In this informative article, you will learn about the risk factors and precautions associated with primary congenital glaucoma. Discover the key factors that contribute to the development of this condition and gain insights into the precautions that can help prevent its onset. By understanding these important aspects, you can take proactive steps to protect yourself or your loved ones from this eye disease. So, let’s delve into the world of primary congenital glaucoma and discover how to safeguard your vision.
Risk Factors for Primary Congenital Glaucoma
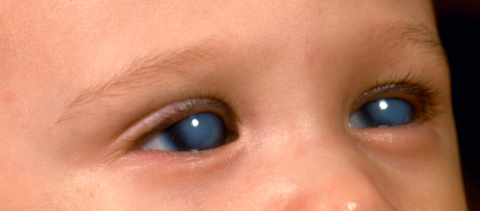
Primary congenital glaucoma (PCG) is a rare condition that affects infants and young children. It is important to understand the risk factors associated with PCG in order to identify those who may be at a higher risk and to take appropriate precautions.
Family History
Having a family history of glaucoma is one of the main risk factors for PCG. If there is a close relative, such as a parent or sibling, who has been diagnosed with glaucoma, there is an increased likelihood of a child developing PCG. It is important to inform your healthcare provider about any family history of glaucoma during the prenatal and postnatal periods.
Ethnicity
Certain ethnicities have a higher prevalence of PCG. For example, PCG is more common among individuals of Caucasian, Middle Eastern, and Asian descent. It is important to be aware of the increased risk associated with specific ethnic backgrounds and to speak with your healthcare provider about any concerns.
Gender
PCG affects both males and females, but there is a slight male preponderance. Boys are more likely to develop PCG compared to girls. It is important for parents to remain vigilant and attentive to any signs or symptoms of glaucoma, especially in boys.
Age at Onset
PCG typically manifests in the first few years of life, often within the first year. Infants with PCG may present with symptoms such as excessive tearing, sensitivity to light, and enlarged eyes. The earlier the onset of PCG, the more severe the disease tends to be. Prompt medical attention and early intervention are crucial for managing PCG effectively.
Genetic Risk Factors
Genetics play a significant role in the development of PCG. Several gene mutations have been associated with an increased risk of PCG.
CYP1B1 Gene Mutations
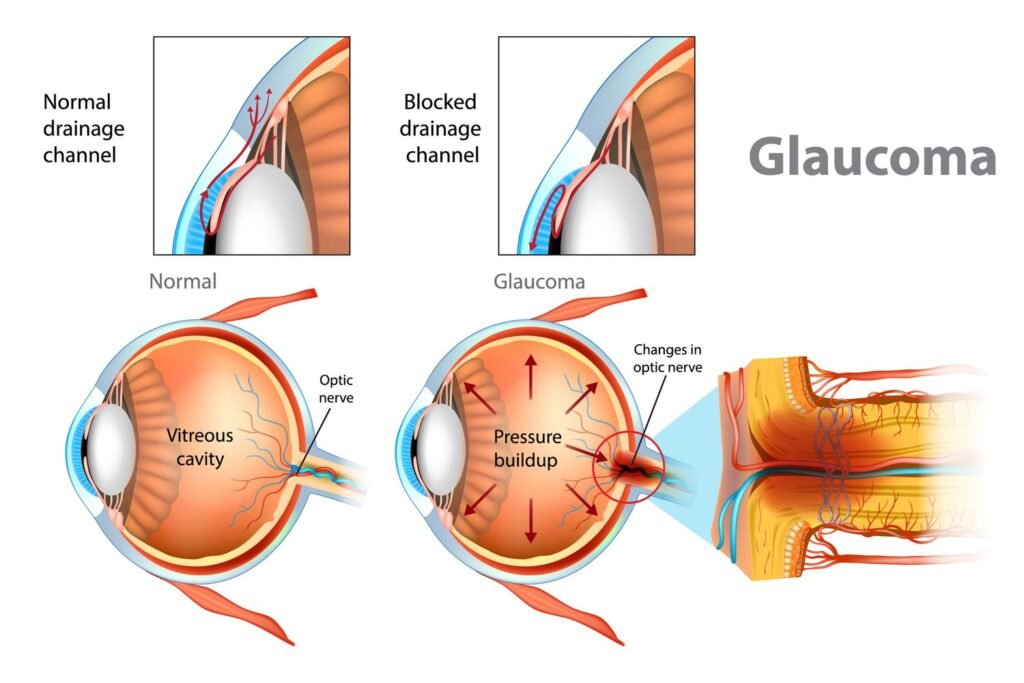
Mutations in the CYP1B1 gene have been identified as one of the major genetic risk factors for PCG. The CYP1B1 gene provides instructions for producing a protein that plays a role in the development and function of the eye’s drainage system. Mutations in this gene can disrupt the normal drainage of fluid from the eye, leading to increased intraocular pressure and the development of glaucoma.
