In the world of female reproductive health, one condition that often goes undiscussed but affects many women is bacterial vaginosis. This common infection can cause discomfort and embarrassment, leading many women to seek out treatment options. Among the various methods available, antibiotics have emerged as a primary tool in combating bacterial vaginosis. This article takes a closer look at the role of antibiotics in treating this condition, exploring how they work and their effectiveness in providing relief. Whether you’re personally dealing with bacterial vaginosis or simply curious about this topic, read on to discover the important role antibiotics play in finding relief from this common ailment.

Overview of Bacterial Vaginosis
Bacterial Vaginosis (BV) is a common vaginal infection that occurs due to an imbalance in the natural bacteria present in the vagina. It is characterized by an overgrowth of certain harmful bacteria, primarily Gardnerella vaginalis, which disrupts the normal vaginal flora. BV is not a sexually transmitted infection (STI), but sexual activity can increase the risk of developing the condition.
Definition of Bacterial Vaginosis
Bacterial Vaginosis is a condition in which there is an overgrowth of harmful bacteria in the vagina, leading to an imbalance in the vaginal microbiota. It is characterized by symptoms such as abnormal vaginal discharge, a fishy odor, and itching or burning sensations.
Prevalence and Risk Factors
Bacterial Vaginosis is one of the most common vaginal infections, affecting women of reproductive age. It is estimated that BV affects about 29% of women in the United States. Certain factors can increase the risk of developing BV, including multiple sexual partners, douching, using intrauterine devices (IUDs) for contraception, and smoking.
Symptoms of Bacterial Vaginosis
The symptoms of Bacterial Vaginosis can vary from mild to severe and may include:
- Thin, white or gray vaginal discharge
- A strong fishy odor, especially after sexual intercourse
- Itching or burning sensation in and around the vagina
- Vaginal discomfort or pain during urination or sexual intercourse
It is important to note that some women with BV may not experience any symptoms at all, leading to a delayed diagnosis and treatment.
Causes and Diagnosis of Bacterial Vaginosis
Causes of Bacterial Vaginosis
The exact cause of Bacterial Vaginosis is still not fully understood, but it is believed to occur due to an imbalance in the vaginal microbiota. The vagina contains a delicate balance of different types of bacteria, including both harmful and beneficial ones. When there is a disturbance in this balance, the harmful bacteria can overgrow and cause BV.
Diagnostic Methods
To diagnose Bacterial Vaginosis, healthcare providers may perform a physical examination and collect a sample of vaginal discharge. The discharge sample is then examined under a microscope or sent to a laboratory for further analysis. The most commonly used diagnostic method is the Amsel criteria, which includes the presence of at least three out of four of the following criteria:
- Thin, white or gray vaginal discharge
- A fishy odor, especially after the addition of potassium hydroxide (KOH) to the sample
- Vaginal pH higher than 4.5
- Clue cells (vaginal cells covered with bacteria) on microscopic examination

Role of Antibiotics in Treating Bacterial Vaginosis
Importance of Antibiotics
Antibiotics play a crucial role in treating Bacterial Vaginosis by targeting and eliminating the harmful bacteria responsible for the infection. These medications can help restore the balance of the vaginal microbiota, reducing symptoms and preventing complications.
Types of Antibiotics Used
Several antibiotics can effectively treat Bacterial Vaginosis. The most commonly prescribed antibiotics for BV include:
- Metronidazole: This antibiotic is available in oral and vaginal gel forms and is highly effective in treating BV.
- Clindamycin: It is also available in oral and vaginal forms and is commonly used as an alternative treatment option.
The choice of antibiotic, dosage, and duration of treatment may vary depending on the severity of symptoms, individual factors, and healthcare provider’s preference.
Effectiveness of Antibiotics in BV Treatment
Antibiotics have shown to be effective in treating Bacterial Vaginosis. Studies have demonstrated that approximately 70-80% of women experience symptom relief and a decrease in harmful bacteria after completing a course of antibiotics. However, BV has a high rate of recurrence, with up to 50% of women experiencing a recurrence within 12 months after treatment.
Antibiotic Administration for Bacterial Vaginosis
Prescription of Antibiotics
Antibiotics for the treatment of Bacterial Vaginosis can be prescribed by healthcare providers, including gynecologists, primary care physicians, or nurse practitioners. It is important to consult a healthcare professional to confirm the diagnosis and determine the most appropriate antibiotic treatment.
Dosage and Duration
The dosage and duration of antibiotic treatment for Bacterial Vaginosis may vary depending on the specific antibiotic prescribed and the severity of symptoms. Commonly prescribed regimens include:
- Metronidazole: A typical course of oral metronidazole is 500mg, twice daily for 7 days. In some cases, a single, high-dose regimen of 2g metronidazole may be prescribed.
