Are you curious about the latest breakthroughs in understanding and treating brain diseases? Look no further! In this article, we will explore the most recent research discoveries that shed light on the complexities of brain diseases. From the intricate mechanisms of Alzheimer’s to the promising advancements in Parkinson’s treatment, this comprehensive overview will provide you with valuable insights into the cutting-edge developments in the field of neuroscience. So get ready to expand your knowledge and gain a deeper understanding of these debilitating conditions.

Overview of Brain Diseases
Definition and classification of brain diseases
Brain diseases refer to a broad category of medical conditions that affect the structure or function of the brain. These diseases can manifest in various ways, including cognitive impairment, movement disorders, and mental health disturbances. The classification of brain diseases is complex, as it encompasses a wide range of disorders with diverse etiologies and symptoms. Common categories of brain diseases include neurodegenerative diseases (e.g., Alzheimer’s and Parkinson’s disease), cerebrovascular diseases (e.g., stroke), autoimmune disorders (e.g., multiple sclerosis), and epilepsy.
Prevalence and impact of brain diseases
Brain diseases have a significant impact on individuals and society as a whole. They affect people of all ages, leading to impairments in cognitive, motor, and emotional functioning. According to the World Health Organization (WHO), neurological disorders are estimated to affect more than one billion people worldwide, and approximately 6.8 million deaths per year are attributed to brain diseases. The burden of these diseases can be profound, often resulting in decreased quality of life, increased healthcare costs, and the need for long-term care and support.
Risk factors and causes of brain diseases
Brain diseases have multifactorial origins, influenced by a combination of genetic, environmental, and lifestyle factors. While the specific causes vary across different conditions, several risk factors have been identified. Genetic predisposition plays a significant role in some brain diseases, with certain genes increasing an individual’s susceptibility to developing specific disorders. Environmental factors such as exposure to toxins, head injuries, infections, and certain lifestyle choices (e.g., smoking, poor diet) can also contribute to the development of brain diseases. Furthermore, age and family history of brain diseases are important risk factors for various conditions.
Diagnostic Techniques for Brain Diseases
Neuroimaging technologies for brain disease diagnosis
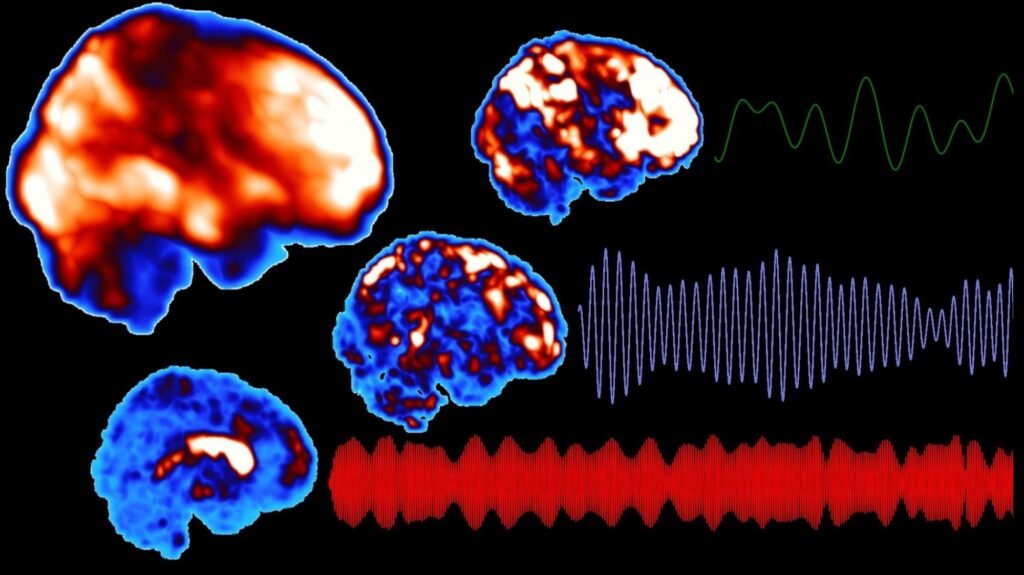
Neuroimaging techniques have revolutionized the diagnosis and understanding of brain diseases. Magnetic resonance imaging (MRI), computed tomography (CT), and positron emission tomography (PET) are commonly used imaging modalities that provide detailed structural and functional information about the brain. MRI can detect abnormalities in brain structure, such as atrophy or tumors, while functional MRI (fMRI) allows the assessment of brain activity during specific tasks. CT scans are useful for identifying acute brain injuries, hemorrhages, or tumors. PET scans provide information about brain metabolism and can help diagnose certain neurodegenerative disorders.
