Are you tired of dealing with digestive disorders that disrupt your daily life? Look no further! In this article, you will find valuable tips and information on how to prevent and effectively manage digestive disorders. From dietary changes to lifestyle modifications, we’ve got you covered. Whether you suffer from indigestion, heartburn, or irritable bowel syndrome, these strategies will help you regain control of your digestive health and improve your overall well-being. Say goodbye to unwanted digestive discomfort and say hello to a happier, healthier gut!
Preventing and Managing Digestive Disorders
Digestive disorders can cause a wide range of uncomfortable symptoms and can significantly impact your quality of life. However, there are several steps you can take to prevent and manage these conditions. By maintaining a healthy diet, avoiding trigger foods, eating regularly and moderately, drinking plenty of fluids, getting enough fiber, managing stress levels, exercising regularly, avoiding smoking and excessive alcohol consumption, maintaining a healthy weight, and properly managing medications, you can reduce your risk of developing digestive disorders and effectively manage any existing conditions.
Maintaining a Healthy Diet
One of the most important factors in preventing and managing digestive disorders is maintaining a healthy diet. This means consuming a variety of nutritious foods, including fruits, vegetables, whole grains, lean proteins, and healthy fats. It is also important to limit your intake of processed foods, sugary drinks, and high-fat foods, as these can contribute to digestive issues. Additionally, it is important to eat regular meals and avoid skipping meals, as this can disrupt your digestive system and lead to problems such as bloating and irregular bowel movements.
Avoiding Trigger Foods
Certain foods can trigger digestive symptoms in some individuals. It is important to identify and avoid these trigger foods in order to prevent discomfort and manage digestive disorders. Common trigger foods include spicy foods, fatty foods, caffeine, alcohol, and foods high in artificial sweeteners. Keeping a food diary can help you identify which foods may be causing your symptoms, allowing you to make necessary adjustments to your diet.
Eating Regularly and Moderately
Eating regularly and in moderate portions is important for maintaining a healthy digestive system. It is recommended to consume three main meals per day and to include healthy snacks in between if needed. This helps to regulate your digestive system and prevent issues such as bloating and indigestion. It is also important to take your time when eating, chewing your food thoroughly and allowing your body to properly break down and digest the food.
Drinking Plenty of Fluids
Staying hydrated is essential for good digestive health. Drinking plenty of fluids helps to soften stools and prevent constipation. It is recommended to drink at least eight glasses of water per day, but individual needs may vary. In addition to water, you can also include other hydrating beverages such as herbal tea and diluted fruit juices. However, it is best to limit your intake of sugary and carbonated drinks, as these can exacerbate digestive issues.
Getting Enough Fiber
Fiber plays a crucial role in maintaining a healthy digestive system. It helps to regulate bowel movements, prevent constipation, and promote overall gut health. It is important to include a variety of high-fiber foods in your diet, such as whole grains, fruits, vegetables, legumes, and nuts. If you are unable to meet your fiber needs through diet alone, fiber supplements may be beneficial. However, it is important to gradually increase your fiber intake and drink plenty of fluids to prevent discomfort.
Managing Stress Levels
Stress can have a significant impact on your digestive system. It can lead to issues such as stomachaches, bloating, and diarrhea. Managing stress levels is therefore important for preventing and managing digestive disorders. There are several techniques you can try to help reduce stress, such as deep breathing exercises, meditation, yoga, and engaging in activities that you enjoy. It may also be helpful to seek professional help, such as talking to a therapist or counselor, if you are struggling with chronic stress or anxiety.
Exercising Regularly
Regular physical activity is not only important for overall health but can also benefit your digestive system. Exercise helps to improve digestion and prevent issues such as constipation. Aim for at least 30 minutes of moderate-intensity exercise most days of the week. This can include activities such as brisk walking, jogging, swimming, or cycling. However, it is important to avoid exercising immediately after eating, as this can lead to discomfort.
Avoiding Smoking and Excessive Alcohol Consumption
Both smoking and excessive alcohol consumption can have negative effects on your digestive system. Smoking can increase the risk of developing conditions such as acid reflux and stomach ulcers. Excessive alcohol consumption can lead to inflammation of the stomach lining and liver damage. It is best to avoid smoking altogether and limit your alcohol intake to moderate levels, which is defined as up to one drink per day for women and up to two drinks per day for men.
Maintaining a Healthy Weight
Maintaining a healthy weight is important for preventing and managing digestive disorders. Obesity can contribute to issues such as acid reflux, gallstones, and fatty liver disease. On the other hand, being underweight can lead to nutrient deficiencies and may increase the risk of developing certain digestive conditions. It is important to maintain a balanced diet and engage in regular physical activity to achieve and maintain a healthy weight.
Properly Managing Medications
Certain medications can have adverse effects on the digestive system. It is important to properly manage your medications and carefully follow instructions from your healthcare provider. If you are experiencing digestive symptoms as a result of medication use, it is important to discuss this with your healthcare provider. They may be able to adjust your medication or provide alternative options that are better tolerated by your digestive system.
