You’ve probably heard of the Japanese Encephalitis Virus, but do you know how it emerged and spread? This article explores the fascinating origins and transmission of the virus, shedding light on its impact on human health and the efforts being made to control its spread. From its initial discovery in Japan to its presence in various parts of Asia, this virus continues to pose a threat to millions of people. Join us as we delve into the world of Japanese Encephalitis Virus and uncover its secrets.
Overview of Japanese Encephalitis Virus
Japanese Encephalitis Virus (JEV) is a flavivirus that infects humans and animals, causing Japanese Encephalitis (JE), a potentially deadly neurological disease. It is primarily transmitted through the bite of infected mosquitoes, particularly those of the Culex genus. JEV is responsible for thousands of cases and deaths each year, mainly in Asia, affecting mostly children and young adults.
Definition of Japanese Encephalitis Virus
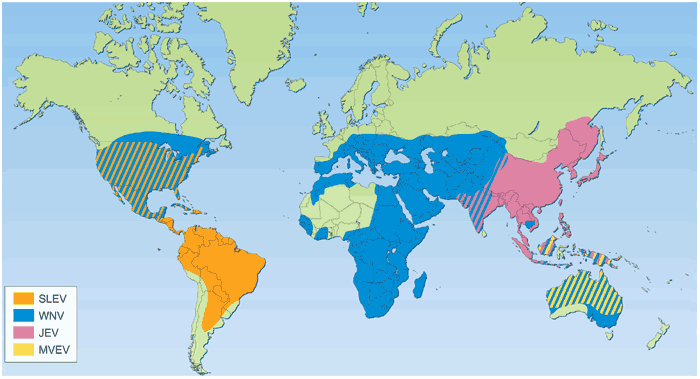
Japanese Encephalitis Virus, a member of the Flaviviridae family, is an RNA virus with a single-stranded, positive-sense genome. It belongs to the genus Flavivirus, which includes other medically important viruses such as dengue and West Nile virus. JEV is closely related to other encephalitis-causing viruses, like Murray Valley encephalitis virus and Saint Louis encephalitis virus.
Historical background of Japanese Encephalitis Virus
The first documented outbreak of Japanese Encephalitis occurred in Japan in the 1870s, hence the name of the virus. However, it was not until the 1930s that the virus was successfully isolated and identified. Since then, JEV has emerged as a significant public health threat in numerous Asian countries, affecting rural populations with agricultural practices that expose them to mosquito vectors. Over the years, various efforts have been made to combat the virus, including the development and implementation of vaccines.
