The Japanese Encephalitis Virus (JEV) has emerged as a significant public health concern, affecting millions of people worldwide. This article explores the impact of JEV on public health, shedding light on its transmission, symptoms, and potential complications. By understanding the gravity of this virus, we can take necessary precautions to prevent its spread and protect ourselves and our communities.
Overview of Japanese Encephalitis Virus
Definition and background
Japanese Encephalitis Virus (JEV) is a flavivirus that belongs to the family Flaviviridae. It is the leading cause of viral encephalitis in Asia and the Western Pacific, particularly in rural areas. The virus is primarily transmitted through infected mosquitoes, primarily of the Culex species, and can infect humans and several animal species, including birds and pigs.
Transmission and reservoir
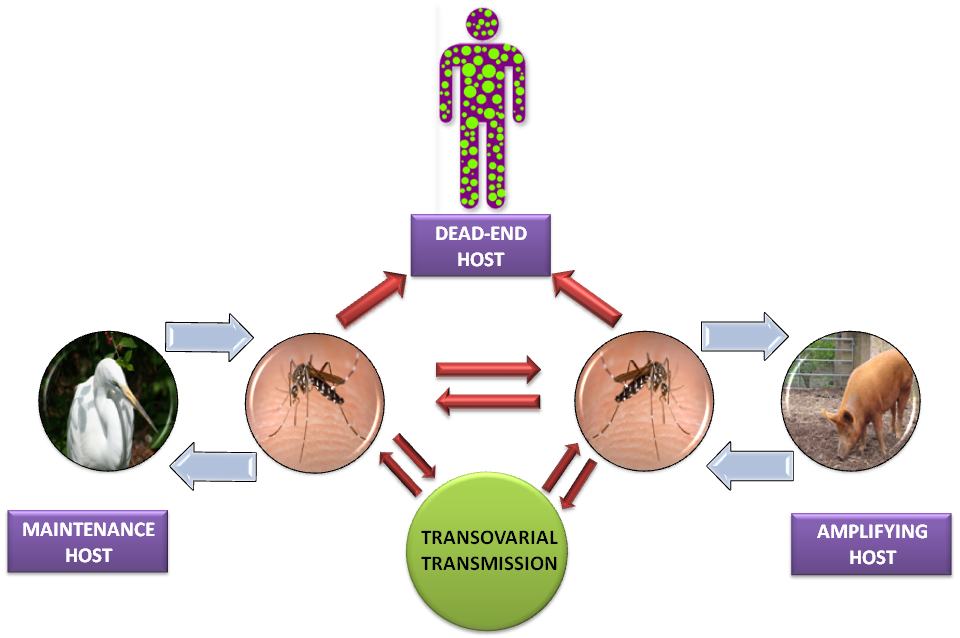
The main mode of transmission of JEV is through infected mosquitoes. Female mosquitoes become infected with the virus when they feed on infected animals, particularly pigs and birds. These infected mosquitoes can then transmit the virus to humans through their bites. Humans do not play a significant role in the transmission cycle, but can serve as incidental hosts.
Geographical distribution
JEV is endemic in many parts of Asia and the Western Pacific, particularly in rural agricultural areas. It is prevalent in countries such as China, India, Japan, and various Southeast Asian countries. The virus is more common in rural areas due to the presence of mosquito breeding sites, such as rice fields and pig farms. Outbreaks of Japanese encephalitis can occur in both endemic and non-endemic regions, particularly during the mosquito breeding season.
Clinical Presentation and Symptoms
Incubation period
The incubation period for Japanese encephalitis is typically between 5 to 15 days, but can range from 4 to 28 days. During this period, infected individuals do not show any symptoms and are unaware of the infection.
Mild and severe forms
The majority of individuals infected with JEV (around 70-80%) are asymptomatic or experience only mild symptoms similar to the flu. However, in a small number of cases, typically less than 1%, the infection can progress to severe encephalitis. Severe cases often present with high-grade fever, headache, neck stiffness, seizures, confusion, and paralysis.