Understanding Digestive Disorders
There are several different types of digestive disorders, each with its own set of symptoms and treatment options. By understanding these conditions, you can better identify and manage any digestive issues you may be experiencing. The following are some common digestive disorders:
Gastroesophageal Reflux Disease (GERD)
GERD is a chronic condition characterized by frequent acid reflux, which occurs when the acid from the stomach flows back into the esophagus. This can lead to symptoms such as heartburn, regurgitation, and difficulty swallowing. Lifestyle changes, dietary modifications, and medications are commonly used to manage GERD.
Irritable Bowel Syndrome (IBS)
IBS is a common digestive disorder characterized by abdominal pain, bloating, constipation, and/or diarrhea. The exact cause of IBS is unknown, but it is believed to involve changes in the muscles and nerves of the digestive system. Management of IBS typically involves lifestyle changes, dietary modifications, stress management, and, in some cases, medications.
Inflammatory Bowel Disease (IBD)
IBD refers to a group of chronic conditions that cause inflammation in the digestive tract. The two main types of IBD are Crohn’s disease and ulcerative colitis. Symptoms may include abdominal pain, diarrhea, blood in stool, weight loss, and fatigue. Treatment for IBD aims to reduce inflammation and manage symptoms through medication, lifestyle changes, and, in some cases, surgery.
Peptic Ulcers
Peptic ulcers are open sores that develop on the lining of the stomach or small intestine. They are commonly caused by an infection with the bacteria Helicobacter pylori or the overuse of nonsteroidal anti-inflammatory drugs (NSAIDs). Symptoms may include abdominal pain, bloating, heartburn, and nausea. Treatment involves medications to reduce stomach acid, antibiotics to eradicate H. pylori infection, and lifestyle modifications.
Gallstones
Gallstones are hardened deposits that form in the gallbladder. They can range in size and may or may not cause symptoms. When symptoms occur, they often include abdominal pain, bloating, and nausea. Treatment options for gallstones may include medication to dissolve the stones, surgical removal of the gallbladder (cholecystectomy), or other procedures to break up or remove the stones.
Celiac Disease
Celiac disease is an autoimmune disorder in which the body’s immune system reacts to gluten, a protein found in wheat, barley, and rye. This reaction leads to damage to the lining of the small intestine. Symptoms of celiac disease can vary widely and may include abdominal pain, diarrhea, bloating, fatigue, and weight loss. The only effective treatment for celiac disease is a strict gluten-free diet.
Gastritis
Gastritis refers to inflammation of the stomach lining. It can be caused by a bacterial infection, the overuse of NSAIDs, excessive alcohol consumption, or certain autoimmune disorders. Symptoms may include abdominal pain, nausea, vomiting, and indigestion. Treatment for gastritis may involve medications to reduce stomach acid, antibiotics to treat bacterial infections, and lifestyle modifications.
Gastroenteritis
Gastroenteritis, also known as the stomach flu, is an inflammation of the stomach and intestines. It is typically caused by a viral or bacterial infection and can lead to symptoms such as diarrhea, abdominal pain, nausea, vomiting, and fever. Treatment for gastroenteritis involves supportive care, such as staying hydrated and getting plenty of rest.
Hemorrhoids
Hemorrhoids are swollen blood vessels in the rectum or anus. They can be internal or external and may cause symptoms such as rectal bleeding, itching, and pain. Treatment for hemorrhoids may involve lifestyle changes, such as increasing fiber intake and staying hydrated, or medical interventions, such as over-the-counter creams or procedures to remove or shrink the hemorrhoids.
Diverticulitis
Diverticulitis occurs when small pouches called diverticula in the lining of the colon become inflamed or infected. Symptoms may include abdominal pain, fever, nausea, and changes in bowel habits. Treatment for diverticulitis may involve antibiotics, a liquid diet, and, in severe cases, surgery to remove the affected portion of the colon.
It is important to consult with a healthcare provider if you experience persistent or severe symptoms of any digestive disorder. They can provide an accurate diagnosis and develop an appropriate treatment plan tailored to your specific needs. Early intervention is key in managing and preventing complications associated with digestive disorders.

Symptoms and Signs of Digestive Disorders
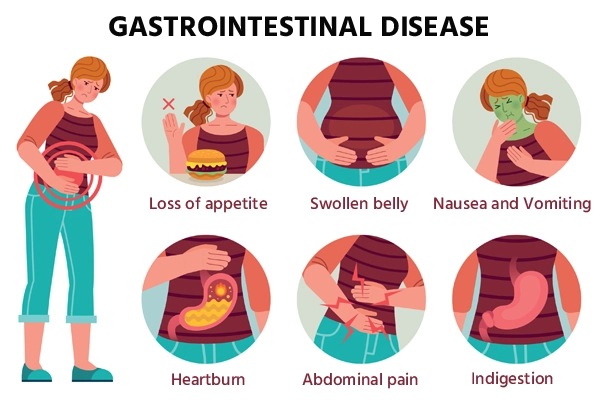
Recognizing the signs and symptoms of digestive disorders is crucial for early intervention and proper management. It is important to be aware of any changes or abnormalities in your digestive system. The following are some common symptoms and signs of digestive disorders:
Heartburn and Acid Reflux
Heartburn and acid reflux are common symptoms of digestive disorders such as GERD. They are characterized by a burning sensation in the chest and throat, often accompanied by a sour or bitter taste in the mouth. These symptoms are caused by the backflow of stomach acid into the esophagus.
