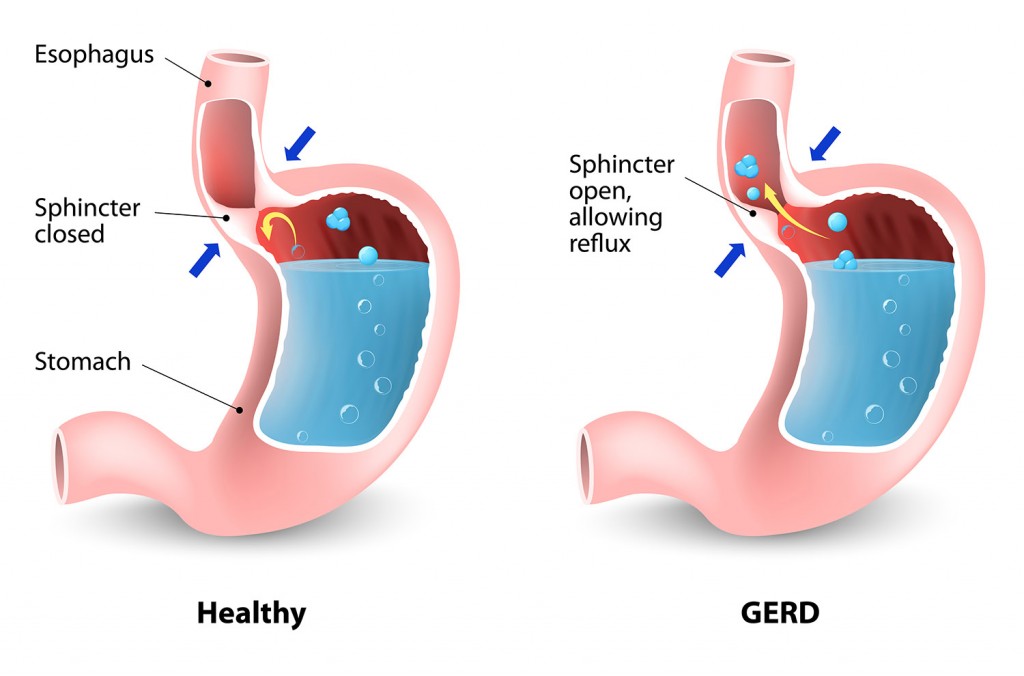
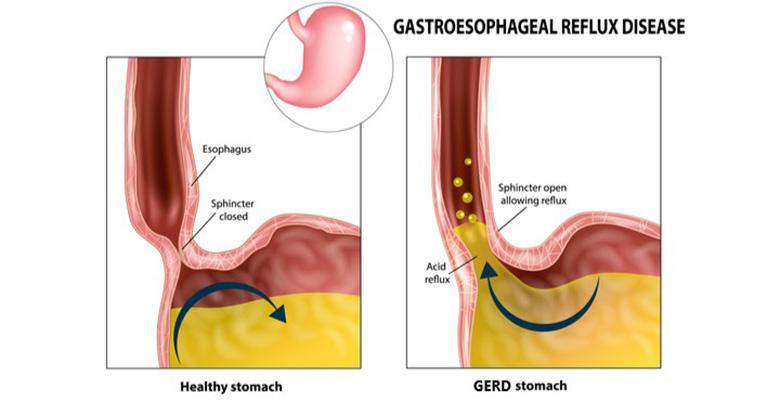
Have you ever experienced that uncomfortable burning sensation in your chest after a meal? If so, you may have encountered gastro-oesophageal reflux disease (GERD). This article aims to provide a comprehensive understanding of GERD, its causes, symptoms, and potential treatment options. So, if you’ve been plagued by heartburn and need some clarity, keep reading!