Neurological manifestations
One of the hallmarks of Japanese encephalitis is its ability to affect the central nervous system. In severe cases, JEV can cause inflammation of the brain, leading to brain damage and neurological deficits. Common neurological manifestations include meningitis, encephalitis, and acute flaccid paralysis. Some patients may also experience seizures and a decline in cognitive and motor functions.
Diagnosis and Laboratory Techniques
Serological tests
Serological tests are commonly used to diagnose Japanese encephalitis. These tests detect the presence of antibodies against JEV in the patient’s blood. The most commonly used serological tests include enzyme-linked immunosorbent assays (ELISA) and neutralization tests. Serological tests are particularly useful during the acute phase of the illness when the virus can still be detected in the blood.
Molecular tests
Molecular tests, such as polymerase chain reaction (PCR), can be used to detect viral genetic material in patient samples. PCR is highly sensitive and can detect JEV even in low viral loads. Molecular tests are especially useful in confirming JEV infection in the early stages before the body has produced detectable levels of antibodies.
Cerebrospinal fluid analysis
Cerebrospinal fluid (CSF) analysis is an important diagnostic tool for Japanese encephalitis. In severe cases, the virus can invade the central nervous system, leading to changes in the composition of the CSF. Analysis of the CSF can help identify the presence of JEV, as well as other markers of inflammation and infection.
Prevention and Control Measures
Vaccination strategies
Vaccination is the most effective way to prevent Japanese encephalitis. There are several vaccines available, including inactivated vaccines and live attenuated vaccines. Vaccination is recommended for individuals living in or traveling to areas where JEV is endemic. Mass vaccination campaigns targeting high-risk populations, such as children and agricultural workers, have been successful in reducing the burden of the disease in some countries.
Vector control
Vector control plays a crucial role in preventing the transmission of JEV. This includes measures such as mosquito surveillance, larval source reduction, insecticide application, and the use of bed nets and insect repellents. Integrated vector management strategies that combine multiple control methods have been shown to be effective in reducing mosquito populations and preventing the spread of JEV.
Public health campaigns
Public health campaigns are essential in raising awareness about Japanese encephalitis and promoting preventive practices. These campaigns involve educating communities about the risk factors, symptoms, and modes of transmission of the virus. They also emphasize the importance of vaccination, vector control, and personal protective measures, such as wearing long sleeves and using insect repellents.
Risk Factors and Vulnerable Populations
Age and gender
Japanese encephalitis can affect individuals of all ages, but children and the elderly are particularly vulnerable. Children are at a higher risk due to their immature immune systems, while older adults may have reduced immune responses. Male individuals, particularly those engaged in outdoor activities or agricultural work, are also at increased risk due to higher exposure to mosquitoes.
Occupation and lifestyle
Occupation and lifestyle can significantly influence the risk of Japanese encephalitis. Agricultural workers, particularly those working in rice fields or pig farms, have a higher risk of exposure to infected mosquitoes. Individuals living in rural areas with inadequate housing and sanitation facilities may also be at increased risk due to the presence of mosquito breeding sites nearby.
Socioeconomic factors
Socioeconomic factors can contribute to the risk of Japanese encephalitis. Poverty and limited access to healthcare services may prevent individuals from receiving timely vaccinations or seeking appropriate medical care. Lack of awareness and education about preventive measures can also increase the risk of infection in vulnerable populations.
Epidemiology and Global Burden
Case incidence and prevalence
Japanese encephalitis is responsible for an estimated 68,000 cases of encephalitis each year. However, the true burden of the disease is likely underestimated due to underreporting and misdiagnosis. The incidence of Japanese encephalitis varies across different regions, with the highest burden seen in countries like India, China, and Myanmar.
Outbreaks and seasonal patterns
Outbreaks of Japanese encephalitis tend to occur during the rainy season when mosquito populations are at their peak. The virus has a cyclical pattern, with several years of low activity followed by periodic outbreaks. The timing and severity of outbreaks can also be influenced by factors such as climate, agricultural practices, and mosquito control measures.
Long-term consequences
Even for those who survive severe Japanese encephalitis, the disease can have long-term consequences. Some individuals may experience neurological sequelae, including cognitive deficits, motor paralysis, and behavioral changes. These long-term consequences can have a significant impact on the quality of life and functional abilities of affected individuals.