Abdominal Pain and Cramping
Abdominal pain and cramping can occur with various digestive disorders, including IBS, IBD, gastritis, and diverticulitis. The pain may be dull, sharp, or cramp-like, and it can range from mild to severe. The location of the pain may vary depending on the specific condition.
Bloating and Excessive Gas
Bloating and excessive gas can be uncomfortable and may be caused by conditions such as IBS, gastritis, and lactose intolerance. These symptoms are often characterized by a feeling of fullness or tightness in the abdomen and the frequent passage of gas.
Diarrhea or Constipation
Both diarrhea and constipation can be symptoms of digestive disorders. Diarrhea is characterized by loose, watery stools, while constipation is characterized by difficulty or infrequency in passing stools. These symptoms can be caused by various conditions, including IBS, IBD, and fecal impaction.
Nausea and Vomiting
Nausea and vomiting can occur with digestive disorders such as gastritis, gastroenteritis, and peptic ulcers. These symptoms are often accompanied by a loss of appetite and can be triggered by certain foods, medications, or other factors.
Blood in Stool
The presence of blood in stool can be a sign of various digestive disorders, including hemorrhoids, peptic ulcers, and inflammatory bowel disease. It is important to seek medical attention if you notice blood in your stool, as it may indicate a serious underlying condition.
Unexplained Weight Loss
Unexplained weight loss can be a cause for concern and may be a sign of a digestive disorder such as celiac disease, IBD, or certain types of cancer. It is important to consult with a healthcare provider if you experience significant and unexplained weight loss.
Fatigue and Weakness
Fatigue and weakness can be symptoms of digestive disorders such as celiac disease, IBD, and malabsorption disorders. These symptoms can be caused by nutrient deficiencies and the body’s inability to properly absorb essential nutrients from food.
Fever and Chills
Fever and chills can indicate an infection or inflammation in the digestive system. These symptoms are often associated with conditions such as gastroenteritis, diverticulitis, and peptic ulcers. It is important to seek medical attention if you experience persistent or high fever accompanied by digestive symptoms.
Difficulty Swallowing
Difficulty swallowing, also known as dysphagia, can be a symptom of digestive disorders such as GERD, esophageal strictures, and certain types of esophageal cancer. This symptom should not be ignored, as it can indicate a narrowing or blockage in the esophagus.
If you experience any of these symptoms or signs of a digestive disorder, it is important to consult with a healthcare provider. They can conduct a thorough evaluation, order any necessary diagnostic tests, and develop an appropriate treatment plan based on your specific symptoms and medical history.
Seeking Medical Evaluation
Knowing when to consult a healthcare provider is crucial for the diagnosis and management of digestive disorders. It is important to seek medical evaluation if you experience persistent or severe symptoms. Additionally, routine screening and check-ups can help detect digestive disorders early on, even before symptoms manifest. The following are important considerations when seeking medical evaluation for digestive disorders:
When to Consult a Healthcare Provider
You should consult a healthcare provider if you experience persistent or severe symptoms, such as chronic abdominal pain, recurring heartburn, unexplained weight loss, or a change in bowel habits that lasts longer than a few weeks. Additionally, if you notice blood in your stool or vomit, have difficulty swallowing, or have a family history of digestive disorders, it is important to seek medical attention.
Routine Screening and Check-ups
Routine screening and check-ups are important, even in the absence of symptoms. Regular visits to your healthcare provider can help detect digestive disorders early on, allowing for prompt intervention and effective management. Your healthcare provider may recommend specific screening tests based on your age, medical history, and risk factors.
Diagnostic Procedures and Tests
If you are experiencing symptoms of a digestive disorder, your healthcare provider may recommend certain diagnostic procedures and tests to accurately diagnose your condition. These may include blood tests, stool tests, imaging tests (such as X-rays or CT scans), endoscopy, colonoscopy, or other specialized tests. These tests can provide valuable information about the state of your digestive system and guide treatment decisions.
Consulting with a Gastroenterologist
A gastroenterologist is a medical specialist who specializes in the diagnosis and treatment of digestive disorders. If your primary care provider suspects a digestive disorder or if your symptoms are not responding to initial treatment, they may refer you to a gastroenterologist. A gastroenterologist has specialized knowledge and experience in managing complex digestive conditions and can provide advanced diagnostic and treatment options.
