You’re not alone if you’ve been dealing with the bothersome symptoms of Benign Prostatic Hyperplasia (BPH). This common condition, also known as an enlarged prostate, affects many men as they age. But fret not, as there are effective ways to manage the symptoms and regain control of your life. Whether it’s frequent urination, difficulty starting and stopping urine flow, or the feeling of not fully emptying your bladder, this article will explore strategies and treatments that can help you keep BPH symptoms at bay. From lifestyle changes to medical interventions, discover how you can find relief and maintain your quality of life.

Understanding BPH
What is BPH?
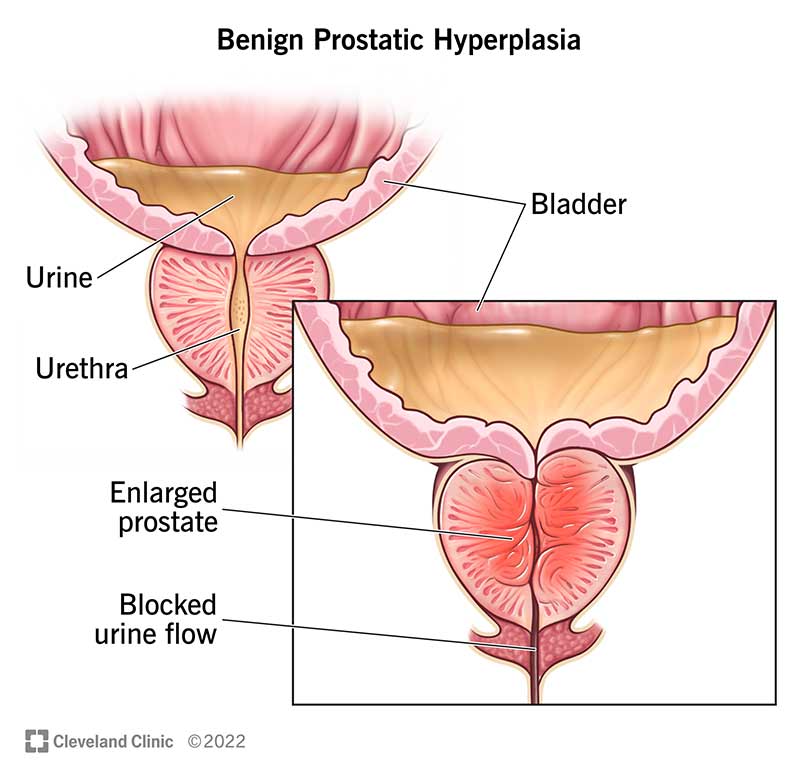
Benign Prostatic Hyperplasia (BPH) is a condition that affects the prostate gland in men. The prostate gland is a walnut-sized organ located below the bladder and plays a role in the reproductive system. BPH occurs when the prostate gland grows in size and presses against the urethra, the tube that carries urine out of the body. This enlargement of the prostate can lead to various urinary symptoms and can impact a man’s quality of life.
Causes of BPH
The exact cause of BPH is still not fully understood. However, it is believed to be primarily influenced by age and hormonal changes. As men age, the levels of testosterone in their bodies decrease, while other hormones such as estrogen may become more prominent. These hormonal imbalances can contribute to the growth of prostate cells, leading to BPH. Other factors that may play a role in the development of BPH include genetic predisposition and inflammation in the prostate gland.
Risk factors for BPH
While BPH can occur in any man as they age, there are certain risk factors that may increase the likelihood of developing this condition. These include advancing age, family history of BPH, obesity, sedentary lifestyle, and certain medical conditions such as diabetes and heart disease. It is important to note that having these risk factors does not guarantee the development of BPH, but they may increase the chances of it occurring.
Diagnosing BPH
Medical history and physical examination
To diagnose BPH, your healthcare provider will begin by taking a detailed medical history, including any symptoms you may be experiencing. They will also perform a physical examination, which may involve a digital rectal examination (DRE) to assess the size and condition of your prostate gland. This examination is done by gently inserting a gloved finger into the rectum to feel the prostate.
Prostate-specific antigen (PSA) blood test
A prostate-specific antigen (PSA) blood test may be conducted to measure the levels of a specific protein produced by the prostate gland. Elevated levels of PSA may indicate a problem with the prostate, such as BPH or prostate cancer. However, it is important to note that PSA levels can also be elevated due to other factors, including prostate infections or recent ejaculation.
