Living with scalp psoriasis can be a challenging experience, but with proper nursing considerations and management, you can effectively cope with this condition. From understanding the causes and symptoms to implementing soothing treatments and lifestyle adjustments, this article provides valuable insights and practical tips to help you navigate through your scalp psoriasis journey. With the support and guidance of nurses, you can find relief and improve your overall well-being, ensuring a happier and more confident you.

Assessment
Physical assessment
During the physical assessment, the nurse will thoroughly examine the patient’s scalp to assess the severity and extent of the psoriasis plaques. They will look for redness, scaling, thickening of the skin, and the presence of silvery-white scales. The nurse will also assess for any signs of infection, such as pustules or crusts. Additionally, they will assess the patient’s hair and hair follicles for any abnormalities or hair loss.
Symptom assessment
The nurse will conduct a thorough symptom assessment by asking the patient about their experience with scalp psoriasis. They will inquire about the presence and intensity of itching, burning, pain, and tenderness. The nurse will also assess any factors that may worsen or alleviate the symptoms, such as stress, environmental changes, or certain hair care products. Understanding the patient’s specific symptoms is crucial for developing an individualized treatment plan.
Psychosocial assessment
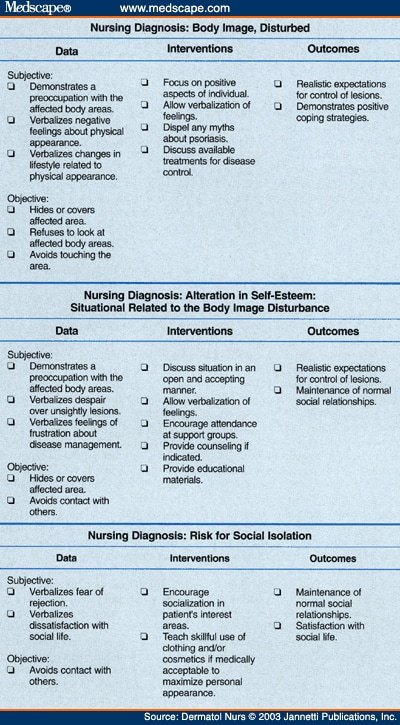
Apart from the physical symptoms, scalp psoriasis can significantly affect a person’s psychosocial well-being. The nurse will conduct a psychosocial assessment to evaluate the impact of scalp psoriasis on the patient’s emotional state, self-esteem, body image, and overall quality of life. This assessment will involve asking open-ended questions and actively listening to the patient’s concerns. It is essential for the nurse to provide a supportive and non-judgmental environment during this assessment.
Diagnosis
Medical history review
To establish a diagnosis, the nurse will review the patient’s medical history, including any previous diagnoses and treatments for psoriasis or other skin conditions. They will gather information about the onset, duration, and progression of scalp psoriasis, as well as any triggers or exacerbating factors. The nurse will also inquire about the patient’s family history of psoriasis or other autoimmune disorders, as there may be a genetic predisposition.
Physical examination
A physical examination is crucial for a comprehensive diagnosis. The nurse will thoroughly examine the patient’s scalp, using a combination of visual inspection and palpation. They will assess the size, shape, and distribution of the psoriasis plaques, as well as the presence of any secondary infections. The nurse will also assess other areas of the body for signs of psoriasis, as scalp psoriasis is often associated with systemic involvement.
Collaborative diagnosis
After conducting a thorough assessment and reviewing the medical history, the nurse will collaborate with the healthcare team, particularly dermatologists, to establish a diagnosis. This collaborative diagnosis takes into account the findings from the physical assessment, symptom assessment, and medical history review. The healthcare team may also rely on additional diagnostic tests, such as skin biopsies, if necessary.
Treatment
Topical treatments
Topical treatments are often the first line of treatment for scalp psoriasis. The nurse will educate the patient on various topical medications, such as corticosteroids, calcipotriol, tazarotene, and coal tar preparations. They will teach the patient how to properly apply these medications to the scalp, ensuring even coverage and avoiding excessive use. The nurse will also provide instructions on potential side effects, like skin thinning or irritation, and how to manage them.
Systemic treatments
In more severe cases or when topical treatments are ineffective, systemic treatments may be necessary. The nurse will collaborate with the healthcare team to educate the patient on oral or injectable medications, such as methotrexate, cyclosporine, or biologic agents. They will explain the benefits and potential risks associated with these treatments. The nurse will also closely monitor the patient’s response to the systemic treatment and report any adverse effects to the healthcare provider.
Scalp-specific treatments
Scalp-specific treatments are essential for managing scalp psoriasis effectively. The nurse may recommend specialized shampoos containing ingredients like salicylic acid or ketoconazole to reduce scaling and itching. They will instruct the patient on proper shampooing techniques, ensuring that the scalp is thoroughly cleansed and the product is left on for the recommended time. The nurse will also provide guidance on how frequently to use these scalp-specific treatments for optimal results.
