Have you ever wondered what psoriasis looks like when it first appears? Well, wonder no more! In this article, we will explore the early stages of psoriasis and how it presents itself on your skin. Psoriasis, a chronic skin condition, can manifest in various ways, and recognizing its initial signs is crucial for early detection and proper treatment. So, if you’re curious about how psoriasis appears when it starts, keep reading to uncover the fascinating world of this skin condition.
Understanding Psoriasis
Psoriasis is a chronic autoimmune skin condition characterized by the rapid buildup of skin cells, resulting in red, raised patches covered with silver or white scales. It is a non-contagious condition that affects around 2% of the global population. The exact cause of psoriasis is still unknown, but it is believed to involve a combination of genetic factors, immune system abnormalities, and environmental triggers.
Definition of Psoriasis
Psoriasis is a chronic autoimmune skin condition that causes red, raised patches covered with silver or white scales. It occurs when the immune system mistakenly attacks healthy skin cells, causing them to grow rapidly and accumulate on the surface of the skin.
Triggers for Psoriasis
While the exact cause of psoriasis is unknown, certain factors are known to trigger or worsen the condition. Common triggers include stress, infections, injuries to the skin, certain medications, smoking, and excessive alcohol consumption. Understanding and avoiding these triggers can help manage psoriasis symptoms.
Prevalence and Types of Psoriasis
Psoriasis is a common condition that affects people of all ages, genders, and ethnicities. It is estimated that around 2% of the global population has psoriasis. There are several types of psoriasis, including plaque psoriasis, guttate psoriasis, pustular psoriasis, inverse psoriasis, and erythrodermic psoriasis. Each type has its own unique characteristics and affects different parts of the body.
Early Symptoms of Psoriasis
Early detection of psoriasis is crucial for successful management and treatment. Here are some common early symptoms to look out for:
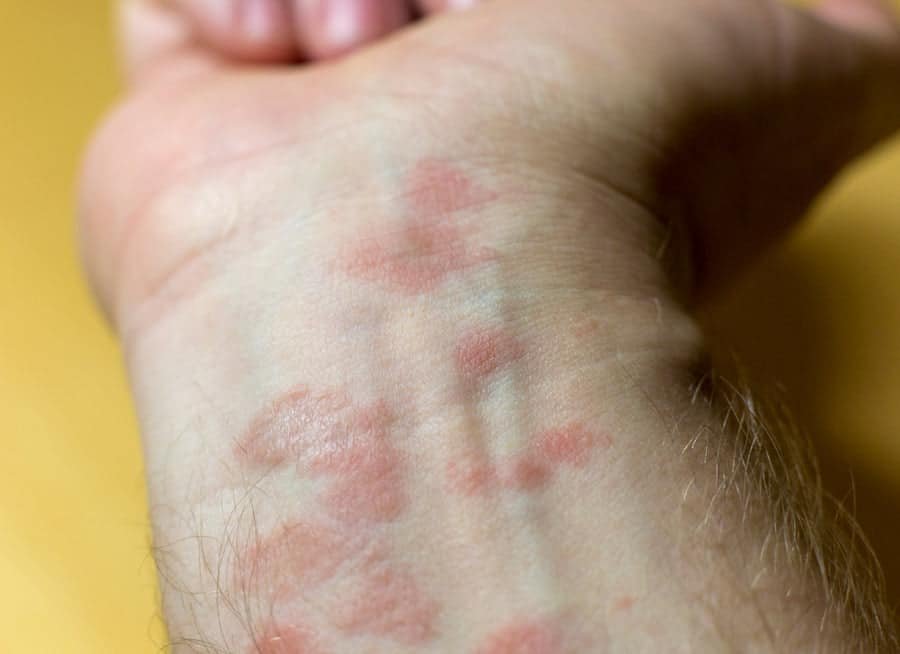
Red Patches on the Skin
One of the earliest symptoms of psoriasis is the appearance of red patches on the skin. These patches are often raised and may be covered with silver or white scales. They can occur on any part of the body, but are commonly found on the elbows, knees, scalp, and lower back.
