Are you or a loved one struggling with bladder incontinence? If so, it’s important to understand what exactly bladder incontinence is and how it can affect your daily life. Bladder incontinence refers to the involuntary leakage of urine, and it can occur for various reasons such as weakened bladder muscles, urinary tract infections, or even certain medications. This article will explore the causes, symptoms, and management techniques for bladder incontinence, providing you with the knowledge you need to effectively deal with this common issue. So, let’s dive in and gain a better understanding of bladder incontinence together.

What is Bladder Incontinence?
Bladder incontinence, also known as urinary incontinence, is a condition characterized by the involuntary leakage of urine. It occurs when the muscles and nerves that control the bladder are weakened or damaged, leading to a loss of control over urination. Bladder incontinence can be a distressing and embarrassing problem that can significantly impact a person’s quality of life. However, it is important to note that bladder incontinence is not a normal part of aging and can be treated and managed effectively with the right approach.
Definition
Bladder incontinence refers to the inability to control the release of urine from the bladder, resulting in involuntary leakage. This loss of bladder control can range in severity, from occasionally leaking small amounts of urine to having a complete inability to hold urine. It can affect people of all ages, although it is more common in older adults and women. There are different types and causes of bladder incontinence, which we will explore further in this article.
Types of Bladder Incontinence
There are several types of bladder incontinence, each with its own causes and symptoms. These include:
-
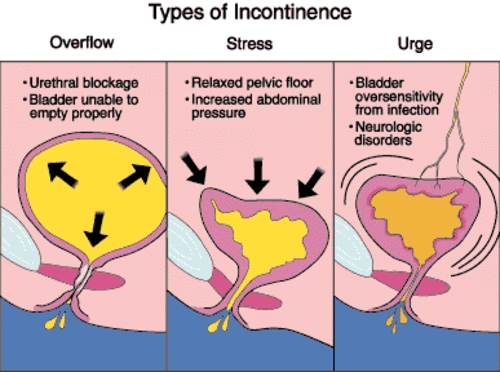
Stress incontinence: This type of incontinence occurs when there is an increase in pressure on the bladder, leading to the leakage of urine. Activities such as coughing, sneezing, laughing, or exercising can trigger this type of incontinence.
-
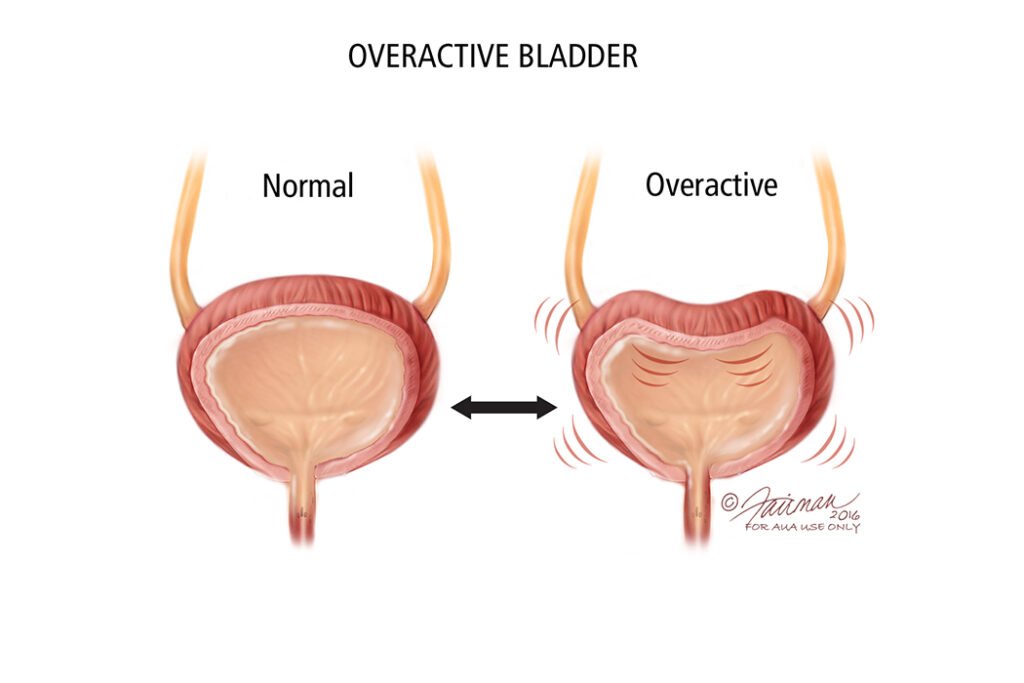
Urge incontinence: Also known as overactive bladder, urge incontinence is characterized by a sudden and strong urge to urinate, followed by involuntary urine leakage. This can happen even when the bladder is not full.
