Are you struggling with high blood glucose levels? Don’t worry, help is at hand! In this article, we will explore effective treatments and strategies to manage elevated blood sugar levels. From lifestyle changes to medication options, we’ve got you covered. Let’s delve into the world of high blood glucose treatment and find solutions to navigate this condition with confidence and control.
Medications for High Blood Glucose Treatment
Insulin Therapy
When it comes to managing high blood glucose levels, insulin therapy is often considered one of the most effective and commonly prescribed treatments. Insulin is a hormone that helps regulate blood sugar by allowing glucose to enter cells and be used for energy. For individuals with diabetes, their bodies either do not produce enough insulin or do not effectively use the insulin they produce. Insulin therapy involves the use of injected insulin to help control blood sugar levels. There are different types of insulin available, including rapid-acting, short-acting, intermediate-acting, and long-acting insulin. The choice of insulin type and administration method will vary depending on the individual’s needs and preferences.
Oral Medications for Type 2 Diabetes
For individuals with type 2 diabetes, oral medications can be used to help lower high blood glucose levels. These medications work in various ways to improve insulin sensitivity, reduce glucose production in the liver, or increase the release of insulin from the pancreas. Some common types of oral medications include metformin, sulfonylureas, meglitinides, thiazolidinediones, and DPP-4 inhibitors. It is important to note that oral medications are typically not used as the sole treatment for individuals with type 1 diabetes, as they still require insulin.
Other Injectable Medications
In addition to insulin, there are also other injectable medications available to help manage high blood glucose levels. These medications are primarily used for individuals with type 2 diabetes who cannot effectively control their blood sugar with oral medications alone. Some examples include GLP-1 receptor agonists, which help stimulate insulin release and suppress glucagon secretion, and amylin analogs, which reduce glucose production from the liver and slow down the emptying of the stomach. These injectable medications can be valuable options for those who may have contraindications or difficulties with insulin therapy.
Lifestyle Changes to Manage High Blood Glucose
Healthy Diet
A healthy diet is a key component of managing high blood glucose levels. It’s important to focus on consuming a balanced diet that includes a variety of nutrient-dense foods. This means incorporating plenty of fruits, vegetables, whole grains, lean proteins, and healthy fats into your meals. It’s also essential to limit the intake of sugary foods and beverages, refined carbohydrates, and unhealthy fats. Portion control is another important aspect of a healthy diet, as it helps maintain stable blood glucose levels throughout the day. Consulting a registered dietitian or healthcare professional can be beneficial in creating a personalized meal plan that meets your specific dietary needs.
Regular Physical Activity
Engaging in regular physical activity is not only important for overall health but also plays a significant role in managing high blood glucose levels. Physical activity helps increase insulin sensitivity, allowing glucose to be more effectively utilized by the body’s cells. Aim for at least 150 minutes of moderate-intensity aerobic activity per week, along with strength training exercises at least two days a week. It’s important to choose activities that you enjoy and are suitable for your fitness level. Consult with your healthcare provider before starting a new exercise regimen, especially if you have any underlying health conditions.
Weight Management
Maintaining a healthy weight or working towards weight loss (if necessary) can greatly contribute to managing high blood glucose levels. Excess weight, especially around the abdomen, can lead to insulin resistance and increase the risk of developing type 2 diabetes. By adopting a balanced diet and engaging in regular physical activity, you can achieve and maintain a healthy weight. If needed, a healthcare professional can provide guidance and support in creating a weight management plan tailored to your specific needs and goals.
Stress Reduction
Stress can significantly impact blood glucose levels, as it triggers the release of stress hormones like cortisol and can interfere with insulin action. Finding effective ways to manage stress is crucial in maintaining stable blood glucose levels. This can include techniques such as meditation, deep breathing exercises, yoga, or engaging in hobbies and activities that bring joy and relaxation. Building a support system and seeking professional help when needed are also important steps in managing stress. It’s important to prioritize self-care and make time for activities that promote mental and emotional well-being.
