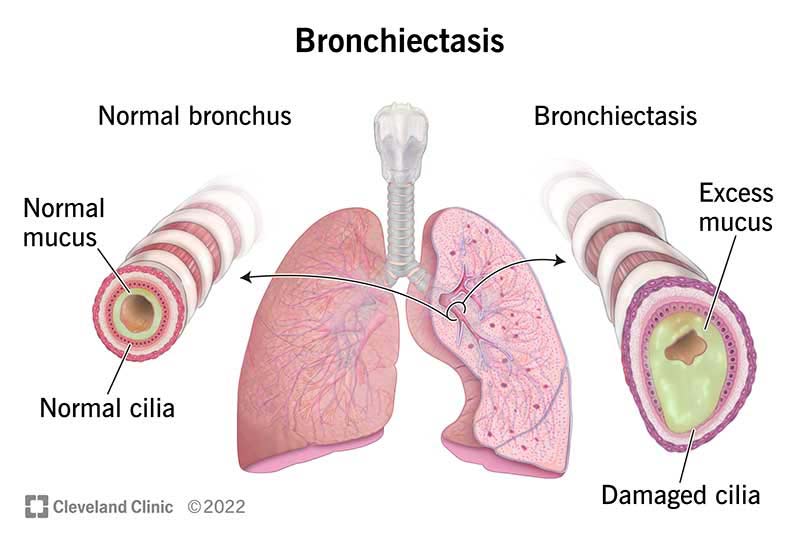
Living with bronchiectasis can be challenging, but with the right tips and strategies, you can effectively manage this condition and improve your quality of life. This article will provide you with valuable insights and practical advice on how to navigate the daily challenges and symptoms associated with bronchiectasis. From understanding the condition to implementing self-care practices and seeking support, you will discover a wealth of information to help you thrive in your journey with bronchiectasis.

Diagnosis of Bronchiectasis
Symptoms to look out for
If you are experiencing persistent symptoms such as a chronic cough, excessive production of sputum or phlegm, recurrent respiratory infections, shortness of breath, and fatigue, it is important to pay attention to these signs as they may indicate bronchiectasis. Other possible symptoms include wheezing, chest pain, and weight loss. It is crucial to be aware of these manifestations and consult a healthcare professional if you notice any of them persisting or worsening.
Medical tests and procedures for diagnosis
Confirming a diagnosis of bronchiectasis typically involves a series of medical tests and procedures. These may include:
-
Chest X-rays: This imaging technique allows healthcare providers to evaluate the structure of your lungs and identify any abnormalities.
-
High-resolution computed tomography (HRCT) scan: HRCT scans offer a detailed view of your lungs, enabling healthcare professionals to detect bronchiectasis and assess its severity.
-
Sputum culture: Collecting a sample of your sputum can help identify the presence of any bacterial infections, which are often associated with bronchiectasis.
-
Pulmonary function tests: These tests measure how well your lungs are functioning, assessing factors such as airflow, lung capacity, and gas exchange.
-
Bronchoscopy: In some cases, a bronchoscopy may be performed to examine the air passages within your lungs more closely. This procedure involves inserting a thin, flexible tube called a bronchoscope through your nose or mouth and into your lungs.
-
Genetic testing: In rare instances, genetic testing may be recommended to determine if there are any underlying genetic factors contributing to the development of bronchiectasis.
It is important to follow the advice and recommendations of your healthcare provider to ensure an accurate diagnosis.
Treatment Options
Pharmacological treatment
Pharmacological treatment is a key component in managing bronchiectasis. Your healthcare provider may prescribe various medications to alleviate symptoms, reduce inflammation, and prevent exacerbations. These may include:
-
Bronchodilators: These medications help to open up your airways, making it easier to breathe. They are often used to relieve symptoms of bronchiectasis, such as wheezing and shortness of breath.
-
Mucolytics: Mucolytic medications are designed to thin and loosen the mucus in your airways, making it easier to cough up and clear. This can help reduce the frequency and severity of cough and chest congestion.
-
Antibiotics: Antibiotics are commonly prescribed to treat bacterial infections associated with bronchiectasis. They can help control existing infections and prevent new ones from developing.
