In order to prevent primary congenital glaucoma, it is important to be aware of the potential risk factors and take proactive measures. This article will provide you with useful information and practical tips on how to identify the signs of primary congenital glaucoma in infants and toddlers, as well as steps you can take to lower the risk of this condition. By understanding the preventive measures, you can ensure the best possible eye health for your child. So let’s explore how we can protect our little ones from primary congenital glaucoma.
Importance of Preventing Primary Congenital Glaucoma
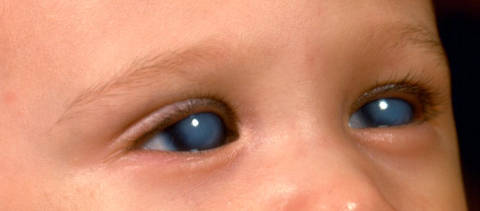
Primary Congenital Glaucoma (PCG) is a rare but potentially serious eye condition that affects infants and young children. It is crucial to prioritize the prevention of PCG, as it can lead to permanent vision loss and other complications if left untreated. By understanding the causes, implementing prevention strategies, and promoting early intervention, we can significantly reduce the impact of PCG on affected individuals and their families.
Understanding Primary Congenital Glaucoma
Definition and Overview
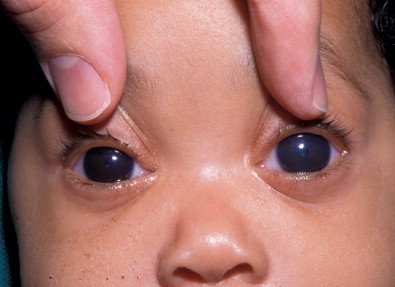
Primary Congenital Glaucoma is an inherited eye disorder characterized by increased pressure within the eye, known as intraocular pressure (IOP). This excessive pressure damages the optic nerve and can lead to irreversible vision loss. PCG typically manifests within the first year of a child’s life, with symptoms including cloudy corneas, excessive tearing, sensitivity to light, and enlarged eyes. Early diagnosis and intervention are crucial to prevent further eye damage and preserve vision.
Causes and Risk Factors
PCG is primarily caused by genetic mutations that affect the drainage system of the eye, leading to impaired fluid outflow and increased IOP. The most common genetic variations associated with PCG include mutations in the CYP1B1 and FOXC1 genes. In some cases, PCG may occur due to non-genetic factors, such as developmental abnormalities in the eye structures. While PCG is a complex condition with multifactorial causes, individuals with a family history of the disease are at a higher risk of developing it.
Diagnosing Primary Congenital Glaucoma
Signs and Symptoms
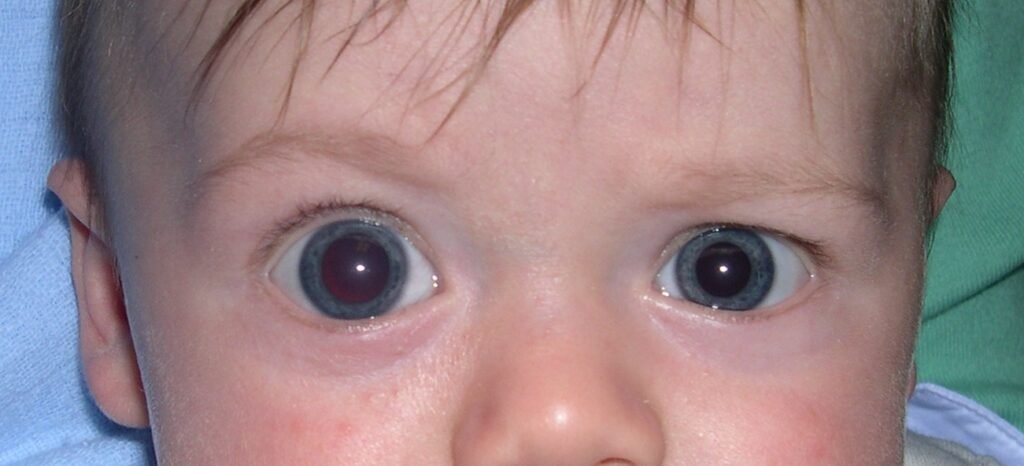
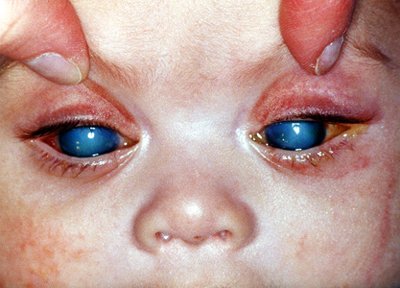
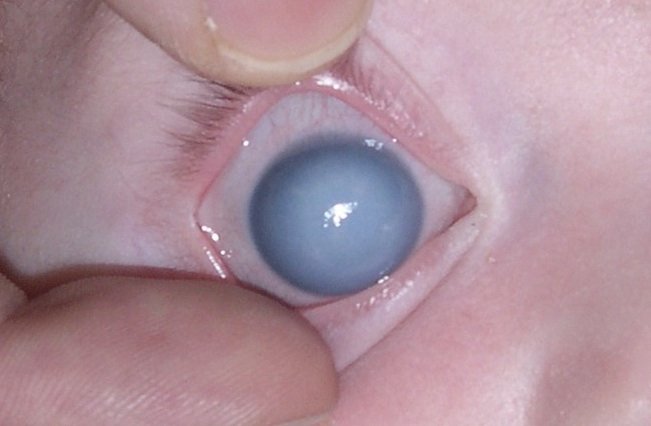
Recognizing the signs and symptoms of PCG is essential for early detection and prompt treatment. Infants with PCG may exhibit enlarged and cloudy corneas, often referred to as “haab eyes.” Other symptoms include excessive tearing, light sensitivity, blepharospasm (involuntary eyelid closure), and poor eye contact. These signs, especially when present in infants, should not be taken lightly and must be brought to the attention of a healthcare professional for further evaluation.
