In today’s fast-paced world, the emergence of new variants of the virus has become a pressing concern, demanding our attention and understanding. With each passing day, these variants introduce new challenges that require innovative solutions. From the B.1.1.7 lineage to the P.1 variant, these permutations of the virus pose a threat to our efforts in controlling the pandemic. In this article, we will explore the causes behind the emergence of these new variants, their potential impact on public health, and the measures we can take to mitigate their spread. So grab a cup of tea and join us as we navigate through the evolving landscape of viral mutations.

Factors contributing to the emergence of new variants
Genetic mutation
Genetic mutation is a natural occurrence in viruses, including the one responsible for the ongoing pandemic. As the virus replicates, errors can occur in its genetic material, resulting in mutations. Some mutations may confer advantages to the virus, such as increased transmissibility or resistance to certain treatments. These advantageous mutations can lead to the emergence of new variants.
Selective pressure
Selective pressure refers to the influence of external factors on the survival and propagation of different virus variants. In the case of the current pandemic, selective pressure can arise from factors such as the human immune response, treatment interventions, or even changes in human behavior. Variants that can evade these pressures have a higher chance of persisting and spreading.
Transmission dynamics
The transmission dynamics of the virus play a crucial role in the emergence of new variants. The more opportunities a virus has to replicate and spread, the greater the chance of new mutations occurring. Factors such as large gatherings, reduced adherence to preventive measures like mask-wearing and social distancing, and the presence of superspreader events can contribute to increased transmission and the emergence of new variants.
Immunological evasion
Immunological evasion refers to the ability of a virus variant to avoid or escape the human immune response. This can occur through mutations that change the virus’s surface proteins, such as the spike protein, which is the target of many vaccines and antibody therapies. Variants that can evade the immune system may be better able to infect individuals who have previously been infected or vaccinated, leading to the emergence of new variants.
Identification and naming of new variants
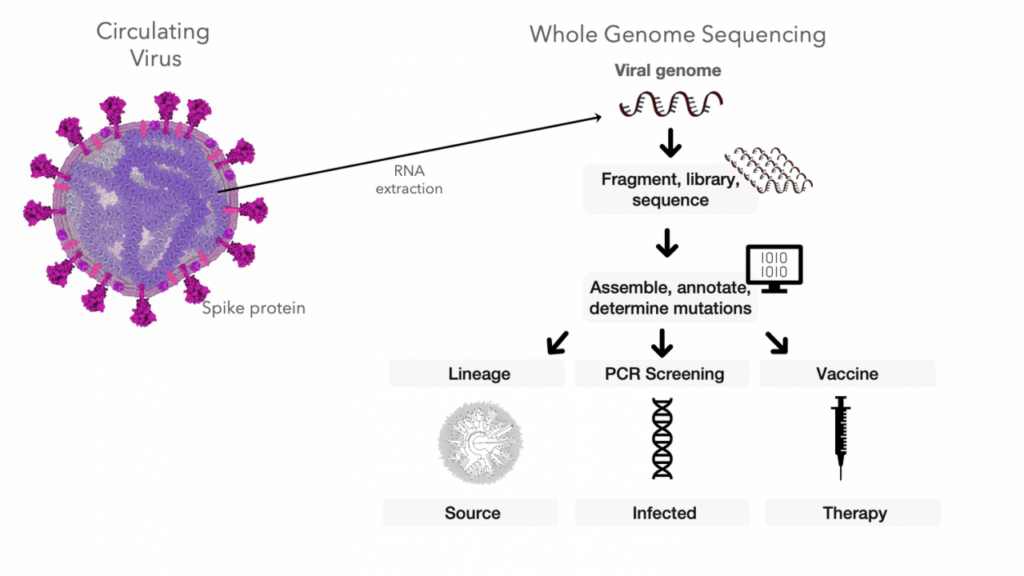
Genomic surveillance
Genomic surveillance involves systematically sequencing the genetic material of the virus to identify any changes or mutations. This surveillance helps researchers and public health officials monitor the emergence and spread of new variants. By analyzing the genetic sequences, scientists can determine if a new variant has emerged and track its prevalence over time.
Lineage classification
Lineage classification is the process of categorizing virus variants into distinct lineages based on their genetic characteristics. This classification helps researchers understand the evolutionary relationships between different variants and their potential implications for transmission, virulence, and response to interventions.