Biomarkers and their role in early detection
Biomarkers are measurable substances or characteristics that indicate the presence or progression of a disease. In the field of brain diseases, biomarkers play a crucial role in early detection and monitoring. For example, in Alzheimer’s disease, biomarkers such as beta-amyloid and tau proteins in cerebrospinal fluid or specific patterns detected by imaging can aid in early diagnosis. Biomarkers are also being explored in other conditions, including Parkinson’s disease, stroke, and multiple sclerosis, to improve diagnostic accuracy and track disease progression.
Genetic testing for inherited brain diseases
Genetic testing has become increasingly important in the diagnosis and management of inherited brain diseases. Advances in genetic sequencing technology have enabled the identification of specific gene mutations associated with conditions like Huntington’s disease and familial forms of Alzheimer’s and Parkinson’s disease. Genetic testing can help determine an individual’s risk of developing these diseases and facilitate genetic counseling, family planning decisions, and potential early interventions or treatment strategies.
Alzheimer’s Disease
Understanding the pathology and progression of Alzheimer’s disease
Alzheimer’s disease is the most common form of dementia and is characterized by the accumulation of plaques (beta-amyloid) and tangles (tau proteins) in the brain. These abnormal protein deposits lead to the loss of neurons and progressive cognitive decline. The precise mechanisms underlying Alzheimer’s disease are still not fully understood, but research indicates that inflammation, oxidative stress, and genetic factors contribute to its development and progression. Early symptoms may include memory loss, confusion, and difficulties with language and problem-solving.
New approaches in early diagnosis and prevention
Early diagnosis of Alzheimer’s disease is crucial for implementing potential interventions and treatments to slow or halt its progression. Researchers are exploring novel diagnostic techniques, such as blood tests, eye exams, and specialized brain imaging, to detect biomarkers or specific brain changes associated with the disease. Identifying individuals at high risk allows for targeted intervention strategies, including lifestyle modifications, cognitive training, and potential future disease-modifying therapies. Moreover, efforts are being made to identify potential preventive measures, such as maintaining a healthy lifestyle, social engagement, and managing cardiovascular risk factors.
Emerging treatments and therapeutic strategies
While there is currently no cure for Alzheimer’s disease, significant progress has been made in developing new treatments and therapeutic approaches. Several drug candidates targeting beta-amyloid and tau pathology are undergoing clinical trials, with the hope of slowing or modifying the disease course. Additionally, research is exploring the potential benefits of anti-inflammatory drugs, antioxidants, and other novel strategies to alleviate symptoms and enhance quality of life for individuals living with Alzheimer’s disease.
Parkinson’s Disease
Characteristics and symptoms of Parkinson’s disease
Parkinson’s disease is a progressive neurodegenerative disorder that primarily affects movement control. It is characterized by the loss of dopamine-producing neurons in a part of the brain called the substantia nigra. The classic motor symptoms of Parkinson’s disease include tremors, bradykinesia (slowness of movement), rigidity, and postural instability. Non-motor symptoms, such as sleep disorders, cognitive impairment, and mood changes, may also be present. The underlying cause of Parkinson’s disease is still not fully understood, but a combination of genetic and environmental factors is thought to contribute to its development.
Advancements in neuroimaging for diagnosis and monitoring
Neuroimaging techniques, such as MRI and PET scans, are valuable tools for assisting in the diagnosis and monitoring of Parkinson’s disease. These imaging methods can help visualize structural changes in the brain and measure dopamine transporter activity, providing objective assessments of disease progression. Recent advancements in functional neuroimaging, such as DaTSCAN, allow for the visualization of dopamine transporter density, aiding in distinguishing Parkinson’s disease from other movement disorders.