Monitoring and Managing Blood Glucose Levels
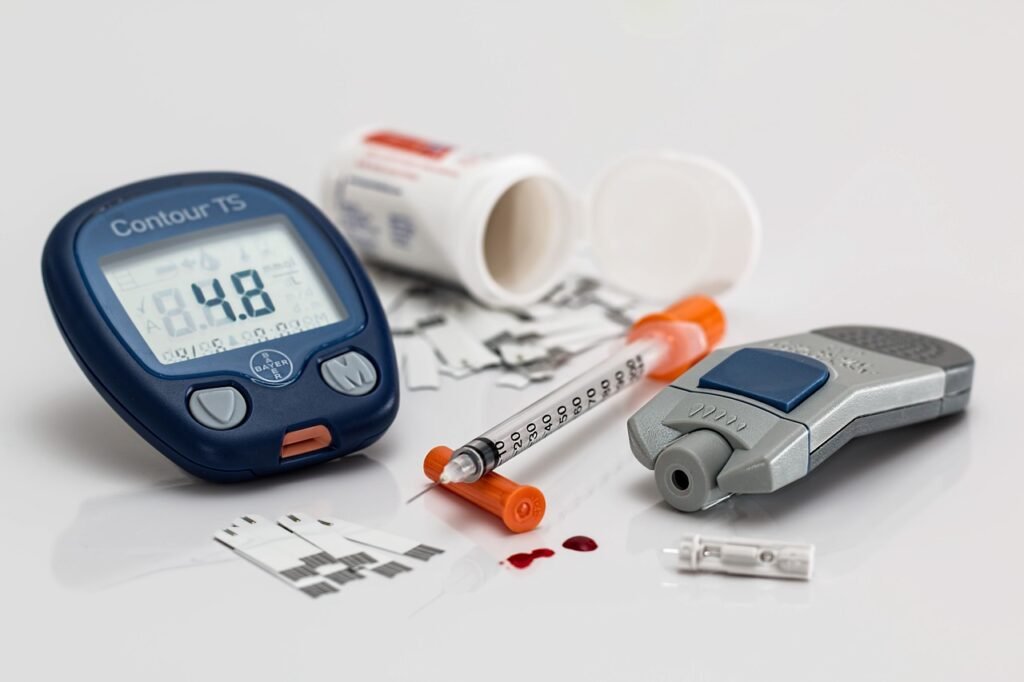
Self-Monitoring of Blood Glucose
Regular self-monitoring of blood glucose levels is an essential part of managing high blood glucose. It allows individuals to track their blood sugar levels and make appropriate adjustments to medication, diet, and physical activity. Self-monitoring involves using a blood glucose meter to obtain a small drop of blood and measure the current glucose level. The frequency and timing of blood glucose monitoring may vary depending on the individual’s treatment plan and their healthcare provider’s recommendations. It’s important to keep a record of blood glucose readings to identify patterns and share them with your healthcare team for better management.
Continuous Glucose Monitoring Systems
Continuous glucose monitoring (CGM) systems provide real-time glucose readings throughout the day, allowing for a comprehensive view of blood glucose fluctuations. These systems consist of a small sensor inserted under the skin, which measures glucose levels in interstitial fluid, and a receiver or smartphone app that displays the data. CGM systems can help individuals identify trends, predict high or low blood glucose levels, and make timely adjustments to their diabetes management plan. It’s important to calibrate CGM systems as directed by the manufacturer to ensure accurate readings.
Insulin Pumps
Insulin pumps are devices that deliver insulin continuously throughout the day, mimicking the function of a healthy pancreas. They are attached to the body via a small tube or patch and can provide precise insulin dosing based on individualized settings. Insulin pumps offer greater flexibility and convenience compared to multiple daily injections, as they allow for more precise insulin delivery and can be adjusted to match varying insulin needs. However, insulin pumps require proper education and training to ensure safe and effective use. Consulting with a healthcare professional is essential when considering an insulin pump as part of your diabetes management plan.