Raised and Thickened Skin
Psoriasis can cause the skin to become thick and raised. This is due to the rapid buildup of skin cells, which leads to the formation of plaques. These plaques can be itchy, painful, and may crack or bleed in severe cases.
Silver or White Scales
Another early symptom of psoriasis is the presence of silver or white scales on the skin. These scales are a result of the excessive production of skin cells. They can be easily scraped off, but tend to reappear quickly.
Dry and Cracked Skin
Psoriasis can cause the skin to become dry and cracked. This can be especially uncomfortable and painful, as the skin loses its natural moisture and becomes more susceptible to irritation.
Itching and Burning Sensation
Itching and burning sensation are common symptoms of psoriasis. The intense itching can be incredibly irritating and can disrupt daily activities. Scratching can lead to skin damage and an increased risk of infection.
Psoriasis on Different Body Parts
Psoriasis can occur on various parts of the body, each with its own unique characteristics and challenges. Here are some examples:
Scalp Psoriasis
Scalp psoriasis is characterized by red patches and scales on the scalp. These patches can be itchy and may extend beyond the hairline, onto the forehead, neck, and ears. Flaking and dryness are common symptoms of scalp psoriasis.
Facial Psoriasis
Facial psoriasis can affect various areas of the face, such as the eyebrows, hairline, and the skin around the nose and mouth. It can cause redness, scaling, and plaques on the face, which can be particularly distressing for the individual.
Nail Psoriasis
Psoriasis can also affect the nails, causing pitting, discoloration, thickening, and irregular nail growth. Nail psoriasis can be painful and may lead to nail deformities if left untreated.
Hand and Foot Psoriasis
Psoriasis on the hands and feet can cause redness, scaling, and painful cracks in the skin. This can make simple tasks, such as walking or using the hands, extremely uncomfortable.
Psoriasis on Elbows and Knees
Psoriasis commonly affects the elbows and knees, causing thickened, scaly patches that can be itchy and painful. The constant movement and friction in these areas can worsen the symptoms.
Inverse Psoriasis
Inverse psoriasis occurs in skin folds, such as the armpits, groin, and under the breasts. It appears as smooth, red patches that are not scaly. Inverse psoriasis can be particularly uncomfortable due to the high levels of moisture and friction in these areas.
Unique Characteristics of Psoriasis
Psoriasis has several unique characteristics that help distinguish it from other skin conditions. These characteristics are important for accurate diagnosis and appropriate treatment of the condition.
Koebner Phenomenon
The Koebner phenomenon is the development of new psoriatic lesions in areas of skin that have been injured or traumatized. This can occur as a result of scratching, cuts, burns, or even mild friction. It is essential to avoid or minimize the risk of injury to prevent the worsening of psoriasis symptoms.
Auspitz Sign
The Auspitz sign refers to the appearance of pinpoint bleeding spots when psoriatic scales are scraped off. This is a characteristic feature of psoriasis and can help confirm the diagnosis.
HLA-Cw6 Gene
A specific gene called HLA-Cw6 is associated with a higher risk of developing psoriasis. Genetic testing can help identify individuals who may be at a higher risk of developing the condition.
Koebner Phenomenon
The Koebner phenomenon is the development of new psoriatic lesions in areas of skin that have been injured or traumatized. This can occur as a result of scratching, cuts, burns, or even mild friction. It is essential to avoid or minimize the risk of injury to prevent the worsening of psoriasis symptoms.