Novel therapies and interventions for Parkinson’s disease
In addition to traditional treatments like dopamine replacement therapy, new therapeutic approaches are being explored for Parkinson’s disease. Deep brain stimulation (DBS) is a surgical procedure that involves implanting electrodes in specific brain regions, such as the subthalamic nucleus, to disrupt abnormal neural activity and alleviate motor symptoms. Another area of research involves targeted drug delivery methods, including the use of nanoparticles, to enhance the delivery of medications to the affected brain regions. Furthermore, stem cell therapy shows promise in restoring dopamine-producing neurons and potentially halting disease progression.
Stroke
Types of strokes and their effects on the brain
Stroke occurs when blood flow to the brain is interrupted, leading to the death of brain cells. There are two main types of stroke: ischemic stroke, caused by a blockage in a blood vessel supplying the brain, and hemorrhagic stroke, resulting from the rupture of a blood vessel. Depending on the location and extent of the damage, a stroke can have various effects, such as paralysis, difficulties with speech or swallowing, cognitive impairment, or emotional changes. Rehabilitation and recovery after stroke play a vital role in optimizing functional outcomes and restoring independence.
Breakthroughs in acute stroke management
Advancements in acute stroke management have significantly improved outcomes for stroke patients. The development of clot-busting medications, known as thrombolytics, allows for the restoration of blood flow in ischemic strokes. Additionally, endovascular clot retrieval procedures (mechanical thrombectomy) have revolutionized the treatment of large vessel occlusions, leading to better functional outcomes. Timely recognition of stroke symptoms is crucial for prompt medical intervention, as delays in treatment can result in permanent brain damage.
Rehabilitation and recovery after stroke
Rehabilitation is a vital component of stroke care, aimed at promoting recovery and optimizing functional abilities. Physical therapy, occupational therapy, and speech therapy are common interventions used to address various impairments caused by stroke. These therapies focus on improving motor control, restoring communication skills, and facilitating activities of daily living. Innovative approaches, such as virtual reality and robotics, are being incorporated into stroke rehabilitation to enhance engagement, intensity, and efficacy of therapy. Stroke support groups and caregiver education programs play a crucial role in assisting survivors and their families during the recovery process.
Multiple Sclerosis
Understanding the immune system’s role in multiple sclerosis
Multiple sclerosis (MS) is an autoimmune disorder characterized by the immune system mistakenly attacking the protective covering of nerve fibers (myelin) in the central nervous system. This immune-mediated damage disrupts the transmission of electrical signals between the brain and the rest of the body, leading to a wide range of symptoms. The exact cause of MS is unknown, but it is thought to involve a combination of genetic and environmental factors, as well as dysregulation of the immune system. Research has shown that certain immune cells, such as T-cells and B-cells, play a significant role in the pathogenesis of MS.
Early detection and personalized treatment strategies
Early detection and diagnosis of MS are crucial for initiating appropriate treatment strategies to manage the disease effectively. Advances in neuroimaging techniques, such as MRI, have enabled the identification of characteristic brain lesions and patterns of disease activity. In addition to imaging, cerebrospinal fluid analysis and blood tests can help confirm the diagnosis and assess immune markers associated with MS. Personalized treatment approaches, including the use of disease-modifying therapies (DMTs), aim to modify the course of the disease, reduce relapses, and slow down disability progression. The selection of DMTs is based on various factors, such as the subtype of MS, disease activity, and individual patient characteristics.
Promising research on neuroprotective therapies
In addition to managing disease activity, there is ongoing research focused on developing neuroprotective therapies for MS. The goal of these treatments is to preserve and repair damaged nerve fibers, ultimately preventing further disability. Potential approaches include the promotion of remyelination, the inhibition of inflammation, and the enhancement of neuronal survival and function. Various potential neuroprotective agents, such as biologics, small molecules, and stem cells, are being investigated in preclinical and clinical studies. Promising findings from these studies offer hope for future interventions that can address the underlying mechanisms of MS and potentially restore lost neurological function.
