In this article, we will explore the topic of Hyperkalemia, a condition characterized by high levels of potassium in the blood. Hyperkalemia can be a serious health concern and understanding the effective treatments available is crucial. From dietary modifications to medications and medical procedures, this article will provide you with valuable information on various treatment options for managing Hyperkalemia and helping you maintain a healthy balance of potassium in your body.
Overview of Hyperkalemia
Hyperkalemia is a medical condition characterized by elevated levels of potassium in the bloodstream. Potassium is an essential mineral that plays a vital role in maintaining the balance of fluids and electrolytes in the body, as well as aiding in nerve and muscle function. However, when potassium levels become too high, it can lead to serious health complications. Hyperkalemia can be caused by various factors, including certain medical conditions, medications, and dietary choices. It is important to understand the causes, symptoms, diagnosis, and management strategies for hyperkalemia in order to effectively treat and prevent this condition.
What is Hyperkalemia?
Hyperkalemia is a condition characterized by high levels of potassium in the blood. A normal potassium level typically falls between 3.5 to 5.0 milliequivalents per liter (mEq/L). When levels exceed 5.5 mEq/L, it is considered hyperkalemia. This condition can affect individuals of all ages and can be mild, moderate, or severe, depending on the extent of potassium elevation. Hyperkalemia can have serious consequences, as high potassium levels can disrupt the electrical signals that regulate heart function, leading to abnormal heart rhythms and potentially life-threatening complications.
Causes of Hyperkalemia
Hyperkalemia can be caused by a variety of factors. Certain medical conditions, such as chronic kidney disease, diabetes, adrenal insufficiency, and metabolic acidosis, can increase the risk of developing hyperkalemia. Additionally, medications like potassium-sparing diuretics, ACE inhibitors, and angiotensin receptor blockers (ARBs) can also contribute to elevated potassium levels. Other causes include excessive potassium intake through diet or supplementation, as well as acute kidney injury and tissue trauma.
Symptoms of Hyperkalemia
The symptoms of hyperkalemia can vary depending on the severity of the condition and the individual’s overall health. Mild cases of hyperkalemia may not present any symptoms and are often discovered incidentally during routine blood tests. However, as potassium levels rise, symptoms may include muscle weakness, fatigue, palpitations, irregular heartbeat, numbness or tingling, nausea and vomiting, and difficulty breathing. In severe cases, hyperkalemia can lead to paralysis and cardiac arrest, requiring immediate medical attention.
Diagnosis and Monitoring
Diagnostic Tests for Hyperkalemia
To diagnose hyperkalemia, healthcare providers will typically order a blood test to measure the levels of potassium in the bloodstream. This test, known as a serum potassium test, is a simple and routine procedure. In addition to measuring potassium levels, other blood tests may be ordered to assess kidney function and identify any underlying causes of hyperkalemia. These tests may include blood urea nitrogen (BUN) and creatinine tests, as well as tests to evaluate acid-base balance and hormone levels.
Monitoring Hyperkalemia
Once hyperkalemia has been diagnosed, ongoing monitoring is essential to ensure proper management and prevent complications. Regular blood tests will be conducted to monitor potassium levels and assess the effectiveness of treatment interventions. The frequency of monitoring will depend on the severity of hyperkalemia and any underlying medical conditions. In some cases, patients may need more frequent monitoring, particularly if they have chronic kidney disease or are taking medications that can affect potassium levels.

Emergency Management
Immediate Measures to Stabilize Potassium Levels
When hyperkalemia reaches critical levels or when patients present with severe symptoms, immediate measures must be taken to stabilize potassium levels. The first step is to discontinue any medications that may be contributing to high potassium levels. In cases where there is a potential for life-threatening complications, emergency treatments such as administering calcium gluconate or calcium chloride may be necessary to protect the heart from the effects of hyperkalemia. Additionally, temporary measures such as using a dialysis machine or applying a rapid-acting beta-2 agonist may be employed to lower potassium levels rapidly.
