Imagine a world where a seemingly harmless respiratory infection could potentially turn deadly. This is the reality of invasive pneumococcal disease, a condition caused by the Streptococcus pneumoniae bacteria. Although it may not be a term you hear often, the lethality of invasive pneumococcal disease cannot be overlooked. In this article, we will explore the risks associated with this ailment and shed light on the importance of prevention and early intervention. So grab a cup of tea, sit back, and join us as we delve into the world of invasive pneumococcal disease.
Definition of Invasive Pneumococcal Disease
Invasive Pneumococcal Disease (IPD) refers to a serious infection caused by the bacteria known as Streptococcus pneumoniae. This disease occurs when the bacteria invade normally sterile sites in the body, such as the bloodstream, brain, or spinal cord. It can manifest as various clinical syndromes, including bacteremia (bacterial infection in the bloodstream), meningitis (infection of the membranes surrounding the brain and spinal cord), and pneumonia (infection in the lungs). IPD can also lead to complications such as sepsis, organ damage, and even death if not promptly diagnosed and treated.
Causes of Invasive Pneumococcal Disease
The main culprit behind the development of invasive pneumococcal disease is the Streptococcus pneumoniae bacteria. This bacterium is a leading cause of pneumonia, particularly in children, as well as other serious infections. The bacteria are often present in the respiratory tract of healthy individuals without causing any harm. However, certain factors can increase the risk of this bacteria becoming invasive and causing disease. These factors include a weakened immune system, chronic conditions like diabetes or heart disease, and exposure to certain environmental conditions and populations, such as overcrowding or living in close quarters.
Symptoms of Invasive Pneumococcal Disease
The symptoms of invasive pneumococcal disease can vary depending on the specific clinical presentation. However, common symptoms include fever, fatigue, cough, chest pain, shortness of breath, confusion, and headache. In cases of meningitis, patients may experience neck stiffness, sensitivity to light, and altered mental status. It is essential to note that the symptoms can rapidly progress and become severe, particularly in vulnerable individuals such as young children, the elderly, and those with underlying health conditions. If you experience any of these symptoms, it is crucial to seek immediate medical attention.
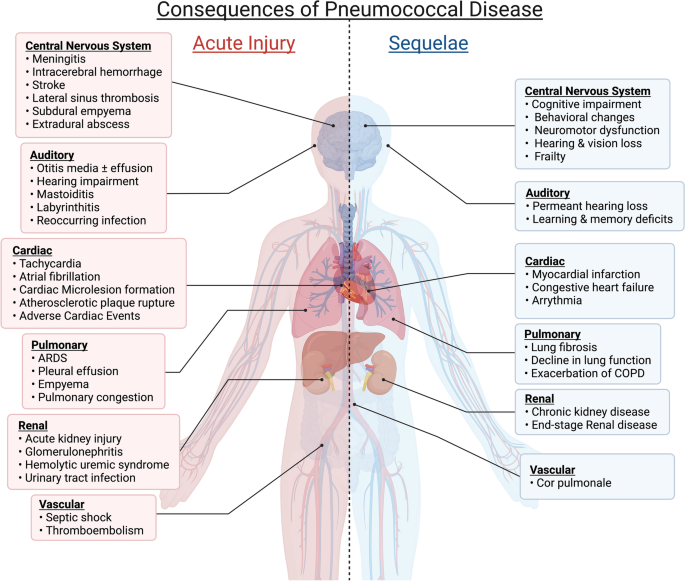
Complications of Invasive Pneumococcal Disease
Invasive pneumococcal disease can lead to various complications, some of which can be life-threatening. These complications include sepsis, a severe infection that has spread throughout the body, which can cause organ failure and even death. Meningitis, an infection of the membranes surrounding the brain and spinal cord, can result in long-term neurological damage, hearing loss, and developmental delays. Pneumonia, which is an infection in the lungs, can impair respiratory function and contribute to respiratory failure. Other potential complications include pleural effusion, empyema (pus-filled cavity), and abscesses in different organs.
Prevalence and Epidemiology
Global Burden of Invasive Pneumococcal Disease
Invasive pneumococcal disease has a significant global burden, particularly in developing countries with limited access to healthcare resources. According to the World Health Organization (WHO), this disease is estimated to cause over 1.6 million deaths annually, with the majority of the fatalities occurring in children under the age of five and the elderly. The burden of IPD is also influenced by geographical factors, socioeconomic conditions, and variations in vaccination coverage.