-
Overflow incontinence: This type of incontinence occurs when the bladder does not empty completely, causing it to constantly overflow. It can result from conditions that obstruct the flow of urine, such as an enlarged prostate in men, or neurological disorders that affect bladder function.
-
Mixed incontinence: Mixed incontinence refers to a combination of two or more types of incontinence, commonly stress and urge incontinence.
-
Functional incontinence: This type of incontinence occurs when a person is unable to reach the toilet in time because of physical or cognitive impairments, such as mobility issues or dementia.
Understanding the specific type of bladder incontinence is important in order to determine the most appropriate treatment and management strategies. Now, let’s explore the causes of bladder incontinence in more detail.
Causes of Bladder Incontinence
Bladder incontinence can have various underlying causes, ranging from medical conditions to lifestyle factors. Understanding the cause of the condition is crucial in order to develop an effective treatment plan. Let’s explore some of the common causes of bladder incontinence:
Medical Conditions
Several medical conditions can contribute to bladder incontinence. These include:
-
Urinary tract infections (UTIs): Infections in the urinary tract can irritate the bladder lining and cause temporary incontinence. This typically resolves once the infection is treated.
-
Neurological disorders: Conditions such as multiple sclerosis, Parkinson’s disease, spinal cord injuries, and stroke can affect the nerves that control bladder function, leading to incontinence.
-
Diabetes: Uncontrolled diabetes can cause damage to the nerves that control bladder function, resulting in incontinence.
-
Pelvic organ prolapse: When the muscles and tissues that support the pelvic organs weaken, the organs can descend into the vagina, putting pressure on the bladder and causing incontinence.
-
Prostate problems: In men, an enlarged prostate or prostate surgery can lead to bladder incontinence.
Age and Gender
Bladder incontinence is more common in older adults, particularly women. This is due to age-related changes in the muscles and tissues that support the bladder and urethra. Additionally, hormonal changes during menopause can contribute to bladder incontinence in women.
Pregnancy and Childbirth
The physical changes that occur during pregnancy, such as hormonal shifts and pressure on the bladder from the growing fetus, can weaken the pelvic floor muscles and lead to incontinence. Vaginal childbirth can also stretch and damage the muscles and nerves that control bladder function.
Menopause
During menopause, the body experiences a decline in estrogen levels, which can weaken the pelvic floor muscles and contribute to bladder incontinence.
Medications and Alcohol
Certain medications, such as diuretics, muscle relaxants, and sedatives, can increase urine production or relax the bladder muscles, leading to incontinence. Alcohol and caffeine can also irritate the bladder and increase urine production.
Urinary Tract Infections
Infections in the urinary tract can irritate the bladder and cause temporary incontinence. Treating the infection usually resolves the incontinence.
Neurological Disorders
Conditions that affect the nerves involved in bladder control, such as multiple sclerosis or Parkinson’s disease, can result in bladder incontinence.
Obesity
Excess weight can put additional pressure on the bladder and pelvic floor muscles, increasing the risk of bladder incontinence.
Identifying the underlying cause of bladder incontinence is crucial in order to determine the most appropriate treatment plan. Once the cause is determined, healthcare providers can develop a personalized approach to managing and treating bladder incontinence. In the next section, we will explore the common symptoms of bladder incontinence.

