophy: Damage to the lining of the small intestine, known as villous atrophy, is a key sign of celiac disease. This can be observed through an endoscopy and biopsy.
-
Positive Antibody Tests: Blood tests that indicate the presence of specific antibodies, such as tissue transglutaminase antibodies and endomysial antibodies, are commonly used to aid in the diagnosis of celiac disease.
Risk Factors and Prevalence
Genetic Factors
Celiac disease has a strong genetic component, and certain gene variants are associated with an increased risk of developing the condition. The most significant genetic factor is the presence of the human leukocyte antigen (HLA) genes HLA-DQ2 and HLA-DQ8. However, it is important to note that not all individuals with these genes will develop celiac disease, and not all individuals with celiac disease have these genes.
Family History
Having a first-degree relative, such as a parent or sibling, with celiac disease increases an individual’s risk of developing the condition. In fact, the risk is approximately ten times higher for individuals with a family history of celiac disease compared to those without.
Age
Celiac disease can develop at any age, from infancy to adulthood. There is an increased risk for individuals who were introduced to gluten during infancy and those who experienced viral or bacterial infections during childhood.
Gender
Celiac disease can affect individuals of any gender, but studies have shown that women are more frequently diagnosed than men. The reason for this gender difference is not yet fully understood.
Other Autoimmune Conditions
There is a strong link between celiac disease and other autoimmune conditions, such as type 1 diabetes, autoimmune thyroid disease, and autoimmune liver diseases. Individuals with these conditions have a higher risk of also developing celiac disease.
Prevalence of Celiac Disease
Celiac disease is relatively common, although many cases go undiagnosed. It is estimated that approximately 1 in 100 people worldwide have celiac disease. However, the prevalence varies among populations and geographic regions.

Diagnostic Tests for Celiac Disease
Blood Tests
Blood tests play a crucial role in the diagnosis of celiac disease. They measure specific antibodies that are typically present in individuals with the condition. The commonly used blood tests for celiac disease include:
-
Tissue Transglutaminase (tTG) Antibodies: This test measures the levels of antibodies that target tissue transglutaminase, an enzyme involved in the immune response to gluten.
-
Endomysial Antibodies (EMA): EMA testing detects the presence of antibodies that react with endomysium, a layer of connective tissue in the intestine that can be damaged by the immune system in celiac disease.
-
Deamidated Gliadin Peptides (DGP): This test measures the levels of antibodies against deamidated gliadin peptides, which are fragments of gluten that have been modified by an enzyme.
-
Total Serum IgA: Since celiac disease is associated with IgA deficiency, a total serum IgA test is often performed to determine if the individual has sufficient levels of this immunoglobulin.
Endoscopy and Biopsy
An upper endoscopy with a biopsy is considered the gold standard for diagnosing celiac disease. During this procedure, a flexible tube with a camera on the end is inserted through the mouth and into the small intestine to visually inspect the lining. Multiple tissue samples (biopsy) are taken from the small intestine to evaluate for characteristic changes associated with celiac disease.
Genetic Testing
Genetic testing for HLA-DQ2 and HLA-DQ8 genes can help determine an individual’s genetic susceptibility to celiac disease. However, genetic testing alone cannot diagnose celiac disease, as the presence of these genes is not exclusive to the condition.
Elimination Diet
In some cases, an elimination diet may be used as a diagnostic tool. This involves removing all sources of gluten from the diet and monitoring symptoms for improvement. If symptoms resolve on a gluten-free diet and return upon reintroduction of gluten, it may suggest celiac disease.
Serologic Testing
In certain instances where initial blood tests are inconclusive, additional serologic testing may be performed to detect specific antibodies associated with celiac disease. These tests can provide further confirmation or assist in ruling out other potential causes.
Blood Tests for Celiac Disease
Tissue Transglutaminase (tTG) Antibodies
The tissue transglutaminase antibody test measures the levels of antibodies that target tissue transglutaminase, an enzyme involved in the immune response to gluten. Elevated levels of tTG antibodies are indicative of the autoimmune response in celiac disease.