Risk Factors for Invasive Pneumococcal Disease
Several risk factors increase the susceptibility to invasive pneumococcal disease. Young children, especially those under the age of two, are more vulnerable due to their immature immune systems. The elderly, individuals with chronic illnesses (such as heart disease or diabetes), and those with weakened immune systems (such as HIV/AIDS patients or organ transplant recipients) are also at higher risk. Environmental factors like overcrowding, living in close quarters, and exposure to tobacco smoke further increase the chances of contracting IPD.
Vulnerable Populations
Certain population groups are more vulnerable to invasive pneumococcal disease due to various factors. Infants and children under the age of two who have not yet received the full course of pneumococcal vaccination are more susceptible to severe forms of IPD. The elderly population, particularly those over the age of 65, are also at increased risk due to age-related weakening of the immune system. Additionally, individuals with certain medical conditions such as chronic lung disease, heart disease, or diabetes, as well as those with compromised immune systems, are more prone to developing severe IPD.
Modes of Transmission and Prevention
Spread of Invasive Pneumococcal Disease
Invasive pneumococcal disease mainly spreads through person-to-person contact. The bacteria reside in the upper respiratory tract of healthy individuals and can be transmitted through respiratory droplets during coughing, sneezing, or close contact with an infected person. The bacteria can also spread indirectly by touching surfaces contaminated with the bacteria and then touching the face, nose, or mouth. It is crucial to practice good hygiene, such as covering your mouth and nose when coughing or sneezing, washing your hands frequently, and avoiding close contact with sick individuals, to minimize the spread of IPD.
Prophylactic Measures and Vaccination
Vaccination plays a vital role in preventing invasive pneumococcal disease. Pneumococcal vaccines, such as the conjugate vaccine and the polysaccharide vaccine, are available and recommended for various age groups. Vaccination is particularly crucial for infants, young children, the elderly, and individuals with underlying medical conditions. These vaccines can help reduce the risk of severe infections, hospitalizations, and complications associated with IPD. In addition to vaccination, antibiotic prophylaxis may be recommended for individuals with specific medical conditions or those at high risk of exposure to the bacteria.
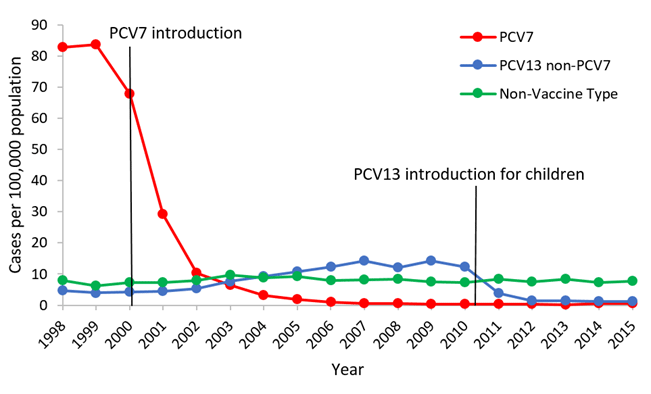
Effectiveness of Vaccination Programs
Vaccination programs have demonstrated significant effectiveness in reducing the burden of invasive pneumococcal disease. Implementation of routine childhood vaccination has led to a decline in IPD cases across different age groups. Countries that have introduced universal pneumococcal vaccination programs have reported a substantial decrease in the incidence of IPD-related hospitalizations and deaths. However, it is essential to ensure high immunization coverage rates, monitor vaccine effectiveness, and conduct regular surveillance to adapt vaccination strategies to new strains and ensure optimal protection against the disease.
Diagnosis and Laboratory Testing
Clinical Assessment and Physical Examination
Diagnosing invasive pneumococcal disease requires a combination of clinical assessment, physical examination, and laboratory testing. Healthcare providers will evaluate the patient’s medical history, including any symptoms they may be experiencing. During the physical examination, they will look for signs such as fever, respiratory distress, stiff neck, and altered mental status. These findings, along with the patient’s demographic factors, medical conditions, and exposure history, will help guide the diagnostic approach.
Laboratory Techniques for Identifying Pneumococcal Infection
Laboratory testing plays a crucial role in identifying and confirming invasive pneumococcal disease. Different techniques are used to detect the presence of the bacteria or its genetic material in patient samples. These include blood cultures, where the bacteria are cultured from a blood sample, and polymerase chain reaction (PCR), a molecular technique that can detect the bacterial DNA. Other tests, such as imaging studies (chest X-ray, CT scan) and lumbar puncture (to obtain cerebrospinal fluid), may be performed to evaluate specific clinical syndromes like pneumonia or meningitis.
