Are you a nurse looking for valuable insights on how to effectively manage patients with metabolic syndrome? Look no further! In this article, we will discuss essential nursing considerations and management strategies for individuals diagnosed with metabolic syndrome. From understanding the underlying causes to implementing lifestyle modifications, we will guide you through the steps needed to provide optimal care and support for your patients. So, let’s dive right in and explore the world of nursing considerations for metabolic syndrome!

Overview of Metabolic Syndrome
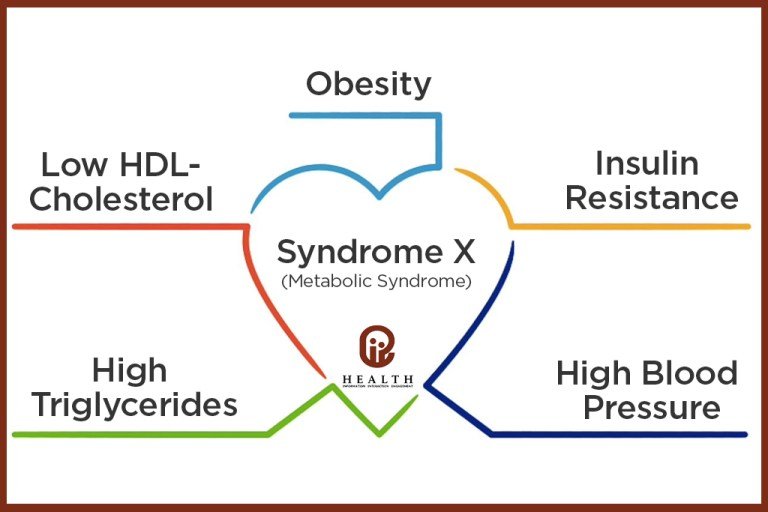
Metabolic syndrome is a cluster of conditions that occur together and increase the risk of heart disease, stroke, and diabetes. The diagnostic criteria for metabolic syndrome include having three or more of the following: elevated waist circumference, elevated blood pressure, elevated fasting blood sugar, elevated triglyceride levels, and reduced HDL cholesterol. These criteria serve as a basis for identifying individuals who may be at risk for developing metabolic syndrome.
The prevalence of metabolic syndrome has been steadily increasing worldwide, and it is estimated that one in four adults in the United States has metabolic syndrome. Several risk factors contribute to the development of metabolic syndrome, including obesity, physical inactivity, poor dietary habits, and genetics. Age, ethnicity, and certain medical conditions such as polycystic ovary syndrome and non-alcoholic fatty liver disease also increase the risk of developing metabolic syndrome.
Complications of metabolic syndrome include an increased risk of cardiovascular disease, type 2 diabetes, and non-alcoholic fatty liver disease. Co-morbidities commonly associated with metabolic syndrome include sleep apnea, certain cancers, and mental health disorders such as depression and anxiety.
Nursing Assessment
A thorough medical history is essential in assessing patients with metabolic syndrome. It is important to inquire about any existing medical conditions, family history of cardiovascular disease or diabetes, and lifestyle habits such as smoking and alcohol consumption. Understanding the patient’s medical history provides valuable information for developing an individualized care plan.
Physical examination plays a vital role in assessing patients with metabolic syndrome. Measurement of waist circumference, blood pressure, and body mass index (BMI) are essential components of the physical examination. Furthermore, a comprehensive examination includes assessing the patient’s cardiovascular, respiratory, and musculoskeletal systems. Physical examination findings provide critical information for identifying potential complications and guiding treatment interventions.
Laboratory and diagnostic tests are crucial for evaluating the metabolic profile of patients with metabolic syndrome. Fasting blood glucose levels, lipid profile, and liver function tests help identify abnormalities and guide treatment decisions. Additionally, imaging studies such as echocardiography and abdominal ultrasound may be performed to assess cardiovascular and hepatic health, respectively.

