Living with Allergic Rhinitis can be quite the challenge, as anyone who has experienced the constant sneezing, itchy eyes, and nasal congestion knows all too well. This article explores the realities of living with this common condition, offering helpful tips and insights on managing symptoms, seeking proper treatment, and finding support. From understanding triggers to adopting lifestyle changes, you’ll gain valuable knowledge to navigate your daily life with Allergic Rhinitis and find ways to alleviate the discomfort it brings.
What is Allergic Rhinitis?
Allergic Rhinitis, also known as hay fever, is a common condition that affects many individuals worldwide. It is an allergic reaction that occurs when an individual’s immune system overreacts to certain substances, known as allergens, in the environment. These allergens can be found both indoors and outdoors, and they trigger symptoms such as sneezing, itching, nasal congestion, and a runny nose. Allergic Rhinitis can significantly impact one’s quality of life, but with proper management and treatment, individuals can find relief from their symptoms and live a more comfortable life.
Definition of Allergic Rhinitis
Allergic Rhinitis is an inflammation of the nasal passages that occurs when an individual is exposed to allergens. The immune system mistakenly identifies these allergens as harmful and releases chemicals, such as histamine, to fight against them. These chemicals cause symptoms such as nasal congestion, itching, sneezing, and a runny nose. Allergic Rhinitis can be classified into two types: seasonal and perennial.
Types of Allergic Rhinitis
-
Seasonal Allergic Rhinitis: This type of allergic rhinitis occurs during specific seasons when certain allergens are in high concentration in the environment. It is commonly known as hay fever and is usually triggered by allergens such as tree pollen, grass pollen, or weed pollen. The symptoms of seasonal allergic rhinitis tend to vary depending on the season and can be experienced for weeks or months.
-
Perennial Allergic Rhinitis: Perennial allergic rhinitis is a year-round condition that occurs due to exposure to allergens that are present indoors, such as dust mites, pet dander, mold, or cockroach debris. Unlike seasonal allergic rhinitis, the symptoms of perennial allergic rhinitis persist throughout the year and are not limited to specific seasons.
Causes and Triggers of Allergic Rhinitis
Allergic Rhinitis is caused by an allergic response to certain substances in the environment, known as allergens. These allergens can be divided into different categories, including airborne allergens, indoor allergens, seasonal triggers, and environmental factors.
Airborne Allergens
Airborne allergens are substances that float in the air and can easily be inhaled. Common airborne allergens include pollen from trees, grasses, and weeds, as well as spores from fungi and molds. When individuals with allergic rhinitis come into contact with these allergens, their immune system releases histamine and other chemicals, leading to the characteristic symptoms of allergic rhinitis.
Indoor Allergens
Indoor allergens are substances found inside buildings and homes, and they can trigger allergic rhinitis symptoms. Common indoor allergens include dust mites, pet dander, mold, cockroach debris, and certain chemicals present in cleaning products or tobacco smoke. These allergens can be present throughout the year and pose a challenge, especially for individuals with perennial allergic rhinitis.
Seasonal Triggers
Seasonal triggers are allergens that are prevalent during specific seasons. These allergens are typically outdoor allergens and include tree pollen, grass pollen, and weed pollen. Seasonal allergic rhinitis is often referred to as hay fever, as these allergens are common during hay-cutting season. The concentration of pollen in the air can vary depending on the weather and geographical location, causing symptoms that coincide with different seasons.
Environmental Factors
Various environmental factors can contribute to the development or exacerbation of allergic rhinitis symptoms. These factors include pollution, smoke, strong odors, changes in weather, and high humidity levels. While these factors may not directly cause allergic rhinitis, they can increase the sensitivity of the nasal passages, making individuals more susceptible to allergens and leading to the worsening of symptoms.

Symptoms of Allergic Rhinitis
Allergic Rhinitis can manifest with a wide range of symptoms that can vary in severity from person to person. These symptoms can be categorized into nasal symptoms, ocular symptoms, other systemic symptoms, and their impact on an individual’s quality of life.