Classification of Japanese Encephalitis Virus
Japanese Encephalitis Virus is classified within the Flaviviridae family, Flavivirus genus. It is a mosquito-borne virus closely related to other flaviviruses, including the dengue, Zika, and West Nile viruses. Within the Flavivirus genus, JEV belongs to the antigenic serocomplex of mosquito-borne encephalitis viruses. It exhibits substantial genetic diversity, with distinct genotypes circulating in different regions of Asia.
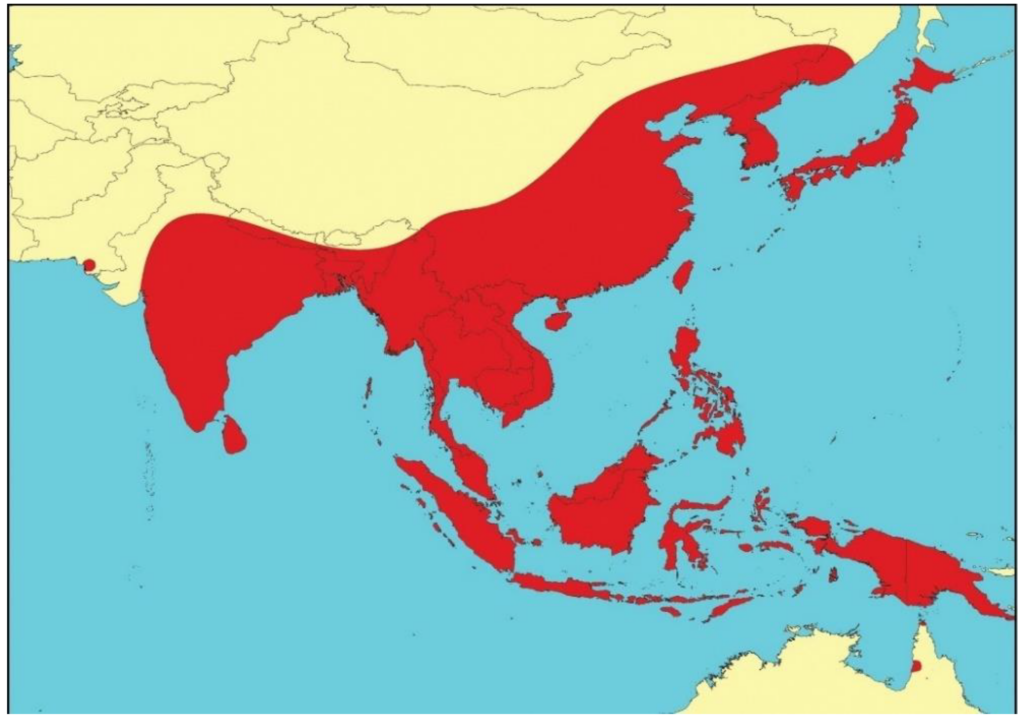
Global distribution of Japanese Encephalitis Virus
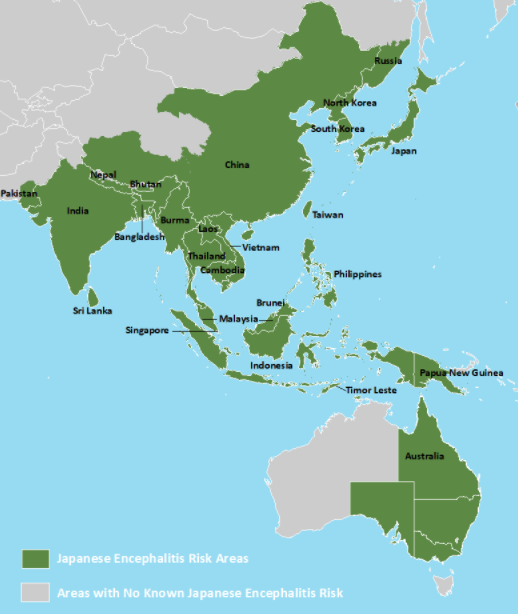
Japanese Encephalitis Virus is endemic in several countries across Asia, with the highest burden of disease reported in the East and Southeast Asian regions. It is estimated that JE affects over 50,000 cases annually, with up to 10,000 deaths. However, sporadic cases and outbreaks have also been documented outside Asia, highlighting the potential for international spread. Cases have been reported in countries such as Australia and Papua New Guinea, emphasizing the need for global awareness and preparedness.
Transmission and Hosts
Vector-borne transmission
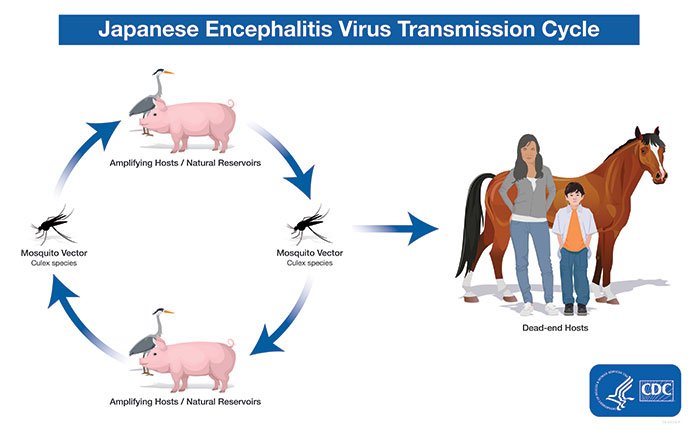
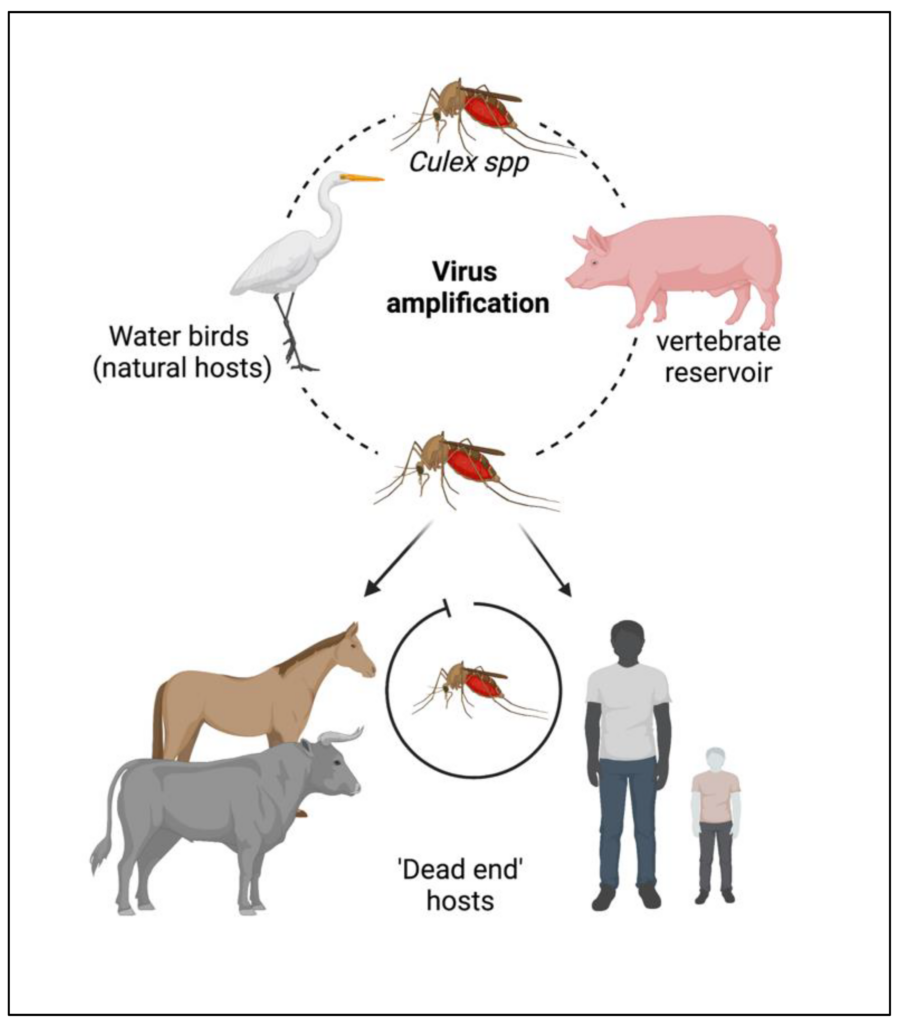
The primary mode of transmission for Japanese Encephalitis Virus is through the bite of infected mosquitoes, particularly the Culex species. Mosquitoes become infected when they feed on infected animals, including pigs and birds, which act as amplifying hosts. They can then transmit the virus to humans during subsequent blood meals. The virus does not spread directly from person to person.
Hosts of Japanese Encephalitis Virus
Japanese Encephalitis Virus has a complex transmission cycle involving several hosts. Mosquitoes, particularly Culex species, serve as the primary vectors. Birds act as amplifying hosts, maintaining the circulation of the virus in nature. Additionally, pigs are highly susceptible to JEV and play a crucial role in the transmission cycle. Humans are incidental hosts, but they can develop severe disease and contribute to the transmission cycle.
