In a world grappling with the ongoing COVID-19 pandemic, vaccines offer a beacon of hope. However, the emergence of new variants has raised concerns about their impact on vaccine efficacy. Recent studies have shed light on the effectiveness of vaccines against these variants, highlighting the need for continued vigilance and research. Join us as we explore the fascinating realm of how variants affect vaccine efficacy, and uncover the evolving landscape of our fight against the virus.
Introduction
The emergence of new variants of the COVID-19 virus has raised concerns about the efficacy of existing vaccines. These variants, also known as mutant strains, are altered versions of the original virus that have developed unique characteristics. Understanding the impact of variants on vaccine efficacy is crucial in order to develop appropriate strategies to combat the ongoing pandemic.
Overview of variants
Variants are genetic variations that occur in viruses as they replicate and spread. These changes may result in differences in the virus’s behavior, including transmission rates, severity of illness, and resistance to treatment. In the case of the COVID-19 virus, several variants have emerged since the start of the pandemic, each with its own set of characteristics.
Importance of vaccine efficacy
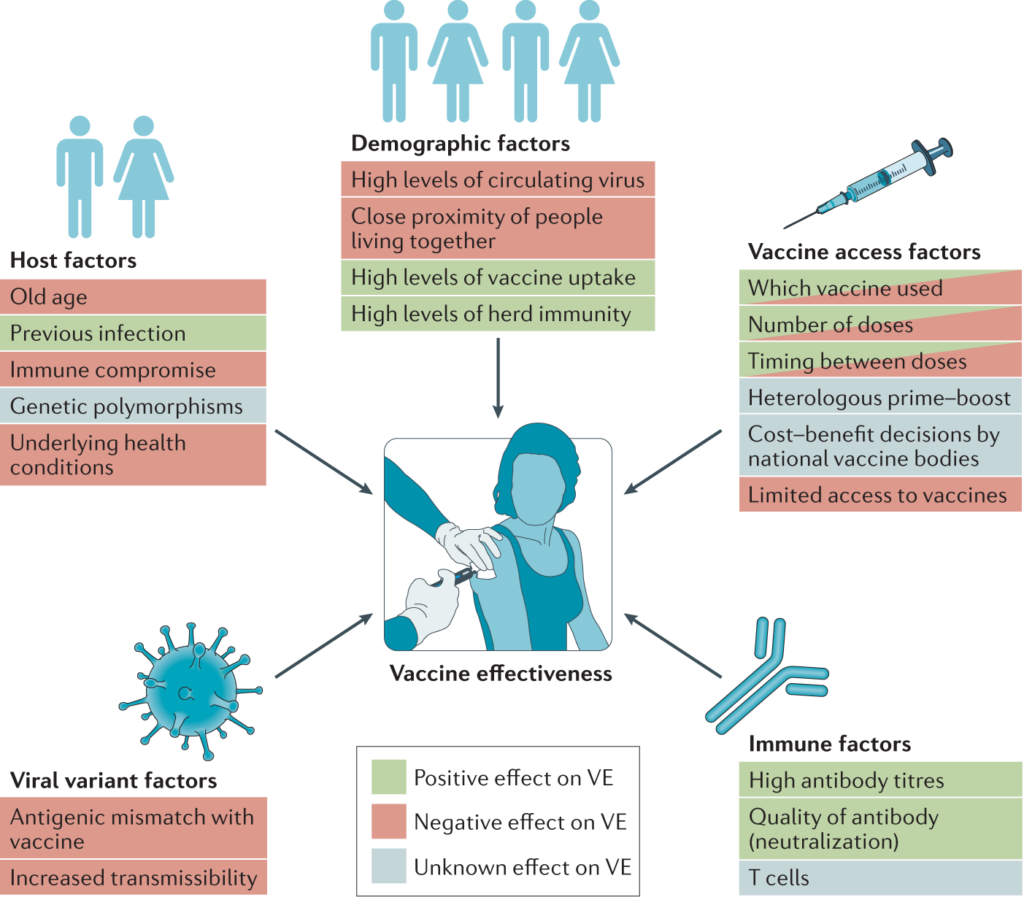
Vaccine efficacy refers to how well a vaccine prevents the target disease. High efficacy is essential in controlling and preventing the spread of infectious diseases. The emergence of variants poses challenges to vaccine effectiveness as they may evade the immune response induced by vaccines. Understanding the impact of variants on vaccine efficacy is crucial for public health officials and researchers to make informed decisions regarding vaccine development and deployment.
Understanding Variants
Definition of variants
Variants are mutations or genetic changes in the virus’s genetic material. These changes can alter the virus’s characteristics, making it behave differently from the original strain. Variants can arise naturally as the virus replicates, or they can emerge due to external factors such as exposure to selective pressure, like the immune response induced by vaccines or previous infections.