Role of Serotyping and Antibiotic Susceptibility Testing
In addition to identifying the presence of the bacteria, serotyping and antibiotic susceptibility testing are important for guiding treatment decisions. Serotyping involves determining the specific serotype or strain of Streptococcus pneumoniae present in a patient’s sample. This information is valuable as different serotypes can vary in their virulence and response to antibiotics. Antibiotic susceptibility testing helps determine which antibiotics the bacteria are susceptible to and which ones may be effective in treating the infection. These tests aid healthcare providers in selecting appropriate antibiotic therapy.
Treatment and Management
Antibiotic Therapy for Invasive Pneumococcal Disease
Prompt and appropriate antibiotic therapy is crucial in the management of invasive pneumococcal disease. The choice of antibiotics depends on factors such as the severity of the infection, the identified serotype, and antibiotic susceptibility testing results. Commonly used antibiotics include penicillin and cephalosporins, although resistance to these drugs is a growing concern. In cases of severe infection, hospitalization may be required for intravenous antibiotics and close monitoring. Treatment plans should be individualized based on the patient’s clinical presentation and underlying medical conditions.
Surgical Interventions for Complications
In some cases, invasive pneumococcal disease can lead to complications that require surgical interventions. For example, individuals with empyema (pus-filled cavity) or abscesses in different organs may require drainage procedures or surgery to remove the infected material. Surgical intervention may also be necessary in cases of invasive disease affecting the central nervous system, such as drainage of abscesses in the brain or placement of a ventriculoperitoneal shunt to relieve elevated intracranial pressure.
Supportive Care and Rehabilitation
Supportive care plays a vital role in the management of invasive pneumococcal disease, particularly for critically ill patients. This includes measures such as adequate fluid resuscitation, oxygen therapy, and monitoring of vital signs. In severe cases, patients may require intensive care unit (ICU) management, including mechanical ventilation or vasopressor support. Rehabilitation may also be necessary for patients recovering from neurological complications, such as meningitis, to optimize their functional outcomes and quality of life.

Long-Term Outcomes and Prognosis
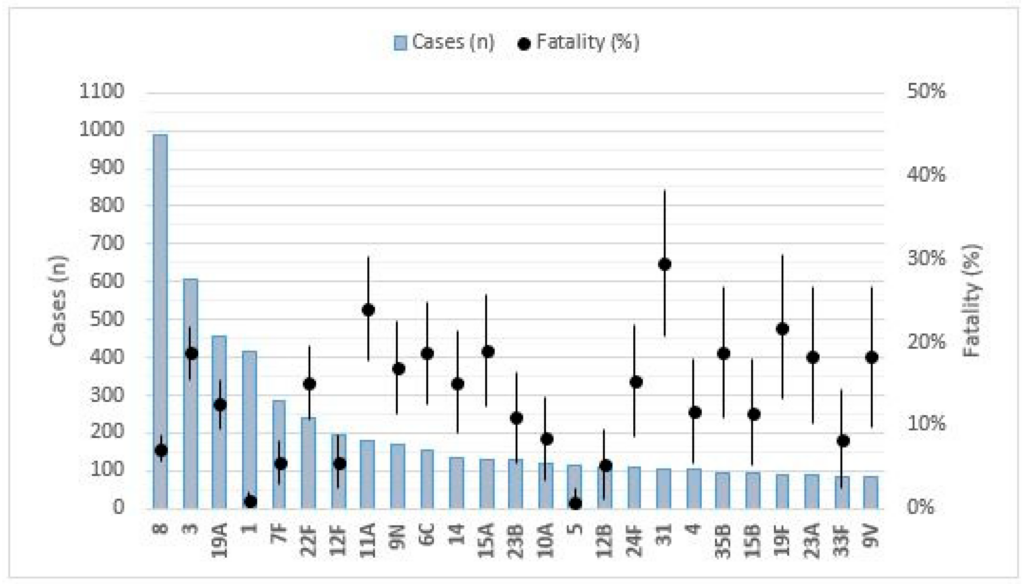
Survival Rates and Mortality
The prognosis of invasive pneumococcal disease depends on various factors, including the patient’s age, overall health, severity of the infection, and timely initiation of appropriate treatment. While mortality rates have decreased with the advent of antibiotics and vaccination, severe cases can still result in significant morbidity and mortality. The mortality rate for IPD can range from 5% to 30%, with the highest rates observed in elderly individuals and those with underlying medical conditions. Early diagnosis, appropriate antibiotic therapy, and access to critical care facilities can improve survival rates.