Amplifying hosts
Birds, especially species of herons and egrets, play a crucial role as amplifying hosts for Japanese Encephalitis Virus. Infected mosquitoes feed on birds, acquiring the virus, which then replicates within the mosquito’s salivary glands. When the infected mosquito feeds on another bird, it transmits the virus, allowing it to continue circulating within avian populations.
Role of humans in transmission
While humans are not an essential part of the Japanese Encephalitis Virus transmission cycle, their proximity to mosquito breeding grounds and outdoor activities expose them to mosquito bites. In areas where the virus is endemic, humans may become infected and potentially contribute to the amplification and spread of the virus. However, humans do not play a significant role in sustaining the virus’s circulation in nature.
Clinical Presentation and Symptoms
Incubation period
After being infected with Japanese Encephalitis Virus, an individual typically experiences an incubation period of 5-15 days before the onset of symptoms. During this time, the virus replicates in the body, primarily in the lymph nodes, and then spreads to the central nervous system.
Early symptoms
In the early stages of Japanese Encephalitis, individuals may experience non-specific flu-like symptoms, including fever, headache, malaise, and muscle pain. These symptoms can be easily mistaken for other viral infections, making early diagnosis challenging.
Severe symptoms
As the infection progresses, severe symptoms can develop, leading to encephalitis. These symptoms may include high fever, neck stiffness, seizures, confusion, and paralysis. In some cases, neurological complications can result in long-term disabilities or death.
