Are you experiencing urinary difficulties such as frequent urination, weak urine flow, or the feeling of not being able to completely empty your bladder? If so, you may be dealing with a condition known as Benign Prostatic Hyperplasia (BPH). In this article, we will explore various strategies and lifestyle changes that can help prevent the progression of BPH and improve your overall quality of life. So, take a moment to discover practical steps you can take to take control of your urinary health.

Understanding Benign Prostatic Hyperplasia
What is Benign Prostatic Hyperplasia?
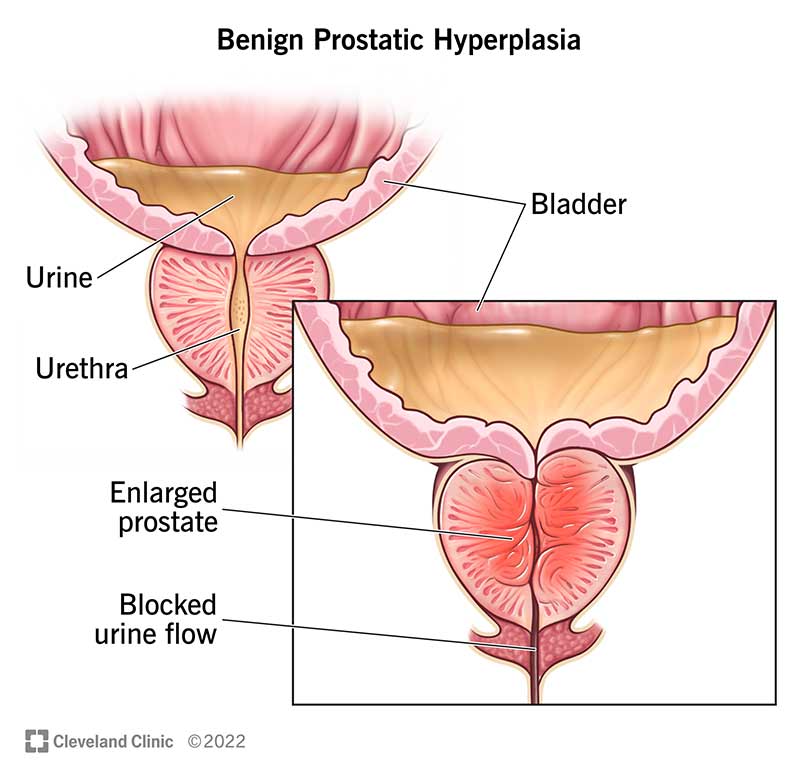
Benign Prostatic Hyperplasia (BPH), also known as enlarged prostate, is a common condition that affects men, especially as they age. It is characterized by the enlargement of the prostate gland, which surrounds the urethra—the tube that carries urine from the bladder out of the body. The exact cause of BPH is not fully understood, but hormonal changes and aging are believed to play a significant role in its development.
Causes of Benign Prostatic Hyperplasia
The exact cause of BPH is still unknown, but several factors contribute to its development. Changes in hormone levels, specifically a higher level of estrogen relative to testosterone, may promote prostate growth. Age is also a major contributing factor, as BPH is rare in younger men but becomes more prevalent with advancing age. Other potential causes include inflammation of the prostate, family history, and lifestyle factors such as obesity and sedentary behavior.
Risk Factors for Benign Prostatic Hyperplasia
While the exact cause of BPH is unclear, several risk factors have been identified. Age is the most significant risk factor, with BPH being uncommon in men under 40 but affecting more than half of men over 60. Family history also plays a role, as men with a family history of BPH are more likely to develop the condition themselves. Ethnicity may also influence the risk, with BPH being more common in African American men. Additionally, certain medical conditions, such as obesity, heart disease, and type 2 diabetes, have been associated with an increased risk of BPH.
Symptoms of Benign Prostatic Hyperplasia
Lower Urinary Tract Symptoms
The symptoms of BPH primarily affect the lower urinary tract and can significantly impact a man’s quality of life. The most common symptom is urinary frequency, where you may find yourself needing to urinate more frequently, especially at night. You may also experience urgency, where you have a sudden and strong urge to urinate. Other symptoms include hesitancy, weak urine flow, dribbling at the end of urination, and the feeling of incomplete bladder emptying. These symptoms can vary in severity and may worsen over time if left untreated.