Different Types of Psoriasis Lesions
Psoriasis can present in various forms, each with its own unique characteristics and appearance. Here are some common types of psoriasis lesions:
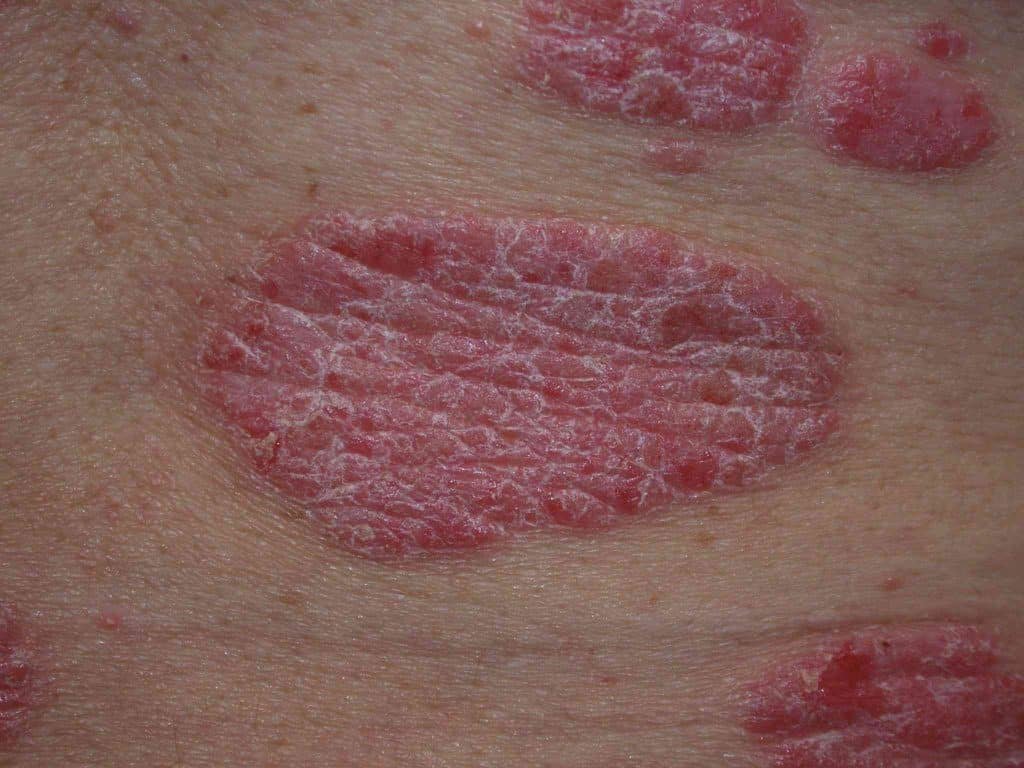
Plaque Psoriasis Lesions
Plaque psoriasis is the most common form of psoriasis, characterized by well-defined red patches with silver or white scales. These patches often appear on the elbows, knees, lower back, and scalp. The plaques can be itchy, painful, and can crack or bleed in severe cases.
