Migraines and headaches can be debilitating, causing immense pain and disrupting your daily life. Understanding the risk factors associated with these conditions can help you take necessary precautions to prevent them. In this article, we will explore the various risk factors that can contribute to migraines and headaches, as well as effective precautions you can take to minimize their occurrence. So, whether you are someone who frequently suffers from migraines or simply interested in learning more about these conditions, read on to discover valuable insights that can improve your overall well-being.

What are migraines and headaches?
Headaches and migraines are two common types of pain experienced by many people. While they may appear similar, there are distinct differences between the two.
Definition of migraines
Migraine is a specific type of headache that is often characterized by intense throbbing pain, typically on one side of the head. It can last for hours or even days, and is often accompanied by other symptoms such as sensitivity to light and sound, nausea, and vomiting. Migraines can be debilitating, affecting a person’s ability to carry out daily activities.
Definition of headaches
Headaches, on the other hand, are a more general term used to describe any pain or discomfort in the head or neck region. They can vary in intensity and duration, and can be caused by a variety of factors, such as tension, sinus congestion, or a head injury.
Difference between migraines and headaches
The main difference between migraines and headaches lies in their symptoms and severity. Migraines are typically more severe and come with additional symptoms, while headaches are often milder and do not have associated symptoms such as nausea or vomiting. Migraines also tend to last longer than regular headaches. It’s important to distinguish between the two as the treatment approaches may differ.
Types of migraines and headaches
There are several different types of migraines and headaches, each with its own set of symptoms and characteristics. Understanding these types can help in identifying and managing the condition.
Migraine without aura
This is the most common type of migraine, accounting for about 70-90% of all migraines. Migraine without aura is characterized by moderate to severe throbbing pain on one side of the head, accompanied by nausea, vomiting, and sensitivity to light and sound.
Migraine with aura
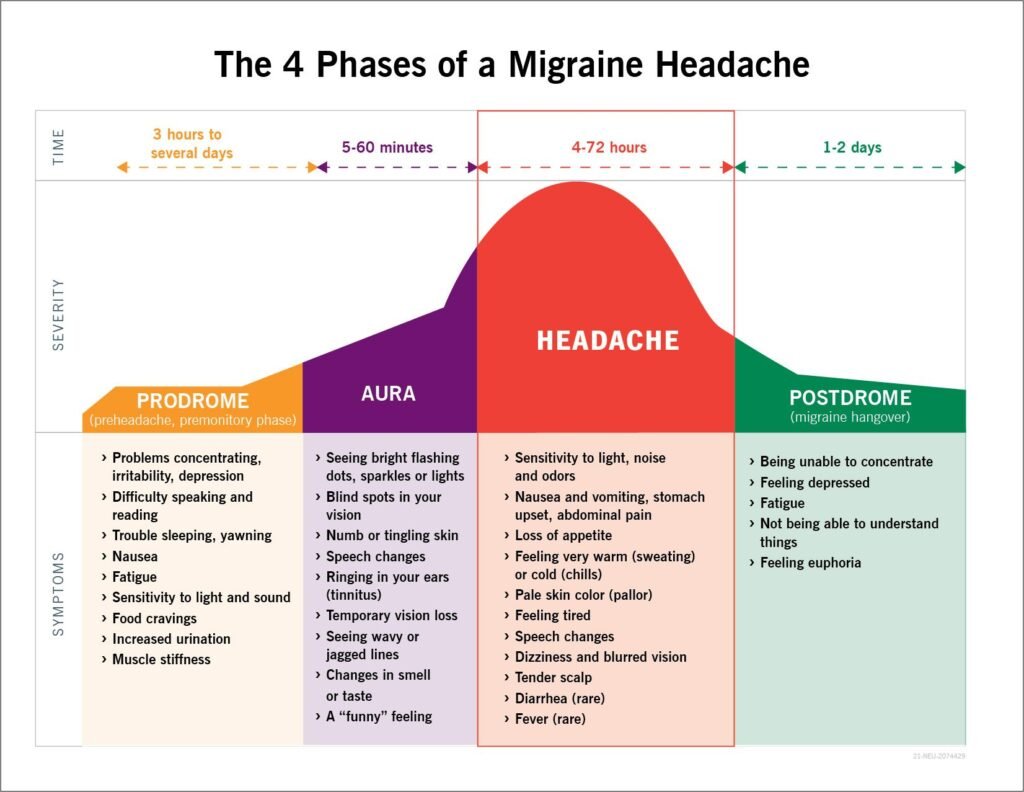
Migraine with aura is less common, affecting about 20% of migraine sufferers. Aura refers to a set of neurological symptoms that occur before or during a migraine attack. These symptoms can include visual disturbances such as seeing flashes of light or experiencing blind spots, as well as tingling or numbness in the face or hands.
