Imagine waking up one day feeling perfectly fine, only to find yourself in the grips of a severe respiratory infection a few hours later. This sudden onslaught of symptoms is the result of a silent and potentially deadly culprit known as invasive pneumococcal disease (IPD). In this article, we will shed light on the impact of IPD, exploring its causes, symptoms, and potential complications. By the end, you will have a deeper understanding of this invisible threat and be equipped with the knowledge to protect yourself and your loved ones. So, let’s dive into the world of invasive pneumococcal disease and unravel its mysteries together.
Definition of Invasive Pneumococcal Disease
Overview
Invasive Pneumococcal Disease (IPD) is a serious infection caused by the bacterium Streptococcus pneumoniae, also known as pneumococcus. It occurs when the bacteria invade parts of the body that are normally sterile, such as the bloodstream, lungs, lining of the brain and spinal cord, and joints. IPD can lead to severe illnesses such as pneumonia, meningitis, and septicemia, which can be life-threatening if not promptly diagnosed and treated.
Causes
IPD is primarily caused by the bacterium Streptococcus pneumoniae, a common inhabitant of the nose and throat in many healthy individuals. However, the bacteria can become invasive and cause disease when they enter the bloodstream or other normally sterile areas of the body. Pneumococcal transmission occurs mainly through respiratory droplets from an infected person, such as through coughing or sneezing. The bacteria can then colonize the respiratory tract of a susceptible individual, potentially progressing to invasive disease.
Symptoms
The symptoms of IPD can vary depending on the specific form of the disease. In cases of invasive pneumonia, symptoms may include high fever, chills, cough with sputum production, chest pain, and shortness of breath. Meningitis, another possible complication of IPD, may present with symptoms including severe headache, neck stiffness, sensitivity to light, fever, confusion, and even coma. Septic arthritis, a less common but serious manifestation of IPD, can cause joint pain, redness, swelling, and limited mobility.
Epidemiology of Invasive Pneumococcal Disease
Global Burden
IPD is a significant global health burden, particularly in low- and middle-income countries. According to the World Health Organization (WHO), an estimated 1.6 million people, including children under the age of 5, die from pneumococcal infections each year. The highest burden is observed in sub-Saharan Africa and Southeast Asia, where limited access to healthcare and high rates of malnutrition contribute to increased susceptibility to pneumococcal diseases.
Risk Factors
Several risk factors increase the susceptibility to IPD. The most significant risk factor is age, with young children, older adults, and individuals with weakened immune systems being more prone to developing severe forms of the disease. Other risk factors include chronic medical conditions such as diabetes, heart or lung disease, and having undergone a splenectomy. Additionally, certain social determinants of health, such as poverty, overcrowding, and lack of access to healthcare, can also increase the risk of IPD.
Age and Gender Distribution
IPD affects individuals of all ages, but certain age groups are more susceptible to severe disease. Young children under the age of 2 and adults aged 65 and older are at higher risk due to their immune systems being less able to mount an effective defense against the bacteria. In terms of gender distribution, IPD incidence tends to be slightly higher in males than females, although the underlying reasons for this difference are not fully understood.
Diagnosis and Testing
Clinical Examination
Diagnosing IPD typically involves a thorough clinical examination performed by a healthcare professional. The examination may include assessing the patient’s vital signs, listening to the lungs for abnormal sounds indicative of pneumonia, checking for signs of meningitis such as neck stiffness, and evaluating the affected joints for signs of arthritis. These clinical findings, along with a detailed medical history, can provide important clues to guide the diagnostic process.
Lab Tests
Laboratory testing plays a crucial role in confirming the diagnosis of IPD. Blood cultures are routinely obtained to identify the presence of pneumococcal bacteria in the bloodstream, although they may yield false-negative results if antibiotics have already been initiated. Additionally, cerebrospinal fluid analysis is essential when meningitis is suspected. Other laboratory tests, such as sputum culture or imaging-guided fluid aspiration, can be helpful in diagnosing invasive pneumonia or septic arthritis.
Imaging
Imaging studies, such as chest X-rays or computed tomography (CT) scans, are often useful in the diagnosis and management of certain complications of IPD. Chest X-rays can help identify signs of pneumonia, such as lung infiltrates or consolidations. CT scans can provide more detailed images to evaluate the extent of lung involvement or identify potential complications, such as pleural effusion or abscess formation.