Complications of Benign Prostatic Hyperplasia
If left untreated, BPH can lead to various complications. One common complication is urinary tract infections (UTIs), which can occur when urine remains in the bladder for an extended period due to incomplete emptying. Another potential complication is acute urinary retention, where you are suddenly unable to urinate and may require emergency medical intervention. Chronic urinary retention, a condition where the bladder does not completely empty with each urination, can also arise. Additionally, BPH can cause bladder stones, kidney damage, and in severe cases, renal failure.
Diagnostic Methods for Benign Prostatic Hyperplasia
Medical History and Physical Examination
To diagnose BPH, your healthcare provider will begin with a detailed medical history to understand your symptoms and assess their impact on your daily life. They will then perform a physical examination, including a digital rectal examination (DRE), to assess the size and condition of the prostate gland. During the DRE, your doctor will insert a gloved, lubricated finger into your rectum to feel the prostate for any abnormalities.
Prostate-Specific Antigen (PSA) Test
In addition to the physical examination, your doctor may order a blood test to measure your prostate-specific antigen (PSA) levels. PSA is a protein produced by the prostate, and an elevated PSA level may indicate an enlarged prostate or other prostate-related conditions. However, it is important to note that a high PSA level does not necessarily confirm BPH and can also be seen in prostate cancer or other prostate disorders.
Digital Rectal Examination (DRE)
As mentioned earlier, a digital rectal examination (DRE) is an important part of the diagnostic process for BPH. It allows your doctor to assess the size, shape, and texture of the prostate gland. During the DRE, your doctor will insert a lubricated, gloved finger into the rectum to feel for any abnormalities, such as an enlarged prostate or nodules.
Transrectal Ultrasound
A transrectal ultrasound may be performed to get a more detailed image of the prostate gland. During this procedure, a probe is inserted into the rectum, and sound waves are used to create images of the prostate on a monitor. This imaging technique helps your doctor evaluate the size of the prostate and identify any irregularities.
Uroflowmetry
Uroflowmetry is a noninvasive test that measures the rate and volume of urine flow during urination. It involves urinating into a special device that records the flow of urine. By assessing the flow pattern and volume, your doctor can gain insights into the severity of your urinary symptoms and identify any potential obstructions caused by an enlarged prostate.
Cystoscopy
Cystoscopy is a procedure that involves inserting a thin, flexible tube with a camera on the end (cystoscope) into the urethra and up to the bladder. It allows your doctor to visually examine the inside of the urethra and bladder, checking for any abnormalities or signs of obstruction. While it may be uncomfortable, cystoscopy provides valuable information about the condition of the lower urinary tract.
Biopsy
In some cases, a biopsy may be necessary to rule out prostate cancer or other conditions. During a biopsy, a small sample of prostate tissue is taken and examined under a microscope for signs of cancer or other abnormalities. This procedure is typically performed under local anesthesia and may cause some discomfort.
Conservative Management Approaches for Benign Prostatic Hyperplasia
Watchful Waiting
In cases of mild to moderate BPH, your doctor may recommend watchful waiting, particularly if your symptoms are not causing significant discomfort or affecting your quality of life. With watchful waiting, you will undergo regular check-ups to monitor the progression of your BPH. Lifestyle modifications, such as avoiding caffeine and alcohol, limiting fluid intake before bed, and practicing double voiding (urinating twice within a short period to ensure the bladder is emptied), may also be recommended.
Lifestyle Modifications
Lifestyle modifications can significantly improve BPH symptoms and reduce the need for medication or surgery. Maintaining a healthy weight through regular exercise and a balanced diet is crucial, as obesity is linked to an increased risk of BPH. It is also important to limit fluid intake before bed and avoid diuretic substances such as caffeine and alcohol. Additionally, bladder training exercises and practicing Kegel exercises can help strengthen the muscles around the bladder and improve urinary control.
