When it comes to providing optimal care for patients with osteoarthritis, nurses play a pivotal role in ensuring their well-being. With a focus on nursing considerations and management, this article sheds light on key aspects to be mindful of when caring for individuals with this degenerative joint condition. From implementing effective pain management strategies to promoting self-care and providing information on available resources, nurses have the power to make a significant impact on the lives of patients living with osteoarthritis. By staying informed and compassionate, nurses can help alleviate symptoms, improve quality of life, and empower patients to take control of their health.
Assessment
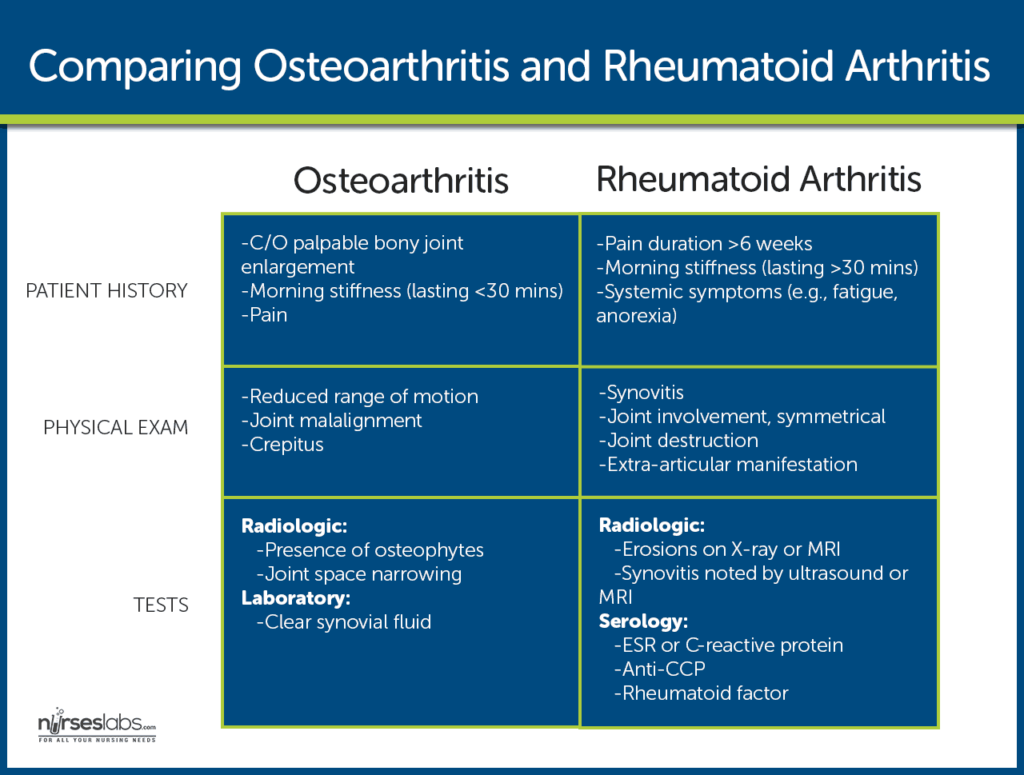
Physical assessment
In order to provide optimal care for patients with osteoarthritis, a thorough physical assessment is crucial. This includes evaluating range of motion, joint stability, and any signs of inflammation or deformity. Assessing the patient’s mobility and ability to perform activities of daily living is also essential in understanding their functional limitations. By conducting a comprehensive physical assessment, healthcare providers can generate a baseline understanding of the patient’s condition and track any changes over time, allowing for tailored interventions and monitoring.
Pain assessment
Pain is one of the most common and distressing symptoms experienced by individuals with osteoarthritis. To effectively manage pain, a thorough pain assessment must be conducted. This involves evaluating the location, intensity, and quality of the pain, as well as any factors that exacerbate or alleviate it. Additionally, nurses should assess the impact of pain on the patient’s daily activities, sleep, and overall quality of life. By understanding the nature and impact of the pain, healthcare providers can develop a comprehensive pain management plan that addresses the individual needs of the patient.