Epilepsy
Causes and triggers of epilepsy
Epilepsy is a neurological disorder characterized by recurrent seizures, resulting from abnormal electrical activity in the brain. There are numerous causes and triggers of epilepsy, including genetic factors, brain injuries, infections, developmental abnormalities, and certain metabolic conditions. In some cases, the underlying cause of epilepsy may be unknown. Seizure triggers can vary among individuals but may include sleep deprivation, stress, medications, alcohol or drug use, and hormonal changes. Identifying and managing these triggers are key components in epilepsy management.
Advancements in seizure prediction and control
Advancements in technology and understanding of brain activity have led to significant progress in the prediction and control of seizures. Electroencephalography (EEG) remains a fundamental tool for recording and analyzing brain wave patterns associated with seizures. Portable EEG devices and wearable technologies allow for continuous monitoring in various settings, aiding in the identification of preictal (before seizures) and ictal (during seizures) patterns. Additionally, implantable devices and responsive neurostimulation systems, such as vagus nerve stimulation (VNS) and deep brain stimulation (DBS), offer potential options for seizure control in individuals with drug-resistant epilepsy.
Innovations in surgical options for epilepsy treatment
For individuals with drug-resistant epilepsy, surgical intervention may be an option to improve seizure control and quality of life. Advances in neuroimaging, such as high-resolution MRI and functional mapping techniques, aid in the precise localization of seizure foci and critical brain regions. Epilepsy surgery can involve removing the seizure focus, disconnecting abnormal brain circuits, or implanting devices to modulate brain activity. Minimally invasive procedures, such as laser interstitial thermal therapy (LITT), offer potential benefits in terms of shorter hospital stays, reduced postoperative complications, and quicker recovery. As surgical techniques continue to evolve, the prospects for successful epilepsy treatment and improved outcomes continue to expand.
Huntington’s Disease
Genetic basis and inheritance patterns of Huntington’s disease
Huntington’s disease (HD) is an inherited neurodegenerative disorder caused by a mutation in the huntingtin gene. The mutation disrupts the normal functioning of brain cells, leading to the progressive degeneration of neurons in various regions of the brain. HD follows an autosomal dominant inheritance pattern, which means that an affected individual has a 50% chance of passing the mutated gene to each of their children. The severity and age of onset can vary among individuals, with symptoms typically appearing in mid-adulthood. Genetic testing can provide important information regarding an individual’s risk of developing HD.
Supportive care and management of symptoms
Huntington’s disease is a complex condition that requires a multidisciplinary approach to care management. While there is no cure for HD, supportive measures aim to address the wide range of physical, cognitive, and psychiatric symptoms associated with the disease. Physical therapy and occupational therapy can help maintain mobility and independence, while speech therapy may address communication difficulties. Medications and psychotherapy techniques can assist in managing psychiatric symptoms, including depression, anxiety, and irritability. Palliative care and end-of-life support are also essential components in the management of advanced stages of HD, focusing on symptom relief and improving quality of life.
Gene therapy and targeted treatments in development
Recent advancements in gene therapy have opened up new possibilities for the treatment of Huntington’s disease. Gene silencing techniques, such as antisense oligonucleotides (ASOs) and RNA interference (RNAi), target the mutated huntingtin gene to reduce the production of harmful proteins associated with the disease. Clinical trials testing these therapeutic approaches have shown promising results in animal models and early-stage human trials. Additionally, researchers are exploring strategies to enhance neuroprotection, promote cellular repair, and improve symptom management. While gene-based therapies are still in the early stages of development, they hold great potential for modifying the course of Huntington’s disease and improving outcomes for affected individuals.
Amyotrophic Lateral Sclerosis (ALS)
Understanding the motor neuron degeneration process in ALS
Amyotrophic Lateral Sclerosis (ALS), also known as Lou Gehrig’s disease, is a progressive neurodegenerative disorder that primarily affects the nerve cells responsible for controlling voluntary muscle movement (motor neurons). The exact cause of ALS is not fully understood, but a combination of genetic and environmental factors is thought to contribute to its development. Motor neuron degeneration results in muscle weakness, eventually leading to paralysis and respiratory failure. Researchers are actively investigating cellular and molecular mechanisms involved in ALS, including protein misfolding and aggregation, oxidative stress, and impaired cellular waste disposal systems.