-
Inhaled corticosteroids: Inhaled corticosteroids are often used to manage airway inflammation in individuals with bronchiectasis. They help reduce swelling and mucus production, thereby improving respiratory function.
It is important to take medications as prescribed, adhere to the recommended dosage and frequency, and communicate with your healthcare provider regarding any concerns or side effects you may experience.
Pulmonary rehabilitation
Pulmonary rehabilitation is a comprehensive program that combines exercise training, breathing techniques, education, and emotional support to improve the overall quality of life for individuals with bronchiectasis. It aims to enhance physical fitness, maximize lung function, and teach self-management strategies for better disease control.
Pulmonary rehabilitation programs are typically conducted under the guidance of healthcare professionals, such as respiratory therapists or physiotherapists. These programs may include:
- Individualized exercise plans tailored to your specific needs and abilities.
- Breathing exercises to improve lung capacity and strengthen respiratory muscles.
- Education on bronchiectasis management, including medication management and infection prevention.
- Psychological support and counseling to address the emotional and psychological impact of living with a chronic lung condition.
Participating in pulmonary rehabilitation can empower you with knowledge and skills to effectively manage your bronchiectasis and lead a healthier, more active life.
Surgical interventions
In some cases, surgical intervention may be considered for individuals with severe bronchiectasis or certain complications. The specific surgical procedures will depend on the location and extent of the bronchiectasis, as well as individual factors.
Surgical options may include:
-
Lung resection: This procedure involves removing the affected part of the damaged lung, which may be necessary if the bronchiectasis is limited to a certain area.
-
Lung transplantation: In severe cases where bronchiectasis has significantly compromised lung function, a lung transplantation may be considered as a viable option.
Surgical interventions are typically reserved for individuals who have not achieved adequate symptom relief and disease control through other treatment approaches. Your healthcare provider will assess your condition and discuss the potential benefits and risks of surgery with you.
Medication Management
Understanding the prescribed medications
Understanding the medications prescribed for bronchiectasis is essential for effective management. Your healthcare provider will explain the purpose, benefits, and potential side effects of each medication. It is important to ask questions and seek clarification to ensure you have a clear understanding of how each medication works and how it should be taken.
Some common medications prescribed for bronchiectasis include bronchodilators, mucolytics, antibiotics, and inhaled corticosteroids. Each medication serves a specific purpose in managing symptoms, reducing inflammation, controlling infections, or improving respiratory function. By understanding the roles of these medications, you can take them correctly and maximize their effectiveness.
Proper administration techniques
In addition to understanding the medications, it is important to learn and practice proper administration techniques. This ensures that you are getting the full benefits of the medications and avoids any potential complications. Here are some key points to keep in mind:
-
Inhalers: If you are prescribed an inhaler, such as a bronchodilator or inhaled corticosteroid, it is crucial to use the correct technique to ensure the medication reaches your lungs. This involves taking slow, deep breaths and coordinating your inhalation with the activation of the inhaler.
-
Mucolytics: Mucolytics are available in various forms, such as tablets or liquid solutions. Follow the instructions provided by your healthcare provider or pharmacist regarding the correct dosage, frequency, and administration method. Some mucolytics may need to be dissolved in water before ingestion, while others can be taken directly.
-
Antibiotics: Antibiotics may be prescribed for short-term or long-term use, depending on the presence of bacterial infections. It is important to take the full course of antibiotics as directed, even if symptoms improve before completing the treatment. This helps ensure that the infection is fully eradicated, reducing the risk of recurrent infections and antibiotic resistance.
Proper administration techniques can significantly improve the effectiveness of the medications, promoting optimal symptom control and disease management.
Managing side effects
While medications play a crucial role in managing bronchiectasis, they may also come with potential side effects. It is important to be aware of these side effects and communicate any concerns or adverse reactions to your healthcare provider.
Common side effects of medications for bronchiectasis may include:
-
Bronchodilators: Potential side effects can include tremors, increased heart rate, and occasional jitteriness. If you experience these side effects, consult your healthcare provider for guidance.
-
Mucolytics: Some individuals may experience nausea, diarrhea, or an allergic reaction to mucolytic medications. Inform your healthcare provider if you experience any of these side effects.