Functional assessment
Understanding the patient’s functional abilities is crucial for developing proper interventions and promoting independence in individuals with osteoarthritis. A functional assessment focuses on evaluating the patient’s ability to perform activities of daily living, such as dressing, grooming, and walking. It also involves assessing the patient’s ability to engage in leisure activities and participate in social interactions. By conducting a functional assessment, nurses can identify areas of impairment or limitation and develop strategies to optimize the patient’s functional capacity and improve their overall quality of life.
Education and Counseling
Educating patients about osteoarthritis
One of the key responsibilities of healthcare providers is to educate patients about osteoarthritis, including its causes, symptoms, and treatment options. By providing education, nurses can empower patients to actively participate in their own care and make informed decisions. They can explain the importance of exercise, weight management, and joint protection strategies in managing the symptoms of osteoarthritis. Additionally, nurses can address common misconceptions or fears that patients may have about the condition, helping to alleviate anxiety and promote a sense of control.
Assisting patients in managing pain
Pain management is a critical component of caring for patients with osteoarthritis. Nurses can assist patients in managing their pain by teaching them various non-pharmacological pain management strategies, such as heat and cold therapy, relaxation techniques, and distraction techniques. They can also provide guidance on appropriate medication use, including over-the-counter pain relievers and prescription medications. By collaborating with the healthcare team, nurses can ensure that patients receive the most effective pain relief while minimizing any potential side effects or drug interactions.
Providing resources for self-care
Promoting self-care and empowering patients to take control of their own health is an essential aspect of nursing care for individuals with osteoarthritis. Nurses can provide patients with resources and information on self-care practices, such as exercises and stretches to improve joint mobility and reduce pain. They can recommend assistive devices, such as braces and splints, to support the affected joints. Additionally, nurses can educate patients on the importance of a healthy diet and weight management in managing the symptoms of osteoarthritis. By providing resources for self-care, nurses can enable patients to actively participate in their own treatment and improve their overall well-being.

Medication Management
Understanding medication options
Medication plays a significant role in managing the symptoms of osteoarthritis. It is important for nurses to have a thorough understanding of the various medication options available to patients with osteoarthritis. This includes nonsteroidal anti-inflammatory drugs (NSAIDs), acetaminophen, and opioids. Nurses should be familiar with the potential side effects, contraindications, and dosage instructions for each medication, in order to effectively educate patients and address any concerns or questions they may have. By providing accurate and up-to-date information, nurses can help patients make informed decisions about their medication management.
Administering medications
As part of their role, nurses may be responsible for administering medications to patients with osteoarthritis. This requires knowledge of proper medication administration techniques, such as the correct dosage, route of administration, and potential interactions with other medications. Nurses must also be vigilant in monitoring for any adverse reactions or side effects. They should document medication administration accurately and communicate any concerns or changes to the healthcare team. By ensuring safe and effective administration of medications, nurses can contribute to the overall management of osteoarthritis and promote optimal patient outcomes.
Monitoring for side effects
Medication management for osteoarthritis involves not only administering medications but also closely monitoring patients for any potential side effects or adverse reactions. Nurses should educate patients about common side effects associated with their prescribed medications, such as gastrointestinal disturbances or allergic reactions. It is important for nurses to instruct patients to report any unusual symptoms promptly. Nurses should also regularly assess patients for signs of medication-related complications, such as changes in blood pressure or kidney function. By monitoring for side effects, nurses can ensure that patients receive the appropriate medications at the correct dosages, while minimizing any potential risks.
Exercise and Physical Therapy
Promoting regular exercise
Regular exercise is crucial for managing the symptoms of osteoarthritis and maintaining joint mobility. As a nurse, you can play a vital role in promoting the importance of exercise to patients with osteoarthritis. Encourage patients to engage in low-impact activities, such as swimming, walking, or cycling, which can help improve joint flexibility and strength without excessive stress on the joints. It is important to educate patients about the benefits of exercise, such as reducing pain and stiffness and improving overall physical and mental well-being. By providing tailored exercise recommendations and emphasizing the importance of regular physical activity, nurses can empower patients to incorporate exercise into their daily routine.