Medications
There are several medications available to manage BPH symptoms and improve urinary flow. Alpha-blockers, such as tamsulosin and terazosin, relax the muscles in the bladder neck and prostate, relieving urinary symptoms. 5-alpha reductase inhibitors, such as finasteride and dutasteride, work by shrinking the prostate gland over time. These medications can be used alone or in combination, depending on the severity of symptoms and individual response.

Minimally Invasive Treatments for Benign Prostatic Hyperplasia
Transurethral Microwave Therapy (TUMT)
Transurethral Microwave Therapy (TUMT) is a minimally invasive procedure that uses microwaves to heat and destroy excess prostate tissue. It is performed by inserting a catheter-like device into the urethra, which emits microwaves to heat and shrink the prostate gland. TUMT is an outpatient procedure that offers a quicker recovery time compared to traditional surgery.
Transurethral Needle Ablation (TUNA)
Transurethral Needle Ablation (TUNA) is another minimally invasive treatment option for BPH. It involves inserting needles into the prostate gland, which emit radiofrequency energy to destroy the excess tissue. TUNA can be performed under local or general anesthesia, and the recovery time is relatively short.
Water-induced Thermotherapy (WIT)
Water-induced Thermotherapy (WIT), also known as the ProstaLund Feedback Treatment (PLFT), is a noninvasive procedure that uses heated water to treat BPH. During the procedure, a device is inserted into the urethra, and heated water is circulated to target and destroy excess prostate tissue. WIT offers a good balance between effectiveness and minimal invasiveness.
Prostatic Urethral Lift (PUL)
Prostatic Urethral Lift (PUL), commercially known as UroLift, is a relatively new and minimally invasive treatment option for BPH. It involves the placement of small implants in the prostate to hold the enlarged tissue away from the urethra, thus relieving urinary symptoms. PUL is typically performed as an outpatient procedure, and patients experience minimal discomfort and quick recovery.
Rezum Treatment
Rezum is a minimally invasive procedure that uses water vapor therapy to treat BPH. It involves the injection of steam into the prostate, which causes the excess tissue to shrink and relieve symptoms. Rezum is an outpatient procedure done under local anesthesia, and patients generally experience significant improvement in urinary symptoms.
Surgical Treatments for Benign Prostatic Hyperplasia
Transurethral Resection of the Prostate (TURP)
Transurethral Resection of the Prostate (TURP) is a surgical procedure performed under general or spinal anesthesia to treat moderate to severe BPH. It involves the removal of excess prostate tissue using a resectoscope, a thin tube inserted through the urethra. TURP offers excellent long-term results but may require a longer recovery period compared to minimally invasive treatments.
Transurethral Incision of the Prostate (TUIP)
Transurethral Incision of the Prostate (TUIP) is a surgical procedure that aims to relieve symptoms by making small incisions in the prostate. This procedure allows the urethra to open wider, improving the flow of urine. TUIP is typically performed under anesthesia and is an appropriate option for men with smaller prostate glands.
Laser Surgery
Laser surgery has become a popular surgical option for BPH due to its precision and effectiveness. There are different types of laser procedures, such as Holmium laser enucleation of the prostate (HoLEP), GreenLight laser therapy, and Thulium laser ablation. These procedures use laser energy to remove or destroy excess prostate tissue, improving urinary flow. Laser surgeries offer reduced bleeding, shorter hospital stays, and faster recovery compared to traditional surgery.
Open Prostatectomy
Open Prostatectomy is a traditional surgical procedure used for men with very large prostate glands that do not respond to other treatment options. It requires a larger incision in the lower abdomen to remove the obstructing prostate tissue. While it is an effective treatment, open prostatectomy is associated with longer hospital stays, more significant blood loss, and a longer recovery period.

Prevention Strategies for Benign Prostatic Hyperplasia
Maintaining a Healthy Lifestyle
Maintaining a healthy lifestyle can significantly reduce the risk of developing BPH or slow down its progression. Regular exercise, a balanced diet rich in fruits, vegetables, whole grains, and lean proteins, and stress management techniques can promote overall prostate health.