-
Antibiotics: Antibiotics can sometimes cause digestive issues such as diarrhea or stomach discomfort. It is important to complete the full course of antibiotics as prescribed. If you experience severe side effects or an allergic reaction, seek immediate medical attention.
-
Inhaled corticosteroids: Regular use of inhaled corticosteroids may increase the risk of oral thrush or a hoarse voice. This can often be minimized by rinsing your mouth with water or brushing your teeth after each dose.
Always consult your healthcare provider if you have any concerns or questions about the side effects of your medications. They can provide you with the necessary guidance and support to manage any potential issues effectively.
Airway Clearance Techniques
How airway clearance helps bronchiectasis
Airway clearance techniques are an integral part of managing bronchiectasis. They help facilitate the removal of excessive mucus or sputum from the airways, reducing congestion and the risk of respiratory infections. By effectively clearing your airways, you can breathe more freely and reduce symptoms such as coughing and breathlessness.
In bronchiectasis, the airways become damaged and widened, making it difficult for mucus to be cleared naturally through coughing. Airway clearance techniques help compensate for this impaired clearance mechanism, promoting effective mucus removal.
Different airway clearance techniques
Several airway clearance techniques can be beneficial for individuals with bronchiectasis. Your healthcare provider can help you determine which techniques are most suitable for your individual needs. Some common techniques include:
-
Chest physiotherapy (CPT): CPT involves percussion, vibration, and postural drainage to help loosen and mobilize mucus. It may be performed by a healthcare professional or taught to you for self-administration.
-
High-frequency chest wall oscillation (HFCWO): HFCWO devices use an inflatable vest that vibrates at high frequencies, helping to dislodge and move mucus in the airways. This technique can be performed independently with proper training and guidance from a healthcare provider.
-
Positive expiratory pressure (PEP) therapy: PEP therapy involves using a device, such as a mask or mouthpiece, to create positive pressure during exhalation. This helps keep the airways open and promotes the mobilization of mucus.
-
Autogenic drainage: Autogenic drainage is a self-controlled technique that involves slow, controlled breathing at different lung volumes to mobilize mucus from different sections of the airways.
Your healthcare provider will guide you on the proper techniques, durations, and frequencies of airway clearance to suit your specific needs. It is essential to follow their instructions and maintain consistency in performing these techniques to optimize the benefits.
Developing a daily airway clearance routine
Incorporating airway clearance techniques into your daily routine can help manage bronchiectasis effectively and maintain healthy lung function. Here are some tips to help you establish a regular airway clearance routine:
-
Schedule: Set aside specific times during the day for airway clearance. It may be beneficial to perform these techniques in the morning to clear any accumulated mucus from overnight and before bedtime to ensure a restful night’s sleep.
-
Consistency: Aim to perform airway clearance techniques consistently every day. Consistency is key to maintaining healthy lung function and minimizing the risk of respiratory infections.
-
Combine techniques: Depending on your healthcare provider’s recommendations, you may benefit from combining different airway clearance techniques to maximize mucus clearance. For example, you may start with autogenic drainage and follow it with chest physiotherapy or positive expiratory pressure therapy.
-
Monitor progress: Regularly assess and discuss your airway clearance routines with your healthcare provider to ensure their effectiveness. They can provide valuable feedback, make adjustments as necessary, and address any concerns you may have.
By incorporating airway clearance techniques into your daily routine, you can take an active role in managing your bronchiectasis and promoting optimal respiratory health.

Breathing Techniques
Deep breathing exercises
Deep breathing exercises play a vital role in maintaining optimal lung function and managing bronchiectasis. By practicing these exercises regularly, you can improve your lung capacity and increase the efficiency of oxygen exchange. Here’s a simple deep breathing exercise to get you started:
-
Find a comfortable position: Sit upright or lie down on your back, placing a hand on your abdomen.
-
Inhale deeply: Breathe in slowly through your nose, focusing on expanding your abdomen as you fill your lungs with air. Ensure your chest remains still while your abdomen rises.
-
Exhale fully: Slowly exhale through your mouth, gently contracting your abdominal muscles to push out the air. Aim to empty your lungs completely.