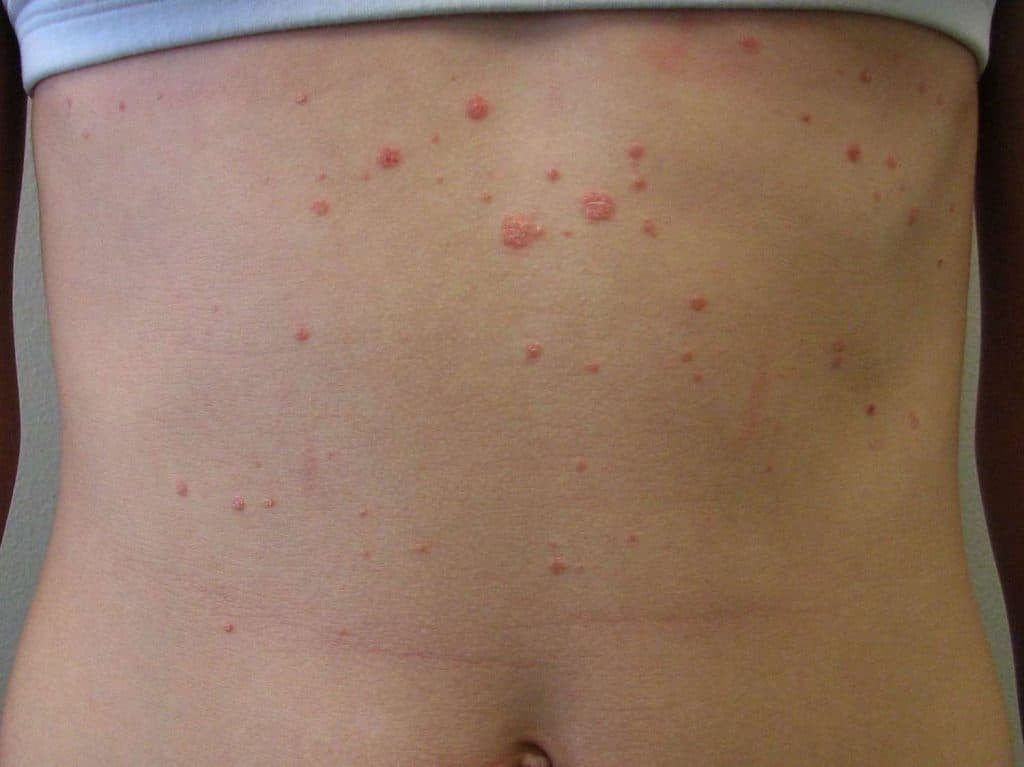
Guttate Psoriasis Lesions
Guttate psoriasis appears as small, teardrop-shaped red spots on the skin. These spots are usually small and widespread, often appearing on the trunk, arms, legs, and scalp. Guttate psoriasis is often triggered by a bacterial or viral infection, and it tends to occur more frequently in children and young adults.
Pustular Psoriasis Lesions
Pustular psoriasis is characterized by the presence of pus-filled blisters surrounded by red skin. These blisters can be painful and may cause flu-like symptoms, such as fever and chills. Pustular psoriasis can affect localized areas of the body or be generalized, covering larger areas.
Inverse Psoriasis Lesions
Inverse psoriasis appears as smooth, red patches in the skin folds, such as the armpits, groin, and under the breasts. Unlike other types of psoriasis, inverse psoriasis does not typically have scales. The high levels of moisture and friction in these areas can make inverse psoriasis particularly uncomfortable.
Erythrodermic Psoriasis Lesions
Erythrodermic psoriasis is a severe form of psoriasis that can cover the entire body with a red, peeling rash. It can cause intense itching, pain, and may lead to severe complications, such as dehydration and infection. Erythrodermic psoriasis requires immediate medical attention.
Chronic Inflammation and Psoriasis
Psoriasis is not just a skin condition; it is also characterized by chronic inflammation in the body. The immune system plays a significant role in the development of psoriasis, leading to an overactive inflammatory response.
Role of Immune System
In psoriasis, T-cells, a type of white blood cell, mistakenly target the skin cells, triggering inflammation and rapid cell growth. This immune system dysfunction leads to the development of psoriatic lesions on the skin.
Inflammatory Response
The chronic inflammation associated with psoriasis can extend beyond the skin. It can affect the joints, resulting in a condition known as psoriatic arthritis. Inflammation in the blood vessels can increase the risk of cardiovascular diseases. It is essential to manage inflammation to prevent complications associated with psoriasis.
Medical Diagnosis of Psoriasis
A medical diagnosis is essential for the accurate identification and appropriate management of psoriasis. Healthcare professionals use various methods to diagnose psoriasis, including:
Physical Examination
During a physical examination, a healthcare professional will examine the skin and nails for signs of psoriasis. They will look for redness, scaling, plaques, and other characteristic lesions associated with psoriasis.
Biopsy and Histopathology
In some cases, a skin biopsy may be required to confirm the diagnosis of psoriasis. A small sample of affected skin is taken and analyzed under a microscope to look for the characteristic changes associated with psoriasis, such as an increased number of skin cells and inflammation.