Importance of Early Intervention
Early intervention is crucial in managing digestive disorders and preventing complications. Many digestive disorders can worsen over time if left untreated. By seeking medical evaluation early on, you increase your chances of receiving timely and effective treatment, which can lead to better outcomes and improved quality of life.
Collaborating in Treatment Planning
It is important to actively participate in the treatment planning process and collaborate with your healthcare provider. Share your symptoms, concerns, and goals, and ask any questions you may have. This collaborative approach ensures that your treatment plan is tailored to your specific needs and preferences.
Monitoring Progress and Response to Treatment
Regular follow-up visits with your healthcare provider are important to monitor your progress and assess your response to treatment. These visits allow for adjustments to your treatment plan if needed and provide an opportunity to address any ongoing or new symptoms.
Managing Persistent or Severe Symptoms
If you are experiencing persistent or severe symptoms despite initial treatment, it is important to communicate this to your healthcare provider. They can reassess your condition, order additional tests if necessary, and explore alternative treatment options.
Seeking Second Opinions
If you are unsure about a diagnosis or treatment plan, or if you simply want a second opinion, it is perfectly acceptable to seek the input of another healthcare provider. Second opinions can provide valuable insights and give you confidence in your treatment decisions.
Considering Surgical Interventions
In some cases, surgical intervention may be required to treat or manage certain digestive disorders. If your healthcare provider recommends surgery, it is important to carefully consider the risks, benefits, and alternatives. Seek clarification on the expected outcomes of the surgery and discuss any concerns you may have.
By actively seeking medical evaluation and engaging in the treatment process, you can effectively manage your digestive disorder and achieve optimal digestive health.

Natural Remedies and Home Care
In addition to medical interventions, there are several natural remedies and home care strategies that can complement the treatment of digestive disorders. These approaches focus on lifestyle modifications, dietary changes, stress management techniques, and alternative therapies. While these remedies may not cure the underlying condition, they can help alleviate symptoms and promote overall digestive health. The following are some natural remedies and home care strategies to consider:
Dietary Modifications
Making dietary modifications can have a significant impact on digestive health. Depending on the specific digestive disorder, certain foods may need to be limited or avoided altogether. For example, individuals with GERD may need to avoid spicy foods, citrus fruits, and fatty foods. Those with IBS may benefit from reducing their intake of high-FODMAP foods, such as certain fruits, vegetables, and grains. Consulting with a registered dietitian can provide guidance on appropriate dietary modifications based on your specific condition.
Probiotics and Digestive Enzymes
Probiotics are beneficial bacteria that can promote a healthy balance of gut flora. They can be consumed through fermented foods such as yogurt, sauerkraut, and kimchi, or in the form of supplements. Digestive enzymes, on the other hand, aid in the breakdown of nutrients and can be beneficial for individuals with conditions such as pancreatic insufficiency. It is important to consult with a healthcare provider before starting any supplementation regimen.
Herbal Remedies and Supplements
Certain herbal remedies and supplements may provide relief for digestive symptoms. For example, peppermint oil has been shown to alleviate symptoms of IBS, while ginger can help reduce nausea and improve digestion. It is important to consult with a healthcare provider or a qualified herbalist before using any herbal remedies or supplements, as they can interact with medications and may not be suitable for everyone.
Stress-Relief Techniques
Stress can have a significant impact on digestive health. Engaging in stress-relief techniques can help reduce symptoms and manage digestive disorders. Techniques such as deep breathing exercises, meditation, yoga, and progressive muscle relaxation can help promote relaxation and reduce stress levels. Finding activities that you enjoy, such as hobbies or spending time with loved ones, can also be beneficial in managing stress.
Hygienic Practices and Personal Care
Practicing good hygiene and personal care is essential for preventing and managing digestive disorders. This includes regular handwashing, especially before eating and after using the restroom, to reduce the spread of harmful bacteria and viruses. It is also important to properly handle and prepare food to avoid foodborne illnesses.
Acupuncture and Acupressure
Acupuncture and acupressure are traditional Chinese medical practices that involve stimulating specific points on the body to promote healing and relieve symptoms. These techniques have been used for centuries to manage various health conditions, including digestive disorders. While research on the effectiveness of acupuncture and acupressure for digestive disorders is limited, some individuals report symptom improvement with these approaches. It is important to seek treatment from a licensed and experienced practitioner.
Safe Pain Management
For individuals with chronic digestive disorders, safe pain management is important. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and aspirin, can worsen symptoms and should be avoided or used with caution. Your healthcare provider can recommend appropriate pain relief options, such as acetaminophen or prescription medications, that are safe for your specific condition.
Alternative Therapies: Yoga and Meditation
Engaging in alternative therapies such as yoga and meditation can have a positive impact on digestive health. Yoga combines physical postures, breathing exercises, and meditation to promote relaxation, improve digestion, and reduce stress. Meditation, on its own, can also help alleviate symptoms of digestive disorders by reducing inflammation and promoting overall well-being.