Types of variants
There are three main types of variants: Variants of Interest (VOIs), Variants of Concern (VOCs), and Variants of High Consequence (VOHCs). VOIs are variants with specific genetic changes that may affect virus characteristics but do not show evidence of increased transmissibility or disease severity. VOCs, on the other hand, have evidence of increased transmissibility, more severe disease outcomes, reduced effectiveness of treatments, or diagnostic detection failures. VOHCs, the most concerning type, have demonstrated significant impact on diagnostics, therapies, or vaccines, resulting in a substantial public health burden.
Factors contributing to variant emergence
Several factors contribute to the emergence of variants. High transmission rates provide more opportunities for the virus to replicate and mutate. Selective pressures, such as the immune response generated through vaccines or natural infections, can drive the evolution of variants that can escape immune recognition. Additionally, genetic changes can occur randomly during viral replication, leading to the emergence of novel variants.

Effects of Variants on Vaccine Efficacy
Reduced vaccine effectiveness
The emergence of variants can result in reduced vaccine effectiveness. The genetic changes in variants may affect the targeting of neutralizing antibodies induced by vaccines, reducing their ability to recognize and neutralize the virus. This can lead to breakthrough infections in individuals who have been vaccinated, although these infections tend to be milder in vaccinated individuals compared to those who are unvaccinated.
Escape mutations
One of the main concerns regarding variants is the presence of escape mutations. These mutations occur in regions of the virus that are targeted by vaccines or natural immune responses. By evading recognition by neutralizing antibodies, variants with escape mutations can continue to replicate and spread, even in vaccinated individuals.
Altered antibody response
Variants can also have an impact on the antibody response induced by vaccines. Some variants may trigger a weaker antibody response, leading to reduced protection against infection or severe disease. This highlights the need to monitor the antibody response induced by vaccines and to develop strategies to enhance protection against variant strains.
Impact on vaccine-induced immunity
The emergence of variants can affect vaccine-induced immunity in several ways. Firstly, variants may reduce the overall level of protection provided by vaccines. Secondly, they may alter the duration of protection, leading to potential waning immunity over time. Lastly, variants can impact the effectiveness of booster shots, as the immune response generated by booster doses may be less effective against variant strains.
Implications for booster shots
The presence of variants raises questions about the need for booster shots to enhance protection against new strains. Booster shots can help strengthen the immune response and provide additional protection against emerging variants. However, the selection and timing of booster shots need to be carefully evaluated, taking into account the potential impact of variants on vaccine efficacy.
Characteristics of Variant Strains
Frequent variants of concern
Several variants of concern have been identified around the world. These include the Alpha variant (B.1.1.7), the Beta variant (B.1.351), the Gamma variant (P.1), and the Delta variant (B.1.617.2). These variants have shown increased transmissibility and, in some cases, reduced vaccine effectiveness compared to the original strain.
Key mutations associated with variants
Variants often carry specific mutations that are associated with changes in their behavior. For example, the Alpha variant carries the N501Y mutation, which is believed to increase the virus’s binding affinity to the ACE2 receptor, leading to increased transmissibility. Similarly, the Beta variant carries the E484K mutation, which may affect the ability of neutralizing antibodies to recognize the virus.
Geographical distribution
The distribution of variants varies across different regions. Some variants may be more prevalent in certain areas due to local transmission dynamics or travel patterns. Monitoring the geographical distribution of variants is crucial in order to implement targeted public health interventions and control measures.

Efficacy of Current Vaccines against Variants
Effectiveness against specific variants
Current vaccines have shown varying levels of effectiveness against specific variants. For example, the Alpha variant has been shown to have reduced susceptibility to some vaccines, while the Beta and Gamma variants have demonstrated reduced neutralization by certain antibodies. However, it is important to note that even with reduced effectiveness, vaccines still provide a significant level of protection against severe disease and hospitalization caused by variants.
Variants with reduced susceptibility to vaccines
Certain variants have shown reduced susceptibility to vaccines, meaning that they can partially evade the neutralizing antibodies induced by vaccination. This reduced susceptibility can result in an increased risk of breakthrough infections in vaccinated individuals, although the severity of these infections tends to be lower compared to unvaccinated individuals.
Effectiveness of different vaccine platforms
Different COVID-19 vaccines utilize different platforms, such as mRNA, viral vector, or protein-based vaccines. The efficacy of these vaccines against variants may vary. For instance, some mRNA-based vaccines have shown good efficacy against certain variants, while viral vector-based vaccines have demonstrated reduced effectiveness against specific strains. Continued monitoring and research are necessary to assess the long-term efficacy and effectiveness of different vaccine platforms against emerging variants.
Research and Development Efforts
Tracking and surveillance of variants
Efforts to track and surveil the emergence and spread of variants are crucial in controlling the pandemic. This involves genomic sequencing of viral samples to identify new variants and monitor changes in their prevalence over time. Robust surveillance systems allow for timely identification of variants and enable public health officials to implement appropriate measures to mitigate their spread.