Screening and Testing
Screening for PCG can be done during routine newborn check-ups. However, a definitive diagnosis requires specialized tests such as gonioscopy (to examine the drainage angle of the eye), measurement of IOP, and evaluation of the optic nerve. Timely and accurate diagnosis is crucial to initiate appropriate treatment and prevent further damage to the child’s eyesight.
Prevention Strategies
Genetic Counseling
Genetic counseling plays a significant role in preventing PCG. Individuals with a family history of the disease should consult with a genetic counselor before planning a pregnancy. Genetic testing can help identify carriers of PCG-associated gene mutations, allowing couples to make informed decisions about their reproductive options. Through genetic counseling, prospective parents can gain insight into the risk of their child inheriting PCG and explore available interventions accordingly.
Prenatal Testing
Prenatal testing, such as chorionic villus sampling (CVS) or amniocentesis, can determine whether a developing fetus carries PCG-associated gene mutations. This information enables parents and healthcare providers to make informed decisions about managing the condition before or after birth. Prenatal testing, combined with genetic counseling, empowers families with knowledge and choices, providing an opportunity for early intervention when necessary.
Avoiding Risk Factors During Pregnancy
While the primary cause of PCG is genetic, certain risk factors during pregnancy may increase the likelihood of a child developing the condition. To minimize these risks, expectant mothers are advised to avoid exposure to harmful substances and medications that may adversely affect fetal eye development. Consultation with a healthcare provider is crucial during pregnancy to ensure necessary precautions are taken to reduce the risk of PCG.
Early Intervention
Treatment Options
The primary goal of early intervention in PCG is to lower intraocular pressure and prevent further damage to the optic nerve. Treatment options vary depending on the severity of the condition and may include medications, such as topical eye drops or oral medications, to reduce IOP. In some cases, surgery, such as trabeculotomy or trabeculectomy, may be necessary to improve fluid drainage and maintain normal IOP levels.
Benefits of Early Treatment
Early treatment is crucial in PCG management, as it can significantly improve the long-term prognosis and quality of life for affected individuals. By addressing the condition promptly, potential vision loss and other complications can be minimized. Regular monitoring and follow-up care are essential to ensure that treatment remains effective and adjustments can be made as the child grows and develops.