Endomysial Antibodies (EMA)
EMA testing involves detecting the presence of antibodies that react with endomysium, a layer of connective tissue in the intestine that can be damaged by the immune system in celiac disease. The presence of EMA antibodies suggests the presence of celiac disease.
Deamidated Gliadin Peptides (DGP)
The deamidated gliadin peptide antibody test measures the levels of antibodies against deamidated gliadin peptides, which are fragments of gluten that have been modified by an enzyme. Elevated levels of DGP antibodies are associated with celiac disease.
Total Serum IgA
Total serum IgA testing is performed to determine if an individual has sufficient levels of immunoglobulin A. Celiac disease is associated with IgA deficiency, so testing IgA levels helps ensure accurate results for other celiac disease blood tests that rely on IgA antibodies.
Endoscopy and Biopsy
Upper Endoscopy
During an upper endoscopy, a flexible tube with a small camera is inserted through the mouth and down the esophagus to the small intestine. This allows the doctor to visually inspect the lining of the small intestine for any abnormalities, such as villous atrophy, which is a characteristic feature of celiac disease.
Biopsy Procedure
Multiple tissue samples, or biopsies, are taken during an endoscopy. These samples are collected from different parts of the small intestine and are later examined under a microscope. The presence of villous atrophy, along with other histological changes, confirms the diagnosis of celiac disease.
Marsh Classification System
The Marsh classification system is used to evaluate the severity of intestinal damage observed in the biopsy samples. It consists of several stages, with Stage 3 being the most severe. The classification can help determine the extent of damage caused by celiac disease and guide treatment decisions.
Genetic Testing
Human Leukocyte Antigen (HLA) Typing
Genetic testing for celiac disease involves HLA typing, which determines an individual’s genetic susceptibility to the condition. HLA genes encode proteins that play a role in the immune response. The presence of certain HLA gene variants, specifically HLA-DQ2 and HLA-DQ8, is associated with an increased risk of developing celiac disease.
HLA-DQ2 and HLA-DQ8 Genes
The HLA-DQ2 and HLA-DQ8 genes are the most significant genetic risk factors for celiac disease. The majority of individuals with celiac disease carry either one or both of these gene variants. However, it is important to note that not all individuals with these genes will develop celiac disease.
Limitations of Genetic Testing
Genetic testing for celiac disease has certain limitations. While the presence of HLA-DQ2 or HLA-DQ8 gene variants increases the risk of developing the condition, it does not provide a definitive diagnosis. Additionally, these gene variants are found in a significant portion of the population who do not have celiac disease.

Elimination Diet as a Diagnostic Tool
Steps in an Elimination Diet
An elimination diet involves completely removing all sources of gluten from the diet for a specified period of time, typically several weeks to a few months. This allows the body to heal and for symptoms to subside.
Gluten Challenge
After the elimination period, a gluten challenge is introduced, where gluten is gradually reintroduced into the diet. Monitoring symptoms during this phase can help determine if there is a gluten intolerance or sensitivity, or if celiac disease is the underlying cause.
Advantages and Disadvantages
The elimination diet can be a useful diagnostic tool, especially in cases where blood tests and biopsy results are inconclusive. However, it requires strict adherence to a gluten-free diet, which can be challenging for some individuals. Additionally, the elimination diet may not be suitable for everyone, particularly those experiencing severe symptoms or complications related to celiac disease.
Complications of Undiagnosed Celiac Disease
Malabsorption and Nutritional Deficiencies
One of the primary complications of undiagnosed or untreated celiac disease is malabsorption, which can lead to various nutritional deficiencies. Without proper absorption of nutrients, the body may lack essential vitamins (such as vitamin D, vitamin B12, and folate), minerals (such as iron and calcium), and other important components.