Naming conventions
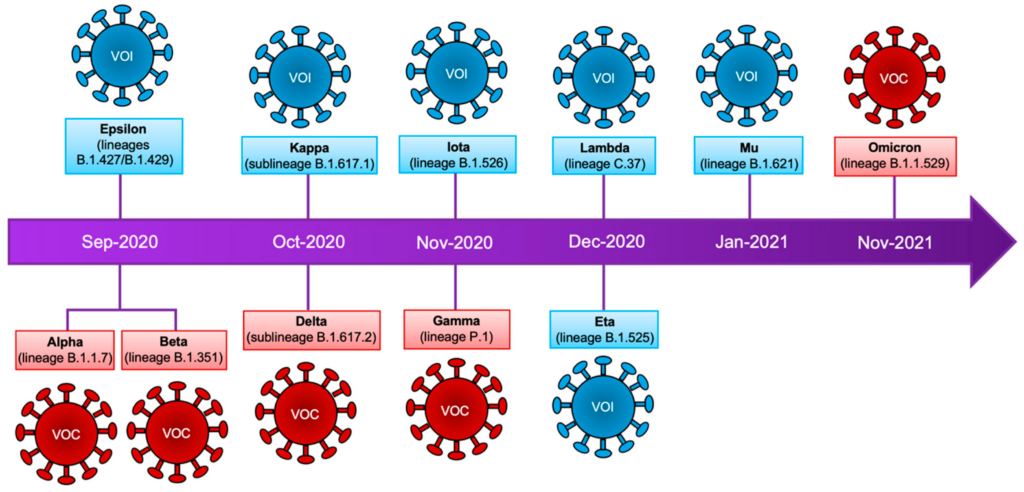
The World Health Organization (WHO) has established a naming system for SARS-CoV-2 variants to avoid stigmatization or potential harm associated with using geographic or individual names. Variants are assigned names based on letters of the Greek alphabet, such as Alpha, Beta, Gamma, and Delta. This standardized naming convention ensures clarity and avoids confusion when referring to different variants.
Impact of new variants on transmission
Increased transmissibility
One of the key concerns with new variants is their potential for increased transmissibility. Some variants, such as the Alpha variant (B.1.1.7), the Beta variant (B.1.351), the Gamma variant (P.1), and the Delta variant (B.1.617.2), have shown higher transmissibility compared to previous strains. This increased transmissibility can lead to more rapid spread and a higher number of cases in a shorter period, putting additional strains on healthcare systems.
Higher replication rates
Certain variants may exhibit higher replication rates, allowing them to replicate and multiply more efficiently within the human body. This increased replication can result in higher viral loads, potentially leading to more severe disease or prolonged shedding of the virus, both of which can contribute to increased transmission.
Effectiveness against vaccines
Another crucial factor in the impact of new variants is their effectiveness against vaccines. Some variants have shown reduced susceptibility to the immunity elicited by prior infection or vaccination. This reduced effectiveness can lead to breakthrough infections in individuals who have been previously infected or vaccinated, potentially compromising the population-wide protection provided by vaccines.
Potential for reinfection
New variants may also have the potential to cause reinfection in individuals who have recovered from a previous infection. Changes in the viral proteins can evade the immune response generated during the initial infection, allowing the virus to infect again. This potential for reinfection adds to the challenges of controlling the spread of the virus and protecting vulnerable populations.
Key new variants of concern
Alpha variant (B.1.1.7)
The Alpha variant, initially identified in the United Kingdom, quickly became a variant of concern due to its increased transmissibility. It has been associated with a higher risk of hospitalization and mortality compared to earlier variants. The Alpha variant contains multiple mutations in the spike protein, including the N501Y mutation, which enhances its binding affinity to human cells.
Beta variant (B.1.351)
Originating in South Africa, the Beta variant has raised concerns due to its reduced susceptibility to neutralizing antibodies and potential impacts on vaccine effectiveness. It carries mutations in the spike protein, including E484K, which can help it evade the immune response. The Beta variant has been associated with higher viral loads and increased severity of disease in some individuals.
Gamma variant (P.1)
First identified in Brazil, the Gamma variant shares similarities with the Beta variant, including the E484K mutation. It has shown increased transmissibility and the potential for reinfection. The Gamma variant has also been associated with a higher risk of severe disease and has spread to several countries worldwide.