Maintaining Ocular Health
Importance of Regular Eye Exams
Regular eye exams are vital for monitoring the health of a child’s eyes, even if they have not been diagnosed with PCG. Routine eye exams can detect any changes or problems early on, allowing for swift intervention if necessary. Eye care professionals can assess visual acuity, evaluate ocular structures, measure IOP, and identify any signs of PCG or other eye conditions during these exams.
Proper Eye Care and Hygiene
Maintaining good eye care and hygiene practices can contribute to the overall ocular health of individuals, including those with PCG. This includes keeping the eyes clean by gently washing them with clean water or using a prescribed eye wash solution. Additionally, proper eyelid hygiene, such as regularly cleaning the eyelids and avoiding rubbing or touching the eyes excessively, can help prevent infections and minimize irritation.
Lifestyle Changes
Diet and Nutrition
While there is no specific diet or nutritional regimen to prevent PCG, a well-balanced diet rich in antioxidants and nutrients can support overall eye health. Foods high in vitamins A, C, and E, as well as omega-3 fatty acids, have been associated with improved eye function. Including a variety of fruits, vegetables, whole grains, and fish in your diet can help provide these essential nutrients.
Importance of Physical Activity
Maintaining an active lifestyle is beneficial for overall health, including ocular health. Engaging in regular physical activity, such as outdoor play, sports, or recreational activities, can contribute to the development of healthy eyes and visual acuity. Physical activity also promotes proper ocular circulation, which enhances the delivery of essential nutrients to the eyes and facilitates the removal of metabolic waste products.
Avoiding Environmental Triggers
Protecting Eyes from Direct Sunlight
Excessive exposure to harmful ultraviolet (UV) radiation from the sun can increase the risk of various eye conditions, including PCG. To protect the eyes, it is essential to wear sunglasses with UV protection and a wide-brimmed hat when spending time outdoors, particularly during peak sunlight hours. This helps shield the eyes from UV radiation and reduces the risk of eye damage or complications.
Reducing Exposure to Harmful Chemicals
Exposure to certain chemicals and toxins in the environment can pose a risk to ocular health, especially during critical periods of eye development. Pregnant women and parents of young children should take precautions to minimize exposure to harmful substances such as smoke, pesticides, and industrial pollutants. This can be achieved by staying in well-ventilated areas, avoiding smoking or second-hand smoke, and using non-toxic household and personal care products.
Community Education and Awareness
Reaching Out to Schools and Parents
Raising awareness about PCG among parents, educators, and healthcare providers is essential in preventing and managing the condition. Providing information and educational resources about PCG, its signs and symptoms, and available interventions can empower individuals to take appropriate actions and seek early medical evaluation. Collaborating with schools and parent organizations to distribute educational materials can help spread awareness within the community.
Promoting Eye Health in the Community
Promoting eye health overall can contribute to the prevention of PCG and other eye conditions. Organizing community initiatives, such as eye health screenings, informational sessions, or workshops, can educate the public about the importance of regular eye exams, early intervention, and maintaining good ocular health practices. By working together, communities can create a supportive environment that prioritizes eye health and encourages proactive measures.
Engaging in Research
Current Studies and Breakthroughs
Ongoing research plays a critical role in advancing our understanding of PCG and improving prevention strategies and treatment options. Current studies focus on identifying additional genes associated with PCG, developing targeted therapies, and investigating potential genetic modifiers for more personalized interventions. Staying updated with the latest research can provide individuals and healthcare professionals with valuable insights and potentially open new avenues for prevention and treatment.
Supporting Research Initiatives
Supporting research initiatives through financial contributions, participation in clinical trials, and advocacy for increased funding can accelerate progress in PCG research. By investing in research efforts, we can contribute to the development of more effective diagnostic tools, therapies, and preventative strategies. Together, we can make a difference in the lives of individuals affected by PCG and work towards a future with improved outcomes and reduced incidence of the condition.
In conclusion, the prevention of Primary Congenital Glaucoma is of utmost importance to safeguard the ocular health and well-being of infants and children. Understanding the causes, implementing prevention strategies, promoting early intervention, maintaining ocular health, making lifestyle changes, avoiding environmental triggers, educating the community, and engaging in research collectively contribute to comprehensive PCG prevention efforts. By prioritizing prevention at individual and societal levels, we can strive towards a future where PCG no longer poses a significant threat to vision and quality of life.