- Clindamycin: The usual dosage for oral clindamycin is 300mg, twice daily for 7 days. Vaginal clindamycin is usually administered as a cream or suppository for 7 days.
It is important to complete the entire course of antibiotics, even if symptoms improve before finishing the medication.
Compliance and Follow-up
To ensure successful treatment outcomes, it is essential to adhere to the prescribed antibiotic regimen and complete the full course of treatment. Additionally, healthcare providers may recommend a follow-up appointment or evaluation after completing the antibiotic treatment to assess the response to treatment and address any concerns or recurrent symptoms.

Potential Side Effects of Antibiotics
Common Side Effects
While antibiotics are generally safe and well-tolerated, they may be associated with some common side effects. These can include:
- Gastrointestinal disturbances such as nausea, vomiting, diarrhea, or abdominal pain
- Headache
- Metallic taste in the mouth
- Dizziness or lightheadedness
If any of these side effects become severe or persistent, it is crucial to contact a healthcare provider for further guidance.
Rare but Serious Side Effects
Although rare, certain antibiotics used in the treatment of Bacterial Vaginosis may have serious side effects. These can include:
- Allergic reactions, such as itching, rash, or swelling
- Severe diarrhea or colitis
- Blood disorders or liver dysfunction
If any of these serious side effects occur, immediate medical attention should be sought.
Alternative Treatment Options
For those who cannot tolerate or prefer not to use antibiotics, alternative treatment options for Bacterial Vaginosis may be considered. These can include:
- Probiotics: Certain strains of beneficial bacteria, such as Lactobacillus, can help restore the natural balance of vaginal flora.
- Boric Acid Suppositories: These suppositories can create an inhospitable environment for harmful bacteria and may be used as an alternative treatment option.
- Natural Remedies: Some natural remedies, such as tea tree oil or hydrogen peroxide, have been explored for BV treatment. However, further research is needed to establish their efficacy and safety.
It is important to discuss these alternative treatment options with a healthcare provider to ensure their safety and effectiveness.
Effects of Antibiotics on Natural Vaginal Flora
Impact on the Vaginal Microbiota
Antibiotics used in the treatment of Bacterial Vaginosis can disrupt the natural balance of the vaginal microbiota. While they target the harmful bacteria causing the infection, they may also affect the healthy bacteria present in the vagina, including the beneficial Lactobacillus species. This disruption can lead to further imbalances and increase the risk of recurrent BV.
Possible Consequences
The disruption of the vaginal microbiota caused by antibiotics can have several consequences. It can lead to a decreased number of beneficial Lactobacillus bacteria, reducing the protective effect they provide against harmful pathogens. Additionally, the alteration of the vaginal pH can create an environment favorable for the overgrowth of harmful bacteria, leading to a recurrence of BV or increased susceptibility to other vaginal infections.
Prevention and Management
To minimize the impact of antibiotics on the natural vaginal flora, it is important to consider certain preventive and management strategies. These can include:
- Probiotics: Taking probiotic supplements or using probiotic-rich products, such as yogurt or vaginal suppositories, can help restore and maintain a healthy vaginal microbiota.
- pH Balance: Maintaining a healthy vaginal pH through gentle cleansing practices and avoiding harsh soaps or douching can promote a balanced vaginal environment.
- Follow-up Care: Regular follow-up appointments with a healthcare provider can help monitor the vaginal microbiota and address any concerns or recurrent symptoms promptly.

Resistance to Antibiotics in Bacterial Vaginosis
Development of Antibiotic Resistance
Antibiotic resistance occurs when bacteria become resistant to the effects of antibiotics and continue to thrive despite treatment. Bacterial Vaginosis has shown a concerning increase in antibiotic resistance, making it more challenging to eradicate the infection. This resistance can occur due to the misuse or overuse of antibiotics, improper dosing, or incomplete courses of treatment.
Factors Contributing to Resistance
Several factors contribute to the development of antibiotic resistance in Bacterial Vaginosis. These include the frequent and inappropriate use of antibiotics, widespread use of over-the-counter medications without proper diagnosis and guidance, and the misuse of antibiotics for other infections. The emergence of resistant strains of bacteria poses a significant challenge in the effective treatment of BV.
Antibiotic Resistance Reversal Strategies
To address the issue of antibiotic resistance in Bacterial Vaginosis, various strategies can be implemented. These may include:
- Rational Antibiotic Use: Healthcare providers should prescribe antibiotics judiciously, adhering to evidence-based guidelines and considering susceptibility patterns of local bacteria.
- Combination Therapy: The use of multiple antibiotics together or in sequential regimens may improve treatment outcomes and reduce the risk of antibiotic resistance.
- Development of New Antibiotics: Continued research and development of novel antibiotics that are effective against resistant BV strains can help overcome antibiotic resistance.