Treatment and Management
Antiviral therapy
There is no specific antiviral treatment for Japanese encephalitis. Supportive care is the mainstay of treatment, which includes measures to alleviate symptoms and manage complications. In severe cases, hospitalization may be necessary to provide close monitoring and intensive care, including respiratory support and seizure management.
Supportive care
Supportive care focuses on managing the symptoms and complications of Japanese encephalitis. This may include the administration of antipyretics to reduce fever, intravenous fluids to prevent dehydration, and medications to control seizures and pain. Physical therapy and rehabilitation may also be needed to help affected individuals regain their motor and cognitive functions.
Post-infection sequelae
Some individuals who have recovered from Japanese encephalitis may experience long-term sequelae. Rehabilitation programs can help manage these sequelae and improve the overall functional outcomes of affected individuals. These programs may include physical therapy, occupational therapy, speech therapy, and counseling to address any psychological or emotional challenges.
Impact on National Healthcare Systems
Financial burden
Japanese encephalitis can impose a significant financial burden on national healthcare systems and affected individuals. The cost of hospitalization, treatment, and long-term care can be substantial, particularly in severe cases that require intensive care. Additionally, the economic impact of the disease can be significant due to decreased productivity and healthcare expenditures.
Health infrastructure challenges
The management of Japanese encephalitis presents various challenges to healthcare systems, particularly in resource-limited settings. Adequate laboratory facilities for diagnosis, availability of vaccines, and trained healthcare professionals for the prevention and management of the disease can be limited in some areas. Strengthening health infrastructure and surveillance systems is crucial for effective control and management of Japanese encephalitis.
Emergency response