Psoriasis Severity Index (PASI)
The Psoriasis Severity Index (PASI) is a tool used to assess the severity of psoriasis. It takes into account the extent of skin involvement, redness, scaling, and thickness of the plaques. This index helps guide treatment decisions and monitor the progression of the condition.
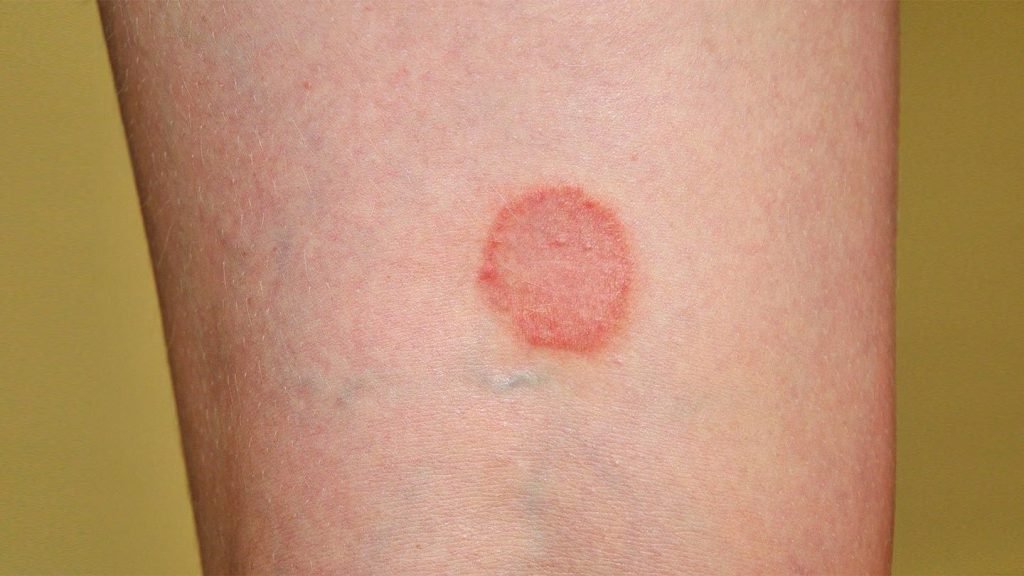
Distinguishing Psoriasis from Eczema
Psoriasis and eczema are both chronic skin conditions that can cause red, itchy patches on the skin. However, there are some distinguishing factors that can help differentiate between the two conditions.
Symptoms Comparison
Psoriasis typically causes raised, silvery scales on the skin, while eczema often presents with dry, scaly patches. Psoriasis lesions may be more well-defined and angulated, while eczema lesions tend to be more irregular in shape.
Visual Appearance
Psoriasis lesions are often raised and can have a silvery sheen. Eczema lesions, on the other hand, are usually red and can appear oozing or crusty.
Age of Onset
Psoriasis can develop at any age, but it often manifests between the ages of 15 and 35. Eczema, on the other hand, tends to begin in early childhood and can persist into adulthood.