Symptoms of Bladder Incontinence
Bladder incontinence can manifest itself through various symptoms, which can vary depending on the type and severity of incontinence. The most common symptoms of bladder incontinence include:
Urinary Leakage
One of the primary symptoms of bladder incontinence is the involuntary leakage of urine. This can range from occasional small leaks to a complete loss of control over urination. Leakage can occur during everyday activities such as coughing, sneezing, laughing, exercising, or even just standing up.
Strong Urgency to Urinate
People with bladder incontinence often experience a sudden and intense urge to urinate, which can be difficult to control. This urgency may make it challenging to reach the bathroom in time, resulting in episodes of leakage.
Frequent Urination
Bladder incontinence may also lead to an increased frequency of urination. Individuals may feel the need to urinate more frequently during the day, and may also need to get up multiple times during the night to urinate.
Nocturia
Nocturia refers to the need to wake up from sleep to urinate. It can disrupt sleep patterns and have a negative impact on overall sleep quality.
Experiencing these symptoms can be not only physically uncomfortable, but also emotionally distressing. It is important to remember that bladder incontinence is a common condition that can be managed effectively with the right treatment plan. In the next section, we will discuss the diagnostic procedures that healthcare providers may use to assess bladder incontinence.
Diagnosis of Bladder Incontinence
In order to diagnose bladder incontinence and develop an appropriate treatment plan, healthcare providers will typically conduct a thorough evaluation. This may involve the following steps:
Medical History
Obtaining a detailed medical history is the first step in diagnosing bladder incontinence. Healthcare providers will ask about the frequency and severity of symptoms, any factors that worsen or improve symptoms, and any underlying medical conditions or medications that could contribute to incontinence.
Physical Examination
A physical examination allows healthcare providers to assess the pelvic area and look for any signs of pelvic organ prolapse or other physical abnormalities that may be contributing to incontinence.
Urinalysis
A urinalysis is a laboratory test that examines a urine sample for signs of infection, blood, or other abnormalities that may be causing or contributing to bladder incontinence.
Bladder Diary
A bladder diary is a record of daily urinary habits, including the amount of fluids consumed, frequency of urination, any episodes of leakage, and associated factors such as activities, foods, and beverages consumed. This diary helps healthcare providers understand patterns and triggers related to incontinence.
Post-void Residual Volume
Measuring the post-void residual volume involves using ultrasound or a catheter to assess how well the bladder empties after urination. This can help determine if there is any urine left in the bladder, which may indicate a problem with bladder emptying.
Bladder Stress Test
A bladder stress test involves coughing or performing activities that increase pressure on the bladder while healthcare providers observe for any signs of urine leakage. This test helps identify stress incontinence, where physical stress triggers bladder leakage.
By utilizing these diagnostic procedures, healthcare providers can accurately diagnose bladder incontinence and determine the most appropriate treatment options. In the next section, we will explore the various treatment options available for bladder incontinence.
Treatment Options for Bladder Incontinence
The treatment options for bladder incontinence depend on the underlying cause, severity, and type of incontinence. Treatment can range from conservative, non-invasive approaches to more invasive interventions. Some of the common treatment options for bladder incontinence include:
Behavioral Techniques
Behavioral techniques involve making lifestyle changes and adopting habits that can help manage and prevent bladder incontinence. These may include timed urination, double voiding (emptying the bladder twice during each bathroom visit), and fluid management strategies.
Pelvic Floor Muscle Exercises
Also known as Kegel exercises, pelvic floor muscle exercises can be effective in strengthening the muscles that support the bladder and control urination. These exercises involve contracting and relaxing the pelvic floor muscles, which can enhance bladder control.
Medications
Certain medications can be prescribed to manage bladder incontinence. These may include medications that relax the bladder muscles, reduce the frequency and urgency of urination, or treat underlying medical conditions that contribute to incontinence.