Osteoporosis and Bone Health Issues
Long-term untreated celiac disease can lead to reduced bone density and an increased risk of osteoporosis and fractures. Malabsorption of calcium and vitamin D, combined with chronic inflammation, can negatively affect bone health.
Infertility and Reproductive Problems
Undiagnosed celiac disease has been associated with infertility and reproductive issues in both men and women. In women, untreated celiac disease may disrupt hormonal balance and lead to irregular menstrual cycles, early menopause, and difficulty conceiving. In men, celiac disease can affect sperm quality and fertility.
Dermatitis Herpetiformis
Dermatitis herpetiformis is a chronic skin condition characterized by itchy, blistering skin lesions. It is closely linked to celiac disease and occurs due to an autoimmune reaction to gluten. The presence of dermatitis herpetiformis may indicate undiagnosed celiac disease.
Neurological Manifestations
Celiac disease can affect the nervous system and lead to various neurological symptoms. These may include headaches, migraines, peripheral neuropathy (numbness and tingling in the hands and feet), ataxia (lack of muscle coordination), and seizures.
Increased Risk of Cancer
Undiagnosed celiac disease has been associated with an increased risk of certain types of cancer, particularly intestinal lymphomas and small bowel adenocarcinomas. Timely diagnosis and adherence to a gluten-free diet can reduce the risk of these complications.

Differential Diagnoses of Celiac Disease
Irritable Bowel Syndrome (IBS)
Celiac disease shares some symptoms with irritable bowel syndrome (IBS), such as abdominal pain, bloating, and changes in bowel movements. However, unlike celiac disease, IBS is not an autoimmune disorder and does not involve an immune response to gluten.
Inflammatory Bowel Disease (IBD)
Inflammatory bowel disease (IBD), including Crohn’s disease and ulcerative colitis, can cause similar gastrointestinal symptoms as celiac disease. It is important to differentiate between these conditions to ensure appropriate treatment.
Food Intolerances
Food intolerances, such as lactose or fructose intolerance, can cause digestive symptoms similar to celiac disease. However, these conditions do not involve an immune response and can often be managed by avoiding specific trigger foods.
Gastroenteritis
Gastroenteritis, commonly known as the stomach flu, can result in temporary digestive symptoms resembling celiac disease. However, the symptoms typically resolve within a few days or weeks, unlike the chronic nature of celiac disease.
Pancreatic Insufficiency
Pancreatic insufficiency, often associated with conditions like chronic pancreatitis or cystic fibrosis, can hinder the digestion and absorption of nutrients. This can lead to symptoms similar to those seen in celiac disease, making it important to consider this differential diagnosis.
The Importance of Early Diagnosis
Preventing Long-term Complications
Early diagnosis of celiac disease is crucial in preventing long-term complications. Timely initiation of a gluten-free diet can help heal the intestinal lining, reduce inflammation, and restore nutrient absorption. This can prevent or minimize the risk of complications such as malabsorption, osteoporosis, reproductive problems, and certain types of cancer.
Improving Quality of Life
Celiac disease can significantly impact an individual’s quality of life. The physical symptoms, dietary restrictions, and potential social challenges associated with the condition can lead to reduced overall well-being. Early diagnosis and appropriate management can help individuals lead a fulfilling and active life while adhering to a gluten-free diet.
Avoiding Unnecessary Medical Interventions
Without a proper diagnosis, individuals with undiagnosed celiac disease may undergo unnecessary medical interventions and treatments for symptoms that are actually caused by their gluten intolerance. Prompt diagnosis can prevent unnecessary testing, procedures, and medications, leading to more appropriate and effective healthcare.
In conclusion, recognizing the symptoms and signs of celiac disease is essential for early diagnosis and appropriate management. Understanding the risk factors, diagnostic tests, and potential complications associated with the condition can help individuals and healthcare professionals identify and address celiac disease promptly. By embracing a gluten-free lifestyle and seeking proper medical care, individuals with celiac disease can improve their overall health and well-being.