Japanese encephalitis outbreaks can require rapid and coordinated emergency response efforts. This includes the deployment of healthcare personnel to affected areas, establishment of temporary treatment facilities, and implementation of vector control measures. Emergency response plans should also focus on communication and coordination between different sectors, such as health, agriculture, and education, to effectively address the outbreak.
Life Cycle and Transmission Cycle
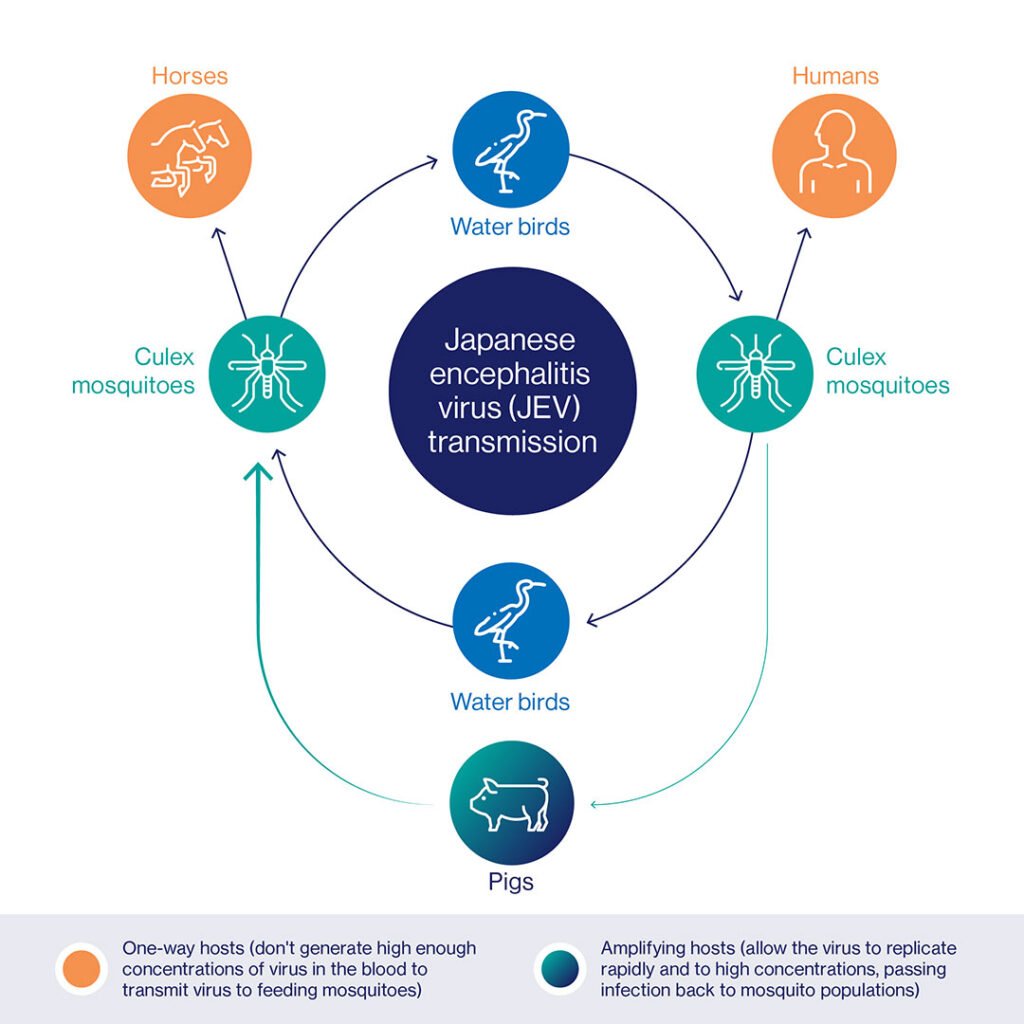
Hosts and vectors
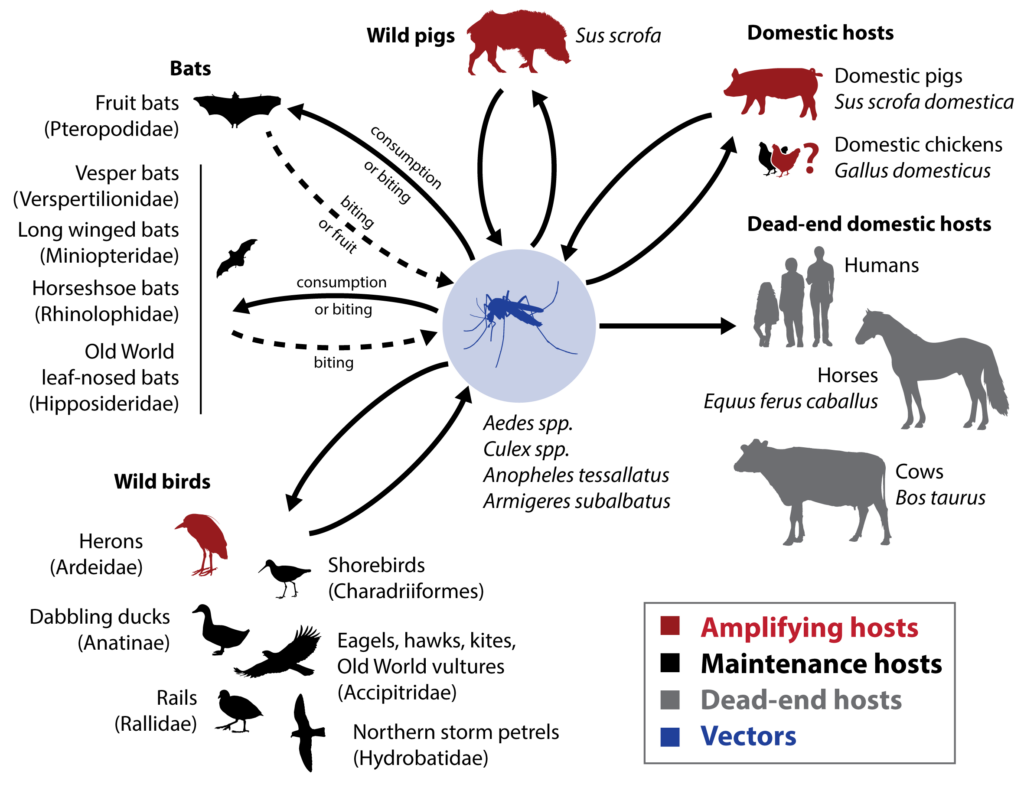
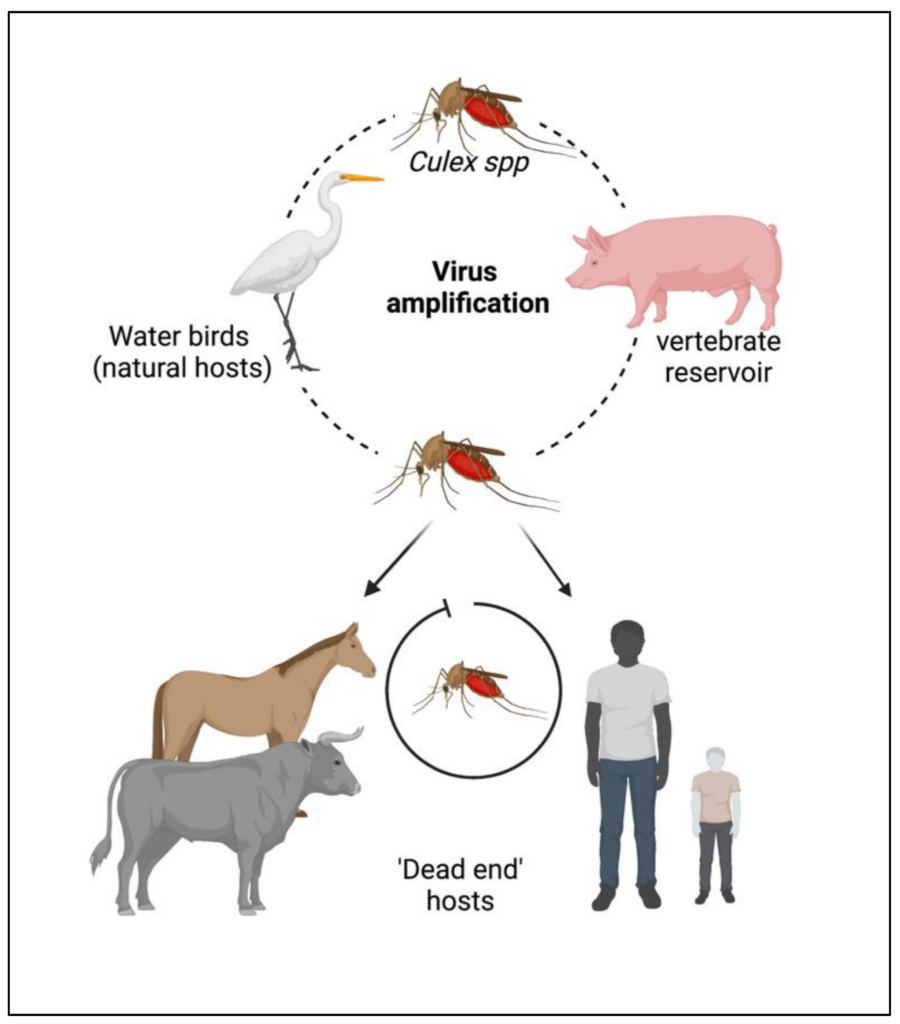
Japanese encephalitis has a complex life cycle involving several hosts and vectors. Birds, particularly wading birds, serve as the primary reservoir for the virus. Mosquitoes, primarily of the Culex species, act as the vectors, transmitting the virus between infected birds and other susceptible hosts, including humans and pigs. Pigs play an important role in amplifying the virus, as they can develop high viral loads and act as reservoirs for transmission to mosquitoes.