Combination therapies
In some cases, the nurse may recommend a combination of topical, systemic, and scalp-specific treatments to effectively manage scalp psoriasis. They will work closely with the healthcare team to develop an individualized treatment plan that addresses the unique needs of the patient. The nurse will educate the patient on the different treatment modalities, their mechanisms of action, and the importance of adherence to the prescribed treatment regimen.
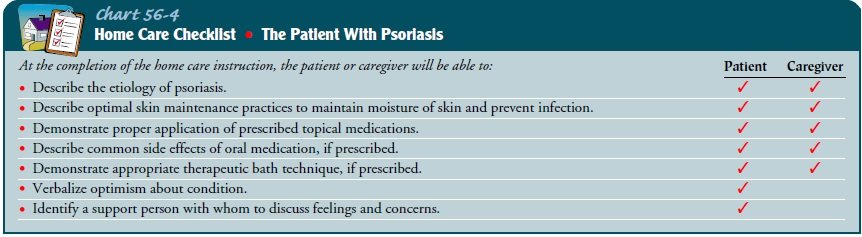
Education
Patient education on scalp psoriasis
Education plays a crucial role in managing scalp psoriasis, and the nurse has a pivotal role in providing thorough patient education. The nurse will explain the chronic nature of scalp psoriasis, emphasizing that it is a lifelong condition that requires long-term management. They will educate the patient about the potential triggers and exacerbating factors, such as stress, weather changes, or certain medications, and how to identify and avoid them.
Teaching self-care techniques
To empower the patient in managing their scalp psoriasis, the nurse will teach self-care techniques. This includes proper scalp hygiene, such as gentle shampooing and avoiding excessive scratching. The nurse will also educate the patient about the importance of moisturizing the scalp regularly to prevent dryness and itchiness. Additionally, they will provide guidance on how to recognize early signs of a flare-up and intervene promptly to prevent worsening of symptoms.
Advising on lifestyle modifications
The nurse will advise the patient on certain lifestyle modifications that can alleviate scalp psoriasis symptoms. This may include stress reduction techniques, such as mindfulness exercises or engaging in relaxing activities. The nurse will also encourage the patient to maintain a balanced diet, rich in fruits, vegetables, and omega-3 fatty acids, as nutrition plays a role in overall skin health. Additionally, the nurse may recommend keeping a symptom diary to identify patterns and triggers.

Psychosocial support
Counseling for stress management
Given the psychosocial impact of scalp psoriasis, the nurse will provide counseling for stress management. They will teach the patient stress reduction techniques, such as deep breathing exercises, meditation, or engaging in hobbies they enjoy. The nurse will also encourage the patient to seek support from loved ones and engage in activities that promote relaxation and emotional well-being.
Support groups and therapy
Connecting patients with support groups can provide valuable emotional support and validation. The nurse will provide information about local or online support groups where individuals with scalp psoriasis can share their experiences and receive encouragement from others who understand their challenges. If necessary, the nurse may refer the patient to a mental health professional for individual therapy to address any underlying emotional distress.
Referral to mental health professionals
In some cases, the impact of scalp psoriasis on a patient’s mental health may require intervention from mental health professionals. The nurse will assess the patient for signs of anxiety, depression, or other mental health conditions. If necessary, they will refer the patient to a psychologist or psychiatrist who can provide comprehensive mental health assessment and support.
Monitoring and Follow-up
Monitoring treatment effectiveness
The nurse plays a vital role in monitoring the effectiveness of the treatment for scalp psoriasis. They will assess the patient regularly, looking for improvements in symptom severity, reduction in scaling, and decreased scalp redness. The nurse will also evaluate the patient’s response to different treatment modalities and make appropriate recommendations and adjustments in collaboration with the healthcare team.
Assessing for treatment side effects
As with any medical intervention, scalp psoriasis treatments can have potential side effects. The nurse will promptly assess the patient for any adverse reactions, such as skin irritation, allergic reactions, or systemic effects from oral medications. They will educate the patient on common side effects, their management, and the importance of reporting any concerning symptoms to the healthcare provider.
Tracking disease progress
Long-term management of scalp psoriasis requires tracking disease progress over time. The nurse will document the patient’s initial presentation and continuously monitor the size, distribution, and severity of the psoriasis plaques. They will also assess the impact of different treatment modalities on the disease progression and adjust the treatment plan accordingly. Regular documentation allows for better evaluation of treatment efficacy and helps guide future interventions.
Regular follow-up appointments
Maintaining regular follow-up appointments is essential for ongoing management of scalp psoriasis. The nurse will ensure that the patient has scheduled appointments with the dermatologist, primary care provider, or other healthcare professionals involved in their care. They will work with the patient to ensure adherence to follow-up appointments and answer any questions or concerns that may arise in between visits.