Physical Therapy and Exercise
For individuals with certain digestive disorders, such as functional bowel disorders or pelvic floor dysfunction, physical therapy may be beneficial. Physical therapists can provide exercises and techniques to improve muscle strength and coordination in the pelvic floor and abdominal muscles, which can help alleviate symptoms and improve bowel function. Engaging in regular physical activity, such as walking or swimming, can also support overall digestive health.
Sleep Hygiene and Restful Practices
Getting adequate sleep and practicing good sleep hygiene is important for overall health, including digestive health. Poor sleep can disrupt digestion and worsen symptoms of digestive disorders. Establishing a regular sleep schedule, creating a relaxing bedtime routine, and creating a comfortable sleep environment can all contribute to restful sleep and improved digestive health.
It is important to note that while natural remedies and home care strategies can be effective in managing symptoms, they should not replace medical treatment or advice from a healthcare provider. Consulting with a healthcare provider before using any natural remedies or home care strategies is essential to ensure safety and effectiveness.
Medications for Digestive Disorders
Medications play a crucial role in the management of digestive disorders. They can help alleviate symptoms, reduce inflammation, control acid production, and promote healing of the digestive system. The specific medications prescribed will depend on the type and severity of the digestive disorder. The following are some commonly used medications for digestive disorders:
Antacids and Acid Reducers
Antacids, such as calcium carbonate and magnesium hydroxide, neutralize stomach acid and provide temporary relief from heartburn and indigestion. Acid reducers, such as histamine H2-receptor antagonists (H2 blockers) and proton pump inhibitors (PPIs), work by reducing the production of stomach acid. These medications are commonly used in the treatment of conditions such as GERD, peptic ulcers, and gastritis.
Proton Pump Inhibitors
Proton pump inhibitors (PPIs) are a class of medications that block the production of stomach acid. They are often prescribed for conditions such as GERD, peptic ulcers, and Barrett’s esophagus. PPIs can provide long-lasting relief from symptoms and promote healing of the esophagus and stomach lining. It is important to use PPIs as directed and for the shortest duration necessary, as prolonged use can have side effects.
H2 Blockers
Histamine H2-receptor antagonists, commonly known as H2 blockers, reduce the production of stomach acid. They are often used to treat conditions such as GERD, peptic ulcers, and gastritis. H2 blockers provide relief from symptoms such as heartburn and can promote healing of the stomach lining. They are available over-the-counter or as prescription strength and can be taken as needed or on a regular basis.
Antibiotics and Antimicrobial Agents
Antibiotics and antimicrobial agents are used to treat bacterial infections that may be causing or contributing to digestive disorders. For example, Helicobacter pylori infection is a common cause of peptic ulcers and gastritis. Antibiotics are used in combination with other medications to eradicate the infection and promote healing of the stomach lining.
Anti-Inflammatory Drugs
Anti-inflammatory drugs, such as corticosteroids and 5-aminosalicylates, are used to reduce inflammation in conditions such as inflammatory bowel disease (IBD). They help to alleviate symptoms and reduce the risk of complications. These medications may be taken orally or administered through injection or suppository, depending on the specific condition and severity.
Anti-Spasmodic Medications
Anti-spasmodic medications help to relieve spasms in the digestive tract and can provide relief from symptoms such as abdominal pain and cramping. These medications are commonly used in the treatment of conditions such as IBS. They work by relaxing the muscles in the intestines and can be taken as needed or on a regular basis.
Biologic Therapies
Biologic therapies are a relatively new class of medications that target specific molecules involved in the immune response. They are used in the treatment of certain digestive disorders, such as Crohn’s disease and ulcerative colitis. These medications can help reduce inflammation, alleviate symptoms, and promote healing of the digestive tract.
Laxatives and Anti-Diarrheal Agents
Laxatives and anti-diarrheal agents are used to manage symptoms such as constipation or diarrhea. Laxatives can help soften stools and promote regular bowel movements, while anti-diarrheal agents can help slow down bowel movements and reduce the frequency of loose stools. It is important to use these medications as directed and consult with a healthcare provider if symptoms persist.
Anti-Nausea Medications
For individuals experiencing nausea and vomiting, anti-nausea medications may be prescribed. These medications work by blocking certain receptors in the brain that trigger nausea and can provide relief from symptoms. They may be taken orally, through injection, or in suppository form, depending on the severity of symptoms.
Pain Relief Medications
Pain relief medications, such as acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs), may be prescribed to manage abdominal pain associated with certain digestive disorders. However, it is important to use NSAIDs with caution, as they can worsen symptoms in some individuals. Your healthcare provider can recommend appropriate pain relief options based on your specific condition.
It is important to follow the prescribed medication regimen as directed by your healthcare provider. Should you experience any side effects or concerns, it is essential to communicate them to your healthcare provider. They can reassess your treatment plan and make any necessary adjustments to ensure your digestive health is effectively managed.