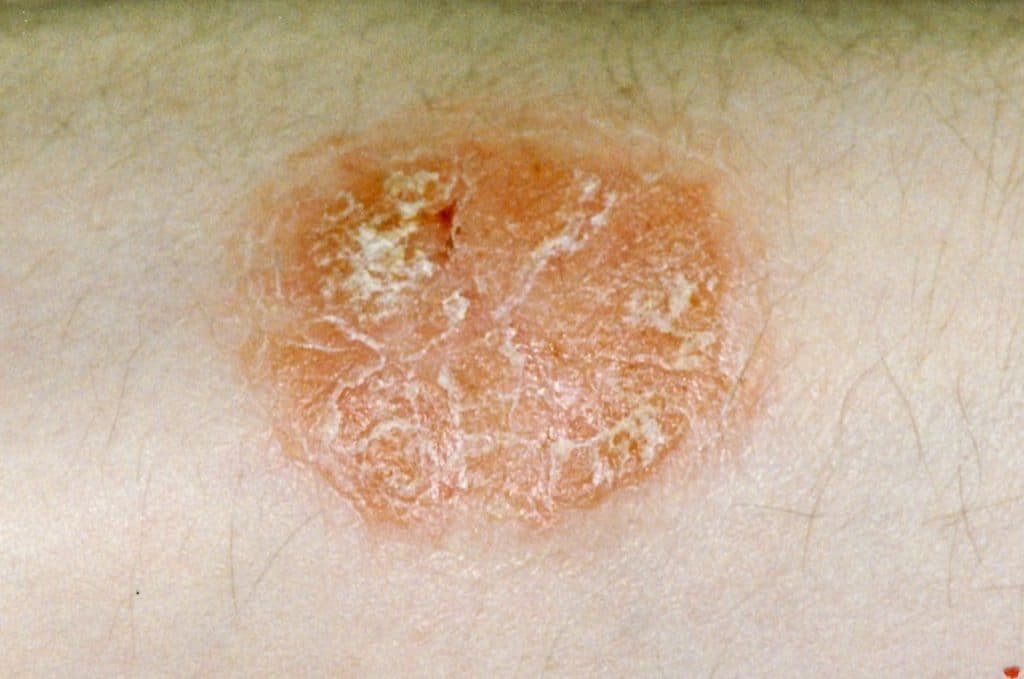
Progression of Psoriasis
Psoriasis is a chronic condition that tends to progress in stages. Understanding the different stages of psoriasis can help individuals identify the severity of their condition and seek appropriate treatment.
Stages of Psoriasis
The stages of psoriasis can vary from mild to severe, with varying degrees of symptoms. Mild psoriasis may involve small, localized patches, while severe psoriasis can cover large areas of the body and cause significant discomfort.
Complications and Associated Conditions
Psoriasis is not just a skin condition; it can also have a significant impact on overall health and well-being. Individuals with psoriasis have an increased risk of developing other conditions, such as psoriatic arthritis, cardiovascular disease, obesity, and metabolic syndrome. It is important to manage psoriasis effectively to reduce the risk of these complications.
Preventing Psoriasis Flares
While psoriasis cannot be cured, there are steps you can take to prevent and manage flare-ups. Here are some strategies to consider:
Lifestyle Changes
Adopting a healthy lifestyle can help reduce the frequency and severity of psoriasis flares. This includes maintaining a balanced diet, engaging in regular exercise, getting enough sleep, and avoiding smoking and excessive alcohol consumption.
Stress Management
Stress is a well-known trigger for psoriasis flares. Finding effective ways to manage stress, such as through meditation, yoga, or counseling, can help reduce the impact of stress on your psoriasis symptoms.
Skin Care Practices
Taking care of your skin is crucial in managing psoriasis. This includes keeping the skin moisturized, avoiding harsh soaps and hot water, and gently exfoliating to remove scales. It is also important to protect the skin from excessive sun exposure.
Avoiding Triggers
Identifying and avoiding triggers can help prevent psoriasis flares. Common triggers include infections, injuries to the skin, certain medications, smoking, and excessive alcohol consumption. By minimizing exposure to these triggers, you can reduce the frequency and severity of psoriasis symptoms.
In conclusion, understanding psoriasis is crucial for those affected by this chronic skin condition. By recognizing the early symptoms, identifying the different types of psoriasis lesions, and understanding the unique characteristics of psoriasis, individuals can better manage their condition and seek appropriate treatment. It is also important to differentiate psoriasis from other skin conditions, such as eczema, and prevent complications associated with chronic inflammation. With proper medical diagnosis and a comprehensive approach to managing psoriasis, individuals can lead fulfilling lives while keeping their symptoms under control.