Hey there! Ever heard of Barrett’s Esophagus? It’s a condition that can develop in your esophagus and might lead to serious complications if left untreated. But don’t worry, in this article, we’ll break it down for you and help you understand what exactly Barrett’s Esophagus is all about. So grab a cup of tea, relax, and let’s dive into the world of esophageal health!

What is Barrett’s Esophagus
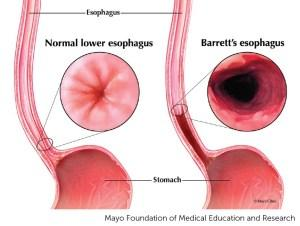
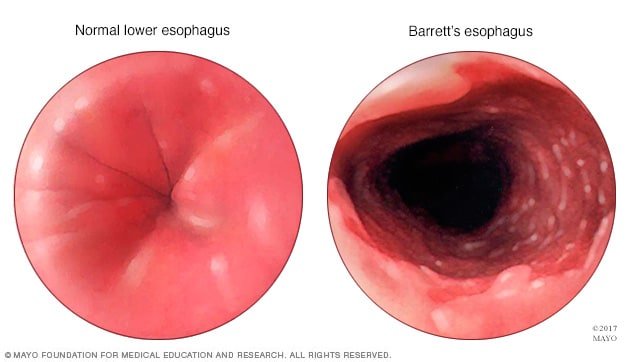
Barrett’s Esophagus is a condition that affects the lining of the esophagus, the tube that connects the throat to the stomach. In this condition, the normal cells of the esophageal lining are replaced by cells that resemble those found in the intestines. This change is known as intestinal metaplasia. Barrett’s Esophagus is often associated with chronic acid reflux, also known as gastroesophageal reflux disease (GERD). It is considered a precancerous condition, meaning that it can increase the risk of developing esophageal cancer.
Definition
Barrett’s Esophagus is defined by the presence of specialized intestinal-type cells in the lining of the esophagus. These cells are not normally found in the esophagus and are considered abnormal. The diagnosis of Barrett’s Esophagus is usually made during an upper endoscopy, a procedure in which a long, flexible tube with a camera is inserted through the mouth to examine the esophagus and collect tissue samples for biopsy.
Causes
The exact cause of Barrett’s Esophagus is not fully understood. It is believed to develop as a result of chronic irritation and inflammation of the esophageal lining caused by acid reflux. When stomach acid repeatedly flows back into the esophagus, it can cause damage to the cells lining the esophagus, leading to their abnormal transformation into intestinal-type cells.
Risk Factors
Several factors can increase the risk of developing Barrett’s Esophagus. Chronic acid reflux is the most significant risk factor. Other risk factors include obesity, smoking, male gender, and age over 50. People with a family history of Barrett’s Esophagus or esophageal cancer are also at higher risk. Additionally, certain medical conditions such as hiatal hernia and connective tissue disorders may contribute to the development of Barrett’s Esophagus.
Signs and Symptoms of Barrett’s Esophagus
Barrett’s Esophagus itself does not typically cause specific symptoms. Most people with Barrett’s Esophagus experience symptoms related to acid reflux, which include:
Heartburn
Heartburn is a burning sensation in the chest that is often accompanied by a sour or bitter taste in the mouth. It is caused by the regurgitation of stomach acid into the esophagus. While occasional heartburn is common, frequent or persistent heartburn may indicate the presence of Barrett’s Esophagus.
Difficulty swallowing
Also known as dysphagia, difficulty swallowing can occur when the esophagus becomes narrowed due to scarring or the growth of abnormal tissues. This can make swallowing food or liquids challenging and may result in a feeling of food getting stuck in the throat.
Chest pain
Chest pain associated with Barrett’s Esophagus is usually a result of acid reflux and inflammation. The pain may be burning or stabbing in nature and can sometimes be mistaken for a heart-related issue. If you are experiencing severe or persistent chest pain, it is important to seek medical attention to rule out any serious conditions.