Surgical Interventions for Digestive Disorders
In some cases, surgical intervention may be necessary to treat or manage certain digestive disorders. Surgical procedures can help alleviate symptoms, correct anatomical abnormalities, or remove diseased tissues or organs. The decision to undergo surgery is typically made after careful consideration of the individual’s condition, symptoms, response to non-surgical treatments, and potential risks and benefits. The following are some surgical interventions for digestive disorders:
Fundoplication for GERD
Fundoplication is a surgical procedure used to treat severe cases of gastroesophageal reflux disease (GERD) that do not respond to medication or lifestyle modifications. The procedure involves wrapping the upper part of the stomach around the lower esophageal sphincter to reinforce the barrier between the stomach and esophagus, preventing acid reflux.
Colectomy for IBD
Colectomy is a surgical procedure that involves the removal of all or part of the colon (large intestine). It is performed in cases of severe or extensive inflammation in individuals with inflammatory bowel disease (IBD), such as ulcerative colitis or Crohn’s disease, that do not respond to medical treatment. The procedure may be done as an open surgery or using minimally invasive techniques.
Sphincterotomy for Gallstones
Sphincterotomy is a procedure used to treat gallstones that are causing symptoms or complications. It involves making a small incision in the muscle of the sphincter of Oddi, which controls the flow of bile and pancreatic juice into the small intestine. This allows for the passage of gallstones and relieves symptoms.
Hemorrhoidectomy for Hemorrhoids
Hemorrhoidectomy is a surgical procedure used to remove hemorrhoids, which are swollen blood vessels in the rectum or anus. It is performed in cases of severe or recurring hemorrhoids that do not respond to non-surgical treatments. The procedure involves the complete removal of the hemorrhoids and is typically done under anesthesia.
Appendectomy for Appendicitis
Appendectomy is a surgical procedure used to remove the appendix, usually due to acute appendicitis. The appendix is a small, finger-like organ attached to the large intestine. If it becomes inflamed or infected, it can lead to severe abdominal pain and other symptoms. Appendectomy is typically performed as an emergency procedure to prevent complications such as appendiceal rupture.
Gastrectomy for Stomach Cancer
Gastrectomy is a surgical procedure used to remove all or part of the stomach in individuals with stomach cancer. Depending on the extent of the cancer, the surgery may involve removing only a portion of the stomach (partial gastrectomy) or the entire stomach (total gastrectomy). Reconstruction of the digestive tract is also done to allow for the passage of food.
Total Pancreatectomy for Pancreatitis
Total pancreatectomy is a surgical procedure used to remove the entire pancreas. It is performed in cases of severe chronic pancreatitis that do not respond to medical treatment or for certain types of pancreatic cancer. Following this procedure, individuals require lifelong pancreatic enzyme replacement therapy and insulin to manage digestion and blood sugar levels.
Colostomy or Ileostomy for Bowel Obstruction
Colostomy or ileostomy is a surgical procedure that involves creating an opening in the abdomen to allow waste to exit the body when normal bowel function is compromised. It is commonly done in cases of bowel obstruction, such as in advanced stages of cancer or inflammatory bowel disease. The procedure involves diverting the fecal flow to a stoma, where it is collected in a pouch attached to the abdomen.
Liver Transplantation for Liver Disease
Liver transplantation is a surgical procedure performed in individuals with end-stage liver disease or certain liver cancers. It involves replacing the diseased liver with a donor liver. Liver transplantation is a complex and specialized surgery that requires a thorough evaluation and coordination with a transplant center.
Esophageal Dilation for Strictures
Esophageal dilation is a procedure used to widen a narrowed or constricted portion of the esophagus, usually due to scar tissue formation (stricture). It is commonly performed in individuals with conditions such as GERD, eosinophilic esophagitis, or damage to the esophagus caused by radiation therapy. The procedure involves gently stretching the esophagus using specialized instruments.
It is important to discuss the potential risks, benefits, and expected outcomes of any surgical procedure with your healthcare provider. They can provide you with the necessary information and support to make an informed decision about your treatment options.
Lifestyle Adjustments and Self-Care
In addition to medical treatments and interventions, making lifestyle adjustments and practicing self-care can have a significant impact on the prevention and management of digestive disorders. These lifestyle adjustments focus on maintaining a healthy diet, practicing mindful eating, managing stress levels, engaging in regular physical activity, getting adequate sleep and rest, avoiding triggers and allergens, maintaining hygiene and sanitation, and reducing or eliminating smoking and excessive alcohol intake. The following are some lifestyle adjustments and self-care strategies to consider:
Meal Planning and Portion Control
Meal planning involves preparing and organizing meals and snacks in advance to ensure a balanced and nutritious diet. It can help prevent impulsive food choices and excessive portion sizes, which can contribute to digestive issues. Portion control involves being mindful of portion sizes and listening to your body’s hunger and fullness cues.
Eating Mindfully and Slowly
Practicing mindful eating involves paying attention to the sensory experience of eating and being fully present during meals. This includes savoring the flavors, textures, and smells of food, and eating slowly to allow for proper digestion and improved satisfaction. Mindful eating can help prevent overeating and promote better digestion.