Development of variant-specific vaccines
Researchers are actively exploring the development of variant-specific vaccines to enhance protection against emerging strains. These vaccines can be designed to specifically target the genetic changes present in variants, potentially providing a more tailored and effective immune response.
Adaptation of existing vaccines
Another approach is to adapt existing vaccines to address the impact of variants. This may involve modifying vaccine formulations or including additional components that target the genetic changes found in variants. By updating vaccines to better match circulating variant strains, it is possible to enhance their efficacy against these specific mutations.
Investigation of cross-protection
Cross-protection refers to the ability of vaccines or natural immune responses to provide partial protection against strains that are different from the one originally targeted. Researchers are studying whether the immune response induced by currently authorized vaccines can provide cross-protection against new variants. Understanding the level of cross-protection can help inform vaccination strategies and optimize the use of available vaccines.

Public Health Measures
Importance of continued preventive measures
While vaccines play a critical role in controlling the spread of the virus, it is important to emphasize the continued adherence to preventive measures. These measures include wearing masks, practicing good hand hygiene, maintaining physical distance, and avoiding crowded indoor spaces. Combining vaccines with these preventive measures can help reduce the transmission of variants and prevent the emergence of new strains.
Enhanced testing and contact tracing
Effective testing and contact tracing are vital in identifying and containing variant-driven outbreaks. Rapid and widespread testing allows for early detection of variant cases, enabling prompt intervention and control measures. Contact tracing helps identify individuals who may have been exposed to variants, allowing for timely testing, isolation, and treatment.
Promoting vaccination coverage
To combat the impact of variants, it is crucial to promote and increase vaccination coverage. Vaccines remain highly effective at preventing severe disease and hospitalization, even against variant strains. Encouraging individuals to get vaccinated and addressing vaccine hesitancy can contribute to reducing the impact of variants on public health.
Ensuring equitable vaccine distribution
Equitable vaccine distribution is essential to mitigate the global impact of variants. Ensuring that vaccines are accessible to populations in low-income countries and marginalized communities is crucial in controlling the spread of the virus and reducing the risk of variant-driven outbreaks. International cooperation and collaboration are vital to address the disparities in vaccine availability and distribution.
Global Impact
Spread of variants across borders
The spread of variants across borders poses significant challenges in controlling the pandemic. As travel restrictions ease and international movement resumes, there is an increased risk of variant importation and subsequent transmission. Close monitoring of international travel and implementation of appropriate measures, such as testing and quarantine protocols, are necessary to prevent the rapid spread of variants.
Challenges for low-income countries
Low-income countries often face unique challenges in responding to variants. Limited healthcare resources, inadequate testing capacities, and vaccine supply constraints can hamper their ability to detect and mitigate the spread of variants. International support and collaboration are crucial in providing technical assistance, capacity building, and equitable access to vaccines for these countries.
Role of international collaboration
Addressing the impact of variants requires global collaboration and coordination. Sharing of data, research findings, and best practices among countries and organizations can help inform effective strategies to control the spread of variants and optimize vaccination efforts. International cooperation is essential in supporting low-income countries and ensuring a comprehensive and unified global response.
Surge in variant-driven outbreaks
The emergence of variants can lead to a surge in outbreaks, especially in areas with low vaccination rates or low adherence to preventive measures. These outbreaks can strain healthcare systems and pose risks to vulnerable populations. Monitoring variant-driven outbreaks and implementing targeted interventions can help mitigate the impacts and prevent the further spread of variants.

Future Outlook
Evolution of variants over time
It is important to recognize that the evolution of variants is an ongoing process that may continue as the virus continues to circulate and replicate. Monitoring the genetic changes in variants is essential to assess the potential impact on vaccine efficacy and to inform the development and deployment of strategies to control the pandemic.
Long-term vaccine strategies
Long-term vaccine strategies should take into account the possibility of ongoing variant emergence. This may include the development of booster shots tailored to target specific variants, the adaptation of existing vaccines to enhance protection against emerging strains, and the exploration of novel vaccine platforms that provide broad and durable immunity against multiple variants.
Preparedness for future pandemics
The COVID-19 pandemic has highlighted the need for robust global preparedness for future outbreaks. Investing in research and development, strengthening healthcare systems, and enhancing surveillance capabilities are crucial in detecting and responding to emerging pathogens. Lessons learned from the current pandemic should inform strategies to improve readiness for future pandemics.
Conclusion
Assessing the ongoing impact of variants on vaccine efficacy is critical in managing the COVID-19 pandemic. Continued research, surveillance, and testing are necessary to monitor the spread of variants and inform public health interventions. Adapting vaccination strategies, tracking variant evolution, and promoting international collaboration are vital in minimizing the impact of variants and controlling the spread of the virus. The challenge of variants underscores the importance of continued research and surveillance in dealing with the ever-evolving nature of infectious diseases. By staying proactive and adaptable, we can effectively combat the challenges posed by variants and work towards ending the global pandemic.