Chronic migraines
Chronic migraines are defined as experiencing a headache on 15 or more days per month for at least three months, with at least 8 of those headaches being migraines. This condition can significantly impact a person’s quality of life and often requires intervention from a healthcare professional.
Tension headaches
Tension headaches are the most common type of headache and are typically described as a constant, dull pain or pressure around the head. They are often caused by stress, muscle tension, or poor posture. Unlike migraines, tension headaches do not typically cause nausea or vomiting.
Cluster headaches
Cluster headaches are less common but can be incredibly painful. They are characterized by severe, excruciating pain that usually occurs on one side of the head, often around the eye. Cluster headaches tend to occur in clusters or cycles, with several headaches happening over a period of weeks or months, followed by periods of remission.
Risk factors for migraines and headaches
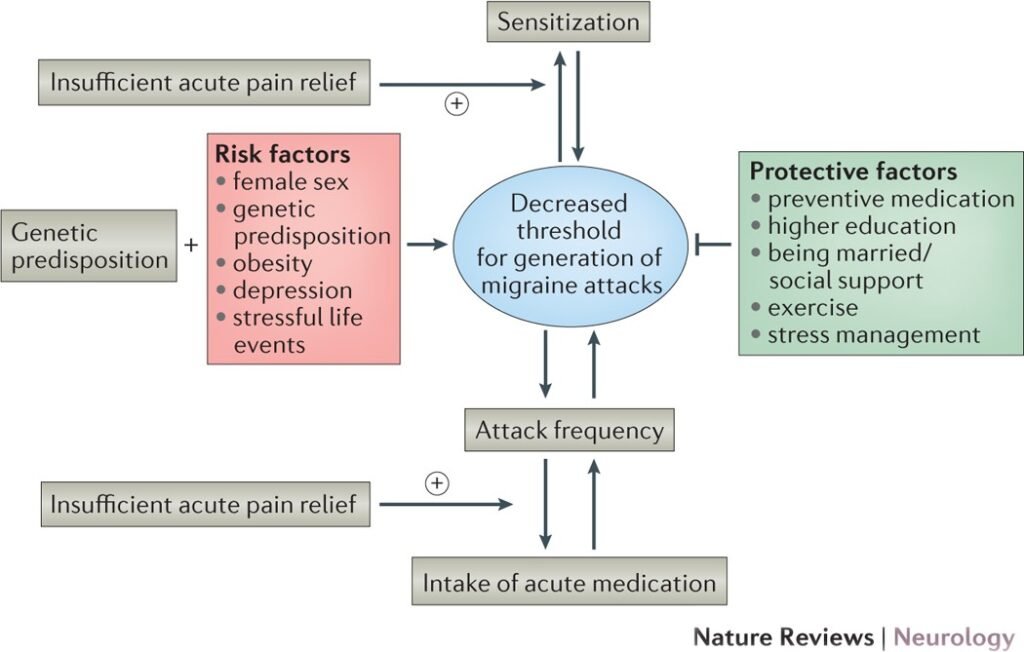
While the exact causes of migraines and headaches are not fully understood, several risk factors have been identified that may increase a person’s likelihood of experiencing these conditions.