Chewing Thoroughly
Chewing food thoroughly is an important part of the digestion process. Properly chewing food allows for better breakdown of nutrients and aids in digestion. Take your time when eating and aim to chew each bite thoroughly before swallowing.
Keeping a Food Diary
Keeping a food diary can help identify potential trigger foods or patterns that may be contributing to digestive symptoms. Record the foods you eat, portion sizes, and any symptoms or reactions you experience. This can help you pinpoint specific foods or combinations that may be causing issues and make necessary adjustments to your diet.
Regular Physical Activity and Exercise
Engaging in regular physical activity and exercise can have numerous benefits for digestive health. Exercise helps to stimulate digestion, promote regular bowel movements, and reduce stress levels. Aim for at least 30 minutes of moderate-intensity exercise most days of the week, such as brisk walking, jogging, swimming, or cycling.
Creating a Relaxing Routine
Creating a relaxing routine can help manage stress levels and promote optimal digestive health. Incorporate activities such as meditation, deep breathing exercises, yoga, or reading into your daily routine to promote relaxation and reduce stress levels. Find activities that you enjoy and that help you unwind.
Adequate Sleep and Rest
Getting enough sleep and rest is important for overall health and well-being, including digestive health. Aim for 7-8 hours of quality sleep each night and establish a regular sleep schedule. Creating a bedtime routine and creating a comfortable sleep environment can help improve sleep quality.
Avoiding Triggers and Allergens
Identifying and avoiding triggers and allergens can help alleviate symptoms of digestive disorders. Keep track of any foods, drinks, or environmental factors that seem to trigger your symptoms and make necessary adjustments to avoid them. This may involve avoiding certain foods, using fragrance-free or hypoallergenic products, or ensuring proper ventilation in your living space.
Maintaining Hygiene and Sanitation
Maintaining good hygiene and sanitation is crucial for preventing digestive infections and promoting optimal digestive health. Wash your hands thoroughly with soap and water before eating and after using the restroom. Practice proper food handling and preparation techniques to reduce the risk of contamination and foodborne illnesses.
Quitting Smoking and Reducing Alcohol Intake
Smoking and excessive alcohol consumption can have a negative impact on digestive health. Smoking can increase the risk of developing conditions such as GERD, stomach ulcers, and certain types of cancer. Excessive alcohol intake can lead to inflammation of the stomach lining and liver damage. Quitting smoking and reducing alcohol intake can significantly improve digestive health.
Making these lifestyle adjustments and practicing self-care can have a positive impact on the prevention and management of digestive disorders. It is important to consult with a healthcare provider or a registered dietitian for personalized recommendations and guidance based on your specific condition and needs.

Support and Resources for Digestive Disorders
Living with a digestive disorder can be challenging, both physically and emotionally. However, there are numerous resources and support networks available to provide information, education, and emotional support. These resources can help individuals better understand their condition, connect with others facing similar challenges, and navigate the healthcare system. The following are some support and resources for digestive disorders:
Patient Support Groups
Patient support groups, either in-person or online, provide a platform for individuals with digestive disorders to connect, share experiences, and provide emotional support. These groups can be valuable sources of information, empathy, and encouragement. They may also provide opportunities for educational events or guest speakers.
Online Communities and Forums
Online communities and forums dedicated to digestive disorders allow individuals to seek information, ask questions, and share their experiences. These platforms can provide a sense of community and support, especially for individuals who may not have access to local support groups or medical specialists.
Educational Materials and Brochures
Educational materials and brochures are often available through healthcare providers, patient advocacy organizations, and digestive health clinics. These resources provide information on various digestive disorders, symptoms, treatment options, and lifestyle management strategies. They can help individuals better understand their condition and make informed decisions about their health.
National and International Associations
National and international associations, such as the American Gastroenterological Association (AGA), Crohn’s and Colitis Foundation, and American Liver Foundation, provide valuable resources, support, and advocacy for individuals with digestive disorders. These associations often have websites with comprehensive information on specific digestive disorders, expert guidelines, research updates, and opportunities for community involvement.
Helplines and Hotlines
Helplines and hotlines offer a direct line of support and information for individuals with digestive disorders. Trained professionals can provide guidance, answer questions, and offer emotional support. Many national and local organizations have helplines dedicated to specific digestive disorders.
Patient Navigators and Advocates
Patient navigators and advocates can assist individuals with digestive disorders in navigating the healthcare system and accessing appropriate care. They can provide guidance on finding healthcare providers, understanding insurance coverage, and connecting with support services. These professionals can be instrumental in ensuring individuals receive the necessary support and resources throughout their healthcare journey.
Digestive Health Clinics and Centers
Digestive health clinics and centers are specialized medical facilities that focus on the diagnosis and management of digestive disorders. These facilities often have multidisciplinary teams of gastroenterologists, nutritionists, nurses, and other healthcare professionals who work collaboratively to provide comprehensive care. They may offer specialized services such as diagnostic testing, endoscopy, nutritional counseling, and access to clinical trials.