Collaboration
Collaborating with dermatologists
The nurse will collaborate closely with dermatologists in managing scalp psoriasis. They will communicate regularly, sharing assessment findings, treatment progress, and any concerns or changes in the patient’s condition. This collaboration ensures continuity of care and allows for the integration of nursing interventions into the overall treatment plan. The nurse may also assist with dermatology procedures, such as skin biopsies or in-office treatments.
Working with interdisciplinary teams
Scalp psoriasis management often involves a multidisciplinary approach. The nurse will collaborate with other healthcare professionals, such as pharmacists, physical therapists, and occupational therapists, to ensure holistic care. This collaboration may involve sharing important patient information, coordinating treatments, and developing comprehensive care plans that address not only the scalp psoriasis but also any underlying health conditions.
Coordinating care with other healthcare providers
Coordinating care with other healthcare providers is crucial to optimize the management of scalp psoriasis. The nurse will communicate with the patient’s primary care provider, specialists, and other involved healthcare professionals, ensuring that everyone is aware of the patient’s condition and treatment plan. This coordination helps prevent conflicting or duplicative interventions and enhances the patient’s overall care experience.
Patient Safety
Identifying and correcting barriers to adherence
Patient adherence to the prescribed treatment plan is essential for achieving positive outcomes in scalp psoriasis management. The nurse will assess potential barriers to adherence, such as financial constraints, lack of understanding, or side effects of the medications. They will actively address these barriers, providing appropriate education, connecting the patient with resources, and involving the healthcare team in developing solutions.
Monitoring for potential complications
Scalp psoriasis can be complicated by secondary infections or other dermatological conditions. The nurse will closely monitor the patient for signs of infection, such as increased redness, swelling, or pain. They will assess the scalp regularly for any signs of worsening or the presence of other dermatological conditions, such as seborrheic dermatitis or fungal infections. Identifying potential complications allows for early intervention and prevention of further health issues.
Promoting a safe and clean scalp environment
Ensuring a safe and clean scalp environment is crucial for scalp psoriasis management. The nurse will educate the patient on proper scalp hygiene practices and recommend gentle cleansing techniques. They will provide guidance on avoiding harsh chemicals, excessive heat styling, or scalp trauma that can exacerbate psoriasis. The nurse will also emphasize the importance of regular moisturization to maintain optimal skin health and minimize symptoms.
Special Populations
Pediatric patients
Scalp psoriasis can affect individuals of all ages, including pediatric patients. When caring for pediatric patients with scalp psoriasis, the nurse will need to adapt their approach to meet the child’s developmental and emotional needs. They will involve the parents or caregivers in the education and treatment process, emphasizing the importance of gentle scalp care and reinforcing adherence to the treatment regimen.
Elderly patients
Elderly patients with scalp psoriasis may face unique challenges, such as decreased mobility, impaired vision, or cognitive decline. The nurse will take these factors into consideration when developing the care plan, ensuring that it is tailored to the individual’s specific physical and cognitive abilities. They will also provide additional support and education to the patient’s caregivers to ensure continuity of care and adherence to the treatment plan.
Pregnant or breastfeeding patients
Special consideration must be given to pregnant or breastfeeding patients with scalp psoriasis, as many treatments may pose risks to the developing fetus or the nursing infant. The nurse will work closely with the healthcare team to identify safe treatment options that minimize potential harm. They will educate the patient about the potential risks and benefits of different treatment modalities and ensure that the patient’s obstetrician or pediatrician is involved in the decision-making process.
Research and Evidence-Based Practice
Keeping up-to-date with current research
As healthcare professionals, nurses need to stay informed about the latest research and evidence in scalp psoriasis management. The nurse will regularly review current literature, attend relevant conferences or seminars, and engage in continuing education opportunities. Staying up-to-date with research helps the nurse provide evidence-based care and incorporate the latest advancements into their practice.
Implementing evidence-based interventions
Evidence-based practice is the foundation of quality care in scalp psoriasis management. The nurse will integrate evidence-based interventions into the patient’s care plan, ensuring that interventions are grounded in the best available evidence. This may include utilizing specific treatment modalities, implementing standardized assessment tools, or adapting interventions based on the patient’s unique needs and preferences.
Contributing to research studies
Nurses have the opportunity to contribute to research studies that seek to advance the knowledge and treatment options for scalp psoriasis. The nurse may participate in clinical trials or assist in data collection and analysis. Contributing to research not only enhances the nurse’s professional development but also contributes to the overall body of evidence in scalp psoriasis management, ultimately benefiting future patients.
In conclusion, nursing considerations and management for scalp psoriasis encompass a comprehensive approach that addresses physical assessment, symptom assessment, psychosocial support, diagnosis, treatment, education, patient safety, monitoring, collaboration, special populations, and research. Nurses play a vital role in providing patient-centered care, ensuring adherence to treatment plans, and promoting the overall well-being and quality of life for individuals with scalp psoriasis. By employing evidence-based practices and collaborating with the healthcare team, nurses can make a significant impact in improving outcomes for patients living with scalp psoriasis.