Acute Treatment Options
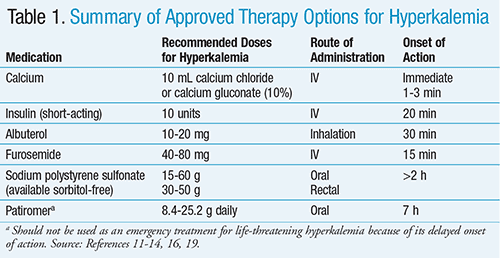
Acute treatment options for hyperkalemia focus on quickly lowering potassium levels while addressing the underlying causes. One common strategy is the administration of medications that help shift potassium from the bloodstream into the cells, such as sodium bicarbonate or insulin combined with glucose. These medications promote the movement of potassium from the blood into the cells, reducing the overall concentration in the bloodstream. Loop diuretics, such as furosemide, may also be used to increase potassium excretion through urine. In severe cases, alternative therapies, such as sodium polystyrene sulfonate (Kayexalate), may be considered to bind excess potassium in the intestines and facilitate its elimination from the body.
Pharmacological Treatments
Calcium Gluconate and Calcium Chloride
Calcium gluconate and calcium chloride are medications commonly used in the emergency management of hyperkalemia. These medications work by stabilizing the electrical conduction within the heart, protecting it from the adverse effects of elevated potassium levels. They are typically administered intravenously and are most effective in treating acute hyperkalemia or preventing complications while other treatment interventions take effect.
Sodium Bicarbonate
Sodium bicarbonate is another medication that can be used to treat hyperkalemia. It works by increasing the pH of the blood, which in turn helps to shift potassium from the bloodstream into the cells. This effect is especially useful in cases where hyperkalemia is accompanied by metabolic acidosis. Sodium bicarbonate is typically administered intravenously and is often used in combination with insulin and glucose.
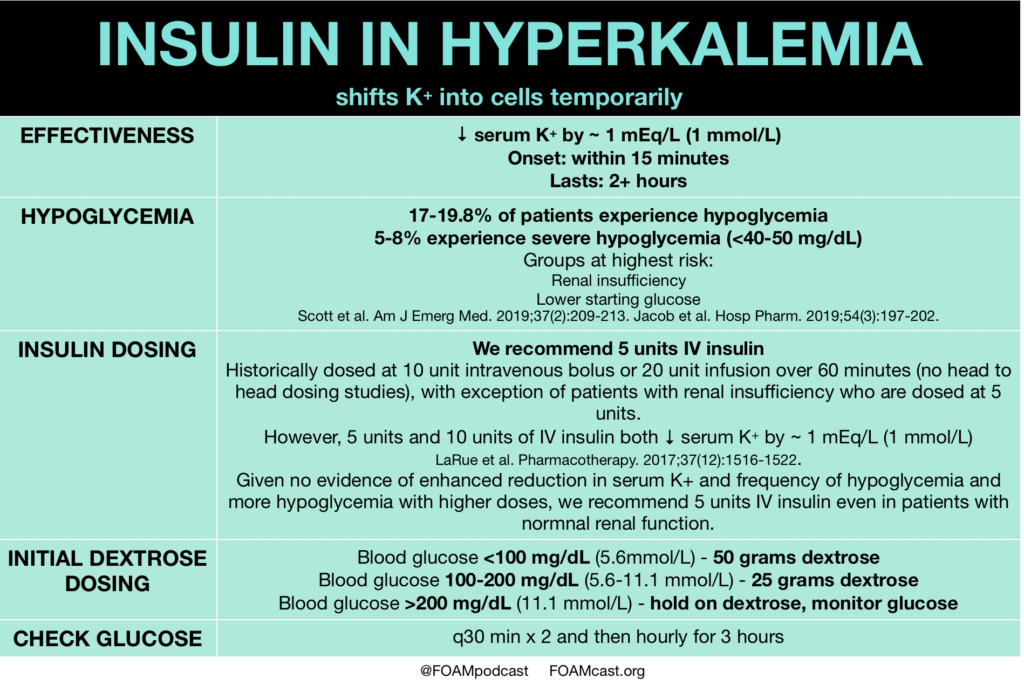
Insulin and Glucose
Insulin, a hormone produced by the pancreas, plays a crucial role in regulating blood sugar levels. However, it also has the ability to promote the movement of potassium from the blood into the cells. When administered in combination with glucose, which helps prevent low blood sugar levels, insulin can effectively lower potassium levels. Insulin and glucose are often used in the acute treatment of hyperkalemia, particularly in cases where potassium levels are critically high or when other interventions have failed.