Nasal Symptoms
- Sneezing: Individuals with allergic rhinitis often experience frequent and repetitive bouts of sneezing. This is one of the earliest and most common symptoms of the condition.
- Nasal Congestion: Allergic rhinitis can lead to a feeling of nasal congestion or blockage. This can make it difficult to breathe through the nose and may result in a stuffy or “blocked” sensation.
- Runny Nose: A runny nose, medically known as rhinorrhea, is a classic symptom of allergic rhinitis. It is characterized by the production of excessive clear or watery nasal discharge.
- Itching: Itching is a common symptom of allergic rhinitis and can be felt inside the nose or on the roof of the mouth. It may also extend to the ears and throat.
Ocular Symptoms
- Itchy, Red, and Watery Eyes: Allergic rhinitis often affects the eyes, leading to itching, redness, and excessive tearing. These symptoms can be bothersome and may significantly impact visual comfort.
Other Systemic Symptoms
In addition to the nasal and ocular symptoms, allergic rhinitis can sometimes cause other systemic symptoms. These symptoms may include fatigue, coughing, throat irritation, headaches, and impaired sense of smell.
Impact on Quality of Life
Allergic rhinitis can have a significant impact on an individual’s quality of life. Chronic nasal congestion and other symptoms can disrupt sleep, leading to daytime fatigue and reduced productivity. Allergic rhinitis can also interfere with social activities, work performance, and overall well-being. It is essential to recognize the impact of allergic rhinitis on quality of life and take appropriate measures to manage and alleviate symptoms.
Diagnosis of Allergic Rhinitis
Diagnosing allergic rhinitis involves a combination of medical history evaluation, physical examination, and allergy tests. This comprehensive approach aims to identify the specific allergens causing the symptoms and help guide treatment decisions.
Medical History and Physical Examination
During the medical history evaluation, the healthcare provider will ask about specific symptoms, their duration and frequency, any triggers or patterns observed, and the impact of symptoms on daily life. This information helps in identifying potential allergens and distinguishing allergic rhinitis from other conditions.
A physical examination may be performed to assess the nasal passages, eyes, throat, and ears. The healthcare provider will look for signs of nasal congestion, redness, swelling, and other characteristic findings associated with allergic rhinitis.
Allergy Tests
Allergy tests are commonly used to determine the specific allergens that trigger allergic rhinitis symptoms. These tests can include skin prick tests, blood tests, or patch tests. Skin prick tests involve placing small amounts of allergens on the skin and then pricking or scratching the skin to allow the allergens to enter. If an individual is allergic to a specific allergen, an allergic reaction, such as redness or swelling, will occur at the site.
Blood tests, such as the specific IgE test, measure the levels of allergy-related antibodies in the blood. This test can help identify the specific allergens to which an individual is sensitized.
Patch tests are used to identify contact allergens that may be causing symptoms in individuals with allergic rhinitis. These tests involve applying allergens to patches that are then placed on the skin for a specific duration.
Differential Diagnosis
In some cases, the symptoms of allergic rhinitis may overlap with those of other respiratory conditions, such as the common cold, sinusitis, or non-allergic rhinitis. It is essential for healthcare providers to perform a thorough evaluation to rule out other possible causes of symptoms and make an accurate diagnosis.

Treatment Options for Allergic Rhinitis
Treatment options for allergic rhinitis aim to alleviate symptoms, reduce inflammation, and improve the individual’s quality of life. The choice of treatment will depend on the severity of symptoms, the presence of co-existing conditions, and individual preferences.