Collaborating with physical therapists
Physical therapy is an integral component of the management of osteoarthritis. As a nurse, you can collaborate with physical therapists to develop individualized treatment plans for patients. By sharing assessment findings and treatment goals, you can help facilitate a coordinated approach to care. Regular communication and collaboration with physical therapists ensure that patients receive appropriate exercises, therapeutic techniques, and guidance in managing their condition. By working together as a team, healthcare providers can provide comprehensive and effective care to patients with osteoarthritis.
Educating patients on appropriate exercises
While exercise is important, it is essential for patients with osteoarthritis to engage in appropriate exercises that do not exacerbate their symptoms or cause harm. Nurses can educate patients on the importance of starting slowly and gradually increasing the intensity and duration of exercise. They can provide guidance on proper joint alignment and body mechanics during exercises to reduce stress on the affected joints. Additionally, nurses can teach patients specific stretching and strengthening exercises that target the affected joints, promoting joint stability and function. By providing education on appropriate exercises, nurses can empower patients to safely engage in physical activity and optimize their management of osteoarthritis.

Mobility and Assistive Devices
Assessing mobility needs
Assessing the mobility needs of patients with osteoarthritis is essential for developing individualized care plans. Nurses should evaluate the patient’s ability to move around independently and identify any mobility impairments or limitations. This may involve assessing gait, balance, and coordination, as well as assessing the patient’s ability to perform activities such as standing up from a seated position or climbing stairs. By understanding the patient’s mobility needs, nurses can implement appropriate interventions and recommend assistive devices to improve the patient’s overall mobility and independence.
Encouraging use of assistive devices
Assistive devices can play a crucial role in improving the mobility and quality of life for individuals with osteoarthritis. Nurses should educate patients on the availability and benefits of various assistive devices, such as canes, walkers, or orthotic supports. They should encourage patients to use these devices as needed to relieve pain, support joints, and enhance stability. By promoting the use of assistive devices, nurses can help reduce the risk of falls and injuries, while increasing the patient’s mobility and ability to perform daily activities.
Providing education on safe mobility
Safe mobility is essential for individuals with osteoarthritis to minimize pain and prevent further joint damage. Nurses can provide education on safe mobility techniques, such as using correct body mechanics when lifting or carrying objects, and maintaining good posture to reduce stress on the joints. They can also teach patients strategies to avoid falls and injuries, such as clearing walkways of tripping hazards and using handrails or grab bars for support. By providing education on safe mobility, nurses can empower patients to take proactive measures to protect their joints and promote independent movement.
Nutrition and Weight Management
Promoting a balanced diet
A balanced diet plays a crucial role in managing osteoarthritis and promoting overall health. Nurses can support patients with osteoarthritis by promoting a balanced diet that includes a variety of nutrients, such as fruits, vegetables, whole grains, lean proteins, and healthy fats. A diet rich in antioxidants and anti-inflammatory foods can help reduce inflammation and pain associated with osteoarthritis. Nurses can provide education on portion control, meal planning, and healthy cooking techniques to assist patients in making informed dietary choices. By promoting a balanced diet, nurses can support the overall well-being of patients with osteoarthritis.
Assisting patients in weight management
Maintaining a healthy weight is essential for individuals with osteoarthritis, as excess weight places additional stress on the joints and can worsen symptoms. Nurses can assist patients in weight management by providing education on healthy eating habits, portion control, and the importance of regular physical activity. They can also offer support and motivation to help patients set realistic weight loss goals and develop strategies for achieving them. By assisting patients in weight management, nurses can help reduce pain and improve the overall management of osteoarthritis.