Alternative Treatments for Bacterial Vaginosis
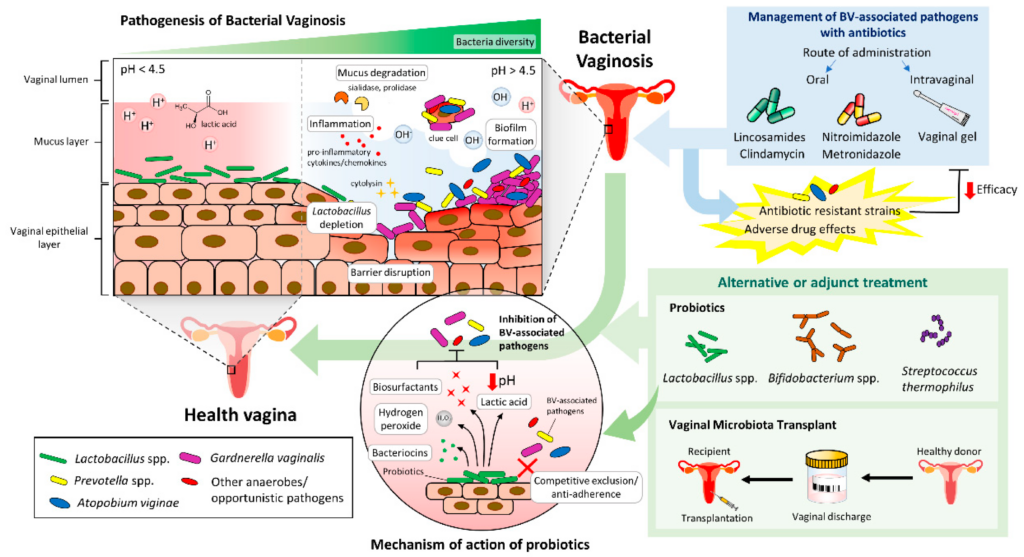
Probiotics
Probiotics are beneficial bacteria that can help restore the natural balance of the vaginal microbiota. They can be taken orally as supplements or used topically as vaginal suppositories. Probiotics, particularly those containing Lactobacillus strains, have shown promise in preventing and treating Bacterial Vaginosis. However, further research is needed to determine the most effective strains, dosages, and delivery methods.
Boric Acid Suppositories
Boric acid suppositories are an alternative treatment option for BV. Boric acid helps restore the pH balance in the vagina, creating an unfavorable environment for harmful bacteria. It is available as a vaginal suppository that can be used for several nights. However, caution should be exercised, and it is recommended to consult a healthcare provider before using boric acid for BV treatment, as it can cause irritation in some individuals.
Natural Remedies
Certain natural remedies have been explored for the management of Bacterial Vaginosis. These may include tea tree oil, hydrogen peroxide, and garlic. While these remedies may have antimicrobial properties, their efficacy and safety for treating BV are not well-established. It is essential to discuss these options with a healthcare provider before use to ensure appropriateness and minimize potential risks.
Preventing Bacterial Vaginosis Recurrence
Maintaining Vaginal Health
To prevent the recurrence of Bacterial Vaginosis, maintaining vaginal health is crucial. This can be achieved through the following practices:
- Avoid douching, as it can disrupt the natural balance of vaginal bacteria.
- Use mild, unscented soaps or cleansers for external genital hygiene.
- Avoid the use of scented products, such as tampons or menstrual pads, that can irritate the vaginal area.
- Wear breathable cotton underwear and avoid tight-fitting clothing that can create a moist environment.
Reducing Risk Factors
Certain risk factors can increase the likelihood of developing Bacterial Vaginosis. Taking steps to reduce these risk factors can help prevent recurrence:
- Limiting the number of sexual partners and practicing safe sex.
- Avoiding the use of strong or irritating substances in and around the vaginal area.
- Discussing contraceptive options with a healthcare provider to minimize the risk of BV.
Post-Treatment Care
After completing antibiotic treatment for Bacterial Vaginosis, it is essential to follow certain post-treatment care measures to reduce the risk of recurrence:
- Completing the full course of antibiotics as prescribed, even if symptoms improve.
- Receiving a follow-up evaluation to ensure the infection has been successfully treated.
- Avoiding sexual activity or using barrier methods, such as condoms, until the infection is fully resolved.
- Discussing with a healthcare provider regarding ongoing management strategies, such as probiotics or pH-balancing products.
Conclusion
The role of antibiotics in the management of Bacterial Vaginosis is crucial in targeting and eliminating the harmful bacteria responsible for the infection. They are highly effective in reducing symptoms and restoring the balance of the vaginal microbiota. However, antibiotic use can have potential side effects, impact the natural vaginal flora, and contribute to antibiotic resistance. Therefore, a holistic approach that incorporates preventive measures, alternative treatments, and post-treatment care is essential for optimal management of Bacterial Vaginosis. Further research is needed to improve treatment outcomes and identify novel strategies to address the challenges associated with this common vaginal infection.