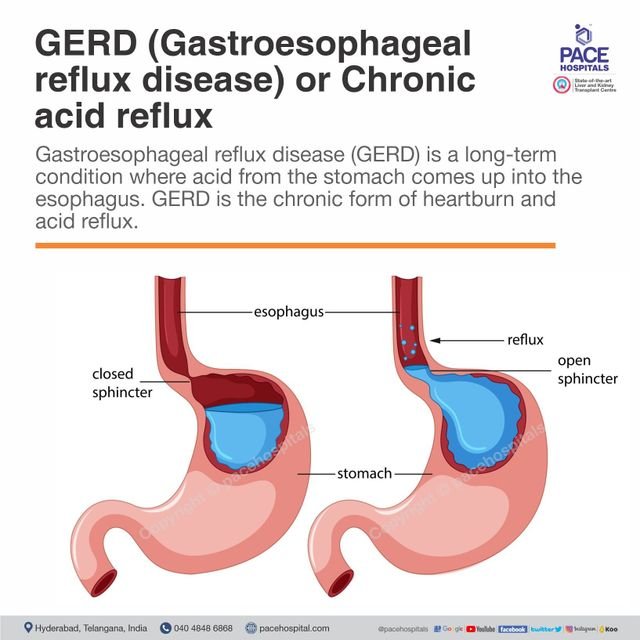
Overview
Gastro-oesophageal Reflux Disease (GERD) is a chronic condition where stomach acid flows back into the oesophagus, causing discomfort and sometimes damage to the lining of the oesophagus. It is a common condition that affects many individuals worldwide. Understanding the causes, symptoms, complications, diagnosis, treatment, prevention, management, risk factors, and lifestyle modifications associated with GERD can significantly improve your quality of life.
Definition
GERD is a chronic condition characterized by the reflux of stomach acid into the oesophagus. The lower oesophageal sphincter, a muscular valve that separates the stomach from the oesophagus, becomes weak or relaxes abnormally, allowing the stomach acid to flow back up into the oesophagus. This acid reflux can cause various symptoms such as heartburn, regurgitation, and chest pain.
Prevalence
GERD is a prevalent condition, affecting a significant number of individuals worldwide. It is estimated that approximately 20% of the population in Western countries experience symptoms of GERD at least once a week, while up to 10% experience symptoms on a daily basis. The incidence of GERD has been increasing in recent years, possibly due to changes in lifestyle, diet, and other environmental factors.
Causes
Several factors can contribute to the development of GERD. Obesity, hiatal hernia, pregnancy, smoking, and certain medications are known risk factors for the condition. Obesity, in particular, can increase abdominal pressure, pushing the stomach contents upward. Hiatal hernia is another condition where a portion of the stomach pushes up into the chest through the diaphragm, weakening the lower oesophageal sphincter. Pregnancy can also put pressure on the stomach, leading to acid reflux. Smoking and certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and calcium channel blockers, can also increase the risk of GERD.
Symptoms
The most common symptoms associated with GERD include heartburn, regurgitation, and chest pain. Heartburn, a burning sensation in the chest that often occurs after meals or when lying down, is one of the hallmark symptoms of GERD. Regurgitation is the sensation of acid rising up into the throat or mouth. Chest pain, often mistaken for a heart attack, can also occur due to the irritation of the oesophagus. Other symptoms may include difficulty swallowing (dysphagia), hoarseness, chronic cough, and a sour taste in the mouth.
Complications
If left untreated, GERD can lead to various complications. Esophagitis, inflammation of the oesophagus, can result from the constant exposure of the oesophageal lining to stomach acid. This can cause pain, difficulty swallowing, and even bleeding. Esophageal stricture, a narrowing of the oesophagus, can also occur due to the scarring caused by repeated acid reflux. Barrett’s oesophagus, a condition where the lining of the oesophagus changes and becomes similar to the lining of the intestine, is another potential complication of GERD. This condition is a precursor to oesophageal cancer. Additionally, GERD can contribute to respiratory problems such as asthma, chronic cough, and recurrent pneumonia.

Diagnosis
To diagnose GERD, your healthcare provider will consider your medical history, perform a physical examination, and may order diagnostic tests when necessary.
Medical History
Your healthcare provider will ask about your symptoms, their frequency and severity, and any factors that may trigger or worsen them. They will also inquire about your diet, lifestyle, and any medications you may be taking. The medical history will help to establish a pattern of symptoms and potential risk factors for GERD.
Physical Examination
During the physical examination, your healthcare provider may check for signs of GERD, such as heartburn or the presence of an inflamed oesophagus. They may also examine your abdomen for any swelling or tenderness. This examination will provide additional information to support the diagnosis.