Treatment for Acute Complications of High Blood Glucose
Diabetic Ketoacidosis (DKA)
Diabetic ketoacidosis (DKA) is a severe and potentially life-threatening complication of high blood glucose levels. It occurs primarily in individuals with type 1 diabetes but can also affect those with type 2 diabetes in rare cases. DKA develops when a shortage of insulin leads to the accumulation of ketones in the blood, causing a state of metabolic imbalance. Symptoms of DKA include excessive thirst, frequent urination, abdominal pain, nausea, vomiting, fruity breath odor, and confusion. Immediate medical attention is required for DKA, as it necessitates fluid replacement, insulin therapy, and electrolyte correction.
Hyperosmolar Hyperglycemic State (HHS)
Hyperosmolar hyperglycemic state (HHS) is another severe complication that can arise from high blood glucose levels, particularly in individuals with type 2 diabetes. HHS is characterized by extremely high blood sugar levels and dehydration. It typically develops over a longer period compared to DKA and is often triggered by underlying medical conditions or infections. The symptoms of HHS may include extreme thirst, dry mouth, fever, confusion, weakness, and visual disturbances. HHS requires immediate medical attention, as treatment involves intravenous fluids, insulin therapy, and addressing the underlying cause.
Hypoglycemia
Hypoglycemia, or low blood sugar, is a common concern for individuals who are managing high blood glucose levels with medication or insulin therapy. It can occur when blood glucose levels drop too low, leading to symptoms such as shakiness, dizziness, sweating, confusion, and irritability. Treating hypoglycemia involves consuming a source of fast-acting carbohydrates, such as fruit juice, glucose tablets, or candy. Regular monitoring of blood glucose levels, understanding the signs and symptoms of hypoglycemia, and carrying appropriate snacks to treat low blood sugar are essential in preventing and managing this acute complication.

Management of Long-Term Complications
Cardiovascular Disease
High blood glucose levels over an extended period can increase the risk of developing cardiovascular disease. It is essential to manage and control blood glucose levels to minimize the risk of long-term complications. Adopting a healthy lifestyle, including regular exercise, a nutritious diet, and maintaining a healthy weight, is crucial in reducing cardiovascular risk. Additionally, managing blood pressure and cholesterol levels, quitting smoking, and regular medical check-ups are important components of cardiovascular disease prevention and management.
Nerve Damage
Consistently high blood glucose levels can cause nerve damage, a condition known as diabetic neuropathy. Symptoms can vary and may include numbness, tingling, pain, and weakness, usually in the hands and feet. Managing blood glucose levels within target ranges can help slow the progression of nerve damage. Assistance from healthcare professionals, including neurologists and pain specialists, may be necessary to manage the symptoms and provide appropriate treatment.
Kidney Disease
Diabetes is a leading cause of kidney disease, known as diabetic nephropathy. Elevated blood glucose levels can damage the small blood vessels in the kidneys, impairing their ability to filter waste and fluids properly. Managing blood glucose levels and maintaining optimal blood pressure are crucial for preventing or slowing the progression of kidney disease. Individuals with diabetes also need regular kidney function tests to monitor their kidney health. Collaborating with healthcare professionals, including nephrologists and dietitians, can help develop a comprehensive treatment plan.
Eye Complications
High blood glucose levels can have detrimental effects on the eyes, potentially causing various eye complications such as diabetic retinopathy, cataracts, and glaucoma. Diabetic retinopathy is particularly concerning, as it can lead to vision loss if left untreated. It is essential to have regular eye examinations to detect any signs of eye complications early on, allowing for timely treatment and management. Controlling blood glucose levels, managing blood pressure, and avoiding smoking are key measures in preventing and reducing the risk of eye complications.