Nutritionists and Dietitians
Nutritionists and dietitians are healthcare professionals who specialize in providing dietary guidance and support for individuals with digestive disorders. They can help develop personalized meal plans, address specific dietary concerns or restrictions, and provide education on proper nutrition for digestive health. Working with a nutritionist or dietitian can help individuals optimize their nutrition and manage symptoms.
Specialized Medical Centers
Specialized medical centers, such as inflammatory bowel disease centers or liver transplant centers, focus on specific digestive disorders or procedures. These centers often have specialized expertise, advanced treatment options, and access to clinical trials or research studies. If specialized care is needed, seeking treatment at a dedicated center can ensure individuals receive the most appropriate and advanced care for their condition.
Clinical Trials and Research Studies
Clinical trials and research studies offer individuals the opportunity to participate in cutting-edge research and access emerging treatments for digestive disorders. Participation in clinical trials can advance scientific knowledge and potentially provide access to innovative therapies. Individuals interested in participating in clinical trials should consult with their healthcare provider and explore available options through research institutions or clinical trial databases.
These resources and support networks can provide valuable information, guidance, and emotional support for individuals with digestive disorders. It is important to reach out to these resources and seek support when needed.
Preventing Digestive Disorders
Prevention is key in reducing the risk of developing digestive disorders. By adopting certain lifestyle habits and making healthy choices, individuals can significantly reduce their risk and promote optimal digestive health. The following are some strategies for preventing digestive disorders:
Regular Health Check-ups
Regular health check-ups are important for identifying potential risk factors or early signs of digestive disorders. Visit your healthcare provider regularly for routine screenings and evaluations. This allows for early detection of any abnormalities and prompt intervention if necessary.
Vaccinations and Immunizations
Certain infections, such as hepatitis A and B, can lead to liver damage and digestive complications. Keeping up to date with vaccinations and immunizations, as recommended by healthcare providers, can help prevent these infections and reduce the risk of associated digestive disorders.
Safe Food Handling and Preparation
Practicing safe food handling and preparation techniques is crucial for preventing foodborne illnesses, which can cause digestive disorders. Wash hands thoroughly before handling food, cook foods to the appropriate temperature, avoid cross-contamination, and refrigerate perishable items promptly. It is also important to be cautious when consuming raw or undercooked foods, especially seafood and meats.
Proper Handwashing Techniques
Proper handwashing is one of the most effective ways to prevent the spread of harmful bacteria and viruses that can cause digestive infections. Wash hands thoroughly with soap and water for at least 20 seconds, especially before handling food, after using the restroom, and after touching surfaces that may harbor germs. If soap and water are not available, use hand sanitizer that contains at least 60% alcohol.
Probiotic and Prebiotic Supplementation
Probiotics are beneficial bacteria that can support a healthy gut microbiome. Prebiotics are substances that feed these beneficial bacteria. Including probiotic-rich foods in your diet, such as yogurt, kefir, sauerkraut, and miso, or taking probiotic supplements can help maintain a healthy balance of gut bacteria. Prebiotics can be found in foods such as bananas, onions, garlic, and whole grains.
Balanced and Nutritious Diet
Maintaining a balanced and nutritious diet is essential for optimal digestive health. Consume a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats. Limit the intake of processed foods, sugary drinks, and high-fat foods. Following dietary guidelines, such as those recommended by national associations, can help ensure a well-rounded and balanced diet.
Avoiding Contaminated Water and Food
Consuming contaminated water or food can lead to digestive infections and illnesses. Avoid drinking untreated water from unfamiliar sources, especially when traveling. Ensure that food is prepared and stored in hygienic conditions, and be cautious when eating raw or undercooked foods. When traveling to areas with poor sanitation, drink bottled water and avoid street food or meals from untrusted establishments.
Maintaining Proper Oral Hygiene
Proper oral hygiene is important for overall health, including digestive health. Brush your teeth at least twice a day, floss daily, and schedule regular dental check-ups. Poor oral hygiene can lead to gum disease and oral infections, which can impact digestive health.
Managing Stress and Anxiety
Managing stress and anxiety is crucial for maintaining optimal digestive health. Chronic stress can lead to digestive issues such as stomachaches, indigestion, and diarrhea. Engaging in stress-relief techniques, such as deep breathing exercises, meditation, physical activity, and engaging in hobbies, can help reduce stress levels and promote overall well-being.
Educating and Raising Awareness
Educating yourself and others about digestive disorders and their prevention can help raise awareness and promote proactive steps to maintain digestive health. Share information with family, friends, and colleagues about the importance of healthy lifestyle habits, regular check-ups, and early intervention. Advocate for digestive health screening and access to appropriate care within your community.
Preventing digestive disorders requires a comprehensive approach that involves adopting healthy lifestyle habits, practicing proper hygiene, and seeking appropriate medical care. By taking proactive steps, individuals can significantly reduce their risk and promote optimal digestive health.