Diagnostic Tests
If necessary, your healthcare provider may order certain diagnostic tests to confirm the presence of GERD or assess its severity. These tests may include an upper gastrointestinal (GI) endoscopy, where a thin tube with a camera is inserted into the oesophagus to examine the lining. A pH monitoring test can measure the acidity in the oesophagus over a period of time. Other tests, such as a barium swallow or oesophageal manometry, may also be performed to evaluate the function of the oesophagus and the lower oesophageal sphincter.
Treatment
The treatment for GERD typically involves a combination of lifestyle modifications, medications, and, in some cases, surgery. The goal is to alleviate symptoms, heal any existing damage to the oesophagus, and prevent the recurrence of acid reflux.
Lifestyle Modifications
Making changes to your lifestyle can significantly reduce the frequency and severity of GERD symptoms. It is advisable to maintain a healthy weight, as obesity is a significant risk factor for GERD. Avoiding triggers such as caffeine, alcohol, spicy foods, and fatty foods can also help. Elevating the head of the bed, eating smaller meals, and avoiding lying down immediately after eating are additional lifestyle changes that can make a difference.
Medications
Medications are commonly prescribed to control the symptoms of GERD and reduce the amount of acid produced in the stomach. Antacids, such as calcium carbonate or magnesium hydroxide, can provide temporary relief by neutralizing stomach acid. H2 blockers, such as ranitidine or famotidine, reduce the production of stomach acid. Proton pump inhibitors (PPIs) are the most potent acid-suppressing medications and are typically prescribed for severe or persistent GERD symptoms.
Surgery
In cases where lifestyle modifications and medications do not provide sufficient relief, surgical intervention may be considered. Fundoplication is a surgical procedure where the upper part of the stomach is wrapped around the lower oesophageal sphincter, reinforcing its closure. The LINX procedure involves placing a ring of small magnetic beads around the junction of the stomach and oesophagus to prevent acid reflux. Endoscopic procedures, such as radiofrequency ablation or stenting, may be performed to treat complications of GERD or to manage symptoms.
Prevention
There are several measures you can take to prevent or reduce the risk of developing GERD.
Dietary Recommendations
Maintaining a healthy diet is crucial in preventing GERD. It is advisable to avoid foods and beverages that trigger acid reflux, such as caffeine, alcohol, spicy foods, fatty foods, and acidic foods. Instead, opt for a diet rich in fruits, vegetables, whole grains, and lean proteins. It may also be helpful to eat smaller, more frequent meals rather than large meals.
Healthy Habits
Certain habits can contribute to the development of GERD. Avoid smoking or using tobacco products, as smoking can weaken the lower oesophageal sphincter. Practice stress reduction techniques, as stress can aggravate GERD symptoms. Additionally, it is essential to maintain a healthy weight and engage in regular physical activity.
Avoiding Triggers
Identifying and avoiding triggers that worsen GERD symptoms is essential for prevention. Keep track of foods, beverages, and activities that seem to trigger symptoms and try to minimize their consumption or frequency. This may involve keeping a food diary or seeking professional guidance from a registered dietitian.
Management
Managing GERD involves regular monitoring of symptoms, maintaining regular physician visits, and seeking support from support groups or healthcare professionals.
Monitoring Symptoms
Keep track of your symptoms, their frequency, and severity. This will help you identify patterns and triggers, enabling you to make necessary adjustments to your lifestyle and treatment plan.
Regular Physician Visits
Scheduled visits with your healthcare provider are crucial for managing GERD effectively. They can monitor your progress, adjust medications if needed, and address any concerns or new symptoms that may arise.
Support Groups
Joining support groups or seeking guidance from healthcare professionals who specialize in digestive disorders can provide valuable information, tips, and emotional support. Support groups can offer insight into others’ experiences with GERD, which can be helpful in managing the condition.
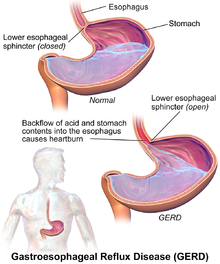
Risk Factors
Certain factors can increase the risk of developing GERD. These include:
Obesity
Being overweight or obese increases the pressure on the stomach, pushing the stomach contents upward and increasing the likelihood of acid reflux.