GLC3A Gene Mutations
Mutations in the GLC3A gene have also been implicated in PCG. The GLC3A gene is thought to play a role in the development of the eye’s trabecular meshwork, which is responsible for regulating the flow of fluid in the eye. Mutations in this gene can interfere with the normal development and function of the trabecular meshwork, leading to an increased risk of PCG.
GLC3B Gene Mutations
In some cases, mutations in the GLC3B gene have been found to be associated with PCG. The exact role of these mutations in the development of PCG is not yet fully understood, and further research is needed to elucidate the mechanisms involved.
Non-Genetic Risk Factors
In addition to genetic factors, certain non-genetic factors have also been associated with an increased risk of PCG.
Prematurity
Premature infants have a higher risk of developing PCG compared to full-term infants. Prematurity is thought to disrupt the normal development of the eye’s drainage system, leading to increased intraocular pressure and glaucoma.
Low Birth Weight
Low birth weight is another non-genetic risk factor for PCG. Infants with a low birth weight are more likely to develop glaucoma compared to infants with a normal birth weight. It is important for healthcare providers to closely monitor infants with a low birth weight for signs of glaucoma.
Consanguinity
Consanguinity, or the marriage between close blood relatives, has been associated with an increased risk of PCG. The likelihood of inheriting genetic mutations that predispose individuals to PCG is higher in consanguineous marriages. It is important for individuals with a family history of PCG and consanguinity to undergo regular eye examinations to detect PCG early.
Precautionary Measures
While it may not be possible to completely prevent the development of PCG, there are several precautionary measures that can be taken to minimize the risk and manage the condition effectively.
Early Diagnosis and Screening
Early diagnosis and screening are vital for the timely detection and management of PCG. It is recommended to have regular eye examinations for all newborns, especially those with a family history of glaucoma or other known risk factors for PCG. Screening tests such as tonometry and gonioscopy can help identify elevated intraocular pressure and abnormalities in the eye’s drainage system.
Regular Eye Examinations
Regular eye examinations throughout childhood are essential for monitoring the progression of PCG and detecting any changes in vision or intraocular pressure. These examinations allow for early intervention and appropriate management strategies to be implemented.
Genetic Counseling
Families with a history of glaucoma or known genetic mutations associated with PCG should consider genetic counseling. Genetic counseling can help individuals understand their risk of developing PCG, determine the best course of action for themselves and their family members, and make informed decisions about family planning.
Treatment Modalities
Effective management of PCG typically involves a multi-modal treatment approach, which may include medication and surgical intervention.
Medication
Medication is often used as the first line of treatment for PCG. Medications such as eye drops or oral medications can help lower intraocular pressure by reducing the production of fluid in the eye or increasing its outflow. It is important to follow the prescribed medication regimen and attend regular follow-up visits to monitor the effectiveness of the medication.
Laser Surgery (Trabeculotomy)
Laser surgery, specifically trabeculotomy, is a commonly used surgical intervention for PCG. During trabeculotomy, a laser is used to create a small hole in the eye’s drainage system, allowing for improved fluid outflow and decreased intraocular pressure. This procedure is typically performed under anesthesia and is generally well-tolerated by infants and young children.
Glaucoma Drainage Implant Surgery
In cases where medication and laser surgery are not sufficient to control intraocular pressure, glaucoma drainage implant surgery may be recommended. A glaucoma drainage implant is a small device that is inserted into the eye to facilitate drainage of fluid and reduce intraocular pressure. This surgery requires careful consideration and monitoring due to its complexity and potential risks.
Complications and Risk Factors
PCG can lead to various complications and may increase the risk of certain eye conditions and vision loss if left untreated or poorly managed.