Diagnosis of Barrett’s Esophagus
If you are experiencing symptoms suggestive of Barrett’s Esophagus or have risk factors for the condition, your doctor may recommend further evaluation to make a definitive diagnosis. The following methods are commonly used for diagnosing Barrett’s Esophagus:
Upper endoscopy
Upper endoscopy, also known as esophagogastroduodenoscopy (EGD), is the gold standard for diagnosing Barrett’s Esophagus. During this procedure, a thin, flexible tube called an endoscope is inserted through the mouth and into the esophagus. The endoscope has a camera at its tip, allowing the doctor to visualize the esophageal lining and identify any abnormalities.
Biopsy
During an upper endoscopy, the doctor may also take tissue samples, known as biopsies, from suspicious areas in the esophagus. These biopsies are then sent to a laboratory for examination under a microscope. The analysis of the biopsy samples can confirm the presence of Barrett’s Esophagus and determine the extent of any cellular abnormalities.
Imaging tests
In some cases, imaging tests such as barium swallow or esophageal ultrasound may be used to evaluate the esophagus and detect any structural abnormalities that could be indicative of Barrett’s Esophagus. These tests can provide additional information and help guide further management decisions.
Treatment Options for Barrett’s Esophagus
The treatment approach for Barrett’s Esophagus depends on the extent of the condition and the presence of cellular abnormalities. The main goals of treatment are to reduce acid reflux, control inflammation, and prevent the progression to esophageal cancer. The following treatment options may be considered:
Medications
Medications called proton pump inhibitors (PPIs) are commonly prescribed for acid reflux and can help reduce the production of stomach acid. PPIs can help alleviate symptoms and promote healing of the esophageal lining. In some cases, other medications such as H2 blockers or prokinetics may be used to manage acid reflux symptoms.
Lifestyle modifications
Certain lifestyle changes can help manage acid reflux and reduce the risk of complications. These include avoiding trigger foods that can exacerbate symptoms, maintaining a healthy weight, elevating the head of the bed while sleeping, and eating smaller, more frequent meals. Quitting smoking and reducing alcohol consumption are also beneficial.
Endoscopic therapies
For individuals with more advanced stages of Barrett’s Esophagus or cellular abnormalities, endoscopic therapies may be recommended. These procedures aim to remove or destroy the abnormal tissue. One commonly used technique is called radiofrequency ablation, which uses heat energy to destroy the abnormal cells. Other options include cryotherapy, photodynamic therapy, and endoscopic mucosal resection.
Surgery
Surgery is generally reserved for cases where other treatment options have failed or when there are severe complications. Surgical procedures for Barrett’s Esophagus typically involve removing a portion of the esophagus and reconnecting it to the stomach. Surgery may also be necessary if the condition progresses to esophageal cancer.
Complications of Barrett’s Esophagus
Barrett’s Esophagus is a significant risk factor for the development of esophageal cancer. Although the overall risk of progression to cancer is relatively low, regular monitoring and management are crucial to detect any cellular changes early. Other potential complications of Barrett’s Esophagus include:
Esophageal cancer
Barrett’s Esophagus increases the risk of developing a specific type of esophageal cancer known as adenocarcinoma. Regular surveillance and monitoring are important to detect any precancerous or cancerous changes in the esophageal lining.
Strictures
The scarring and tissue abnormalities associated with Barrett’s Esophagus can lead to the development of strictures, which are narrowings of the esophagus. Strictures can cause difficulty swallowing and may require intervention to stretch or dilate the narrowed area.
Esophagitis
Esophagitis refers to inflammation of the esophagus, often caused by acid reflux. In individuals with Barrett’s Esophagus, chronic inflammation can occur, leading to esophagitis. This can cause discomfort, pain, and other symptoms.
Prevention and Management of Barrett’s Esophagus
While there is no guaranteed way to prevent Barrett’s Esophagus, certain strategies can help reduce the risk and manage the condition more effectively:
Regular screenings
If you have risk factors for Barrett’s Esophagus, such as chronic acid reflux, it is important to undergo regular screenings. Discuss with your doctor how often you should have an upper endoscopy to check for any changes in the esophagus and detect any cellular abnormalities early.