Surgical Interventions
In some cases, surgical intervention may be necessary to treat bladder incontinence. Procedures such as bladder suspension, sling procedures, or artificial urinary sphincters can help support the bladder and improve urine control.
Bladder Training
Bladder training involves gradually increasing the intervals between urination to train the bladder to hold urine for longer periods. This technique can be effective in managing urge incontinence and increasing bladder capacity.
Vaginal Devices and Inserts
Certain devices, such as vaginal pessaries or urethral inserts, can provide additional support to the pelvic organs and help manage bladder incontinence.
The choice of treatment will depend on the individual’s specific situation and goals. Healthcare providers will consider factors such as the severity of incontinence, the presence of underlying medical conditions, and the individual’s preferences and lifestyle. Alongside these treatment options, certain lifestyle changes can also be beneficial in managing bladder incontinence. Let’s explore these lifestyle changes in more detail.
Lifestyle Changes to Manage Bladder Incontinence
In addition to medical treatments, introducing certain lifestyle changes can play a significant role in managing bladder incontinence. These lifestyle modifications include:
Diet Modifications
Making changes to your diet can help manage bladder incontinence. Limiting or avoiding foods and drinks that can irritate the bladder, such as caffeine, alcohol, spicy foods, citrus fruits, and carbonated beverages, can help reduce symptoms.
Fluid Management
Proper fluid management is important for maintaining bladder health. While it is important to stay hydrated, reducing fluid intake in the evening can help minimize nighttime incontinence episodes.
Toilet Habits
Establishing a regular voiding schedule and taking the time to fully empty the bladder can help manage bladder incontinence. Additionally, avoiding rushing to the bathroom and making sure to completely empty the bladder can help prevent any residual urine that may lead to infection or incontinence.
Weight Management
Maintaining a healthy weight is important for managing bladder incontinence. Excess weight can put additional pressure on the bladder, exacerbating symptoms. Engaging in regular physical activity and adopting a well-balanced diet can support weight management.
Smoking Cessation
Smoking can worsen bladder incontinence symptoms. The toxins in cigarette smoke can irritate the bladder and increase coughing, which can trigger episodes of stress incontinence. Quitting smoking can improve overall bladder health.
Avoiding Bladder Irritants
Certain substances can irritate the bladder and worsen incontinence symptoms. This includes caffeine, alcohol, artificial sweeteners, spicy foods, and acidic fruits. Avoiding these bladder irritants can help manage symptoms.
By implementing these lifestyle changes, individuals can experience an improvement in bladder control and overall quality of life. Now, let’s discuss additional coping strategies and support options for individuals with bladder incontinence.

Coping Strategies and Support for Bladder Incontinence
Living with bladder incontinence can be challenging, both physically and emotionally. However, there are coping strategies and support options available to help individuals manage and overcome these challenges. Some of these strategies include:
Emotional Support
Seeking emotional support from loved ones, support groups, or healthcare professionals can be invaluable for individuals with bladder incontinence. Sharing experiences and feelings with others who understand can provide a sense of validation and support.
Pelvic Floor Physical Therapy
Pelvic floor physical therapy involves working with a specialized physical therapist who can provide targeted exercises, techniques, and strategies to strengthen the pelvic floor muscles and improve bladder control.
Bladder Training
Behavioral techniques, such as bladder training, can be effective in managing bladder incontinence. Working with healthcare providers or pelvic health specialists, individuals can develop personalized bladder training strategies to regain control over urination.
By employing these coping strategies and utilizing available support options, individuals can better manage bladder incontinence and improve their overall well-being. In the next section, we will discuss prevention and self-care measures that can help reduce the risk of developing bladder incontinence.
Prevention and Self-Care Measures for Bladder Incontinence
While some risk factors for bladder incontinence, such as age and gender, cannot be controlled, there are certain preventive measures and self-care strategies that individuals can adopt to reduce their risk or manage their symptoms. These include:
Maintaining a Healthy Weight
Maintaining a healthy weight can help reduce the risk of developing bladder incontinence. By adopting a balanced diet and engaging in regular physical activity, individuals can support overall bladder health.