Beta-2 Agonists
Beta-2 agonists, such as albuterol, are medications commonly used to treat respiratory conditions like asthma. However, they also have the ability to lower potassium levels in the blood. These medications work by stimulating the beta-2 receptors in the body, which ultimately promotes the movement of potassium from the bloodstream into the cells. Beta-2 agonists are typically administered via inhalation and can provide rapid relief in cases of acute hyperkalemia.
Loop Diuretics
Loop diuretics are a class of medications that play a crucial role in managing fluid and electrolyte imbalances. In the treatment of hyperkalemia, loop diuretics, such as furosemide, act by increasing the excretion of potassium through urine. By inhibiting the reabsorption of sodium and chloride in the kidneys, loop diuretics indirectly lead to increased potassium excretion. While loop diuretics may not be effective as a standalone treatment for hyperkalemia, they are often used in combination with other interventions to lower potassium levels.
Sodium Polystyrene Sulfonate (Kayexalate)
Sodium polystyrene sulfonate, commonly known by its brand name Kayexalate, is a medication used in the management of hyperkalemia. It works by binding excess potassium in the intestines, facilitating its elimination from the body through bowel movements. This medication is typically administered orally or rectally and is considered an option when other treatments have failed or are contraindicated.
Non-Pharmacological Treatments
Dietary Modifications
Dietary modifications play a crucial role in managing hyperkalemia. Individuals with this condition are advised to limit their intake of high-potassium foods, such as bananas, oranges, tomatoes, potatoes, and dried fruits. Additionally, reducing or avoiding salt substitutes, which often contain potassium chloride, is also recommended. Working closely with a registered dietitian can help individuals develop a well-balanced meal plan that meets their nutritional needs while keeping potassium levels in check.
Potassium-Reducing Medications
In some cases, individuals with chronic hyperkalemia may benefit from potassium-reducing medications. These medications, such as sodium polystyrene sulfonate or patiromer, work by binding excess potassium in the body, facilitating its elimination through the bowel or urine. They are typically prescribed when dietary modifications alone are not sufficient to control potassium levels.
Dialysis
For individuals with severe or refractory hyperkalemia, dialysis may be necessary. Dialysis is a procedure that involves the use of a machine to filter waste products and excess fluids from the blood when the kidneys are unable to perform this function effectively. In addition to removing toxins, dialysis can also help lower potassium levels by removing excess potassium from the bloodstream. Dialysis is typically recommended for individuals with chronic kidney disease or acute kidney injury who are unable to adequately manage their potassium levels through other means.
Emerging Therapies
Advancements in medical research have led to the development of emerging therapies for hyperkalemia. These innovative treatments aim to improve the management of hyperkalemia by targeting specific mechanisms involved in potassium regulation. Examples include new medications that selectively bind potassium in the intestines, thereby reducing its absorption into the bloodstream. While these therapies are still undergoing clinical trials, they hold promise for the future treatment and prevention of hyperkalemia.
Management of Underlying Causes
Correction of Acid-Base Balance
In cases where hyperkalemia is accompanied by metabolic acidosis, addressing the acid-base imbalance is essential. This may involve administering medications or fluids to correct the pH of the blood. By restoring the acid-base balance, potassium levels can be better regulated, reducing the risk of recurrent hyperkalemia.
Treating Kidney Dysfunction
Since the kidneys play a crucial role in regulating potassium levels, addressing any kidney dysfunction is vital in managing hyperkalemia. This may involve treating underlying conditions that contribute to impaired kidney function, such as chronic kidney disease or acute kidney injury. Additionally, optimizing fluid and electrolyte balance through medications and fluid therapy can help improve kidney function and reduce the risk of hyperkalemia.