Dietary Modifications
Certain dietary modifications may help prevent or manage BPH symptoms. Increasing fiber intake, particularly from fruits and vegetables, can help regulate bowel movements and prevent constipation, which can worsen urinary symptoms. Consuming foods rich in omega-3 fatty acids, such as fatty fish and flaxseeds, may also be beneficial due to their anti-inflammatory properties.
Herbal Supplements
Some herbal supplements have been studied for their potential benefits in managing BPH symptoms. Saw palmetto, pygeum africanum, and beta-sitosterol are some of the commonly used herbal supplements. However, it is important to consult with a healthcare professional before starting any herbal supplements, as their efficacy and safety may vary.
Avoiding Certain Substances
Avoiding substances that can irritate the bladder and worsen BPH symptoms is important. Limiting caffeine and alcohol intake, as well as avoiding spicy foods and artificial sweeteners, may help reduce urinary symptoms. It is also important to stay well-hydrated throughout the day to promote optimal urinary function.
Complications and Potential Risks
Postoperative Complications
Postoperative complications can occur after surgical treatments for BPH. These may include bleeding, infection, urinary incontinence, erectile dysfunction, and retrograde ejaculation. While these complications are relatively rare, it is important to discuss the potential risks and benefits of surgery with your healthcare provider.
Side Effects of Medications
Medications used to manage BPH symptoms may have side effects that vary depending on the specific drug. Alpha-blockers can cause dizziness and low blood pressure, while 5-alpha reductase inhibitors may lead to sexual side effects such as decreased libido and erectile dysfunction. It is crucial to discuss any concerns or side effects with your doctor to determine the best treatment approach.
Potential Challenges and Risks
Managing BPH can present challenges and risks for some individuals. The symptoms of BPH can have a significant impact on quality of life, affecting sleep, sexual function, and daily activities. It is important to address these challenges and seek appropriate medical attention to minimize discomfort and prevent complications. Regular follow-up and monitoring are essential to ensure the effectiveness of treatment and detect any recurrence or progression of the condition.

Follow-up and Monitoring
Importance of Regular Check-ups
Regular check-ups with your healthcare provider are crucial to monitor your BPH and ensure the effectiveness of treatment. These check-ups allow the healthcare provider to evaluate your symptom progression, monitor the size of your prostate, assess treatment response, and make any necessary adjustments to your management plan. It is important to attend these appointments and openly communicate any changes or concerns you may have.
Post-treatment Care
After undergoing treatment for BPH, it is important to follow any post-treatment care instructions provided by your healthcare provider. This may include taking prescribed medications, practicing lifestyle modifications, engaging in regular physical activity, and attending scheduled follow-up appointments. Adhering to post-treatment care ensures optimal recovery and long-term management of your BPH.
Monitoring for Recurrence or Progression
Even after successful treatment, it is crucial to monitor for any recurrence or progression of BPH symptoms. Regular self-assessment and awareness of changes in urinary symptoms can help detect any potential issues early. If you notice a worsening of symptoms or any new concerns, it is important to consult your healthcare provider promptly to determine the appropriate course of action.
Future Research and Innovations
Advancements in Treatment Approaches
Ongoing research aims to further advance the treatment approaches for BPH. New minimally invasive procedures and surgical techniques continue to be developed to improve patient outcomes and reduce recovery time. Additionally, studies are exploring novel medications and combination therapies to enhance symptom relief and minimize side effects.
Potential Breakthroughs in Preventive Measures
Research also focuses on identifying potential breakthroughs in preventive measures for BPH. Investigating the role of lifestyle modifications, dietary interventions, and targeted medical treatments may help identify strategies to delay the onset or slow the progression of BPH. Continued research in the field of prostate health holds promise for improved prevention strategies in the future.
In conclusion, understanding benign prostatic hyperplasia is essential for men, especially as they age. By recognizing the causes, risk factors, symptoms, and available treatment options, individuals can actively manage their BPH and maintain a good quality of life. With appropriate diagnosis, lifestyle modifications, medications, minimally invasive treatments, or surgical interventions, men can effectively manage BPH and minimize its impact on their daily lives. Regular check-ups, post-treatment care, and ongoing research will continue to guide advancements in the field and improve the management and prevention of this common condition.