Controlling acid reflux
Managing acid reflux is essential in preventing the progression of Barrett’s Esophagus. This can be achieved with lifestyle modifications, such as avoiding trigger foods and maintaining a healthy weight, as well as taking medications prescribed by your doctor to reduce stomach acid production.
Quitting smoking
Smoking has been shown to increase the risk of developing Barrett’s Esophagus and esophageal cancer. Quitting smoking not only reduces this risk but also has numerous other health benefits. If you need help quitting, consult your healthcare provider for guidance and resources.
Living with Barrett’s Esophagus
Living with Barrett’s Esophagus involves making certain adjustments to your lifestyle and being proactive in managing the condition. Here are some tips to help you navigate life with Barrett’s Esophagus:
Dietary changes
Certain food choices can trigger acid reflux and worsen symptoms. It is important to identify your personal trigger foods and avoid them. Common culprits include spicy foods, citrus fruits, tomatoes, fatty foods, chocolate, caffeine, and alcohol. Opting for smaller, more frequent meals can also help prevent excessive acid production and reduce reflux.
Monitoring symptoms
Keep track of your symptoms and discuss any changes or concerns with your healthcare provider. Regular check-ins and follow-ups are essential for monitoring the progression of Barrett’s Esophagus and detecting any potential complications early.
Support groups
Connecting with others who have Barrett’s Esophagus can provide valuable support and information. Joining a support group or seeking online communities can help you navigate challenges, share experiences, and learn from others who are going through a similar journey.
Research and Advances in Barrett’s Esophagus
Ongoing research and advancements in Barrett’s Esophagus aim to improve early detection, risk stratification, and treatment options. Here are some areas of active research:
Genetic studies
Scientists are studying genetic factors that may contribute to the development and progression of Barrett’s Esophagus. Understanding the genetic underpinnings of the condition may help identify individuals at higher risk and lead to targeted interventions.
New treatment approaches
Researchers are exploring novel therapeutic strategies to target the abnormal cellular changes in Barrett’s Esophagus. These include the use of immune-based therapies, molecular-targeted agents, and innovative endoscopic techniques.
Surveillance techniques
Efforts are underway to develop more accurate and less invasive surveillance techniques for Barrett’s Esophagus. New imaging modalities, such as advanced endoscopic imaging and molecular imaging, are being investigated to improve the detection of precancerous or cancerous changes.

Barrett’s Esophagus FAQs
Is Barrett’s esophagus reversible?
Barrett’s Esophagus is generally considered a permanent condition. However, with appropriate management and treatment, the progression to esophageal cancer can be prevented, and the risk of complications can be minimized. Ongoing surveillance and regular check-ups are important to monitor any changes in the esophageal lining.
Can Barrett’s esophagus cause weight loss?
Barrett’s Esophagus itself does not directly cause weight loss. However, if acid reflux and its related symptoms are severe, it may lead to a reduced appetite and weight loss. Managing acid reflux effectively through lifestyle modifications and medications can help prevent weight loss.
Can lifestyle changes alone treat Barrett’s esophagus?
Lifestyle changes, such as modifying diet, maintaining a healthy weight, and quitting smoking, are important components of managing Barrett’s Esophagus. However, in most cases, additional interventions may be necessary, such as medication or endoscopic therapies. It is essential to work closely with your healthcare provider to develop an individualized treatment plan.
Conclusion
Barrett’s Esophagus is a condition characterized by the presence of abnormal cells in the esophageal lining. Although it is a precancerous condition, with proper management and surveillance, the risk of developing esophageal cancer can be minimized. Regular screenings, controlling acid reflux, and adopting a healthy lifestyle are key in preventing and managing Barrett’s Esophagus. Advances in research and treatment continue to improve outcomes and offer hope for those affected by this condition. If you suspect you may have Barrett’s Esophagus or have risk factors, consult with your healthcare provider for further evaluation and personalized care.