Delta variant (B.1.617.2)
The Delta variant, initially identified in India, has rapidly become a dominant strain in many countries. This variant is highly transmissible, potentially more severe, and has shown reduced neutralization by some antibodies. The Delta variant carries multiple mutations in the spike protein, including L452R and P681R, which may contribute to its increased transmissibility and potential immune evasion.
Geographical distribution and spread of new variants
Origin and initial spread
Each new variant has its own origin and initial spread. The Alpha variant, for example, was first detected in the United Kingdom and subsequently spread to many countries around the world. Similarly, the Beta variant originated in South Africa, the Gamma variant in Brazil, and the Delta variant in India. The initial spread of these variants was facilitated by factors such as international travel and globalization.
Global distribution
Over time, new variants have spread globally, often reaching different continents and countries. The interconnectedness of the modern world through travel and trade has allowed for the rapid dissemination of these variants. Some variants, like the Delta variant, have shown exceptional transmissibility, leading to explosive outbreaks in multiple regions and contributing to their global distribution.
Factors influencing local prevalence
The prevalence of new variants can vary across different regions and even within specific localities. Factors such as population density, adherence to preventive measures, vaccination coverage, and public health responses can all influence the local prevalence of new variants. Additionally, certain regions may be more susceptible to the introduction and spread of variants due to lower healthcare capacity or limited access to vaccines and other interventions.
Efficacy of vaccines against new variants
Vaccine effectiveness studies
Numerous studies have been conducted to assess the effectiveness of vaccines against new variants. These studies evaluate the ability of vaccines to prevent infection, reduce the severity of disease, and minimize transmission. Vaccine effectiveness studies involve monitoring vaccinated individuals and comparing their outcomes with unvaccinated individuals, taking into account the presence of different variants in the population.
Effectiveness of existing vaccines
While the emergence of new variants has raised concerns regarding the effectiveness of existing vaccines, studies have shown that many vaccines still provide substantial protection against severe disease, hospitalization, and death. Although some breakthrough infections may occur with new variants, vaccinated individuals are still significantly less likely to experience severe outcomes compared to those who are unvaccinated.
Development of variant-specific vaccines
As new variants continue to emerge, researchers are actively working on the development of variant-specific vaccines. These vaccines specifically target the unique genetic characteristics of the variants to elicit a more targeted and effective immune response. The development and deployment of variant-specific vaccines can further enhance protection against emerging variants and contribute to the control of the pandemic.

Public health measures to control new variant spread
Testing and surveillance strategies
Robust testing strategies, including widespread diagnostic testing and genomic surveillance, are essential for the detection and monitoring of new variants. Testing helps identify and isolate infected individuals, while genomic surveillance provides crucial information on variant prevalence, transmission patterns, and potential impacts on public health measures.
Contact tracing and quarantining
Contact tracing plays a vital role in identifying and containing the spread of new variants by identifying individuals who may have been exposed to the virus. Quarantining individuals who have come into contact with confirmed cases helps prevent further transmission and interrupt chains of transmission. Prompt and efficient contact tracing and quarantining are crucial in controlling the spread of new variants.
Travel restrictions and border control
Travel restrictions and border control measures have been implemented by many countries to limit the importation of new variants. These measures include testing requirements, quarantine protocols, and travel bans from regions with high variant prevalence. By limiting the introduction of new variants from outside sources, countries can reduce the risk of rapid transmission and mitigate the impact of new variants on their population.
Vaccine deployment and booster shots
Widespread vaccine deployment, including prioritizing high-risk groups and ensuring equitable access, is essential for reducing the transmission and impact of new variants. Additionally, the administration of booster shots to maintain and enhance vaccine-induced immunity against new variants is an ongoing consideration. Boosters can help strengthen the immune response to variants and provide longer-term protection as new variants continue to emerge.
Potential long-term consequences of new variants
Evolutionary trajectory of the virus
The emergence of new variants highlights the ongoing evolutionary trajectory of the virus. Mutations and subsequent selection pressures can lead to the continuous development of new strains with varying properties. The interplay between the virus and its hosts, as well as the effectiveness of public health responses and interventions, will shape the future evolutionary path of the virus and its potential long-term consequences.