Allergen Avoidance
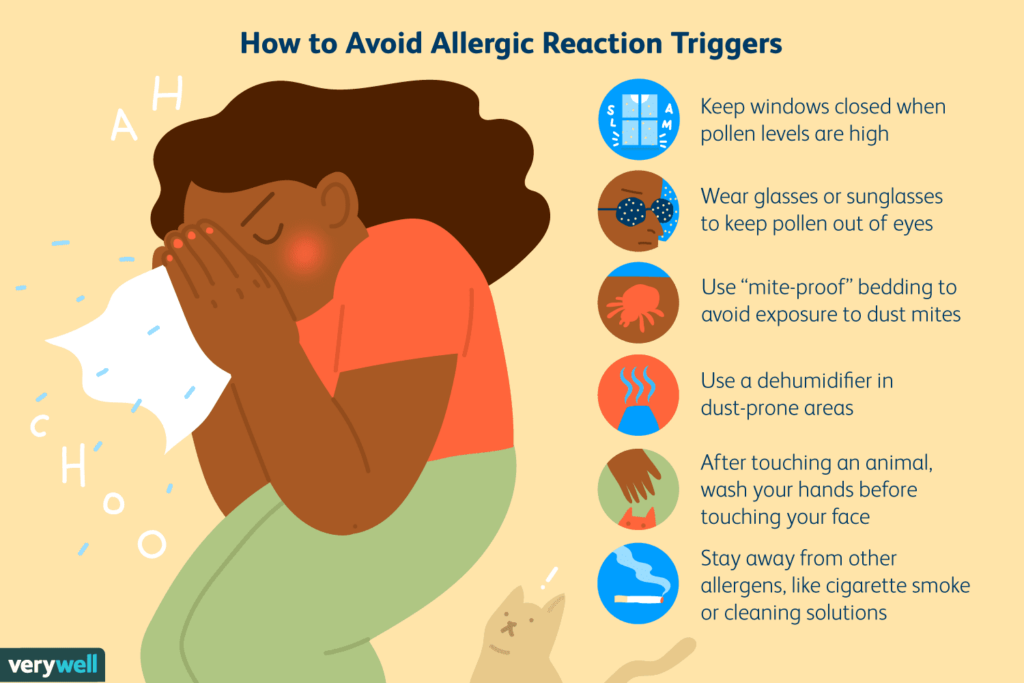
One of the primary strategies for managing allergic rhinitis is to avoid or minimize exposure to allergens. This can involve implementing measures such as:
- Keeping windows closed during high pollen seasons
- Using air purifiers or filters to reduce indoor allergens
- Cleaning surfaces regularly to remove dust mites
- Removing carpets or rugs that may harbor allergens
- Avoiding exposure to smoke or strong odors
- Limiting outdoor activities during peak pollen times
Medications
Medications are often used to control the symptoms of allergic rhinitis. The choice of medication may depend on the severity of symptoms and whether they are persistent or intermittent. Commonly used medications include:
- Antihistamines: These medications block histamine, a chemical released during an allergic reaction, and help relieve symptoms such as sneezing, itching, and a runny nose.
- Decongestants: Decongestants can help alleviate nasal congestion by narrowing blood vessels in the nasal passages. They provide temporary relief but should not be used for an extended period due to the risk of rebound congestion.
- Nasal Steroids: Nasal corticosteroids are anti-inflammatory medications that reduce swelling, congestion, and itching in the nasal passages. They are effective in managing both nasal and ocular symptoms and can be used long-term.
- Leukotriene Receptor Antagonists: These medications block the action of leukotrienes, which are substances involved in the allergic response. They can help control symptoms, particularly in individuals with associated conditions such as asthma.
- Nasal Cromolyn: Nasal cromolyn is a medication that stabilizes mast cells, preventing the release of histamine and other chemicals. It is available as a nasal spray and can be used as a preventative measure.
Immunotherapy
For individuals with severe or persistent allergic rhinitis, immunotherapy may be considered. Immunotherapy, also known as allergy shots, involves regular injections of small amounts of allergens under the skin. The aim is to desensitize the immune system and reduce the severity of allergic reactions over time. Immunotherapy is generally recommended for individuals with specific allergens that cannot be easily avoided and who have not responded well to other treatments.
Complementary and Alternative Medicine
Complementary and alternative medicine approaches, such as acupuncture and herbal remedies, may be considered by some individuals with allergic rhinitis. While the evidence supporting the effectiveness of these approaches is limited, some individuals report symptom improvement with these treatments. It is important to consult with a healthcare provider before initiating any complementary or alternative treatments and to use them as adjuncts to conventional medical therapies.