Patient Education
Patient education plays a pivotal role in the management of metabolic syndrome. Dietary recommendations focus on promoting a healthy and balanced diet that is low in saturated fat, cholesterol, and sodium. Encouraging the consumption of fruits, vegetables, whole grains, and lean protein sources is essential for maintaining optimal health. Portion control, meal planning, and reading food labels are key aspects of dietary education.
Physical activity guidelines emphasize the importance of engaging in regular exercise to promote weight loss, improve cardiovascular health, and enhance insulin sensitivity. Encouraging aerobic exercises, such as brisk walking or cycling, along with resistance training helps patients meet recommended physical activity levels. Individualized exercise plans tailored to the patient’s abilities and preferences are essential for long-term adherence.
Lifestyle modifications encompass various aspects of a patient’s daily routine, beyond diet and exercise. Educating patients about the importance of stress management, adequate sleep, and smoking cessation can significantly improve their overall health. Providing resources and support to help patients make sustainable lifestyle changes is crucial in the management of metabolic syndrome.
Monitoring and Evaluation
Blood pressure control is a critical component of managing metabolic syndrome. Regular monitoring of blood pressure levels allows for early detection and intervention for hypertension. Lifestyle modifications, such as dietary changes and physical activity, are the first-line interventions for blood pressure control. If necessary, pharmacological interventions may be prescribed to achieve target blood pressure goals.
Blood glucose management is another vital aspect of metabolic syndrome management. Regular monitoring of blood glucose levels helps identify any fluctuations and guides treatment decisions. Promoting self-monitoring of blood glucose and providing education on symptoms of hyperglycemia or hypoglycemia empowers patients to actively manage their blood sugar levels.
Regular monitoring of lipid profiles is essential in evaluating cardiovascular risk in patients with metabolic syndrome. Assessing levels of total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides helps guide treatment interventions. Lifestyle modifications, such as dietary changes and physical activity, are important in achieving optimal lipid levels. Additionally, lipid-lowering medications may be prescribed to further manage dyslipidemia.
Weight management is a crucial aspect of metabolic syndrome management. Monitoring weight regularly allows for early identification of weight gain or loss and guides treatment decisions. Encouraging patient adherence to dietary and physical activity recommendations supports weight loss or maintenance.
Psychosocial assessment is an important component of monitoring and evaluation in patients with metabolic syndrome. Assessing for signs of depression, anxiety, or other mental health disorders is crucial in providing holistic care. Identifying psychological factors that may impact patient adherence to treatment recommendations allows for appropriate interventions and support.

Pharmacological Interventions
Anti-hypertensive medications are commonly prescribed to patients with metabolic syndrome. These medications help to lower blood pressure and decrease the risk of cardiovascular complications. Medications such as angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), beta-blockers, and diuretics are commonly used in the management of hypertension associated with metabolic syndrome.
Anti-diabetic medications, such as metformin, are often prescribed for individuals with metabolic syndrome and impaired glucose tolerance or type 2 diabetes. These medications help improve insulin sensitivity and glucose control, reducing the risk of diabetes-related complications.
Lipid-lowering agents, such as statins, are frequently prescribed to manage dyslipidemia in patients with metabolic syndrome. These medications help reduce LDL cholesterol levels and decrease the risk of cardiovascular events.
Collaborative Care
The management of metabolic syndrome requires a collaborative and interdisciplinary approach. Healthcare professionals from various disciplines, including nurses, physicians, dietitians, and pharmacists, work together to provide comprehensive care to patients. By pooling their knowledge and expertise, the healthcare team can develop individualized care plans that address the specific needs of each patient.
Referrals to specialists may be necessary when managing metabolic syndrome. Cardiovascular specialists, endocrinologists, and dietitians may be consulted to provide specialized care and guidance in managing cardiovascular risk factors and optimizing metabolic control. Collaboration with these specialists ensures that patients receive the most appropriate and tailored interventions.