Long-term complications
Survivors of Japanese Encephalitis may experience long-term complications, including neurological deficits such as paralysis, movement disorders, and cognitive impairments. These complications can significantly impact the quality of life and require long-term medical and rehabilitative care.
Diagnosis and Laboratory Testing
Clinical diagnosis
Clinical diagnosis of Japanese Encephalitis is challenging due to the non-specific nature of early symptoms. However, healthcare providers in endemic regions may suspect JEV infection based on the patient’s symptoms and travel history to high-risk areas during transmission seasons. Confirmation through laboratory testing is necessary for definitive diagnosis.
Serological tests
Serological tests are commonly used to diagnose Japanese Encephalitis Virus infection. These tests detect the presence of specific antibodies against JEV in the patient’s blood. Enzyme-linked immunosorbent assays (ELISAs) and hemagglutination inhibition assays are commonly used for serological testing.
Molecular detection methods
Molecular detection methods, such as polymerase chain reaction (PCR), are used to detect the presence of Japanese Encephalitis Virus genetic material in patient samples. PCR can provide a rapid and accurate diagnosis during the early stages of infection when viral RNA is still detectable.
Virus isolation
Virus isolation involves growing the Japanese Encephalitis Virus from patient samples in a laboratory setting. This process allows for further characterization and identification of the virus, aiding in surveillance efforts and understanding the genetic diversity of circulating strains.
Prevention and Control Measures
Vaccination strategies
Vaccination is a crucial strategy for the prevention and control of Japanese Encephalitis. A safe and effective vaccine is available, primarily targeted at individuals residing in or traveling to endemic areas. Vaccination campaigns focus on high-risk groups, such as children and agricultural workers, prioritizing areas with a high incidence of the disease.
Vector control
Controlling mosquito populations is an essential component of Japanese Encephalitis prevention. Measures include eliminating mosquito breeding sites, such as stagnant water sources, and implementing insecticide spraying programs in high-risk areas. Mosquito nets and personal protective measures, such as wearing long sleeves and using insect repellents, can also reduce exposure to mosquito bites.
Surveillance systems
Surveillance systems play a crucial role in monitoring the spread of Japanese Encephalitis and detecting outbreaks. These systems involve monitoring disease incidence, identifying high-risk areas, and tracking viral circulation in mosquito populations. Early detection and response can help mitigate the impact of outbreaks and guide targeted control measures.
Public health education
Public health education initiatives are essential in raising awareness about Japanese Encephalitis and promoting preventive measures. This includes educating communities about the importance of vaccination, mosquito bite prevention, and early recognition of symptoms. Health authorities work with local communities to ensure widespread knowledge and adoption of preventive measures.
Outbreaks and Epidemiology
Major outbreaks throughout history
Japanese Encephalitis has caused several major outbreaks throughout history, particularly in Asia. Notable outbreaks include those in Japan in the 1930s, Taiwan in the 1960s, and China in the 1970s. These outbreaks resulted in significant morbidity and mortality, highlighting the severity and impact of the disease.
Epidemiological patterns
Epidemiological patterns of Japanese Encephalitis vary across regions but generally follow a seasonal pattern tied to mosquito activity. The incidence of the disease is often highest during the rainy season, when mosquito populations are abundant. Agricultural practices, such as rice farming, can increase the risk of exposure to mosquito vectors and contribute to the disease’s endemicity.
Seasonal variations
Japanese Encephalitis exhibits seasonal variations in its incidence, with peak transmission occurring during specific times of the year in different regions. In temperate areas, transmission is typically highest in the summer and early fall. In tropical regions, where mosquito activity is more constant, the disease may occur year-round, with peaks during the rainy season.
Risk factors for outbreaks
Several factors contribute to the risk of Japanese Encephalitis outbreaks. These include the presence of susceptible populations, the density of mosquito vectors, and environmental conditions conducive to mosquito breeding. Areas with inadequate vaccination coverage, poor sanitation, and limited access to healthcare are at higher risk for outbreaks.
Impact on Public Health
Case fatality rate
Japanese Encephalitis has a significant impact on public health, with a case fatality rate ranging from 15% to 30% among individuals who develop severe neurological complications. This high mortality rate highlights the importance of early detection, prompt medical intervention, and prevention strategies to reduce the burden of the disease.