Managing Allergic Rhinitis at Home
In addition to medical treatments, there are several steps individuals with allergic rhinitis can take to manage their symptoms and reduce exposure to allergens in their home environment.
Creating an Allergen-Free Environment
- Keep windows closed during high pollen seasons to prevent pollen from entering the house.
- Use air purifiers or filters to remove allergens from the air.
- Vacuum carpets and upholstery regularly to reduce dust mites.
- Wash bedding frequently in hot water to kill dust mites.
- Keep pets out of bedrooms and off furniture, as their dander can trigger symptoms.
- Use hypoallergenic pillowcases and mattress covers to reduce exposure to allergens.
Nasal Irrigation
Nasal irrigation, also known as nasal rinsing or nasal douche, can help flush out allergens and mucus from the nasal passages. This can provide temporary relief from congestion and post-nasal drip. Nasal irrigation can be done using a neti pot, bulb syringe, or nasal irrigation kits available in pharmacies.
Preventing Outdoor Exposure
- Check pollen forecasts to be aware of high pollen days and limit outdoor activities during these times.
- Wear sunglasses to protect the eyes from pollen and other allergens.
- When returning from outdoor activities, change clothes and shower to remove any allergens that may have collected on the body or hair.
Maintaining a Healthy Lifestyle
- Eating a balanced diet that includes fruits, vegetables, and whole grains can help support overall immune health.
- Regular exercise and physical activity can help improve lung function and reduce the severity of allergic rhinitis symptoms.
- Avoiding tobacco smoke and secondhand smoke is crucial, as smoke can aggravate allergic rhinitis symptoms.

Allergic Rhinitis and Children
Allergic rhinitis is not limited to adults and can occur in children as well. It is estimated that approximately 10-40% of children worldwide are affected by allergic rhinitis. Managing allergic rhinitis in children requires special considerations and involves a collaborative approach between parents, healthcare providers, and school personnel.
Prevalence in Children
The prevalence of allergic rhinitis in children varies depending on various factors, including geographical location, genetic predisposition, and exposure to allergens. Children with a family history of allergies, such as asthma or allergic rhinitis, are at a higher risk of developing the condition.
Tips for Parents
- Work closely with your child’s healthcare provider to develop an appropriate treatment plan for managing their allergic rhinitis symptoms.
- Educate your child about their condition and how to avoid triggers or allergens that may worsen their symptoms.
- Encourage your child to wash their hands regularly to minimize exposure to allergens and reduce the risk of illness.
Managing Symptoms in School
It is essential to communicate with your child’s school personnel about their allergic rhinitis and any specific triggers that may affect them. Consider providing the school with written instructions from your child’s healthcare provider regarding medication administration and emergency management plans. Encourage your child to carry necessary medications, such as antihistamines or nasal sprays, with them at school, under the guidance of healthcare providers and school policies.
Allergic Rhinitis and Pregnancy
Pregnancy is a unique period in a woman’s life, and managing allergic rhinitis during pregnancy requires special considerations to ensure the safety of both the mother and the unborn child.
Effects on Pregnancy
Allergic rhinitis itself does not directly impact pregnancy outcomes, but the symptoms can be bothersome and affect the overall well-being of pregnant individuals. Nasal congestion and sleep disturbances associated with allergic rhinitis can lead to discomfort and fatigue, making it important to manage symptoms effectively.
Safe Treatment Options
It is crucial to consult with healthcare professionals before using any medications during pregnancy. Many common medications used to treat allergic rhinitis, such as antihistamines and nasal steroids, are considered safe during pregnancy under the guidance of healthcare providers. It is important to weigh the potential benefits against any potential risks to the mother or the baby.
Non-pharmacological approaches, such as nasal irrigation, saline nasal sprays, and avoiding allergens, can also be beneficial during pregnancy. These approaches can help alleviate symptoms and minimize the need for medication.
Consulting with Healthcare Professionals
During pregnancy, it is essential for individuals with allergic rhinitis to communicate openly with their healthcare providers regarding the management of their symptoms. Regular prenatal visits provide an opportunity to discuss any concerns, review medications, and ensure the well-being of both the mother and the baby.