Hiatal Hernia
A hiatal hernia occurs when a portion of the stomach pushes up into the chest through the diaphragm, weakening the lower oesophageal sphincter and leading to acid reflux.
Pregnancy
During pregnancy, the growing uterus places pressure on the stomach, which can cause stomach acid to reflux into the oesophagus.
Smoking
Smoking weakens the lower oesophageal sphincter, making it easier for stomach acid to reflux into the oesophagus.
Certain Medications
Some medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and calcium channel blockers, can relax the lower oesophageal sphincter, leading to acid reflux.
Complications
When left untreated, GERD can lead to various complications.
Esophagitis
Repeated exposure of the oesophageal lining to stomach acid can cause inflammation and swelling, leading to esophagitis. This condition may cause pain, difficulty swallowing, and even bleeding.
Esophageal Stricture
The scarring caused by repeated acid reflux can lead to a narrowed oesophagus, known as an esophageal stricture. This can make it difficult to swallow and may require special procedures to dilate the oesophagus.
Barrett’s Esophagus
Barrett’s esophagus is a condition where the lining of the oesophagus changes and becomes similar to the lining of the intestine. This change in the lining is a precursor to oesophageal cancer and requires ongoing monitoring.
Respiratory Problems
GERD can contribute to various respiratory problems, including asthma, chronic cough, and recurrent pneumonia. The refluxed stomach acid can irritate the airways, causing inflammation and triggering respiratory symptoms.
Lifestyle Modifications
Making specific lifestyle modifications can help manage and alleviate symptoms of GERD.
Dietary Changes
Avoiding foods that trigger acid reflux can significantly reduce symptoms. Limit or eliminate caffeine, alcohol, spicy foods, fatty foods, and acidic foods from your diet. Instead, opt for a diet rich in fruits, vegetables, whole grains, and lean proteins.
Eating Habits
Changing eating habits can also make a difference. Eat smaller, more frequent meals throughout the day rather than large meals. Avoid lying down immediately after eating, as this can promote acid reflux. Elevate the head of your bed by using a wedge or raising the mattress to reduce nighttime acid reflux.
Weight Management
Maintain a healthy weight and engage in regular physical activity. Obesity and overweight can contribute to the development of GERD, and weight loss can help alleviate symptoms.
Medications
Several medications are available to manage the symptoms and reduce the amount of acid produced in the stomach.
Antacids
Antacids, such as calcium carbonate or magnesium hydroxide, can provide temporary relief by neutralizing stomach acid. They may be taken as needed after meals or at bedtime.
H2 Blockers
H2 blockers, such as ranitidine or famotidine, reduce the production of stomach acid. They are taken on a regular basis to control symptoms and promote healing of the oesophagus.
Proton Pump Inhibitors
Proton pump inhibitors (PPIs) are the most potent acid-suppressing medications and are typically prescribed for severe or persistent GERD symptoms. PPIs reduce the production of stomach acid and can provide long-term relief.
Surgical Options
In certain cases, surgical intervention may be necessary to manage GERD effectively.
Fundoplication
Fundoplication is a surgical procedure where the upper part of the stomach is wrapped around the lower oesophageal sphincter, reinforcing its closure. This procedure helps to prevent acid reflux and can provide long-term relief of symptoms.
LINX Procedure
The LINX procedure involves the placement of a ring of small magnetic beads around the junction of the stomach and oesophagus. This ring helps to strengthen the lower oesophageal sphincter, preventing acid reflux.
Endoscopic Procedures
Endoscopic procedures, such as radiofrequency ablation or stenting, may be performed to treat complications of GERD or to manage symptoms. These minimally invasive procedures aim to reduce the severity of acid reflux and promote healing of the oesophagus.
In conclusion, understanding GERD is essential for managing the condition effectively. With the right lifestyle modifications, medications, and surgical options, individuals with GERD can experience reduced symptoms, improved quality of life, and a decreased risk of complications. Regular monitoring, physician visits, and seeking support from support groups or healthcare professionals can also contribute to successful management of GERD. By following dietary recommendations, adopting healthy habits, and avoiding triggers, individuals can significantly reduce the risk of developing GERD or alleviate existing symptoms. With the proper knowledge and care, GERD can be effectively managed, allowing individuals to live a comfortable and fulfilling life.