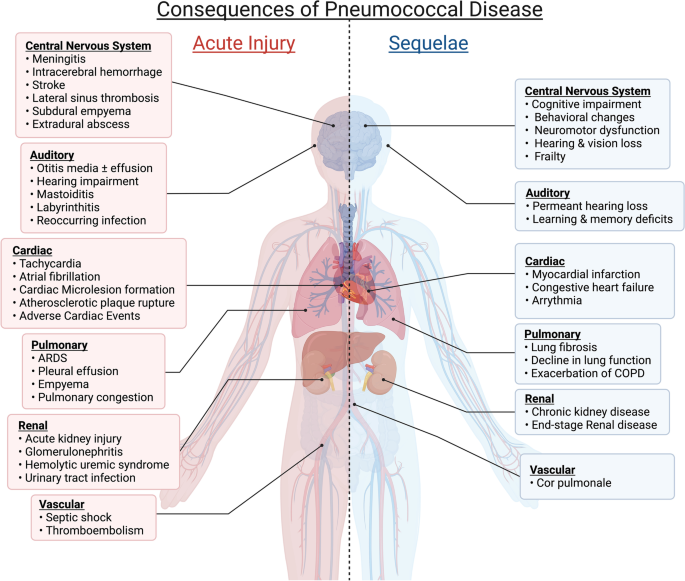
Complications of Invasive Pneumococcal Disease
Meningitis
Meningitis is a severe complication of IPD that occurs when the pneumococcal bacteria infect and cause inflammation of the membranes surrounding the brain and spinal cord. This can lead to neurological symptoms, such as headache, stiff neck, altered mental status, and even seizures or coma. Prompt diagnosis and treatment with appropriate antibiotics are crucial in preventing significant morbidity and mortality associated with pneumococcal meningitis.
Pleural Effusion
Invasive pneumonia caused by pneumococci can result in the accumulation of fluid in the pleural space, leading to a condition known as pleural effusion. This occurs when the bacteria invade the lungs and cause inflammation, resulting in the production of fluid that accumulates between the layers of the pleura. Pleural effusion can cause symptoms such as chest pain, cough, shortness of breath, and reduced lung function.
Septic Arthritis
Another potential complication of IPD is septic arthritis, which occurs when the bacteria invade and infect a joint. This can lead to joint pain, swelling, redness, warmth, and limited mobility. Prompt treatment with antibiotics and, in some cases, joint drainage is essential to prevent further damage to the affected joint and potential long-term complications.

Public Health Impact
Morbidity and Mortality
IPD can cause significant morbidity and mortality, particularly in vulnerable populations. Pneumonia caused by pneumococcal infection is a leading cause of illness and death globally, especially among children under the age of 5 and older adults. Meningitis and other invasive forms of the disease can also result in severe complications and long-term neurological sequelae if not promptly diagnosed and treated.
Economic Cost
The economic burden associated with IPD is substantial, including both direct healthcare costs and indirect costs related to lost productivity and disability. Hospitalization, antibiotics, laboratory tests, and intensive care can contribute to the financial burden on healthcare systems and individuals. Additionally, the long-term consequences of surviving severe IPD, such as neurological disabilities, can have significant economic implications on affected individuals and their families.
Preventive Strategies
Preventing IPD requires a multi-faceted approach. Vaccination is a vital component of prevention, particularly for high-risk populations such as infants, older adults, and immunocompromised individuals. Other preventive strategies include appropriate use of antibiotics, good hygiene practices (such as handwashing and respiratory etiquette), and addressing social determinants of health, such as poverty and access to healthcare.
Vaccination against Invasive Pneumococcal Disease
Vaccine Types
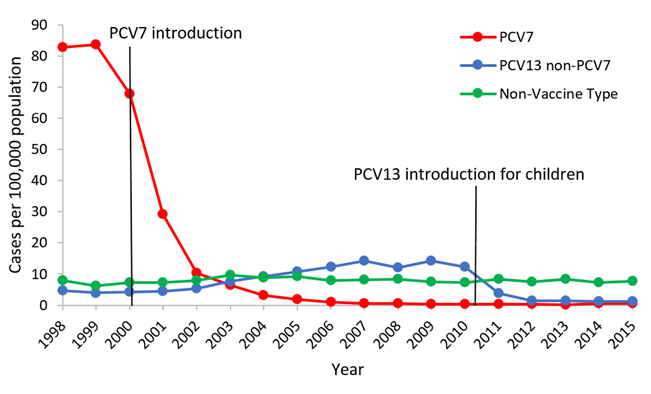
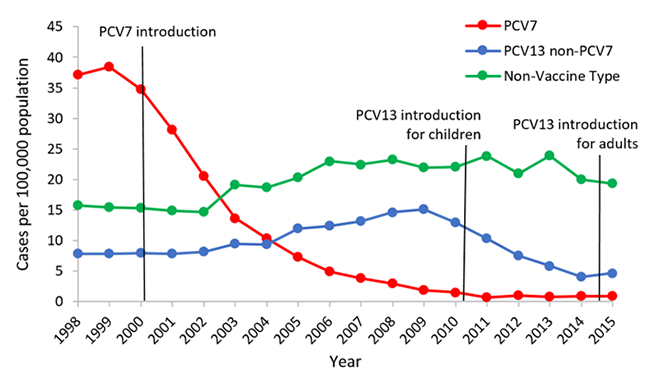
Several types of vaccines are available for the prevention of IPD. These include pneumococcal conjugate vaccines (PCVs) and pneumococcal polysaccharide vaccines (PPVs). PCVs provide protection against the most common serotypes of pneumococcal bacteria responsible for IPD in children, while PPVs are recommended for adults, particularly those at higher risk of severe disease.