Sequelae and Functional Impairments
Invasive pneumococcal disease can have long-term consequences and lead to sequelae or functional impairments. Survivors of IPD, especially children and adults with meningitis, may experience neurologic deficits such as hearing loss, developmental delays, or cognitive impairments. Pneumonia caused by Streptococcus pneumoniae can also result in respiratory impairments or lung damage that may require ongoing monitoring and management. Rehabilitation services and multidisciplinary care teams play a crucial role in minimizing the impact of these sequelae and optimizing patients’ functional outcomes.
Recurrence and Reinfection
While reinfection and recurrence of invasive pneumococcal disease can occur, they are relatively rare. Streptococcus pneumoniae can cause infections in individuals even after previous exposure or previous episodes of IPD. However, the risk of recurrence is generally low, particularly in individuals who have received appropriate antibiotic therapy and have been vaccinated against the bacteria. Reinfection is more common in individuals with underlying medical conditions or those with weakened immune systems. Prevention strategies such as vaccination and appropriate antibiotic prophylaxis may help reduce the risk of reinfection.
Preventing Antibiotic Resistance
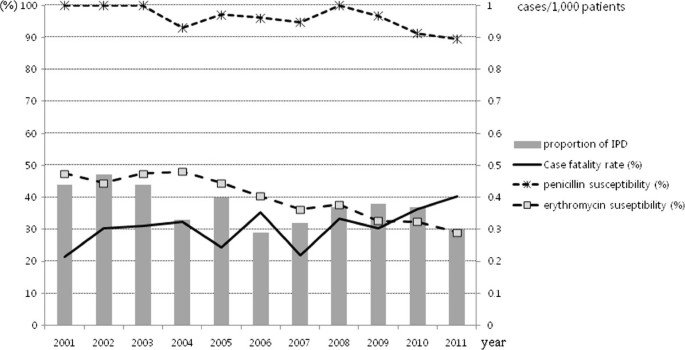
Impact of Antibiotic Resistance on Invasive Pneumococcal Disease
Antibiotic resistance is a growing concern in the management of invasive pneumococcal disease. Streptococcus pneumoniae has shown increasing resistance to several commonly used antibiotics, making treatment more challenging. This resistance can lead to treatment failure, prolonged illness, and increased mortality rates. Consequently, it is crucial to promote the appropriate use of antibiotics, adhere to recommended treatment guidelines, and implement strategies to monitor and combat antimicrobial resistance. Vaccination programs also play a crucial role in preventing antibiotic resistance by reducing the overall burden of infection.
Strategies for Antimicrobial Stewardship
Antimicrobial stewardship refers to the responsible use of antibiotics to preserve their effectiveness and minimize the development of resistance. Implementing strategies such as optimizing antibiotic prescribing practices, promoting appropriate duration of therapy, and using narrower-spectrum antibiotics when possible can help combat antibiotic resistance. It is important for healthcare professionals to stay updated on the latest guidelines and recommendations for IPD treatment to ensure appropriate antibiotic stewardship and reduce the risk of resistance.
Surveillance and Monitoring
Surveillance and monitoring programs are essential for detecting changes in antimicrobial resistance patterns and identifying emerging strains. These programs involve monitoring antibiotic susceptibility trends, identifying clusters of infections, and assessing the effectiveness of various treatment regimens. Surveillance data can guide public health interventions, inform treatment guidelines, and aid in the development of new vaccines and therapies. Ongoing monitoring is crucial to adapt strategies to combat antibiotic resistance and minimize the impact of invasive pneumococcal disease.
Healthcare Infrastructure and Resources
Availability of Diagnostic Facilities
The availability of diagnostic facilities is essential for timely and accurate diagnosis of invasive pneumococcal disease. Well-equipped healthcare facilities should have the necessary laboratory capabilities to perform blood cultures, PCR testing, and other relevant diagnostic procedures. Access to radiological facilities for imaging studies, such as chest X-rays or CT scans, is also critical for evaluating patients with suspected complications. Healthcare infrastructure should be able to provide prompt and reliable laboratory testing to ensure early detection and appropriate management of IPD.