Urine tests
Your healthcare provider may request a urine sample to check for urinary tract infections or other underlying conditions that may be contributing to your symptoms. These tests can help rule out other potential causes of urinary problems.
Digital rectal examination
In addition to assessing the size and condition of the prostate gland, a digital rectal examination (DRE) can also help detect any abnormalities or indications of prostate cancer. This examination is a quick and relatively painless procedure.
Transrectal ultrasound
A transrectal ultrasound involves the use of a probe inserted into the rectum to create images of the prostate gland using sound waves. This imaging technique can provide detailed information about the size and structure of the prostate, helping to evaluate the extent of enlargement and ruling out other conditions.
Uroflowmetry
Uroflowmetry is a simple test that measures the rate and volume of urine flow when you urinate. The test involves voiding into a special device that measures these parameters. Abnormal flow patterns or reduced flow rates may indicate the presence of BPH.

Common Symptoms of BPH
Urinary frequency
One of the most common symptoms of BPH is increased urinary frequency. You may find yourself needing to urinate more often than usual, both during the day and at night. This can disrupt your sleep and daily activities.
Nocturia (frequent urination at night)
Nocturia refers to the need to wake up multiple times during the night to urinate. This can significantly disrupt your sleep patterns and leave you feeling tired during the day.
Urgency to urinate
BPH can cause a sudden and urgent need to urinate. You may feel the need to rush to the bathroom frequently throughout the day, which can be bothersome and inconvenient.
Weak urine flow
Another common symptom of BPH is a weak urine flow. You may notice that your stream is slower and less forceful than usual, making it difficult to completely empty your bladder.
Incomplete bladder emptying
BPH can interfere with the complete emptying of the bladder, leaving behind urine that can cause discomfort and increase the risk of urinary tract infections. You may feel a persistent sensation of needing to urinate even after just having done so.
Hesitant or intermittent urination
Difficulty initiating urination or starting and stopping several times during the process can also be attributed to BPH. This can further prolong the time it takes to empty the bladder fully.
Dribbling at the end of urination
BPH can cause urine to dribble out slowly or leak after you have finished urinating. This can be frustrating and may require additional measures to ensure adequate emptying of the bladder.
Lifestyle Modifications
Fluid management
Managing your fluid intake can help alleviate some of the symptoms associated with BPH. It is advisable to avoid excessive consumption of fluids, especially before bedtime, to reduce nocturia and minimize disruptions to your sleep. However, it is important to maintain adequate hydration throughout the day, so be sure to drink enough water.
Bladder training
Bladder training involves gradually increasing the time intervals between urination. By consciously delaying urination slightly when you feel the urge, you can help retrain your bladder to hold larger amounts of urine and reduce the frequency of urination.
Timed voiding
Similar to bladder training, timed voiding involves emptying your bladder at regular intervals throughout the day, regardless of whether you feel the need to urinate. This technique can help prevent the bladder from becoming excessively full and reduce episodes of urgency and frequency.
Dietary adjustments
Certain dietary changes can be beneficial in managing BPH symptoms. Avoiding or minimizing the consumption of irritants such as caffeine and alcohol can help reduce urinary frequency and urgency. Additionally, incorporating foods rich in antioxidants and nutrients, such as fruits, vegetables, and whole grains, can contribute to overall prostate health.
Pelvic floor muscle exercises
Exercises that target the pelvic floor muscles, often referred to as Kegel exercises, can help strengthen these muscles and improve bladder control. Regular practice of these exercises can enhance your ability to start and stop urination more effectively and prevent urine leakage.
Stress management techniques
Stress and anxiety can exacerbate BPH symptoms. Employing stress management techniques such as deep breathing exercises, meditation, or engaging in activities that promote relaxation can help lower stress levels and alleviate symptoms.
Medication Options
Alpha blockers
Alpha blockers are medications that relax the muscles in the prostate and bladder neck, improving urine flow and relieving symptoms. These medications work quickly and can provide immediate relief.
5-alpha reductase inhibitors
5-alpha reductase inhibitors help reduce the size of the prostate gland by inhibiting the conversion of testosterone to another active hormone. These medications can take several months to show noticeable effects on symptoms.