Effectiveness
Vaccines have proven to be highly effective in preventing IPD and reducing associated morbidity and mortality. PCVs, in particular, have been successful in reducing the incidence of invasive pneumococcal diseases in children and adults, as well as the prevalence of antibiotic-resistant strains. While no vaccine is 100% effective, vaccination significantly decreases the likelihood of developing severe illness in vaccinated individuals.
Herd Immunity
Vaccination against pneumococcal disease can also confer indirect protection through the concept of herd immunity. When a significant portion of the population is vaccinated, the transmission of the bacterium within the community is reduced, thereby protecting vulnerable individuals who may not have been vaccinated or have a reduced immune response to the vaccine. Herd immunity plays a vital role in preventing widespread outbreaks and reducing the overall burden of pneumococcal disease.
Treatment and Management
Antibiotics
Prompt administration of appropriate antibiotics is crucial in the treatment of IPD to maximize positive outcomes. The choice of antibiotics depends on several factors, including the severity of the illness, the underlying health status of the individual, and the local antibiotic resistance patterns. Commonly used antibiotics for treating IPD include penicillin, ceftriaxone, and vancomycin.
Supportive Care
In addition to antibiotics, supportive care is an important component of managing IPD. This may include measures such as supplemental oxygen, intravenous fluids, and pain management. In severe cases, intensive care management may be necessary, including mechanical ventilation or hemodynamic support. Close monitoring and collaboration between healthcare providers are essential in ensuring optimal care for individuals with IPD.
Follow-up Care
Following treatment for IPD, individuals may require regular follow-up care to monitor for any lingering effects of the infection or potential complications. This may involve repeat laboratory testing, imaging studies, or referral to specialized healthcare providers, depending on the specific needs of the individual. It is important for healthcare providers to provide appropriate guidance and support to individuals during their recovery process.
Emerging Trends and Research
Serotype Distribution
Ongoing surveillance and research continue to shed light on the serotype distribution of pneumococcal bacteria responsible for IPD. This data helps inform vaccine development and public health strategies by identifying the most prevalent and virulent serotypes. Understanding the changing epidemiology of pneumococcal serotypes can guide the selection of vaccine formulations and ensure optimal protection against evolving strains.
Antibiotic Resistance
Antibiotic resistance is a significant concern in the management of IPD. Pneumococci have demonstrated the ability to develop resistance to commonly used antibiotics, posing challenges in treating severe infections. Continuous monitoring of antibiotic resistance patterns is crucial in guiding the selection of appropriate antibiotics and informing treatment guidelines. Additionally, efforts to promote responsible antibiotic use and development of novel therapeutic approaches are important in combating antibiotic resistance.
Novel Therapeutic Approaches
Researchers are continuously exploring novel therapeutic approaches to combat IPD. These include the development of new vaccines against emerging pneumococcal serotypes, as well as alternative treatment strategies such as targeted antimicrobial agents or host-directed therapies. Advancements in genomics and molecular diagnostics are also playing a role in identifying potential vaccine targets and improving diagnostic tools for IPD.
Challenges and Future Directions
Development of Universal Vaccines
One of the major challenges in preventing IPD is the development of universal vaccines that provide broad protection against all pneumococcal serotypes. While current vaccines cover a significant proportion of serotypes responsible for IPD, new serotypes may continue to emerge, necessitating ongoing efforts to develop vaccines with broader coverage. Additionally, addressing issues such as vaccine accessibility and vaccine hesitancy is vital in achieving optimal vaccine coverage.
Improving Surveillance
Efficient and comprehensive surveillance systems are crucial in monitoring the burden of IPD and tracking the emergence of antibiotic resistance. Enhanced surveillance can help identify susceptible populations, assess vaccine effectiveness, and guide public health interventions. Strengthening laboratory capabilities, promoting data sharing and collaboration across national and international levels, and utilizing new technologies can contribute to improved surveillance and control of IPD.
Addressing Health Disparities
Inequities in healthcare access and social determinants of health contribute to the disproportionate burden of IPD in certain populations. Addressing health disparities through increased access to quality healthcare, vaccination programs, and targeted interventions can help reduce the impact of IPD on vulnerable individuals and communities. Collaboration between healthcare providers, policymakers, and community organizations is essential in ensuring equitable prevention and management of IPD.
Conclusion
Invasive Pneumococcal Disease is a significant global health issue associated with severe morbidity, mortality, and economic burden. Streptococcus pneumoniae, the bacteria responsible for IPD, can cause life-threatening complications such as pneumonia, meningitis, and septic arthritis. Vaccination, appropriate diagnosis, and timely treatment are crucial in preventing and managing IPD. Ongoing research, surveillance, and the development of novel therapeutic approaches are necessary to address evolving epidemiology, antibiotic resistance, and challenges in vaccine coverage. By implementing preventive strategies, improving healthcare access, and addressing health disparities, we can work towards reducing the impact of IPD and improving public health outcomes worldwide.