-
Repeat: Continue this deep breathing cycle for several minutes, gradually increasing the duration as you become more comfortable.
Practicing deep breathing exercises for a few minutes each day can promote better lung function, reduce breathlessness, and enhance your overall well-being.
Pursed lip breathing
Pursed lip breathing is a simple breathing technique that can be beneficial for individuals with bronchiectasis. It helps slow down your breathing, promote better airflow, and reduce the feeling of breathlessness. Here’s how to practice pursed lip breathing:
-
Relax your body: Find a comfortable position, either sitting or standing.
-
Inhale slowly: Take a deep breath in through your nose, counting to two as you fill your lungs.
-
Purse your lips: Pucker your lips together, as if you were about to blow out a candle.
-
Exhale slowly: Breathe out slowly and steadily through your pursed lips, counting to four. Focus on making your exhalation longer than your inhalation.
-
Repeat: Practice this pursed lip breathing technique for several breaths, gradually increasing the duration as you feel more comfortable.
Pursed lip breathing can be practiced during activities that cause breathlessness, such as climbing stairs or engaging in physical exertion. It can help alleviate symptoms and support better breathing control.
Diaphragmatic breathing
Diaphragmatic breathing, also known as belly breathing or abdominal breathing, involves utilizing the diaphragm to achieve deeper, more efficient breaths. It can help improve ventilation, oxygenation, and respiratory muscle strength. Follow these steps to practice diaphragmatic breathing:
-
Find a comfortable position: Sit or lie down in a relaxed position, placing one hand on your chest and the other on your abdomen.
-
Inhale deeply: Breathe in slowly through your nose, allowing your abdomen to rise as you fill your lungs with air. Ensure your chest remains still, focusing on expanding your abdomen.
-
Exhale fully: Gently contract your abdominal muscles as you exhale slowly through your mouth. Imagine drawing your belly button towards your spine.
-
Repeat: Practice diaphragmatic breathing for several minutes, gradually increasing the duration as you become more comfortable with the technique.
Incorporating diaphragmatic breathing into your daily routine can help improve respiratory function, reduce breathlessness, and enhance overall lung health.
Infection Prevention
Maintaining good hygiene practices
Preventing respiratory infections is crucial for individuals with bronchiectasis as infections can exacerbate symptoms and lead to complications. Practicing good hygiene can significantly reduce the risk of contracting infections. Here are some important hygiene practices to incorporate into your daily routine:
-
Regular handwashing: Wash your hands thoroughly and frequently with soap and water, especially before eating, after using the restroom, and after being in public places.
-
Avoid touching your face: Refrain from touching your face, particularly your eyes, nose, and mouth, as this can introduce germs into your respiratory system.
-
Respiratory hygiene: Cover your mouth and nose with a tissue or your elbow when coughing or sneezing. Dispose of tissues properly and wash your hands afterward.
-
Cleaning and disinfecting: Regularly clean and disinfect frequently-touched surfaces, such as doorknobs, countertops, and electronic devices.
By incorporating these hygiene practices into your daily routine, you can reduce the risk of respiratory infections and protect your lung health.
Vaccination recommendations
Vaccinations play a crucial role in preventing infections and maintaining respiratory health, particularly for individuals with bronchiectasis. It is important to stay up-to-date with the recommended vaccinations and discuss with your healthcare provider which vaccinations are specifically recommended for you. Key vaccinations for individuals with bronchiectasis may include:
-
Influenza vaccine: The annual influenza vaccine helps protect against seasonal flu viruses, which can cause severe respiratory illness in individuals with bronchiectasis.
-
Pneumococcal vaccine: The pneumococcal vaccine protects against several strains of Streptococcus pneumoniae, a bacterium commonly associated with respiratory infections. There are different types of pneumococcal vaccines, and your healthcare provider will recommend the specific one(s) that are appropriate for you.
-
Other vaccines: Depending on your age, medical history, and specific risk factors, your healthcare provider may recommend additional vaccinations, such as the tetanus-diphtheria-pertussis (Tdap) vaccine or the varicella (chickenpox) vaccine.