Age and gender
Migraines and tension headaches are more common in women, while cluster headaches are more prevalent in men. Additionally, migraines often start in adolescence or early adulthood and tend to decrease in frequency and severity with age.
Family history
A family history of migraines or headaches can increase an individual’s risk of developing these conditions. Genetics may play a role in predisposing certain individuals to migraines and headaches.
Hormonal changes
Hormonal fluctuations, such as those that occur during the menstrual cycle or pregnancy, have been linked to migraines in some individuals. Women may find that their migraines are more likely to occur during certain times of their cycle.
Stress
Stress is a common trigger for both migraines and tension headaches. High levels of stress can lead to muscle tension and altered pain perception, increasing the likelihood of headaches.
Sleep patterns
Irregular sleep patterns, such as too much or too little sleep, can trigger migraines and headaches. Maintaining a regular sleep routine is important in preventing these conditions.
Diet and hydration
Certain foods and drinks, such as caffeine, alcohol, chocolate, and processed foods, can trigger migraines and headaches in susceptible individuals. Dehydration can also contribute to headaches, so it’s important to stay hydrated.
Environmental factors
Exposure to certain environmental stimuli, such as bright lights, strong smells, and loud noises, can trigger migraines and headaches in some people. Changes in weather or barometric pressure can also be a trigger.
Certain medications
Some medications, particularly those that dilate blood vessels, can trigger migraines in susceptible individuals. It’s important to be aware of potential side effects and discuss any concerns with a healthcare provider.
Head or neck injuries
Previous head or neck injuries, such as concussions or whiplash, can increase the risk of developing migraines or tension headaches. These conditions may also occur as a result of trauma.
Smoking and alcohol consumption
Both smoking and excessive alcohol consumption have been linked to an increased risk of migraines and headaches. Quitting smoking and moderating alcohol intake may help reduce their frequency.
Common triggers for migraines and headaches
In addition to the risk factors mentioned above, there are several common triggers that can precipitate migraines and headaches. Identifying and avoiding these triggers can help in managing these conditions.
Foods and additives
Certain foods and food additives have been known to trigger migraines and headaches. Some common culprits include aged cheeses, processed meats, chocolate, and artificial sweeteners. It’s helpful to keep a food diary to track potential triggers.
Caffeine
While caffeine can provide temporary relief for some individuals, excessive consumption or sudden withdrawal can trigger migraines and headaches. It’s important to monitor caffeine intake and avoid excessive use.
Alcohol
Alcohol is a common trigger for migraines and headaches, particularly red wine, beer, and certain spirits. It’s advisable to limit alcohol intake or avoid it altogether, depending on personal triggers.
Stress and anxiety
Stress and anxiety can cause muscle tension and alter pain perception, leading to migraines and headaches in susceptible individuals. Finding effective stress management techniques is crucial in reducing the frequency and severity of these conditions.
Changes in sleep patterns
Disruptions to sleep patterns, such as insufficient sleep or irregular sleep schedules, can trigger migraines and headaches. Establishing a regular sleep routine and practicing good sleep hygiene are essential for preventing these conditions.
Sensory stimuli
Strong smells, bright lights, and loud noises can provoke migraines and headaches in some individuals. Avoiding these sensory stimuli or wearing sunglasses and earplugs in bright and noisy environments can help reduce their impact.
Weather changes
Changes in weather or fluctuations in barometric pressure can trigger migraines and headaches. While we can’t control the weather, being aware of these triggers and taking preventive measures, such as wearing appropriate clothing or using air purifiers, may help.
Physical exertion
Intense physical exertion or strenuous exercise can trigger migraines and headaches in some individuals. It’s important to listen to your body, pace yourself during exercise, and avoid overexertion.
Hormonal changes
For many women, hormonal changes associated with the menstrual cycle, pregnancy, or menopause can trigger migraines. Understanding these hormonal shifts and discussing preventive strategies with a healthcare provider can be helpful.