Increased Intraocular Pressure
One of the main complications of PCG is elevated intraocular pressure. Increased intraocular pressure can lead to optic nerve damage and loss of vision if not properly managed. Regular monitoring of intraocular pressure and timely intervention are crucial to prevent long-term damage.
Optic Nerve Damage
Prolonged elevation of intraocular pressure can cause damage to the optic nerve, which is responsible for transmitting visual information from the eye to the brain. Optic nerve damage can result in permanent vision loss if not addressed promptly and effectively.
Vision Loss
Untreated or poorly managed PCG can ultimately lead to vision loss. The severity of vision loss varies depending on factors such as the age of onset, duration of untreated glaucoma, and effectiveness of treatment. Early diagnosis, appropriate treatment, and regular follow-up care are essential for preserving vision and maintaining quality of life.
Types of Glaucoma
There are two main types of glaucoma: primary congenital glaucoma (PCG) and secondary congenital glaucoma.
Primary Congenital Glaucoma
Primary congenital glaucoma refers to cases where glaucoma is present at birth or develops within the first few years of life. PCG is typically caused by abnormalities in the eye’s drainage system, leading to increased intraocular pressure and subsequent optic nerve damage.
Secondary Congenital Glaucoma
Secondary congenital glaucoma refers to glaucoma that is caused by other underlying conditions, such as developmental abnormalities or other eye diseases. This type of glaucoma may present in infancy or early childhood and requires specific management based on the underlying cause.
Symptoms and Diagnosis
Recognizing the symptoms of PCG and obtaining an accurate diagnosis are crucial for initiating appropriate treatment and managing the condition effectively.
Symptoms in Infants
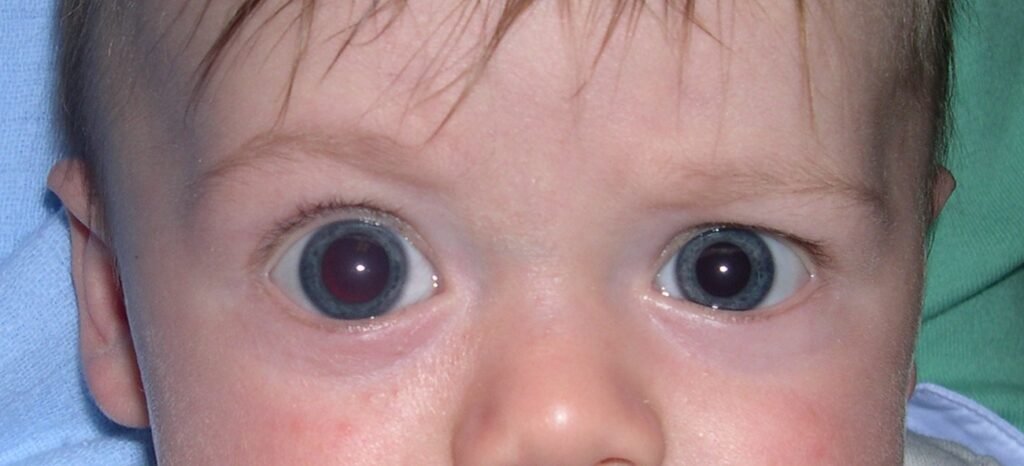
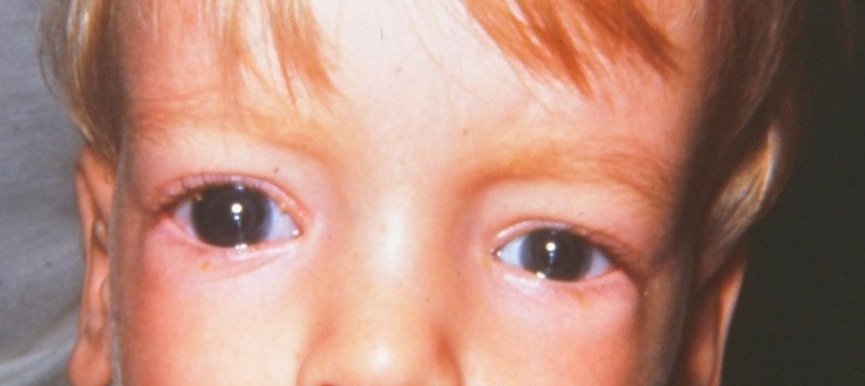
Infants with PCG may exhibit certain symptoms, including excessive tearing, sensitivity to light, and enlarged or cloudy eyes. These symptoms may be present at birth or develop within the first year of life. It is important for parents to be aware of these signs and seek medical attention if they suspect their child may have PCG.