Referring patients to a dietitian
For individuals with osteoarthritis, nutrition plays a crucial role in managing symptoms and promoting overall health. Nurses can refer patients to a registered dietitian who specializes in working with patients with chronic conditions, including osteoarthritis. A dietitian can provide individualized dietary recommendations and meal planning guidance to meet the specific needs and preferences of patients. By involving a dietitian in the care team, nurses can ensure that patients receive comprehensive nutrition support to optimize their management of osteoarthritis and improve their overall well-being.

Pain Management Techniques
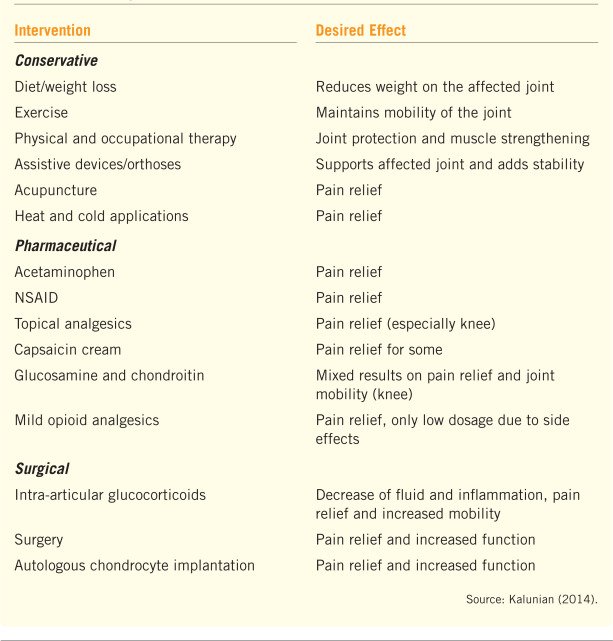
Implementing non-pharmacological pain management strategies
In addition to medication management, non-pharmacological pain management strategies can play a significant role in relieving pain for patients with osteoarthritis. Nurses can implement non-pharmacological interventions, such as heat and cold therapy, transcutaneous electrical nerve stimulation (TENS), and acupuncture. These techniques can help reduce pain, inflammation, and muscle tension. Nurses can also recommend the use of assistive devices, such as braces or splints, to provide joint support and alleviate pain. By implementing non-pharmacological pain management strategies, nurses can offer patients alternative options for pain relief and improve their overall comfort.
Teaching relaxation techniques
Relaxation techniques can be effective in managing pain and promoting overall well-being for individuals with osteoarthritis. Nurses can teach patients various relaxation techniques, such as deep breathing exercises, guided imagery, and progressive muscle relaxation. These techniques can help reduce stress, tension, and anxiety, which may contribute to increased pain levels. By providing education and support in relaxation techniques, nurses can empower patients to actively participate in their own pain management and improve their overall quality of life.
Administering pain medications
In cases where non-pharmacological pain management strategies are not sufficient, medications may be prescribed to provide pain relief for individuals with osteoarthritis. Nurses play a vital role in administering pain medications and monitoring their effectiveness. It is important for nurses to assess the patient’s pain level before administering medication, as well as regularly assess the patient’s response to the medication. Nurses should educate patients on the potential side effects and precautions associated with pain medications and ensure they are well-informed about safe usage. By administering pain medications and monitoring their effects, nurses can help alleviate pain and improve the overall comfort of patients with osteoarthritis.
Joint Protection Strategies
Educating patients on joint protection
Educating patients on joint protection strategies is crucial in managing osteoarthritis and preventing further joint damage. Nurses can provide education on techniques to reduce stress on the joints, such as using ergonomic tools, modifying daily activities, and maintaining proper posture. They can also teach patients to avoid repetitive motions and excessive force on the joints, which can exacerbate symptoms. By educating patients on joint protection strategies, nurses can empower them to take an active role in preserving joint function and minimizing pain.