Care coordination and communication are vital in supporting patients with metabolic syndrome. Nurses play a pivotal role in ensuring that the patient’s care is well-coordinated and that all healthcare providers are informed about the patient’s progress and treatment plan. Effective communication between the patient, family members, and the healthcare team promotes continuity of care and enhances patient outcomes.

Patient Monitoring and Follow-up
Regular check-ups are essential in monitoring the progress and managing metabolic syndrome. These check-ups allow for the assessment of vital signs, weight, and other relevant parameters. Monitoring changes in blood pressure, blood glucose levels, and lipid profiles enables healthcare providers to make informed decisions regarding treatment interventions.
Compliance assessment is an important aspect of patient monitoring and follow-up. Evaluating the patient’s adherence to lifestyle modifications, medication regimens, and follow-up appointments helps identify any barriers and provides opportunities for intervention. Providing education, support, and resources to promote compliance is crucial in achieving positive outcomes.
Medication adherence is a key component of managing metabolic syndrome. Regular follow-up appointments allow healthcare providers to assess medication adherence and address any concerns or challenges the patient may have. Educating patients about the importance of taking medications as prescribed and addressing any side effects or concerns enhances medication adherence.
Promotion of Self-care
Encouraging healthy lifestyle choices is a cornerstone of self-care in managing metabolic syndrome. Providing education on nutrition, physical activity, and stress management empowers patients to take charge of their health. Offering resources such as healthy recipes, exercise programs, and stress-reduction techniques helps patients make informed decisions and sustain healthy habits.
Monitoring and managing symptoms are important aspects of self-care for individuals with metabolic syndrome. Educating patients about the signs and symptoms of cardiovascular events, hyperglycemia, or hypoglycemia helps them recognize and respond to potential complications. Empowering patients to monitor their own symptoms and seek timely medical attention promotes early intervention and better outcomes.
Supporting behavioral changes is essential in promoting self-care for patients with metabolic syndrome. Recognizing the challenges and barriers patients face when making lifestyle modifications and providing ongoing support is crucial. Encouraging patients to set achievable goals, celebrating their successes, and providing positive reinforcement enhances their ability to sustain behavioral changes.
Preventing Complications
Education on early warning signs is crucial in preventing complications associated with metabolic syndrome. Patients should be educated on the signs and symptoms of cardiovascular events, such as chest pain, shortness of breath, and sudden weakness or numbness. Timely recognition of these symptoms prompts appropriate medical intervention and reduces the risk of complications.
Regular screenings for cardiovascular risk factors, such as blood pressure, blood glucose, and lipid levels, are essential in preventing complications. Routine monitoring allows healthcare providers to detect abnormalities early and intervene promptly. Regular screenings also provide an opportunity to reinforce patient education on lifestyle modifications and motivate patients to maintain healthy habits.
Managing co-morbidities is an integral part of preventing complications in patients with metabolic syndrome. Identifying and treating conditions such as sleep apnea, non-alcoholic fatty liver disease, and mental health disorders reduces the risk of complications and improves overall health. Collaboration with specialists and regular monitoring of co-morbidities ensures timely interventions and optimal health outcomes.
Addressing Psychological Impact
Psychosocial support is crucial in addressing the psychological impact of metabolic syndrome. Nurses play a vital role in providing emotional support and counseling to patients and their families. Creating a supportive and non-judgmental environment allows patients to express their concerns and fears. Offering empathy, active listening, and validation helps patients cope with the emotional challenges associated with metabolic syndrome.
Counseling and coping strategies are essential in addressing the psychological impact of metabolic syndrome. Providing patients with resources and techniques to manage stress, anxiety, and depression enhances their ability to cope with the challenges of living with metabolic syndrome. Encouraging patients to join support groups or seek professional counseling can provide additional support and guidance.
In conclusion, nursing considerations for metabolic syndrome encompass various aspects of patient care, including assessment, education, monitoring, and collaboration with other healthcare professionals. By providing comprehensive care, empowering patients with knowledge and resources, and promoting self-care, nurses can play a pivotal role in supporting individuals with metabolic syndrome and reducing the risk of complications.