Alternative and Complementary Therapies
Herbal Remedies
Some individuals may explore the use of herbal remedies to manage high blood glucose levels. While certain herbs and spices, such as cinnamon, bitter melon, and fenugreek, have shown potential in helping regulate blood sugar levels, it’s important to discuss their use with a healthcare professional. Herbal remedies can interact with medications and may not be suitable for everyone. The dosage, potential side effects, and overall effectiveness should be thoroughly evaluated before incorporating herbal remedies into a treatment plan.
Supplements
Certain dietary supplements, such as chromium, magnesium, and alpha-lipoic acid, have been suggested to have blood sugar-regulating effects. However, it is important to note that scientific evidence regarding their effectiveness is conflicting and limited. Before starting any supplements, it is crucial to consult with a healthcare professional to evaluate their safety, potential benefits, and potential interactions with other medications or treatments.
Acupuncture
Acupuncture is an ancient Chinese practice that involves inserting thin needles into specific points on the body to restore balance and promote healing. Some individuals may turn to acupuncture as a complementary treatment for managing high blood glucose levels. While research on its effectiveness in diabetes management is still limited, some studies have shown promising results in improving blood glucose control and reducing insulin resistance. If considering acupuncture, it is important to seek a qualified and licensed acupuncturist who specializes in diabetes management and to discuss it with your healthcare team.
Mind-Body Techniques
Mind-body techniques, such as meditation, mindfulness, and yoga, have gained popularity as complementary strategies for managing stress and blood glucose levels. These practices can help promote relaxation, improve mental well-being, and potentially enhance glucose control. Engaging in mind-body techniques can be a valuable addition to one’s diabetes management plan. It is important to seek guidance from qualified instructors or healthcare professionals experienced in these techniques to ensure proper implementation and maximize their benefits.

Importance of Regular Medical Care and Team Approach
Medical Check-ups
Regular medical check-ups are crucial for individuals managing high blood glucose levels. These check-ups allow healthcare professionals to monitor blood glucose control, assess overall health, and address any concerns or complications promptly. During check-ups, healthcare providers may conduct physical examinations, perform blood tests, review self-monitoring records, and adjust treatment plans if necessary. It is essential to attend scheduled appointments and communicate openly with your healthcare team to achieve optimal blood glucose management.
Diabetes Education and Support
Diabetes education and support play a vital role in successfully managing high blood glucose levels. Diabetes educators can provide valuable information and resources to help individuals understand their condition, learn self-care skills, and make informed decisions about their treatment plans. Support groups and online communities can also provide emotional support and a platform to share experiences and knowledge. It is important to actively seek out diabetes education programs and support networks tailored to your needs and actively participate in them.
Collaborating with Healthcare Professionals
Collaboration between individuals managing high blood glucose levels and their healthcare professionals is crucial for effective diabetes management. It is important to establish open and honest communication with your healthcare team, including physicians, nurses, dietitians, pharmacists, and diabetes educators. Sharing your concerns, goals, and preferences will enable your healthcare team to develop a comprehensive treatment plan that aligns with your needs and lifestyle. Regular follow-up appointments and ongoing communication ensure that your treatment plan remains personalized and effective.
Conclusion
Taking control of high blood glucose requires a combination of various treatment approaches, lifestyle modifications, and regular medical care. Medications, such as insulin therapy and oral medications, can help regulate blood sugar levels effectively. Making healthy lifestyle changes, such as adopting a balanced diet, engaging in regular physical activity, managing weight, and reducing stress, significantly contribute to maintaining stable blood glucose levels. Monitoring blood glucose levels through self-monitoring, continuous glucose monitoring systems, and utilizing insulin pumps can help individuals make timely adjustments to their diabetes management plans. Treatment for acute complications, such as DKA or hypoglycemia, requires immediate medical attention. Long-term complications can be managed through cardiovascular disease prevention, nerve damage management, kidney disease monitoring, and eye examinations. Exploring alternative and complementary therapies, alongside regular medical care and a team approach, can enhance one’s diabetes management plan. By actively engaging with healthcare professionals and finding the right treatment plan, individuals can successfully take control of their high blood glucose levels and lead a healthy and fulfilling life.