Medication overuse
Overuse or dependency on pain medications, such as over-the-counter pain relievers, can actually lead to more frequent and severe migraines and headaches. It’s important to follow recommended dosage guidelines and consult with a healthcare provider if pain medication is required frequently.
Preventive measures for migraines and headaches
While migraines and headaches can be challenging to manage, there are several preventive measures that can be implemented to reduce their frequency and severity. It’s important to remember that not all strategies work for everyone, so it may take some trial and error to find the most effective approach.
Identifying and avoiding triggers
Keeping a headache diary can help identify triggers and patterns. Once triggers are identified, it’s important to avoid or minimize exposure to them as much as possible.
Establishing a regular sleep routine
Maintaining a consistent sleep schedule, aiming for the recommended 7-9 hours of sleep per night, can help prevent migraines and headaches caused by sleep disruptions.
Managing stress
Implementing stress management techniques, such as deep breathing exercises, meditation, or engaging in activities that help you relax, can reduce the likelihood of migraines and headaches triggered by stress.
Maintaining a balanced diet
Eating a well-balanced diet that includes whole foods, avoiding trigger foods, and staying hydrated can help prevent migraines and headaches.
Staying hydrated
Dehydration can contribute to headaches, so it’s important to drink plenty of water throughout the day. Aim for at least 8 glasses (64 ounces) of water daily.
Regular exercise
Engaging in regular physical activity can help reduce the frequency and severity of migraines and headaches. Aim for at least 30 minutes of moderate-intensity exercise on most days of the week.
Avoiding excessive caffeine and alcohol
Limiting caffeine intake, especially from sources like coffee or energy drinks, and avoiding excessive alcohol consumption can help in preventing migraines and headaches.
Using relaxation techniques
Practicing relaxation techniques, such as deep breathing exercises, progressive muscle relaxation, or yoga, can help reduce stress and prevent migraines and headaches.
Limiting exposure to sensory stimuli
Minimizing exposure to bright lights, loud noises, and strong smells can help prevent migraines and headaches triggered by sensory stimuli. Wearing sunglasses, using earplugs or noise-canceling headphones, and avoiding strong scents may be helpful.
Maintaining a headache diary
Keeping a detailed record of headache patterns, triggers, symptoms, and treatments in a headache diary can help identify patterns and learn what strategies are most effective in managing migraines and headaches.
Medical treatments for migraines and headaches
While preventive measures can be effective in managing migraines and headaches, some individuals may require medical treatment to alleviate symptoms and improve their quality of life. It’s important to consult with a healthcare professional for a proper diagnosis and to discuss appropriate treatment options.
Over-the-counter medications
Over-the-counter pain relievers, such as acetaminophen, ibuprofen, or aspirin, can be effective in reducing mild to moderate migraine and headache symptoms. It is important to follow the recommended dosage and consult with a healthcare provider if over-the-counter medications are not providing adequate relief.
Prescription medications
For more severe or frequent migraines, prescription medications may be necessary. These can include triptans, which help to constrict blood vessels and reduce inflammation in the brain, or preventive medications such as beta-blockers, antidepressants, or anti-seizure medications.
Botox injections
Botox injections have been approved by the FDA for the treatment of chronic migraines. This treatment involves injecting Botox into specific muscles of the head and neck to help prevent migraines.
Nerve block injections
Nerve block injections involve injecting anesthetic or corticosteroids to block pain signals and provide temporary relief for migraines and headaches.
Triptans
Triptans are a class of prescription medications specifically designed to treat migraines. They work by constricting blood vessels and reducing inflammation in the brain, providing relief from migraine symptoms.
Antidepressants
Certain antidepressants, such as tricyclic antidepressants or selective serotonin reuptake inhibitors (SSRIs), can be prescribed off-label to help prevent migraines and reduce their frequency.
Calcitonin gene-related peptide (CGRP) inhibitors
CGRP inhibitors are a newer class of drugs specifically designed to prevent migraines. They work by blocking a protein called calcitonin gene-related peptide, which is thought to play a role in the development of migraines.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Prescription-strength NSAIDs, such as naproxen sodium or diclofenac sodium, can be used to provide relief for migraines and headaches.