Strengthening Pelvic Floor Muscles
Regularly practicing pelvic floor muscle exercises, such as Kegels, can help strengthen the pelvic floor muscles and improve bladder control. These exercises can be beneficial not only for the prevention of incontinence but also for managing existing symptoms.
Avoiding Bladder Irritants
Being mindful of substances that can irritate the bladder, such as caffeine, alcohol, and spicy foods, can help prevent bladder incontinence or reduce symptoms. Moderation or avoidance of these bladder irritants can support bladder health.
Quitting Smoking
Smoking can worsen bladder incontinence symptoms and contribute to various other health issues. Quitting smoking can improve bladder function and overall health.
Emptying the Bladder Regularly
Emptying the bladder at regular intervals, rather than holding urine for extended periods, can help prevent bladder incontinence. This can be achieved through a regular voiding schedule.
Keeping Proper Hygiene
Maintaining proper hygiene, including wiping from front to back after using the toilet and practicing good perineal care, can reduce the risk of urinary tract infections and potential complications leading to bladder incontinence.
Implementing these preventive and self-care measures can contribute to the maintenance of overall bladder health and reduce the risk of developing bladder incontinence. In the next section, we will explore the impact of bladder incontinence on quality of life.
Impact of Bladder Incontinence on Quality of Life
Bladder incontinence can have a significant impact on an individual’s quality of life. It can affect various aspects, including emotional well-being, social interactions, and work life.
Emotional and Psychological Effects
Bladder incontinence can cause feelings of embarrassment, shame, and loss of control. It can lead to a decreased quality of life, anxiety, depression, and social isolation. These emotional and psychological effects can have a profound impact on a person’s well-being and overall happiness.
Social Implications
Bladder incontinence can greatly impact social interactions and activities. Individuals may avoid social events, intimate relationships, or physical activities due to fear of leakage or embarrassment. This can result in a loss of enjoyment and a sense of isolation.
Work and Professional Life
Bladder incontinence can also impact an individual’s work and professional life. Frequent bathroom trips or interruptions due to leakage can affect productivity, concentration, and confidence in the workplace.
It is important to recognize the emotional and social implications of bladder incontinence and seek appropriate support. Understanding that bladder incontinence is a common condition and that effective treatment options are available can help individuals regain control and improve their quality of life.
Conclusion
Bladder incontinence is a common and treatable condition characterized by the involuntary leakage of urine. It can be caused by various factors, including medical conditions, age, gender, pregnancy, childbirth, menopause, medications, urinary tract infections, neurological disorders, and obesity. Symptoms of bladder incontinence may include urinary leakage, strong urgency to urinate, frequent urination, and nocturia.
Diagnosis of bladder incontinence involves a combination of medical history, physical examination, urinalysis, bladder diary, post-void residual volume measurement, and bladder stress test. Treatment options can include behavioral techniques, pelvic floor muscle exercises, medications, surgical interventions, bladder training, and the use of vaginal devices and inserts. Alongside medical treatments, making certain lifestyle changes, such as diet modifications, fluid management, toilet habits, weight management, smoking cessation, and avoiding bladder irritants, can contribute to the management of bladder incontinence. Coping strategies, emotional support, and pelvic floor physical therapy can also aid in managing the condition.
Implementing preventive measures, such as maintaining a healthy weight, strengthening pelvic floor muscles, avoiding bladder irritants, quitting smoking, emptying the bladder regularly, and practicing proper hygiene, can help reduce the risk of developing bladder incontinence.
Bladder incontinence can have a significant impact on an individual’s quality of life, including emotional and psychological effects, social implications, and challenges in the workplace. However, with proper management and support, individuals can regain control and improve their overall well-being. It is important to seek help from healthcare providers and support networks to develop a personalized treatment plan and enhance quality of life.