Access to Antibiotics and Vaccines
Access to antibiotics and vaccines is a key factor in the prevention and management of invasive pneumococcal disease. Healthcare systems need to ensure the availability of essential antibiotics for IPD treatment, including those effective against resistant strains. Access to pneumococcal vaccines is crucial to prevent infections and reduce the burden of IPD. Governments and healthcare organizations must work together to ensure affordable and equitable access to these life-saving interventions globally, particularly in resource-limited settings.
Challenges in Developing Countries
Developing countries face several challenges in dealing with invasive pneumococcal disease. Limited healthcare resources, including diagnostic facilities, trained healthcare personnel, and critical care infrastructure, can hinder the timely diagnosis and management of IPD. Lack of access to affordable vaccines and antibiotics, particularly in underserved populations, contributes to the burden of the disease. Addressing these challenges requires investment in healthcare systems, strengthening laboratory capacities, improving access to essential medications, and expanding vaccination programs to reach vulnerable populations.
Public Health Interventions and Policy
Government Initiatives for Disease Control
Governments play a crucial role in implementing initiatives for the control of invasive pneumococcal disease. This includes the development and implementation of national vaccination programs targeting specific age groups and high-risk populations. Governments can also implement policies to improve access to healthcare services and essential antibiotics. Investing in public health infrastructure, surveillance systems, and data collection helps in the detection and monitoring of IPD. Governments must collaborate with healthcare professionals, international organizations, and other stakeholders to develop evidence-based policies and strategies for disease control.
Education and Awareness Campaigns
Education and awareness campaigns are essential for informing the public, healthcare professionals, and policymakers about invasive pneumococcal disease. These campaigns aim to increase knowledge about risk factors, symptoms, and preventive measures. Public health messages can emphasize the importance of vaccination, appropriate antibiotic use, and personal hygiene practices to reduce the transmission of the bacteria. Healthcare providers should be trained to recognize and manage IPD effectively. Well-designed educational campaigns can empower individuals and communities, helping prevent the spread of the disease and improve health outcomes.
International Collaboration for Prevention and Research
International collaboration plays a vital role in the prevention and research of invasive pneumococcal disease. Sharing knowledge, expertise, and resources helps accelerate progress in understanding the epidemiology, treatment, and prevention of IPD. Collaborative efforts can facilitate the development of new vaccines, therapies, and diagnostic tools. International organizations, research institutions, and healthcare providers can work together to conduct studies, share data, and develop evidence-based guidelines for IPD prevention and management. Collaborations also promote global equity by ensuring that all populations have access to effective interventions.
Future Directions and Research Priorities
Development of Novel Vaccines and Therapies
Continuous research and development are needed to improve prevention and treatment options for invasive pneumococcal disease. The development of novel vaccines that cover a wider range of serotypes is crucial to enhance protection against the bacteria. Moreover, research into alternative therapies, such as new antibiotics or immunotherapies, can help combat antibiotic resistance and improve treatment outcomes. Targeted research studies are necessary to evaluate the long-term effectiveness of vaccination programs and identify novel therapeutic approaches to tackle invasive pneumococcal disease.
Advancements in Diagnostic Techniques
Advancements in diagnostic techniques can lead to earlier and more accurate detection of invasive pneumococcal disease. Rapid point-of-care tests that can identify pneumococcal infections on-site and provide timely results would greatly aid diagnosis in resource-limited settings. New technologies, such as next-generation sequencing, have the potential to improve surveillance, identify novel strains, and monitor antimicrobial resistance. Investments in research and development of diagnostic techniques can enhance our understanding of IPD epidemiology and help in implementing effective control measures.
Investigation of Host-Pathogen Interactions
Understanding the complex interactions between the host immune system and the Streptococcus pneumoniae bacterium is crucial for developing targeted prevention and treatment strategies. Research into host-pathogen interactions can provide insights into the factors contributing to invasive disease, immune responses, and potential therapeutic targets. Investigating host genetic factors that influence susceptibility to IPD and studying the impact of vaccination on immune responses can guide the development of more effective vaccines and personalized treatment approaches.
In conclusion, invasive pneumococcal disease is a serious infection caused by Streptococcus pneumoniae. It can manifest as various clinical syndromes and lead to severe complications. Vaccination, appropriate antibiotic therapy, and supportive care are essential for management and prevention. Governments, healthcare systems, and international collaborations play a crucial role in controlling the disease, improving healthcare infrastructure, and conducting research. Continuous efforts in research and development are necessary to enhance diagnostic techniques, combat antibiotic resistance, and develop novel vaccines and therapies. With concerted efforts, invasive pneumococcal disease can be effectively managed, leading to improved health outcomes worldwide.