Treating Adrenal Dysfunction
Adrenal insufficiency, a condition characterized by decreased production of adrenal hormones, can contribute to hyperkalemia. Treating the underlying adrenal dysfunction is essential in managing hyperkalemia associated with this condition. This may involve hormone replacement therapy, such as corticosteroids, to restore normal adrenal function and help regulate potassium levels.
Addressing Medication-Related Causes
Certain medications, such as potassium-sparing diuretics, ACE inhibitors, and ARBs, contribute to hyperkalemia. In these cases, adjusting the dose or discontinuing these medications may be necessary to manage potassium levels effectively. However, it is essential to work closely with a healthcare provider to ensure that any medication adjustments do not compromise the management of other underlying medical conditions.
Prevention and Long-Term Management
Educating Patients about Potassium Levels
Educating patients about the importance of monitoring potassium levels and understanding the dietary and medication factors that can contribute to hyperkalemia is crucial in preventing recurrent episodes. Patients should be aware of high-potassium foods and advised to read food labels carefully to identify potassium content. Proper education empowers individuals to make informed choices and actively participate in managing their health.
Regular Blood Testing and Monitoring
Regular blood testing is essential in monitoring potassium levels and detecting any changes early on. The frequency of blood tests may vary depending on the severity of hyperkalemia, underlying medical conditions, and the effectiveness of treatment interventions. Close monitoring allows healthcare providers to assess the efficacy of treatment and make any necessary adjustments to ensure optimal potassium control.
Lifestyle Modifications
In addition to dietary modifications, lifestyle changes can help prevent hyperkalemia. Maintaining a healthy lifestyle that includes regular exercise, adequate hydration, and stress reduction can support overall kidney function and electrolyte balance. Avoiding activities that can lead to excessive muscle breakdown or tissue trauma, such as extreme exercise or injury, can also help prevent acute hyperkalemia.
Medication Adjustments
Individuals taking medications known to contribute to hyperkalemia should work closely with their healthcare providers to determine appropriate dosages or alternative treatment options. Adjusting medication regimens or adding potassium-reducing medications may be necessary to prevent recurrent hyperkalemia.
Regular Follow-Up Care
Regular follow-up care is vital in managing hyperkalemia effectively. Individuals with this condition should schedule routine appointments with their healthcare providers to monitor potassium levels, assess treatment effectiveness, and address any concerns or questions. Ongoing communication and collaboration with healthcare providers ensure that treatment plans are tailored to the individual’s specific needs, helping to prevent complications and improve long-term outcomes.
Complications and Prognosis
Potential Complications of Hyperkalemia
Hyperkalemia can lead to various complications if left untreated or poorly managed. The most significant concern is the risk of abnormal heart rhythms, which can have potentially life-threatening consequences, including cardiac arrest. Other complications may include muscle weakness, paralysis, respiratory distress, and kidney dysfunction. The severity of complications often depends on the extent of hyperkalemia and the underlying medical conditions present. However, with appropriate management strategies and regular monitoring, the risk of complications can be minimized.
Prognosis and Outlook
The prognosis for individuals with hyperkalemia depends on several factors, including the severity of the condition, the underlying cause, and the individual’s overall health. Mild to moderate cases of hyperkalemia can often be managed effectively with lifestyle modifications, medication adjustments, and regular monitoring. However, individuals with severe hyperkalemia or those with significant underlying medical conditions may require more aggressive treatment interventions and close medical supervision. With proper management, the prognosis for hyperkalemia is generally favorable, and individuals can lead normal, healthy lives with minimal complications.

Conclusion
Hyperkalemia is a medical condition characterized by high levels of potassium in the blood. It can have serious consequences if left untreated or poorly managed. Understanding the causes, symptoms, diagnosis, and management of hyperkalemia is essential in providing effective treatment and preventing complications. From immediate measures to stabilize potassium levels in emergencies to pharmacological and non-pharmacological treatments for long-term management, there are various strategies available. With proper education, regular monitoring, and appropriate lifestyle modifications, individuals with hyperkalemia can lead healthy lives and minimize the risk of complications. Working closely with healthcare providers and adhering to treatment plans is key to maintaining optimal potassium levels and promoting overall well-being.