Physical Examination
During a physical examination, an eye care professional may observe signs such as increased corneal diameter, corneal clouding, and enlarged eyes. These physical findings are often indicative of increased intraocular pressure and may prompt further diagnostic tests.
Tonometry
Tonometry is a diagnostic test used to measure the pressure inside the eye. Elevated intraocular pressure is a hallmark of glaucoma, including PCG. Tonometry can help confirm the diagnosis of PCG and monitor intraocular pressure levels throughout treatment.
Gonioscopy
Gonioscopy is a procedure that allows for the visualization and evaluation of the drainage angle of the eye. This test helps determine the extent of any abnormalities in the drainage system and can aid in the diagnosis and management of PCG.
Optic Disc Evaluation
Evaluation of the optic disc, the area where the optic nerve enters the eye, is essential in diagnosing and monitoring PCG. In PCG, the optic disc may show signs of damage or glaucomatous changes. Regular evaluation of the optic disc is important in determining the effectiveness of treatment and preventing further optic nerve damage.
Management of Primary Congenital Glaucoma
The management of PCG involves a combination of medical treatment and surgical intervention, depending on the severity of the condition.
Medical Management
Medical management of PCG typically involves the use of medications to lower intraocular pressure. Medications may be administered in the form of eye drops or oral medications. It is important to carefully follow the prescribed medication regimen and attend regular follow-up visits to ensure adequate control of intraocular pressure.
Surgical Intervention
Surgical intervention is often necessary for infants and children with PCG who do not respond adequately to medication or have severe disease. Procedures such as trabeculotomy or glaucoma drainage implant surgery may be recommended to improve the functioning of the eye’s drainage system and reduce intraocular pressure.
Follow-Up Care and Prognosis
Regular follow-up care is essential for monitoring the progression of PCG and adjusting treatment as needed. The long-term prognosis for PCG varies depending on factors such as the severity of the condition, age at onset, and effectiveness of treatment.
Ongoing Monitoring and Follow-Up Visits
Regular monitoring of intraocular pressure and routine eye examinations are important components of ongoing care for individuals with PCG. Follow-up visits allow healthcare providers to assess the effectiveness of treatment, address any concerns or complications, and make adjustments to the treatment plan if necessary.
Long-Term Outlook
With early diagnosis and appropriate intervention, the long-term outlook for individuals with PCG can be favorable. Timely treatment can help control intraocular pressure, prevent optic nerve damage, and preserve vision. However, it is important to note that individuals with PCG may require lifelong monitoring and management to maintain optimal eye health.
Visual Impairment and Quality of Life
PCG can have a significant impact on a child’s visual function and quality of life. Vision loss, even with treatment, may affect a child’s ability to perform daily activities and participate fully in educational and recreational activities. It is important for individuals with PCG and their families to receive appropriate support and resources to optimize visual functioning and overall well-being.
In conclusion, primary congenital glaucoma is a rare but potentially serious condition that can affect infants and young children. Understanding the risk factors associated with PCG, such as family history, ethnicity, and age at onset, is essential for early detection and intervention. Genetic and non-genetic risk factors contribute to the development of PCG, and precautionary measures such as early diagnosis, regular eye examinations, and genetic counseling can help minimize the risk and manage the condition effectively. Treatment modalities, including medication and surgical intervention, aim to control intraocular pressure and preserve vision. Complications such as elevated intraocular pressure, optic nerve damage, and vision loss can occur if PCG is left untreated or poorly managed. There are different types of glaucoma, with primary congenital glaucoma being the most common in children. Recognizing the symptoms of PCG and obtaining an accurate diagnosis through physical examination, tonometry, gonioscopy, and optic disc evaluation are crucial for initiating appropriate treatment. Management of PCG involves a combination of medical treatment and surgical intervention, and regular follow-up care is necessary to monitor the progress and ensure optimal outcomes. PCG can have a significant impact on a child’s visual function and quality of life, highlighting the importance of providing appropriate support and resources for individuals with the condition.