Disability-adjusted life years (DALYs)
The burden of Japanese Encephalitis extends beyond mortality, with many survivors experiencing long-term disabilities and impairments. Disability-adjusted life years (DALYs) is a measure that incorporates both premature death and years lived with disability. JEV infection contributes significantly to DALYs, emphasizing the long-term consequences of the disease on affected individuals and their communities.
Economic burden
Japanese Encephalitis places a significant economic burden on affected countries. The costs include medical expenses for treatment and rehabilitation, loss of productivity due to disability, and expenses related to prevention and control measures. These economic burdens can have long-lasting effects on individuals, families, and healthcare systems in endemic regions.
Psychological impact
The psychological impact of Japanese Encephalitis extends beyond the physical consequences. The disease’s potential to cause severe neurological complications and long-term disabilities can lead to mental health issues, including anxiety, depression, and social stigmatization. It is crucial to address the psychological impact of the disease and provide comprehensive support to affected individuals and their families.
Global Response and Research Efforts
Collaborative networks and organizations
International collaboration plays a vital role in addressing the challenges posed by Japanese Encephalitis. Organizations like the World Health Organization (WHO) work closely with member states, providing guidance on prevention strategies, facilitating surveillance networks, and coordinating research efforts. Collaborative networks allow for the sharing of knowledge, resources, and best practices in JE prevention, control, and research.
Research advancements
Research on Japanese Encephalitis Virus has significantly advanced our understanding of the virus, its transmission, and the development of effective prevention and control measures. Studies have focused on improving diagnostics, characterizing virus genotypes, investigating host-pathogen interactions, and evaluating the effectiveness of vaccines. These advancements contribute to the ongoing efforts to combat the disease.
Vaccine development
The development and deployment of vaccines have been critical in reducing the burden of Japanese Encephalitis. Several vaccines are available, including inactivated vaccines and live attenuated vaccines. These vaccines have been shown to be safe and effective in preventing Japanese Encephalitis Virus infection and reducing the severity of disease. Ongoing research aims to develop new-generation vaccines with enhanced immunogenicity and broader protection against different genotypes.
Surveillance and monitoring
Surveillance and monitoring of Japanese Encephalitis play a crucial role in understanding the epidemiology of the disease and detecting emerging threats. Surveillance systems allow for the early detection of outbreaks, identification of high-risk areas, and evaluation of the effectiveness of control measures. Continuous monitoring is essential in tracking the changing dynamics of the virus and informing public health interventions.
Emerging Threats and Future Prospects
Climate change and vector distribution
Climate change has the potential to affect the distribution and abundance of mosquito vectors, including those responsible for transmitting Japanese Encephalitis Virus. Changes in temperature, rainfall patterns, and other environmental factors can influence mosquito breeding habitats and extend the geographical range of the virus. Monitoring these changes and implementing adaptive strategies are essential for future preparedness.
Antiviral resistance
The emergence of antiviral resistance in Japanese Encephalitis Virus is a potential future threat. Although antiviral drugs are not currently a primary treatment for the disease, the development of resistance could hinder future treatment options and control efforts. Research into the mechanisms of antiviral resistance and the development of alternative treatment strategies are ongoing.
Emerging variants of the virus
The genetic diversity of Japanese Encephalitis Virus is a significant concern as new variants emerge. These variants may exhibit changes in antigenicity, vector competence, or virulence, potentially affecting the effectiveness of existing vaccines and control measures. Continuous surveillance and research on circulating strains are essential to ensure the ongoing relevance and efficacy of prevention strategies.
Cross-species transmission
Japanese Encephalitis Virus has the potential for cross-species transmission, as evidenced by infections in animals such as horses, cows, and goats. Cross-species transmission poses challenges in disease control and prevention, as it can lead to the maintenance and amplification of the virus in new reservoir hosts. Understanding the factors influencing cross-species transmission is crucial in developing targeted interventions.
Conclusion
Japanese Encephalitis Virus remains a significant public health concern, particularly in the endemic regions of Asia. The virus’s complex transmission cycle, potential for severe neurological complications, and global distribution highlight the need for continued research, prevention, and surveillance efforts. Collaborative networks, research advancements, and effective prevention strategies have made significant progress in mitigating the impact of Japanese Encephalitis. However, ongoing vigilance and investment in research and public health interventions are crucial to controlling the disease and protecting vulnerable populations globally.