Vaccinations can significantly reduce the risk of contracting infections that can worsen bronchiectasis symptoms and lead to complications. Consult your healthcare provider for personalized vaccination recommendations based on your medical history and specific needs.
Avoiding exposure to respiratory infections
Minimizing exposure to respiratory infections is an essential aspect of infection prevention for individuals with bronchiectasis. While it is not always possible to completely avoid infections, there are steps you can take to reduce the risk of exposure:
-
Limit crowded spaces: Avoid crowded places, especially during peak cold and flu seasons, as these environments can increase the likelihood of coming into contact with individuals carrying respiratory infections.
-
Practice social distancing: Maintain a safe distance from individuals who have a contagious illness, such as a cold or flu.
-
Wearing masks: Consider wearing a mask, especially during periods of increased respiratory infections or in situations where social distancing is challenging.
-
Educate close contacts: Inform your family, friends, and close contacts about the importance of respiratory hygiene and the risks associated with respiratory infections. Encourage them to practice good hygiene and stay home if they are feeling unwell.
By taking these preventative measures, you can reduce the risk of exposure to respiratory infections and help manage the impact of bronchiectasis on your respiratory health.

Exercise and Physical Activity
Benefits of exercise for bronchiectasis
Engaging in regular exercise and physical activity provides numerous benefits for individuals with bronchiectasis. Exercise can help improve lung function, increase cardiovascular fitness, enhance muscle strength, and boost overall well-being. Some specific benefits of exercise for bronchiectasis include:
-
Improved lung capacity: Regular exercise can enhance lung capacity and oxygen uptake, allowing your body to utilize oxygen more efficiently.
-
Reduced breathlessness: Engaging in exercise trains the respiratory muscles, helping to improve breathing control and reduce breathlessness during physical exertion.
-
Enhanced fitness: Exercise can improve cardiovascular fitness and endurance, allowing you to perform everyday activities with greater ease and less fatigue.
-
Strengthened muscles: Physical activity helps strengthen the muscles involved in respiration, supporting better lung function and reducing respiratory effort.
Choosing appropriate exercises
When selecting exercises for bronchiectasis, it is important to choose activities that are safe and appropriate for your fitness level and individual needs. Consider the following factors when choosing exercises:
-
Aerobic exercises: Aerobic exercises, such as walking, cycling, swimming, and dancing, can improve cardiovascular fitness and help increase lung capacity.
-
Strength training: Incorporating strength training exercises, such as resistance exercises or weightlifting, can improve overall muscle strength and respiratory muscle function.
-
Flexibility exercises: Performing flexibility exercises, such as stretching or yoga, can promote better posture, lung expansion, and respiratory muscle flexibility.
It is crucial to start with exercises of low intensity and gradually increase the intensity and duration as your physical fitness improves. Consult your healthcare provider or a qualified exercise professional to create an exercise plan that best suits your individual needs.
Modifying activities for individual needs
Individuals with bronchiectasis may have varying exercise tolerance levels and specific considerations. It is important to listen to your body and make modifications as necessary to ensure your safety and comfort. Here are some general considerations for modifying activities:
-
Work at your own pace: Perform exercises at a pace that feels comfortable for you, gradually increasing the intensity as your fitness improves.
-
Take rest breaks: Allow yourself adequate rest breaks during exercise, particularly if you experience breathlessness or fatigue. Listen to your body and adjust your exercise duration or intensity accordingly.
-
Consider the environment: Be mindful of the environment in which you perform exercises. Extreme temperatures or poor air quality can impact your respiratory health. Opt for indoor exercise during extreme weather conditions or when the air quality is compromised.
-
Stay hydrated: Drink plenty of water before, during, and after exercise to stay well-hydrated and maintain optimal respiratory function.
Consult with your healthcare provider or a qualified exercise professional for personalized guidance and recommendations on modifying exercises to suit your individual needs and abilities.
Diet and Nutrition
Balanced diet recommendations
Maintaining a healthy and balanced diet is important for individuals with bronchiectasis. A well-rounded diet can support optimal lung function, immune system health, and overall well-being. Consider the following dietary recommendations:
-
Fruits and vegetables: Consume a variety of fruits and vegetables to ensure an adequate intake of essential vitamins, minerals, and antioxidants. These nutrients support respiratory health and help strengthen the immune system.