Combination therapy
Combining alpha blockers and 5-alpha reductase inhibitors may provide more significant symptom relief for some men with BPH. This combination targets both the relaxation of prostate and bladder muscles as well as the reduction in prostate size.
Phytotherapy (herbal supplements)
Certain herbal supplements, such as saw palmetto, beta-sitosterol, and rye grass pollen extract, have been used in the management of BPH symptoms. Although these supplements are widely available, their effectiveness is still a subject of debate. Consult with your healthcare provider before starting any herbal supplements.
Anticholinergic drugs
Anticholinergic drugs help relax the bladder muscles and reduce urinary urgency and frequency. However, these medications may cause side effects such as dry mouth, constipation, and blurred vision. They are often used in combination with other medications.
Phosphodiesterase-5 inhibitors
Phosphodiesterase-5 inhibitors, commonly used to treat erectile dysfunction, have been found to have a positive impact on urinary symptoms associated with BPH. These medications help relax the smooth muscles in the prostate and bladder neck, leading to improved urine flow.
Minimally Invasive Treatments
Transurethral resection of the prostate (TURP)
Transurethral resection of the prostate (TURP) is a surgical procedure that involves removing obstructive prostate tissue using a thin tube inserted through the urethra. This procedure is considered the gold standard for treating BPH but may be associated with some risks and side effects.
Transurethral incision of the prostate (TUIP)
Transurethral incision of the prostate (TUIP) involves making small cuts in the prostate to relieve the pressure on the urethra and improve urine flow. This procedure is generally recommended for men with smaller prostate glands and is associated with fewer risks compared to TURP.
Transurethral microwave therapy (TUMT)
Transurethral microwave therapy (TUMT) aims to destroy excessive prostate tissue using microwave energy delivered through a special catheter. This minimally invasive procedure can provide relief from BPH symptoms and is generally well-tolerated.
Transurethral needle ablation (TUNA)
Transurethral needle ablation (TUNA) involves inserting needles into the prostate and delivering low-level radiofrequency energy to heat and destroy excess prostate tissue. This procedure can improve urine flow and reduce the size of the prostate without the need for extensive surgery.
Water-induced thermotherapy (WIT)
Water-induced thermotherapy (WIT) uses heated water to destroy prostate tissue, reducing its size and relieving symptoms. This treatment is performed by inserting a heated catheter into the prostate and is typically done on an outpatient basis.
Prostatic urethral lift (PUL)
Prostatic urethral lift (PUL) is a minimally invasive procedure that involves using small implants to hold the enlarged prostate tissue away from the urethra, thereby improving urine flow. This procedure does not involve removing or destroying any prostate tissue.
Prostatic arterial embolization (PAE)
Prostatic arterial embolization (PAE) is a non-surgical procedure that involves injecting small particles into the arteries supplying the prostate gland. This leads to a reduction in blood flow, causing the prostate to shrink and relieve urinary symptoms.

Surgical Procedures
Open prostatectomy
Open prostatectomy is a traditional surgical procedure performed under general anesthesia to remove enlarged prostate tissue. This procedure may be recommended for men with very large prostate glands or who have other complicating factors.
Transurethral electrovaporization of the prostate (TVP)
Transurethral electrovaporization of the prostate (TVP) is a surgical procedure that involves using an electric current to vaporize excessive prostate tissue, thereby improving urine flow. This procedure is similar to TURP but uses different energy sources.
Holmium laser enucleation of the prostate (HoLEP)
Holmium laser enucleation of the prostate (HoLEP) is a minimally invasive surgical procedure that uses a laser to remove obstructive prostate tissue. This method is considered safe and effective, with fewer risks compared to traditional open surgery.
Photoselective vaporization of the prostate (PVP)
Photoselective vaporization of the prostate (PVP) is a laser-based procedure that vaporizes and removes excess prostate tissue to improve urine flow. This technique is less invasive than traditional surgery and offers a faster recovery time.
Greenlight laser therapy
Greenlight laser therapy is a minimally invasive procedure that utilizes laser energy to vaporize obstructive prostate tissue. This technique allows for precise removal of prostate tissue while minimizing damage to surrounding structures.