Persistent challenges for public health
New variants pose persistent challenges for public health systems worldwide. The continuous monitoring, testing, and surveillance needed to detect and respond to new variants require sustained resources and capacity. Additionally, the potential for reduced vaccine effectiveness against certain variants necessitates ongoing research and adaptation of vaccination strategies to maintain control over the pandemic.
Implications for future pandemics
The emergence of new variants has significant implications for future pandemics caused by similar viruses. Understanding the factors contributing to variant emergence and the impact of variants on transmission and disease severity can inform preparedness strategies for future outbreaks. Lessons learned from the current pandemic, including improvements in surveillance, research, and vaccine development, can help mitigate the impact of future viral variants.

Ongoing research on new variants
Viral genome sequencing
Ongoing research involves extensive viral genome sequencing efforts to identify and characterize new variants. Genomic surveillance enables the rapid detection and monitoring of changes in the virus’s genetic makeup. Continued sequencing efforts provide valuable data for researchers to track the evolution and spread of new variants and inform public health responses.
Laboratory experiments and modeling
Laboratory experiments and computational modeling play a crucial role in understanding the biological characteristics and behaviors of new variants. These studies help assess the transmissibility, replication rates, and potential impacts of variants on vaccines and treatments. Through these experiments and models, researchers can anticipate the behavior and consequences of newly emerging variants.
Collaborative efforts and data sharing
International collaboration and data sharing among researchers, public health agencies, and scientific communities are vital for gaining a comprehensive understanding of new variants. Sharing genomic data, research findings, and best practices helps accelerate the global response to emerging variants. Collaborative efforts facilitate the collective identification of new variants, understanding their significance, and developing effective control strategies.
Future considerations and preparedness
Continuous monitoring and surveillance
Continuous monitoring and surveillance are critical for tracking the evolution and emergence of new variants. By monitoring variant prevalence, transmissibility, and vaccine effectiveness, public health authorities can adapt their strategies and interventions to mitigate the spread and impact of emerging variants. Sustained investment in surveillance systems and technologies will be crucial in preparing for future outbreaks.
Healthcare system readiness
The ongoing battle against new variants underscores the importance of healthcare system readiness. Adequate healthcare infrastructure, including testing capacities, hospital bed availability, and healthcare workforce preparedness, is vital for managing potential surges in cases and providing appropriate care. Strengthening healthcare systems’ capacity and resilience can help mitigate the strain caused by new variants.
Research and development of antivirals
While vaccines play a crucial role in controlling the spread of the virus, antiviral treatments can provide an additional tool in managing the impact of new variants. Ongoing research and development efforts focus on identifying effective antiviral drugs that can target the virus and restrict its replication. Developing a diverse arsenal of antiviral treatments can help mitigate the impact of emerging variants and offer alternative options for treatment.
Adapting public health strategies
Effective public health strategies need to be adaptable to the changing landscape of new variants. Flexibility in testing protocols, contact tracing strategies, and preventive measures is essential to address the evolving challenges posed by new variants. Continuous evaluation of strategies and the incorporation of scientific evidence can enhance the effectiveness of public health interventions in controlling the spread of new variants and protecting public health.
The emergence of new variants of the virus presents ongoing challenges for public health authorities and the global community. Genetic mutations, selective pressures, transmission dynamics, and immunological evasion contribute to the emergence of these variants. Robust genomic surveillance, lineage classification, and standardized naming conventions aid in the identification and characterization of new variants.
New variants can impact transmission by exhibiting increased transmissibility, higher replication rates, and potential immune evasion. Key variants of concern, such as Alpha, Beta, Gamma, and Delta, have spread globally, influenced by factors like travel and population density. Efficacy studies show that existing vaccines still provide protection against severe disease, but variant-specific vaccines are being developed to enhance immunization efforts.
Public health measures, including testing, contact tracing, travel restrictions, and vaccine deployment, are implemented to control variant spread. The potential long-term consequences of new variants include the virus’s evolutionary trajectory, persistent challenges for public health, and implications for future pandemics. Ongoing research through viral genome sequencing, laboratory experiments, modeling, and collaborative efforts contribute to preparedness and future considerations.
Continuous monitoring and surveillance, readiness of healthcare systems, research and development of antivirals, and the adaptation of public health strategies are crucial in addressing the challenges posed by new variants. By staying vigilant, informed, and proactive, communities and public health authorities can effectively respond to the emergence and spread of new variants, minimizing their impact on global health.