-
Lean proteins: Include lean protein sources, such as poultry, fish, legumes, and tofu, in your diet. Protein is essential for tissue repair and immune system function.
-
Whole grains: Choose whole grains, such as whole wheat bread, brown rice, and oats, instead of refined grains. Whole grains provide fiber, vitamins, and minerals, promoting digestive health and overall well-being.
-
Healthy fats: Incorporate sources of healthy fats, such as avocados, nuts, seeds, and olive oil, into your diet. These fats provide essential fatty acids that support lung health and reduce inflammation.
-
Hydration: Drink an adequate amount of water throughout the day to stay well-hydrated. Proper hydration helps maintain mucus consistency and supports optimal respiratory function.
Consult with a registered dietitian or healthcare professional to develop a personalized diet plan that suits your individual needs and promotes overall health.
Identifying foods that trigger symptoms
Certain foods may trigger symptoms in individuals with bronchiectasis. While triggers can vary from person to person, some common culprits include:
-
Dairy products: Dairy products, such as milk and cheese, can sometimes increase mucus production and contribute to congestion. If you find that consuming dairy worsens your symptoms, consider reducing your intake or opting for dairy alternatives.
-
Processed foods: Processed foods, particularly those high in sodium or additives, may contribute to inflammation and worsen respiratory symptoms. Aim to limit your intake of processed foods and opt for whole, unprocessed alternatives whenever possible.
-
Allergenic foods: Some individuals with bronchiectasis may have specific food allergies or sensitivities that can trigger respiratory symptoms. If you suspect a particular food is causing or worsening your symptoms, consult with a healthcare professional for an allergy test or elimination diet.
It can be helpful to keep a food diary to track your symptoms and identify any potential trigger foods. Discuss your findings with your healthcare provider or a registered dietitian to develop a personalized dietary plan that supports your respiratory health.
Importance of staying well-hydrated
Staying well-hydrated is essential for individuals with bronchiectasis as it helps maintain mucus consistency and promotes effective airway clearance. Here are some key points to keep in mind regarding hydration:
-
Water intake: Drink an adequate amount of water throughout the day, aiming for at least eight cups of fluid. This includes water, herbal teas, and other hydrating beverages. Your fluid needs may vary depending on your overall health and activity level.
-
Monitor urine color: Pay attention to the color of your urine, as it can be an indicator of hydration status. Clear to pale yellow urine typically indicates adequate hydration, while darker urine may suggest dehydration.
-
Avoid excessive caffeine and alcohol: Limit your consumption of caffeinated beverages, such as coffee and sodas, as they can have a diuretic effect and contribute to dehydration. Similarly, alcohol should be consumed in moderation, as it can dehydrate the body.
Staying well-hydrated supports healthy mucus production, eases airway clearance, and helps maintain optimal respiratory function. Be mindful of your hydration levels and adjust your fluid intake according to your specific needs and lifestyle.

Coping with Exacerbations
Recognizing exacerbation symptoms
Exacerbations, or flare-ups, can occur in individuals with bronchiectasis and may be triggered by respiratory infections, environmental factors, or other underlying conditions. It is important to recognize the symptoms of exacerbations to take appropriate action and prevent further complications. Common symptoms of exacerbations may include:
-
Increased cough: Persistent or worsening cough, with or without the production of more mucus than usual.
-
Change in sputum characteristics: Change in the color, consistency, or odor of the sputum, such as a darker color or a foul smell.
-
Breathlessness: An increase in breathlessness or difficulty breathing, especially during activities that were previously manageable.
-
Increased fatigue: Unusual or excessive fatigue or a decline in overall energy levels.
-
Fever: The presence of a fever, particularly if it is accompanied by other respiratory symptoms.
If you notice any of these symptoms or experience a decline in your respiratory health, contact your healthcare provider promptly to address the exacerbation appropriately.
Self-care during exacerbations
When experiencing an exacerbation, self-care measures can help manage symptoms and support recovery. Consider the following self-care strategies:
-
Stay well-hydrated: Drink plenty of fluids to keep your body hydrated and to help maintain optimal mucus consistency.