Demonstrating proper body mechanics
Proper body mechanics are essential for individuals with osteoarthritis to avoid unnecessary strain on the joints and prevent injuries. Nurses can demonstrate and teach patients how to use correct body mechanics during daily activities, such as lifting heavy objects or getting in and out of a car. They can provide guidance on proper joint alignment, the use of assistive devices for support, and the importance of engaging appropriate muscles during movements. By demonstrating proper body mechanics, nurses can help patients reduce joint stress, prevent further damage, and enhance overall mobility and function.
Assisting patients in adapting activities
Adapting activities to accommodate the limitations imposed by osteoarthritis is essential for maintaining independence and quality of life. Nurses can assist patients in identifying modifications or alternative approaches to daily activities that reduce joint stress and pain. This may include recommending the use of assistive devices, suggesting adaptive equipment, or providing strategies for conserving energy and minimizing joint strain. By assisting patients in adapting activities, nurses can promote independence and enable individuals with osteoarthritis to continue engaging in the activities they enjoy.
Psychosocial Support
Assessing emotional well-being
Living with osteoarthritis can have a significant impact on a patient’s emotional well-being. Nurses should be attentive to any signs of anxiety, depression, or emotional distress in patients with osteoarthritis. Assessing emotional well-being involves listening to patients, providing a supportive and non-judgmental environment, and asking open-ended questions to encourage conversation. Nurses can conduct regular assessments to monitor changes in emotional well-being and address any concerns or needs promptly. By assessing emotional well-being, nurses can provide appropriate support and resources to enhance the overall quality of life for individuals with osteoarthritis.
Providing counseling and support
Nurses can provide counseling and support to patients with osteoarthritis to help them cope with the challenges associated with the condition. This may involve active listening, empathy, and validation of the patient’s emotions and experiences. Nurses can offer information and resources to help patients understand and manage their emotions, communicate effectively with family and friends, and develop coping strategies. By providing counseling and support, nurses can help patients navigate the emotional aspects of living with osteoarthritis and promote a sense of well-being.
Referring to mental health professionals
In cases where patients with osteoarthritis require more intensive or specialized mental health support, nurses should be prepared to refer them to mental health professionals. Mental health professionals can provide specific counseling or therapy services to address the emotional and psychological impacts of osteoarthritis on an individual’s well-being. Nurses should be familiar with available resources in their healthcare setting and work collaboratively with mental health professionals to ensure patients receive the appropriate care and support. By referring to mental health professionals, nurses can ensure that individuals with osteoarthritis have access to comprehensive care that addresses their psychological needs.
Preventive Measures
Educating patients on injury prevention
Prevention is key when it comes to managing osteoarthritis and minimizing the risk of further joint damage. Nurses should educate patients on injury prevention strategies to reduce the incidence and severity of joint injuries. This may involve teaching patients proper techniques for lifting heavy objects, avoiding repetitive movements that strain the joints, and using protective equipment during physical activities. By providing education on injury prevention, nurses can empower patients to take proactive steps to protect their joints and prevent exacerbation of their symptoms.
Encouraging regular health screenings
Regular health screenings are essential for individuals with osteoarthritis to monitor their joint health and detect any potential complications. Nurses should encourage patients to schedule regular appointments with their healthcare providers to have their joints assessed and to address any concerns or changes in symptoms. Regular health screenings can help identify any disease progression or development of coexisting conditions that may impact the management of osteoarthritis. By encouraging regular health screenings, nurses can ensure that patients receive appropriate and timely interventions to optimize their overall health and well-being.
Promoting healthy habits
In addition to managing osteoarthritis, promoting healthy habits contributes to overall well-being and can help prevent the development or progression of chronic diseases. Nurses should promote healthy lifestyle habits, such as maintaining a balanced diet, engaging in regular physical activity, getting adequate sleep, and managing stress levels. These habits can help individuals with osteoarthritis manage their symptoms, reduce the risk of comorbid conditions, and improve their overall quality of life. By promoting healthy habits, nurses can empower individuals with osteoarthritis to take control of their health and well-being and prevent further complications.