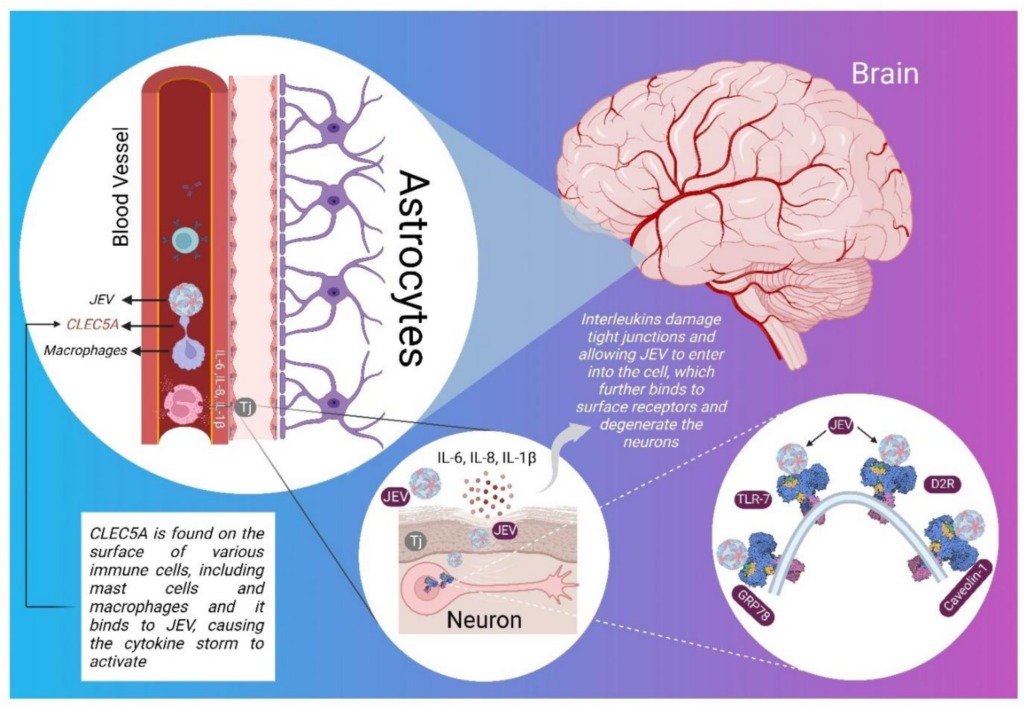
Viral replication process
Once JEV is transmitted to a human host through a mosquito bite, it replicates in various tissues, including the skin, lymph nodes, and central nervous system. The virus targets neurons in the brain, leading to inflammation and damage. The replication process can trigger a cascade of immune responses, resulting in the release of pro-inflammatory molecules and cytokines that contribute to the neurological manifestations of the disease.
Transmission pathways
The main transmission pathway for Japanese encephalitis is through the bite of infected mosquitoes. Mosquitoes become infected when they feed on infected animals, mainly birds or pigs, which serve as reservoirs of the virus. The infected mosquitoes can then transmit the virus to humans during subsequent blood meals. It is important to note that direct human-to-human transmission of JEV is rare and not considered a significant mode of spread.
Research and Future Directions
Vaccine development
Ongoing research is focused on the development of new and improved vaccines for Japanese encephalitis. This includes the exploration of novel vaccine platforms, such as virus-like particles and DNA vaccines. The development of more affordable and heat-stable vaccines is also crucial to enhance vaccine accessibility and coverage, particularly in low-resource settings.
Vector control strategies
Research efforts are directed towards the development of innovative vector control strategies to reduce the transmission of JEV. This includes the use of genetically modified mosquitoes or bacteria to reduce mosquito populations or render them unable to transmit the virus. Integrated vector management approaches that combine multiple control methods, such as mosquito nets and insecticide application, are also being investigated.
Improved diagnostics
Advancements in diagnostic techniques are essential for early and accurate detection of JEV infection. Research is focused on the development of rapid diagnostic tests that can provide results in a timely manner, allowing for prompt treatment or preventive measures. Additionally, efforts are being made to improve the sensitivity and specificity of serological and molecular tests to enhance diagnostic accuracy.
In conclusion, Japanese encephalitis represents a significant public health concern in many parts of Asia and the Western Pacific. It is a mosquito-borne viral infection that can cause severe neurological complications and long-term sequelae. Prevention and control efforts, including vaccination, vector control, and public health campaigns, are crucial in reducing the burden of the disease. Continued research and development of vaccines, vector control strategies, and improved diagnostics are essential to further enhance prevention and management efforts.