-
Rest and conserve energy: Allow yourself adequate rest to conserve energy and support the healing process.
-
Take prescribed medications: Take your prescribed medications as directed by your healthcare provider to alleviate symptoms, control infections, and manage inflammation.
-
Perform airway clearance techniques: Continue with your recommended airway clearance techniques to remove excessive mucus from your airways and improve respiratory function.
-
Follow a balanced diet: Maintain a nutritious diet to support overall well-being and provide the necessary nutrients for recovery.
Always consult your healthcare provider for personalized advice and guidance during exacerbations, as they can recommend additional measures, adjust medications, or provide specific instructions based on your individual needs.
Seeking medical assistance when necessary
If you experience severe symptoms or notice a rapid deterioration in your respiratory health, it is essential to seek immediate medical assistance. Prompt medical attention can help prevent complications and improve the outcome during exacerbations. Here are some signs that warrant immediate medical attention:
-
Severe breathlessness: If you are struggling to breathe or experiencing severe shortness of breath, seek medical assistance immediately.
-
Chest pain: The presence of chest pain, particularly if it is severe or accompanied by other symptoms, should not be ignored.
-
High fever: If you have a high fever, especially if it is persistent or accompanied by other respiratory symptoms, consult a healthcare professional promptly.
-
Rapid decline in respiratory function: If you notice a rapid decline in your respiratory function or experience a significant increase in symptoms over a short period, contact your healthcare provider right away.
Do not hesitate to contact emergency services if you are experiencing a medical emergency. Trust your instincts and prioritize seeking timely medical assistance to ensure your well-being.
Managing Mental and Emotional Well-being
Coping with the emotional impact of living with bronchiectasis
Living with a chronic lung condition like bronchiectasis can have a significant emotional impact. It is normal to experience a range of emotions, including frustration, anxiety, sadness, or anger. Here are some strategies to cope with the emotional challenges:
-
Educate yourself: Learning about bronchiectasis and understanding its management can help alleviate anxiety and empower you to take an active role in your own care.
-
Seek support: Reach out to a support network of family, friends, or support groups who can offer understanding, empathy, and encouragement. Consider joining online forums or support groups specifically for individuals with respiratory conditions.
-
Talk to a mental health professional: If you find that your emotional well-being is significantly impacted, consider seeking support from a mental health professional, such as a therapist or counselor, who can provide guidance and coping strategies.
-
Practice self-care: Engage in activities that bring you joy, relaxation, and fulfillment. This may include hobbies, mindfulness exercises, journaling, or engaging in creative pursuits.
Supportive strategies for managing stress and anxiety
Chronic respiratory conditions like bronchiectasis can sometimes lead to increased stress and anxiety. It is important to develop supportive strategies to manage these emotions effectively. Consider the following techniques:
-
Deep breathing and relaxation: Practice deep breathing exercises, meditation, or other relaxation techniques to reduce anxiety and promote a sense of calm.
-
Stress management: Identify sources of stress and explore stress management techniques. This may include time management strategies, setting realistic expectations, prioritizing self-care, and seeking support when needed.
-
Positive mindset: Cultivate a positive mindset and focus on the aspects of your life that bring you joy and fulfillment. Incorporate gratitude practices into your routine to shift your focus to the positive aspects of your journey.
-
Exercise and physical activity: Engaging in regular physical activity releases endorphins and helps manage stress and anxiety. Choose activities that you enjoy and that align with your physical abilities.
Remember to prioritize your mental and emotional well-being as an essential component of managing bronchiectasis. Be kind to yourself, practice self-compassion, and seek support when needed.
Living with bronchiectasis may present certain challenges, but with the right strategies and support, you can effectively manage the condition and maintain a high quality of life. It is important to collaborate closely with your healthcare provider, follow the recommended treatments and lifestyle modifications, and stay proactive in managing your respiratory health. Remember, you are not alone on this journey, and support is available to help you navigate the complexities of bronchiectasis. With proper management, a positive mindset, and the necessary support, you can lead a fulfilling and enjoyable life despite the challenges posed by bronchiectasis.