Complications and Long-Term Effects
Allergic rhinitis, if left untreated or poorly managed, can lead to various complications and long-term effects. It is important to address the condition effectively to reduce the risk of complications and improve the overall quality of life.
Sinusitis
One common complication of allergic rhinitis is sinusitis, which is an inflammation or infection of the sinuses. Sinusitis can occur when the nasal passages are blocked due to excessive mucus production and congestion. Symptoms of sinusitis include facial pain or pressure, headache, nasal discharge, and a reduced sense of smell.
Middle Ear Infections
Allergic rhinitis can increase the risk of middle ear infections, also known as otitis media. The congestion and inflammation associated with allergic rhinitis can interfere with the normal drainage of the Eustachian tubes, leading to the accumulation of fluid in the middle ear. This creates an ideal environment for bacterial or viral infections to develop.
Asthma
There is a strong link between allergic rhinitis and asthma. Many individuals with allergic rhinitis also have asthma, and both conditions often share similar triggers. The presence of allergic rhinitis can worsen asthma symptoms and increase the risk of asthma attacks. Effective management of allergic rhinitis is crucial in preventing the progression or worsening of asthma.
Impact on Sleep
Nasal congestion and other symptoms of allergic rhinitis can significantly impact sleep quality. The resulting sleep disturbances can lead to fatigue, daytime sleepiness, and impaired cognitive function. Addressing allergic rhinitis symptoms can help improve sleep and overall well-being.
Tips for Traveling with Allergic Rhinitis
Traveling with allergic rhinitis requires some preparation to minimize exposure to allergens and manage symptoms effectively. By taking a few simple steps, individuals with allergic rhinitis can enjoy their travels while minimizing the impact of allergens.
Researching Destination Allergens
Before traveling, it is helpful to research the allergens that may be present at the chosen destination. Different regions and seasons can have varying levels of pollen, mold, or dust mites that may trigger allergic rhinitis symptoms. Obtaining this information in advance can help individuals plan their trip and take appropriate measures to minimize exposure.
Packing Essentials
Packing essential items can help individuals manage their allergic rhinitis symptoms while away from home. These items may include:
- Medications: Ensure an adequate supply of prescribed medications, such as antihistamines or nasal sprays.
- Allergy-Relief Products: Consider packing hypoallergenic bedding covers, hypoallergenic travel pillows, and eye drops to alleviate ocular symptoms.
- Nasal Irrigation Kit: Having a portable nasal irrigation kit can help individuals flush out allergens and maintain nasal hygiene while on the go.
- Portable Air Purifiers: Consider using portable air purifiers in hotel rooms or other accommodations to reduce exposure to indoor allergens.
Dealing with Allergies during the Trip
While traveling, implementing strategies to minimize exposure to allergens can help manage allergic rhinitis symptoms. These strategies may include:
- Keeping car windows closed and using air conditioning while driving to reduce exposure to outdoor allergens.
- Choosing accommodations with hypoallergenic bedding and smoke-free environments.
- Cleaning the hotel room or accommodation thoroughly to remove dust or allergens that may be present.
- Carrying a small travel-sized HEPA air purifier to reduce allergens in the hotel room.
By being prepared and taking appropriate precautions, individuals with allergic rhinitis can enjoy their travel experiences while minimizing the impact of allergens on their symptoms.
In conclusion, allergic rhinitis is a common condition characterized by an allergic response to certain substances in the environment. It can significantly impact an individual’s quality of life, but with proper management and treatment, individuals can find relief from their symptoms and live more comfortably. By understanding the causes and triggers, recognizing the symptoms, seeking a proper diagnosis, and following appropriate treatment options, individuals can effectively manage their allergic rhinitis and minimize the impact it has on their daily life. It is crucial to work with healthcare professionals, take proactive steps to manage symptoms at home and during travel, and make necessary lifestyle modifications to promote overall well-being. Remember, with the right approach, living with allergic rhinitis can be manageable and allow individuals to thrive in their daily lives.