Ergotamine medications
Ergotamine medications constrict blood vessels and can be effective in relieving migraines. They are available in various forms, including tablets, nasal sprays, and suppositories.
Transcranial magnetic stimulation (TMS)
Transcranial magnetic stimulation is a non-invasive procedure that involves the use of magnetic fields to stimulate specific areas of the brain. It has been shown to be effective in reducing the frequency and severity of migraines in some individuals.
Lifestyle modifications for managing migraines and headaches
In addition to medical treatments, making certain lifestyle modifications can also help manage migraines and headaches effectively.
Maintaining a regular sleep schedule
Establishing a regular sleep routine and ensuring adequate sleep can help reduce the frequency and severity of migraines and headaches.
Establishing a healthy diet
Eating a well-balanced diet that includes whole foods, avoiding trigger foods, and maintaining regular meal times can contribute to managing migraines and headaches.
Regular exercise
Engaging in regular physical activity, such as walking, swimming, or cycling, can help reduce the frequency and severity of migraines and headaches.
Stress management techniques
Implementing stress management techniques, such as deep breathing exercises, yoga, or meditation, can help decrease stress levels and prevent migraines and headaches.
Avoiding triggers
Identifying personal triggers and avoiding them as much as possible can help prevent migraines and headaches. This may involve avoiding certain foods, managing exposure to sensory stimuli, or adopting relaxation techniques.
Practicing relaxation techniques
Engaging in relaxation techniques, such as deep breathing exercises or progressive muscle relaxation, can help reduce stress and prevent migraines and headaches.
Getting regular massages
Regular massages, particularly those that target tension in the neck and shoulders, can help relieve muscle tension and reduce the frequency and severity of migraines and headaches.
Creating a calm and quiet environment
Creating a calm and quiet environment, especially during migraines and headaches, can help relieve symptoms and promote relaxation.
Acupuncture
Acupuncture is a traditional Chinese medicine technique that involves the insertion of thin needles into specific points on the body. It has been shown to be effective in reducing the frequency and severity of migraines and headaches.
Biofeedback
Biofeedback is a technique that helps individuals become more aware of their body’s responses to certain stimuli. It can be beneficial in managing migraines and headaches by helping individuals recognize and control physiological changes associated with headaches.
When to seek medical help
While migraines and headaches are often manageable with preventive measures and lifestyle modifications, there are certain situations in which medical attention should be sought.
Frequent and severe headaches
If headaches are frequent and severe, it’s important to consult with a healthcare professional for a proper diagnosis and appropriate treatment.
Headaches accompanied by neurological symptoms
Headaches accompanied by neurological symptoms, such as difficulty speaking, numbness or weakness in the limbs, or changes in vision, should be evaluated by a healthcare professional to rule out other underlying conditions.
Headaches causing significant disruptions to daily life
If migraines or headaches are significantly impacting daily life, it’s important to seek medical attention for a comprehensive evaluation and individualized treatment plan.
New onset headaches after age 50
Headaches that occur for the first time after age 50 should be evaluated by a healthcare professional to rule out any underlying causes that may require treatment.
Worsening pattern or change in headache patterns
If there is a noticeable change in the frequency, severity, or pattern of migraines or headaches, medical attention is recommended to determine the cause and appropriate treatment.
Headaches after head injury or trauma
If migraines or headaches occur after a head injury or trauma, it is important to seek medical attention to assess for any potential complications or underlying conditions.
Conclusion
Migraines and headaches are common conditions that can significantly impact a person’s quality of life. Understanding the differences between migraines and headaches, as well as the various types, risk factors, triggers, and preventive measures, can help individuals effectively manage these conditions. While lifestyle modifications and preventive measures are often the first line of defense, seeking medical attention when necessary can provide additional support and treatment options. With proper management and care, individuals can minimize the impact of migraines and headaches on their daily lives.