Robotic-assisted prostate surgery
Robotic-assisted prostate surgery, also known as robotic prostatectomy, involves using a robotic system to assist the surgeon in performing precise and minimally invasive removal of prostate tissue. This technique offers better visualization and enhanced surgical precision.
Alternative and Complementary Therapies
Acupuncture
Acupuncture is an ancient practice that involves the insertion of thin needles at specific points on the body. Some men with BPH have reported improvements in their symptoms through acupuncture. However, further research is needed to confirm its effectiveness.
Saw palmetto
Saw palmetto is a popular herbal supplement that is believed to help reduce BPH symptoms by inhibiting the production of hormone-like substances that contribute to prostate enlargement. While some men report symptom relief with saw palmetto, scientific evidence is limited.
Pygeum
Pygeum is another herbal supplement that is derived from the bark of the African plum tree. It has been used traditionally to address BPH symptoms. Some studies suggest that pygeum may have anti-inflammatory and antiandrogenic effects, but more research is needed.
Beta-sitosterol
Beta-sitosterol is a plant sterol present in various fruits, vegetables, and nuts. It has been studied for its potential benefits in reducing urinary symptoms associated with BPH. While results vary, some men have reported improvements in their symptoms when using beta-sitosterol.
Rye grass pollen extract
Rye grass pollen extract is derived from three different types of grass and has been used in European countries for many years as a treatment for BPH symptoms. This natural supplement is believed to have anti-inflammatory properties and may help improve urine flow.
Zinc and other supplements
Zinc is a mineral that plays a role in prostate health. It has been suggested that men with BPH may have lower zinc levels. However, evidence supporting the use of zinc supplements specifically for BPH is limited. Consult with your healthcare provider before starting any new supplements.

Coping Strategies and Support
Educating oneself about BPH
One of the most important coping strategies for dealing with BPH is to educate yourself about the condition. Understanding the causes, symptoms, and available treatment options can empower you to make informed decisions and actively manage your symptoms.
Seeking emotional support
Dealing with the symptoms of BPH can be challenging, both physically and emotionally. It is important to seek emotional support from loved ones, friends, or support groups. Sharing your experiences and concerns with others who have faced similar challenges can provide a sense of validation and relief.
Joining support groups
Joining a support group specifically focused on BPH or prostate health can offer valuable insights from others who are going through similar experiences. Support groups provide a safe space for sharing information, discussing coping strategies, and obtaining emotional support.
Engaging in relaxation techniques
Stress management is crucial in managing BPH symptoms. Engaging in relaxation techniques such as deep breathing exercises, meditation, or yoga can help reduce stress levels and improve overall well-being.
Maintaining a healthy lifestyle
Leading a healthy lifestyle can have a positive impact on your BPH symptoms. Regular exercise, maintaining a balanced diet, getting enough sleep, and avoiding excessive alcohol and caffeine consumption can contribute to your overall health and well-being.
Regular follow-up with healthcare provider
It is important to have regular follow-up appointments with your healthcare provider to monitor your BPH symptoms and evaluate the effectiveness of your chosen treatment plan. Your healthcare provider can also make necessary adjustments to your treatment if needed.
When to Seek Medical Attention
Worsening symptoms
If your BPH symptoms worsen or if new symptoms develop, it is important to seek medical attention. This may include severe urinary hesitation, inability to urinate, increased pain, blood in the urine, or recurrent urinary tract infections.
Development of complications
BPH can lead to complications such as urinary tract infections, bladder stones, or kidney damage. If you experience any signs of complications, such as fever, chills, severe pain, or changes in urine color, seek immediate medical attention.
Impact on daily life
If your BPH symptoms significantly interfere with your daily life, work, or leisure activities, it is advisable to consult with your healthcare provider. They can help assess the severity of your symptoms and recommend appropriate treatment options.
Unbearable pain or discomfort
If you experience severe pain or discomfort that is intolerable, it is essential to seek immediate medical attention. Severe pain may indicate a urinary obstruction or other serious complications that require prompt medical intervention.
By understanding the basics of BPH, the available diagnostic methods, treatment options, coping strategies, and when to seek medical attention, you can take control of your condition and make informed decisions to manage your symptoms effectively. Remember to consult with your healthcare provider to determine the most suitable approach for your specific situation. With the right knowledge and support, you can navigate through the challenges of BPH and improve your quality of life.