Potential biomarkers for early diagnosis and disease monitoring
Early diagnosis of ALS remains challenging, as the disease often presents with subtle symptoms that mimic other conditions. Biomarkers are being studied as potential diagnostic tools to aid in the early detection and monitoring of ALS. Biomarkers may include abnormalities in cerebrospinal fluid composition, blood markers, or neurophysiological changes detected by electrophysiological tests. Identification of reliable biomarkers would allow for earlier interventions and the monitoring of disease progression, potentially improving clinical trial outcomes and therapeutic management strategies for ALS.
Exploring novel therapeutic approaches for ALS
While there is currently no cure for ALS, research efforts continue to explore novel therapeutic approaches to slow the disease progression and improve quality of life for affected individuals. Several potential therapeutic targets are being investigated, including neuroprotective strategies, anti-inflammatory agents, neurotrophic factors, and gene-based therapies. Stem cell therapy holds promise as a potential treatment option by replacing damaged motor neurons and supporting neuroregeneration. Additionally, advancements in assistive technologies, such as brain-computer interfaces and robotics, offer new avenues for enhancing communication and mobility in individuals with advanced ALS.
Mental Health Disorders
The connection between brain and mental health
Mental health disorders, such as major depressive disorder, anxiety disorders, and schizophrenia, are associated with abnormalities in brain structure, functionality, and neurotransmitter systems. Neuroscience research has provided valuable insights into the complex interplay between genetic, environmental, and neurobiological factors underlying these conditions. Imbalances in neurotransmitters, altered brain circuitry, and dysregulation of the stress response have been implicated in the pathogenesis of various mental health disorders. Understanding the biological basis of mental health conditions can inform the development of targeted interventions and personalized treatment approaches.
Neurobiology of major depressive disorder
Major depressive disorder (MDD) is a prevalent mental health condition characterized by persistent feelings of sadness, loss of interest or pleasure, disturbances in sleep and appetite, and impaired concentration. Neurobiology studies have revealed changes in brain regions involved in emotion regulation and reward processing in individuals with MDD. Dysfunctions in the neurotransmitter systems, particularly serotonin, norepinephrine, and dopamine, play a critical role in the pathophysiology of MDD. Antidepressant medications work by modulating these neurotransmitter systems, aiming to restore balance and alleviate depressive symptoms. However, ongoing research is focused on identifying novel targets and treatment strategies to improve treatment response rates and address treatment-resistant depression.
Advancements in addressing anxiety disorders and schizophrenia
Anxiety disorders and schizophrenia are complex mental health conditions associated with significant impairments in cognitive, emotional, and social functioning. Research on anxiety disorders has highlighted alterations in brain regions involved in fear processing, such as the amygdala and prefrontal cortex. Antianxiety medications and psychotherapy techniques, including cognitive-behavioral therapy (CBT), have shown efficacy in managing anxiety symptoms. In the case of schizophrenia, studies have identified abnormalities in various brain regions, neurotransmitter systems (particularly dopamine), and synaptic connectivity. Antipsychotic medications and psychosocial interventions play crucial roles in reducing symptom severity and improving overall functioning in individuals with schizophrenia. Ongoing research aims to develop more precise therapeutic interventions, minimize side effects, and individualize treatment plans based on neurobiological profiles.
In conclusion, brain diseases encompass a wide range of conditions that have significant impacts on individuals and society. Advances in diagnostic techniques, such as neuroimaging and biomarkers, have improved early detection and monitoring of these diseases. Understanding the underlying causes, risk factors, and pathological processes is crucial for the development of effective treatments and interventions. Ongoing research efforts continue to uncover promising therapeutic strategies and targeted approaches for brain diseases, with the ultimate goal of improving outcomes and enhancing the quality of life for individuals affected by these conditions.

